Abstract
Inflammatory bowel disease (Crohn’s disease (CD) and ulcerative colitis (UC)) is a multifactorial disease resulting from immune dysregulation in the gut. The underlying colitis is characterized by high levels of inflammatory cytokines, including TNFα. Biological intervention for IBD patients using anti-TNFα antibodies is often an effective therapeutic solution. However, TNFα neutralization fails to induce remission in a subgroup of IBD patients, primarily in UC patients. There is a dearth of suitable animal models representing TNFα non-responders. Here we have combined one of the best UC models currently available, namely Winnie and the TNFαKO mouse to generate a TNFα-deficient Winnie to study early onset colitis. The induced TNFα deficiency with underlying colitis does not influence general health (viability and body weight) or clinical parameters (colon weight, colon length and histological colitis) when compared with the Winnie genotype alone. The molecular characterization resulted in identification of Il1β as the major elevated cytokine during early phases of colitis. Further, in vitro functional assay using bone marrow-derived dendritic cells confirmed IL-1β as the major cytokine released in the absence of TNFα. This study has generated a successful model of colitis that remains TNFα non-responsive and has demonstrated that IL-1β expression is a major pathway for the progression of colitis in this system. These data also suggest that IL-1β can be a potential target for clinical intervention of UC patients who fail to respond to TNFα neutralization.
Similar content being viewed by others
Main
Inflammatory bowel diseases (IBD) include Crohn’s disease (CD) and ulcerative colitis (UC), which are both chronic relapsing inflammatory disorders of the gastro-intestinal tract.1 The mucosal immune system is dynamically regulated to a state of tolerance to luminal antigens including commensal bacteria and food-derived antigens. However, breaches of mucosal immune tolerance can occur due to both environmental and genetic factors resulting in perturbed intestinal homeostasis. Several different events can trigger inflammatory responses that may result in chronic inflammation and pathological changes associated with IBD. A common ground for this multifactorial disorder is an increased production of diverse panel of cytokines,2, 3 some of which are pro-inflammatory and hence targets for therapeutic blockade.4 Among the cytokine milieu dysregulated in IBD-like chronic inflammatory conditions, tumor necrosis factor α (TNFα) is a major pro-inflammatory cytokine that drives downstream immune responses resulting in IBD. Colonic macrophages are reported to be the major source of TNFα in active IBD.5 Studies of macrophages isolated from the colon of patients with active IBD have reported elevated TNFα production.6, 7 Additionally, TNFα is also produced by numerous other immune cells such as T and B lymphocytes,8, 9 intestinal epithelial cells10 and several other cells.11 It is well known that TNFα polymorphisms result in increased pathogenic TNFα-driven intestinal gut pathology in CD.12 Clinical investigations have led to the discovery of anti-TNFα monoclonal antibodies (Infliximab and others) which have dramatically changed the medical approach to IBD.
Similar to CD, a subgroup of UC patients also exhibit increased TNFα levels in the colon. In fact, Braegger et al.13 reported the presence of TNFα in stool samples in such UC patients. Numerous studies have confirmed the crucial role of TNFα in colitis.14, 15 Results obtained by Corazza et al. were particularly relevant in exploring the role of TNFα in the onset of UC. Using TNFαKO murine models they were able to demonstrate the importance of TNFα production by non-T cells of the colonic mucosa in the pathogenesis of colitis.16 However, there is a subgroup of human IBD non-responders to anti-TNFα therapies, particularly in the UC cohort.17 Animal models have significantly contributed to the elucidation of the pathological mechanisms of IBD and to the validation of immunological targets for IBD treatment.18 However, using the currently available murine models we are unable to decipher the exact mechanism as to why some subgroups of UC patients do not respond to anti-TNFα therapies.
