Abstract
Study Design
Biomechanical analysis.
Objectives
To show the role of additional rods and long-term fatigue strength to prevent the instrumentation failure on three-column osteotomies.
Summary of Background Data
Three-column osteotomy such as pedicle subtraction osteotomy (PSO) and vertebral column resections are surgical correction options for fixed spinal deformity. Posterior fixation for the PSO involves pedicle screweand rod-based instrumentation, with the rods being contoured to accommodate the accentuated lordosis. Pseudarthrosis and instrumentation failure are known complications of PSO.
Methods
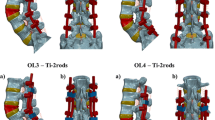
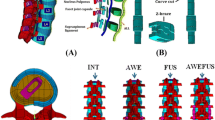
Unilateral pedicle screw and rod constructs were mounted in ultra-high-molecular-weight polyethylene blocks using a vertebrectomy model with the rods contoured to simulate posterior fixation of a PSO. Each construct was cycled under a 200 N load at 5 Hz in simulated flexion and extension to rod failure. Three configurations (n 5 5) of titanium alloy rods were tested: single rod (control), double rod, and bridging rod. Outcomes were total cycles to failure and location of rod failure.
Results
Double-rod and bridging-rod constructs had a significantly higher number of cycles to failure compared with the single-rod construct (p <.05). Single-rod constructs failed at or near the rod bend apex, whereas the majority of double-rod and bridging-rod constructs failed at the screwerod or rodeconnector junction.
Conclusions
Double-rod and bridging-rod constructs are more resistant to fatigue failure compared with single-rod constructs in PSO instrumentation and could be considered to mitigate the risk of instrumentation failure.
Similar content being viewed by others
References
Kim WJ, Kang JW, Kang SI, et al. Factors affecting clinical results after corrective osteotomy for lumbar degenerative kyphosis. Asian Spine J 2010;4:7–14.
Kim YJ, Bridwell KH, Lenke LG, et al. Results of lumbar pedicle subtraction osteotomies for fixed sagittal imbalance: a minimum 5-year follow-up study. Spine 2007;32:2189–97.
Hyun SJ, Rhim SC. Clinical outcomes and complications after pedicle subtraction osteotomy for fixed sagittal imbalance patients: a long-term follow-up data. J Korean Neurosurg Soc 2010;47:95–101.
Joseph Jr SA, Moreno AP, Brandoff J, et al. Sagittal plane deformity in the adult patient. J Am Acad Orthop Surg 2009;17:378–88.
Potter BK, Lenke LG, Kuklo TR. Prevention and management of iatrogenic flatback deformity. J Bone Joint Surg Am 2004;86-A:1793–808.
La Grone MO. Loss of lumbar lordosis. A complication of spinal fusion for scoliosis. Orthop Clin North Am 1988;19:383–93.
Bridwell KH, Lewis SJ, Lenke LG, et al. Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance. J Bone Joint Surg Am 2003;85-A:454–63.
Bridwell KH, Lewis SJ, Rinella A, et al. Pedicle subtraction osteotomy for the treatment of fixed sagittal imbalance. Surgical technique. J Bone Joint Surg Am 2004;86-A(suppl 1):44–50.
Gill JB, Levin A, Burd T, Longley M. Corrective osteotomies in spine surgery. J Bone Joint Surg Am 2008;90:2509–20.
Bridwell KH, Lewis SJ, Edwards C, et al. Complications and outcomes of pedicle subtraction osteotomies for fixed sagittal imbalance. Spine 2003;28:2093–101.
Kim YJ, Bridwell KH, Lenke LG, et al. Pseudarthrosis in adult spinal deformity following multisegmental instrumentation and arthrodesis. J Bone Joint Surg Am 2006;88:721–8.
Mok JM, Cloyd JM, Bradford DS, et al. Reoperation after primary fusion for adult spinal deformity: rate, reason, and timing. Spine 2009;34:832–9.
Scheer JK, Tang JA, Deviren V, et al. Biomechanical analysis of revision strategies for rod fracture in pedicle subtraction osteotomy. Neurosurgery 2011;69:164–72; discussion 172.
Smith JS, Sansur CA, Donaldson 3rd WF, et al. Short-term morbidity and mortality associated with correction of thoracolumbar fixed sagittal plane deformity: a report from the Scoliosis Research Society Morbidity and Mortality Committee. Spine 2011;36:958–64.
Yang BP, Ondra SL, Chen LA, et al. Clinical and radiographic outcomes of thoracic and lumbar pedicle subtraction osteotomy for fixed sagittal imbalance. J Neurosurg Spine 2006;5:9–17.
Cho KJ, Suk SI, Park SR, et al. Complications in posterior fusion and instrumentation for degenerative lumbar scoliosis. Spine 2007;32:2232–7.
Lindsey C, Deviren V, Xu Z, et al. The effects of rod contouring on spinal construct fatigue strength. Spine 2006;31:1680–7.
Tang JA, Leasure JM, Smith JS, et al. Effect of severity of rod contour on posterior rod failure in the setting of lumbar pedicle subtraction osteotomy (PSO): a biomechanical study. Neurosurgery 2013;72:276–82; discussion 283.
Hyun SJ, Lenke LG, Kim YC, et al. Comparison of standard 2-rod constructs to multiple-rod constructs for fixation across 3-column spinal osteotomies. Spine 2014;39:1899–904.
ASTM. Standard test methods for spinal implant constructs in a ver-tebrectomy model. Designation F1717-011-16.
Nguyen TQ, Buckley JM, Ames C, Deviren V. The fatigue life of contoured cobalt chrome posterior spinal fusion rods. Proc Inst Mech EngH 2011;225:194–8.
Booth KC, Bridwell KH, Lenke LG, et al. Complications and predictive factors for the successful treatment of flatback deformity (fixed sagittal imbalance). Spine 1999;24:1712–20.
Ikenaga M, Shikata J, Takemoto M, Tanaka C. Clinical outcomes and complications after pedicle subtraction osteotomy for correction of thoracolumbar kyphosis. J Neurosurg Spine 2007;6:330–6.
Chang KW, Cheng CW, Chen HC, et al. Closing-opening wedge osteotomy for the treatment of sagittal imbalance. Spine 2008;33:1470–7.
Cho KJ, Bridwell KH, Lenke LG, et al. Comparison of Smith-Petersen versus pedicle subtraction osteotomy for the correction of fixed sagittal imbalance. Spine 2005;30:2030–7; discussion 2038.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author disclosures: ZSJ (none); Sİ (none); DP (none); YTA (none); WKC (none).
Rights and permissions
About this article
Cite this article
Jager, Z.S., İnceoğlu, S., Palmer, D. et al. Preventing Instrumentation Failure in Three-Column Spinal Osteotomy: Biomechanical Analysis of Rod Configuration. Spine Deform 4, 3–9 (2016). https://doi.org/10.1016/j.jspd.2015.06.005
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1016/j.jspd.2015.06.005