In order to address the lack of a model with relevance to the anti-TNFα non-responding UC patient group we planned to develop a viable model based on the best recently described murine model of UC currently available, namely Winnie. Winnie colitis is due to a missense mutation in the Muc2 mucin gene19 resulting in spontaneous distal colitis developing as early as 5 weeks of age. In the Winnie mouse the colonic pathology is predominantly mediated by the dysregulation of numerous cytokines, including elevated TNFα similar to human UC where the intestinal inflammation is most severe in the distal colon and the disease severity increases with age.20 In order to remove the effect of TNFα in the Winnie spontaneous colitis, we generated Winnie/TNFα knockout to explore the axis between TNFα and intestinal inflammation that may resemble UC non-responders to anti-TNFα therapies,21, 22 or patients who become non-responder (secondary non-responder) in the absence of anti-Infliximab antibodies.23
Detailed histological and immunological assessment of early differences between Winnie and TNFα KO Winnie revealed that TNFα KO Winnie exacerbates pathogenesis associated with an increased inflammatory cytokines secretion, particularly IL-1β. Furthermore, elevated Il1β transcription was detectable in 5-week-old mice prior to the onset of morphological signs of UC, suggesting that this cytokine may represent a predictive biomarker for UC patients who are non-responder to anti-TNFα therapy and possibly an alternative target for combinatorial biological approaches.
Results
TNFα deficiency does not influence general health and clinical parameters
TNFα is commonly considered the primary immunological target for IBD treatment. To investigate the axis between TNFα and UC onset, we used a breeding strategy based on double heterozygote breeders (Figure 1a) to obtain the double mutants and all the controls from the same breeding pair. This strategy permitted the evaluation of viability and weight of the offspring depending on the different genotypes and independently from differences related to diverse mothers. Results shown in Figure 1a demonstrate that all the resulting strains were viable and no significant variation from the predicted genotype (6.25%) was obtained in the 4-week-old offspring.
Generation and characterization of the new TNFα KO Winnie murine model. (a) TNFα KO Winnie mice were generated by breeding double heterozygote breeders for TNFα and Winnie genes to obtain the double mutants and all the controls from the same breeding pair. All the resulting strains were viable and no significant variation from the predicted genotype was obtained in the 4-week-old offspring. (b) Weight analysis of 4-week-old mice from different genotypes reveals a significant decrease in body weight in mice carrying the Winnie mutation independently of the TNFα phenotype in both males and females. Statistical evaluation between C57/BL6 mice and each murine line was performed using unpaired two-tailed Student’s t-test. ***P<0.001, **P<0.01, *P<0.05
Figure 1b shows that significant differences in mouse weight could be seen in 4-week-old mice from different genotypes. Overall, Winnie and TNFα KO Winnie (both male and female) mice were lighter (8.28±0.23 and 8.76±0.39, respectively) than WT (C57/BL6) and TNFα KO controls (12.59±0.31 and 12.39±0.46, respectively). Between Winnie and TNFα KO Winnie there was no difference in body weight. These results show that mice carrying the Winnie mutation had lower body weight independently from TNFα.
TNFα deficiency does not influence the initial development of intestinal inflammation
Macroscopic or histological colitis as demonstrated by colon shortening and hematoxylin and eosin (H&E) histological scoring of inflammation in C57/BL6 mice (7.22±0.42) was not significantly different from TNFα KO mice (6.81±0.15); however, the colon length of both groups were significantly longer than Winnie (6.01±0.27) and TNFα KO Winnie (6.13±0.20) if compared with WT mice (Figures 2a and b). The differences were much more striking when adjusted for body weight (Figure 2c).
Macroscopic and histological characterization of the TNFα KO Winnie. Representative images of dissected colons (a) and measures of colon length (b) from the new transgenic line and the relative controls indicate a significant reduction in Winnie and TNFα KO Winnie compared with WT. This observation is strikingly evident when the colon length is adjusted for the body weight (c). Hematoxylin and eosin staining of 3 μm sections of colon (d) and the average score of inflammation (e) show no significant differences between the TNFα KO Winnie and the controls. Statistical evaluation between C57/Bl6 mice and each murine line was performed using unpaired two-tailed Student’s t-test. ***P<0.001, *P<0.05
Detailed histological analysis (ulceration, re-epithelization, transmural inflammation and chronic inflammation) revealed a similar picture where there was no difference in inflammatory scores between C57/BL6 mice and TNFα KO mice while the inflammatory scores being higher in Winnie and TNFα KO Winnie (Figures 2d and e). However, there was no difference between Winnie and TNFα KO Winnie cohorts.
TNFα deficiency results in elevated expression of Ifnγ and Il1β during early onset colitis
The cytokine expression and secretion signatures responsible for the increased inflammation in Winnie and TNFα KO Winnie were investigated to identify any potential molecular mechanisms mediated by TNFα during early onset colitis. We employed a panel of cytokine markers of Th1 (Il1β, Ifnγ and Il12), Th2 (Il4, Il10), Th17 (Il17a) and T-regs (Foxp3) populations to specifically quantify the relative gene expression across all cohorts by qPCR. Relative expression analysis revealed a striking elevation of Il1β (Figure 3a) and Ifnγ (Figure 3b) in TNFα KO Winnie mice compared with all other mice strains. Strikingly, in the Winnie background, the absence of TNFα leads to a molecular pathway that results in a pattern suggestive of an increased Th1 signature. The Th1-promoting cytokine Il12 (Figure 3c) was also upregulated in TNFα KO Winnie, reinforcing the elevated Ifnγ observed. The expression of the anti-inflammatory cytokine Il10 was also increased in Winnie and TNFα KO Winnie (Figure 3d), although the ratio between Il12 and Il10 is higher in TNFα KO Winnie. Furthermore, both in Winnie and TNFα KO Winnie, we observed a higher expression of the Th2 cytokine Il4 (Figure 3e) compared with controls. The expression of Il17a and Foxp3 was also evaluated, but results were below detection.
TNFα KO Winnie mice show an increased Th1 signature at the molecular level. mRNA was extracted from the colon of all the 5-week-old mice genotypes. The expression level of Il1β, Ifnγ, Il12, Il10 and Il4 was measured by qPCR and normalized to the housekeeping gene Gapdh (a, b, c, d, e, respectively). Bars represent mean relative expression±S.E.M. (n=4) for each genotype. Statistical evaluation between C57/Bl6 mice and each murine line was performed using unpaired two-tailed Student’s t-test. ***P<0.001, **P<0.01, *P<0.05
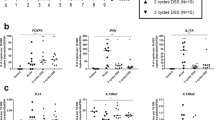
Additionally, we evaluated the mechanism behind TNFα negative feedback on IL-1β secretion. In particular, we compared NLRP3 and caspase-1 activation in Winnie and TNFα KO Winnie intestinal samples. In line with the increased IL-1β secretion, we observed a marked increase in the levels of NLRP3 activation in Winnie mice particularly in the absence of TNFα (Figure 4a). The level of caspase-1 activation was increased in Winnie compared with WT, but the absence of TNFα strongly affected caspase-1 activation, which resulted in approximately doubled expression levels in TNFα KO Winnie (Figure 4b). Finally, we evaluated the serum levels of cytokines of 5-week-old mice (4 mice per group) by Bead-based Multiplex assay. Among the pro/anti-inflammatory molecules analyzed, IL-6 was elevated in the serum of Winnie and TNFα KO Winnie compared with the control, approximately two and three times higher, respectively, (Figure 5a). IFNγ and IL-1α were elevated in the TNFα KO Winnie serum (Figures 5b and c, respectively). Serum IL-1β was not increased in TNFα KO Winnie (data not shown), suggesting that systemic secretion of IL-1β was low, perhaps due to the early age and level of colitis.
Ileum homogenates show higher expression of NLRP3 and active form of caspase-1 in TNFα KO Winnie. Western blot analyses showed that the expression of NLRP3 (a) was higher in both Winnie and TNFα KO Winnie mice. Similarly, (b) the active form of caspase-1 (25 kDa) was significantly higher in both Winnie and TNFα KO Winnie mice. Quantitative data (bar graphs) were obtained by using ImageJ (NIH, USA) software. Statistical analysis was performed by using one-way ANOVA followed by Tukey’s multiple comparison as post-test. ***P<0.001, **P<0.01, *P<0.05
TNFα KO Winnie mice secrete high levels of circulating inflammatory cytokines. Circulating levels of IL-6, IFNγ and IL-1α (a, b and c, respectively) were determined by Bead-based Multiplex assay from serum samples of 5-week-old TNFα KO Winnie and all the control lines. Bars represent mean cytokines concentration±S.E.M. (n=4). Statistical evaluation between C57/Bl6 mice and each murine line was performed using unpaired two-tailed Student’s t-test. ***P<0.001, *P<0.05
TNFα modulates IL-1β secretion in TNFα KO bone marrow-derived dendritic cells
To investigate the functional interaction between TNFα and IL-1β, we used bone marrow-derived dendritic cells (BMDCs) from wild type and TNFα KO mice. Figure 6a shows that 24 h after LPS administration, significantly higher IL-1β concentrations were detected in the supernatant of TNFα KO BMDCs as well as higher expression of Il-1β was detected in TNFα KO BMDCs exposed to LPS (Figure 6b). Addition of TNFα to TNFα KO BMDCs modulated IL-1β secretion to the same level as wild-type BMDCs (Figure 6a). We further evaluated the effect of TNFα by the administration of anti-TNFα in the BMDCs supernatant. Figure 6a shows that in wild-type BMDCs, TNFα depletion did not affect IL-1β secretion whereas TNFα KO BMDCs restored IL-1β secretion (Figure 6a) consistent with our observation in colitis.
IL-1β upregulation in TNFα KO BMDCs. BMDCs were cultured from WT (black bars) and TNFα KO (white bars) mice, treated with TNFα and anti-TNFα antibody at day 7 and concomitantly exposed to 1 μg/ml of LPS. Twenty-four hours later, the secretion of IL-1β was determined by ELISA (a). Bars represent mean cytokine concentration±S.E.M. (n=3). For each treatment statistical evaluation between WT and TNFα KO DCs was performed using two-way ANOVA and Bonferroni as post-test. For TNFα KO DCs treated with LPS, paired two-tailed Student’s t-test was conducted to compare BMDCs treated or untreated with TNFα. The expression level of Il1β was measured in WT and TNFα KO DCs by qPCR and normalized to the housekeeping gene Gapdh. Bars represent mean relative expression±S.E.M. (n=4) (b). Statistical evaluation between WT and TNFα KO DCs was performed using unpaired two-tailed Student’s t-test. *P<0.05, **P<0.01, ***P<0.001
Discussion
In 1998 the introduction of biological therapies with blocking antibodies against TNFα for CD patients represented a revolutionary change for the therapy of these patients. It is now well established that the majority of IBD patients are responsive to the anti-TNFα therapy, but a significant percentage (up to 40% in some groups of UC) can be defined as primary non-responsive.21, 22 In this study we have described a potentially important mechanism linking TNFα-mediated inflammatory cytokine control through IL-1β. The murine model developed in this study incorporates a TNFα deficiency on a background of increased colitis that is closely representative of UC non-responders.
Murine models of IBD have been successfully used for the understanding of the biological basis of the disease and for the development of new drugs.24 Studies pioneered by Corazza et al.16 dissected the different role of the lymphocyte-derived TNFα for colitis induction. Although TNFα is a pivotal factor for the initiation of the inflammatory response, the absence of TNFα is deleterious in murine models of inflammatory disorders including experimental autoimmune encephalomyelitis25 and dextran sodium sulfate-induced colitis.26 The shortcomings of the aforementioned murine models needed to be addressed in order to investigate the role of TNFα in UC non-responders. Among the available models, we used the spontaneous colitis model (Winnie) characterized by chronic intestinal inflammation resulting from a missense mutation in the Muc2 mucin gene.19 In Winnie, the defective mucus layer and increased intestinal permeability result in a spontaneous intestinal inflammation of the distal colon. To investigate predictive markers of TNFα-independent UC in a spontaneous and progressive colitis model, we crossed Winnie mice with TNFα KO (commercial line 5540) to create double KO mice (TNFα KO Winnie).
We crossed heterozygote mice to obtain all the required strains from the same breeding stock. From the genotype analysis we confirmed that all strains were viable. In our system the well-documented association between TNFα deficiency and low body weight was observed only for male mice even if at a lesser extent. Instead, the Winnie genotype, independently from TNFα, shows a marked reduction in the body weight. Macroscopic and histological assessment of the colon also suggest that the intestinal inflammation in the Winnie model was not affected by TNFα deficiency. Our study shows that in the absence of TNFα there is a significant compensatory increase in IL-1β production. This observation is even more interesting in the context of young mice (5-week-old) that do not yet show morphological signs of inflammation, including accumulation of inflammatory cells. Additionally, we also demonstrated that following LPS exposure, TNFα KO DCs produce three times the amount of IL-1β compared with WT DCs and that exogenous TNFα administration can delete the observed difference. Both these evidences point to a functional role for IL-1β in the pathogenesis of IBD. Recent research suggest that IL-1β secretion is mainly mediated by the inflammasome activation in general and NLRP3 in particular.27 Our data indicate that inflammasome activation may be a key aspect of protection in the absence of TNFα. We also observed an increased expression of Ifnγ and Il4 in the absence of TNFα. It is not surprising to observe these results given a similar scenario to that observed in Winnie when IL-17 is blocked with anti-IL-17 antibodies in vivo.28
TNFα KO mice were previously described as a model mounting a vigorous, disorganized inflammatory response leading to death in response to the injection with heat-killed Corynebacterium parvum.29 TNFα anti-inflammatory properties were previously known, but mainly attributed to the ability to induce T-cell apoptosis.30 Here we demonstrate that TNFα KO DCs produce large amounts of IL-1β, an inflammatory cytokine detectable in patients with active UC.31 Our data suggest the existence of a negative feedback between TNFα and IL-1β as recently noticed by West et al.,32 indicating IL-1β as one of the predictive markers for anti-TNFα non-responders during colonic onset of inflammation.
In conclusion, we believe we have described a valuable model that closely represents a cohort of UC patients that are non-responsive to current anti-TNFα therapies and also identified a potential biomarker for UC non-responders to anti-TNFα therapies. Further research to functionally characterize the role of IL-1β would be the next step in targeted combinatorial therapy in UC non-responders patients.
Material and methods
Mice
Investigation has been conducted according to national and international guidelines and has been approved by the authors' institutional review board (Organism For Animal Wellbeing – OPBA). The new murine transgenic line TNFα KO Winnie was created by breeding heterozygous mice from TNFα knockout line and heterozygous Winnie mice, a murine line established from Dr. Eri’s group at the University of Tasmania. The TNFα knockout murine line was purchased from Jackson Laboratories (B6.129S-Tnftm1Gkl/J, stock No: 005540; weight: approximately 20 g) (Bar Harbor, ME, USA).
All animal experiments were carried out in accordance with Directive 86/609 EEC enforced by Italian D.L. n. 116 1992, and approved by the Committee on the Ethics of Animal Experiments of Ministero della Salute – Direzione Generale Sanità Animale (768/2015-PR 27/07/2015) and the official RBM veterinarian. Animals were killed if found in severe clinical condition in order to avoid undue suffering.
Histological examination
Tissue section from the distal colon were fixed in 10% buffered formalin and embedded in paraffin. Sections of 3 μm were stained with H&E. Images were acquired using Leica LMD 6500 (Leica Microsystems, Wetzlar, Germany). The histological score was calculated by adding the values relative to the following parameters: ulceration (0–3), re-epithelization (0–3), transmural inflammation (0–3) and chronic inflammation (0–3).
RNA extraction and qPCR analysis
Total RNA was isolated from the medial part of the large intestine. The RNA was extracted using TRIzol (Thermo Fisher Scientific, MA, USA) according to the manufacturer’s instructions. Five hundred nanograms of total RNA was reverse transcribed with the High Capacity cDNA Reverse Transcription kit (Thermo Fisher Scientific) by using random primers for cDNA synthesis. Gene expression of Il1β, Ifnγ, Il12, Il10, Il4 and Gapdh was performed with TaqMan gene expression assays (Thermo Fisher Scientific) murine probes: Mm00434228_m1, Mm01168134_m1, Mm01288989_m1, Mm00439614_m1, Mm00445259_m1, Mm99999915_g1, respectively. Real-time analysis was performed on CFX96 System (Biorad, Hercules, CA, USA) and the expression of all target genes was calculated relative to Gapdh expression using the ΔΔCt method.
Multiplex cytokine ELISA
Serum from 5-week-old male mice of each experimental group was analyzed using the Bead-based Multiplex for the Luminex platform (LaboSpace srl, Milano, Italy).
Generation and culture of murine DCs
BMDCs were obtained from TNFα KO mice (5540 line). Briefly, single-cell suspension of BMDCs cells from the tibiae and femurs of 6- to 8-week-old male mice were flushed with 0.5 mM EDTA (Thermo Fisher Scientific), and depleted of red blood cells with ACK lysing buffer (Thermo Fisher Scientific). Cells were plated in a 10 ml dish (1 × 106 cells/ml) in RPMI 1640 (Thermo Fisher Scientific) supplemented with 10% heat-inactivated fetal bovine serum (Thermo Fisher Scientific), 100 U/ml penicillin (Thermo Fisher Scientific), 100 mg/ml streptomycin (Thermo Fisher Scientific), 25 μg/ml rmGM-CSF (Miltenyi Biotec, Bergisch Gladbach, Germany), and 25 μg/ml rmIL-4 (Miltenyi Biotec) at 37 °C in a humidified 5% CO2 atmosphere. On day 5 cells were harvested, re-stimulated with new growth factors and plated 1 × 106 cells/ml on 24-well culture plate. On day 7 BMDCs were stimulated with 1 μg/ml of LPS (L6143, Sigma-Aldrich, St Louis, MO, USA) and, at the same time, with TNFα standard (40 ng/ml) and anti-TNFα or anti-IL-1β antibody (400 ng/ml and 80 ng/ml, respectively). Supernatants were collected 24 h after LPS stimulation.
Western blot analysis
Ileum were homogenated as already reported by Terlizzi et al.33 Homogenized samples were used to examine the expression of NLRP3 (AbCam, UK) and caspase-1 active form (25 kDa; AbCam, Cambridge, UK). Quantitative data were evaluated by means of ImageJ (NIH, Bethesda, MD, USA) software.
ELISA
Cell culture supernatants were analyzed for IL-1β release in triplicate, using an ELISA kit (R&D Systems, Minneapolis, MN, USA) following the manufacturer’ instructions.
Statistical analysis
Statistical analysis was performed using the Graphpad Prism statistical software release 5.0 for Windows XP. All data were expressed as means±S.E.M. of data obtained from at least three independent experiments. We evaluated statistical significance with two-tailed Student’s t-test, one-way ANOVA followed by Tukey’s multiple comparison as post-test and the two-way ANOVA test using the Bonferroni as a post-test for the grouped analysis. Results were considered statistically significant at P<0.05.
References
Corridoni D, Arseneau KO, Cominelli F . Inflammatory bowel disease. Immunol Lett 2014; 161: 231–235.
Neurath MF . Cytokines in inflammatory bowel disease. Nat Rev Immunol 2014; 14: 329–342.
Chen ML, Sundrud MS . Cytokine networks and T-cell subsets in inflammatory bowel diseases. Inflamm Bowel Dis 2016; 22: 1157–1167.
Strober W, Fuss IJ . Proinflammatory cytokines in the pathogenesis of inflammatory bowel diseases. Gastroenterology 2011; 140: 1756–1767.
Tracey KJ, Cerami A . Tumor necrosis factor: a pleiotrophic cytokine and therapeutic target. Ann Rev Med 1994; 45: 491–503.
Reinecker HC, Steffen M, Witthoeft T, Pflueger I, Schreiber S, MacDermott RP et al. Enhanced secretion of tumour necrosis factor-alpha, IL-6, and IL-1 beta by isolated lamina propria mononuclear cells from patients with ulcerative colitis and Crohn’s disease. Clin Exp Immunol 1993; 94: 174–181.
Derkx B, Taminiau J, Radema S, Stronkhorst A, Wortel C, Tytgat G et al. Tumour-necrosis factor antibody treatment in Crohn’s disease (letter). Lancet 1993; 342: 173–174.
Yu M, Wen S, Wang M, Liang W, Li H-H, Long Q et al. TNF-α-secreting B cells contribute to myocardial fibrosis in dilated cardiomyopathy. J Clin Immunol 2013; 33: 1002–1008.
Rimoldi M, Chieppa M, Salucci V, Avogadri F, Sonzogni A, Sampietro GM et al. Intestinal immune homeostasis is regulated by the crosstalk between epithelial cells and dendritic cells. Nat Immunol 2005; 6: 507–514.
Jung HC, Eckmann L, Yang SK, Panja A, Fierer J, Morzycka-Wroblewska E et al. A distinct array of proinflammatory cytokines is expressed in human colon epithelial cells in response to bacterial invasion. J Clin Invest 1995; 95: 55–65.
Guy-Grand D, DiSanto JP, Henchoz P, Malassis-Séris M, Vassalli P . Small bowel enteropathy: role of intraepithelial lymphocytes and of cytokines (IL-12, IFN-gamma, TNF) in the induction of epithelial cell death and renewal. Eur J Immunol 1998; 28: 730–744.
Barber GE, Yajnik V, Khalili H, Giallourakis C, Garber J, Xavier R et al. Genetic markers predict primary non-response and durable response To anti-TNF biologic therapies in crohn's disease. Am J Gastroenterol 2016; 111: 1816–1822.
Braegger CP, Nicholls S, Murch SH, Stephens S, MacDonald TT . Tumour necrosis factor alpha in stool as a marker of intestinal inflammation. Lancet 1992; 339: 89–91.
Neurath MF, Pettersson S, Meyer zum Büschenfelde KH, Strober W . Local administration of antisense phosphorothioate oligonucleotides to the p65 subunit of NK-kB abrogates established experimental colitis in mice. Nat Med 1996; 2: 998–1004.
Simpson SJ, Shah S, Comiskey M, de Jong YP, Wang B, Mizoguchi E et al. T cell-mediated pathology in two models of experimental colitis depends predominantly on the interleukin 12/signal transducer and activator of transcription (Stat)-4 pathway, but is not conditional on Interferon γ expression by T cells. J Exp Med 1998; 187: 1225–1234.
Corazza N, Eichenberger S, Eugster HP, Mueller C . Nonlymphocyte-derived tumor necrosis factor is required for induction of colitis in recombination activating gene (RAG)2(-/-) mice upon transfer of CD4(+)CD45RB(hi) T cells. J Exp Med 1999; 190: 1479–1492.
Papamichael K, Rivals-Lerebours O, Billiet T, Vande Casteele N, Gils A, Ferrante M et al. Long-Term Outcome of Patients with Ulcerative Colitis and Primary Non-response to Infliximab. J Crohns Colitis 2016; 10: 1015–1023.
Khanna PV, Shih DQ, Haritunians T, McGovern DP, Targan S . Use of animal models in elucidating disease pathogenesis in IBD. Semin Immunopathol 2014; 36: 541–551.
Heazlewood CK, Cook MC, Eri R, Price GR, Tauro SB, Taupin D et al. Aberrant mucin assembly in mice causes endoplasmic reticulum stress and spontaneous inflammation resembling ulcerative colitis. PLoS Med 2008; 5: e54.
Eri RD, Adams RJ, Tran TV, Tong H, Das I, Roche DK et al. An intestinal epithelial defect conferring ER stress results in inflammation involving both innate and adaptive immunity. Mucosal Immunol 2011; 4: 354–364.
Ben-Horin S, Chowers Y . Tailoring anti-TNF therapy in IBD: drug levels and disease activity. Nat Rev Gastroenterol Hepatol 2014; 11: 243–255.
Guerra I, Bermejo F . Management of inflammatory bowel disease in poor responders to infliximab. Clin Exp Gastroenterol 2014; 7: 359–367.
Baert F, Noman M, Vermeire S, Van Assche G, D' Haens G, Carbonez A et al. Influence of immunogenicity on the long-term efficacy of infliximab in Crohn's disease. N Engl J Med 2003; 348: 601–608.
Strober W . Why study animal models of IBD? Inflamm Bowel Dis 2009; 15: 1438–1447.
Kassiotis G, Kollias G . Uncoupling the proinflammatory from the immunosuppressive properties of tumor necrosis factor (TNF) at the p55 TNF receptor level: implications for pathogenesis and therapy of autoimmune demyelination. J Exp Med 2001; 193: 427–434.
Naito Y, Takagi T, Handa O, Ishikawa T, Nakagawa S, Yamaguchi T et al. Enhanced intestinal inflammation induced by dextran sulfate sodium in tumor necrosis factor-alpha deficient mice. J Gastroenterol Hepatol 2003; 18: 560–569.
Perera AP, Kunde D, Eri R . NLRP3 Inhibitors as potential therapeutic agents for treatment of Inflammatory Bowel Disease. Curr Pharm Des 2017; 23: 2321–2327.
Wang R, Hasnain SZ, Tong H, Das I, Che-Hao Chen A, Oancea I et al. Neutralizing IL-23 is superior to blocking IL-17 in suppressing intestinal inflammation in a spontaneous murine colitis model. Inflamm Bowel Dis 2015; 21: 973–984.
Marino MW, Dunn A, Grail D, Inglese M, Noguchi Y, Richards E et al. Characterization of tumor necrosis factor-deficient mice. Proc Natl Acad Sci USA 1997; 94: 8093–8098.
Zhou T, Fleck M, Müeller-Ladner U, Yang P, Wang Z, Gay S et al. Kinetics of Fas-induced apoptosis in thymic organ culture. J Clin Immunol 1997; 17: 74–84.
Lacruz-Guzmán D, Torres-Moreno D, Pedrero F, Romero-Cara P, García-Tercero I, Trujillo-Santos J et al. Influence of polymorphisms and TNF and IL1β serum concentration on the infliximab response in Crohn's disease and ulcerative colitis. Eur J Clin Pharmacol 2013; 69: 431–438.
West NR, Hegazy AN, Owens BMJ, Bullers SJ, Linggi B, Buonocore S et al. Oncostatin M drives intestinal inflammation and predicts response to tumor necrosis factor–neutralizing therapy in patients with inflammatory bowel disease. Nat Med 2017; 23: 579–589.
Terlizzi M, Di Crescenzo VG, Perillo G, Galderisi A, Pinto A, Sorrentino R . Pharmacological inhibition of caspase-8 limits lung tumour outgrowth. Br J Pharmacol 2015; 172: 3917–3928.
Acknowledgements
This work was supported by the Italian Ministry of Health, 'GR-2011-02347991' and by Regione Puglia 'NATURE–XUANRO4'. We are grateful to all members of LAB-81 and to the I.C. Bregante Volta of Monopoli (BA) for their constructive help and support.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Edited by M Piacentini
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Cell Death and Disease is an open-access journal published by Nature Publishing Group. This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
De Santis, S., Kunde, D., Galleggiante, V. et al. TNFα deficiency results in increased IL-1β in an early onset of spontaneous murine colitis. Cell Death Dis 8, e2993 (2017). https://doi.org/10.1038/cddis.2017.397
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cddis.2017.397
- Springer Nature Limited
This article is cited by
-
Inactivation of the gene encoding procalcitonin prevents antibody-mediated arthritis
Inflammation Research (2023)
-
Dual role of melatonin as an anti-colitis and anti-extra intestinal alterations against acetic acid-induced colitis model in rats
Scientific Reports (2022)
-
Inflammation triggers immediate rather than progressive changes in monocyte differentiation in the small intestine
Nature Communications (2019)