Abstract
Background
Although many emergency department (ED) settings have implemented an electronic medical information system (EMIS) and EMIS tools in an effort to improve timeliness of care outcomes, there remains a paucity of scientific information on this topic. We therefore performed a scoping review to describe the range of EMIS interventions and their impacts on time-based outcomes in the ED.
Methods
We searched four bibliographic databases to identify potentially relevant records published after 2014 in English. Two reviewers assessed records for eligibility using a two-step screening process. We then extracted data on the type of EMIS, outcomes assessed, and reported results. Findings were summarized in tabular form and grouped by time-based outcome.
Results
Twenty-five studies met the eligibility criteria, with approximately half being retrospective studies. Interventions varied among studies; they generally included a new or updated EMIS, EMIS tools related to disease diagnosis and/or management, triage tools, or health information exchange platforms. Included studies compared interventions with relevant comparator groups, such as prior versions of an EMIS, absence of an EMIS, pen-and-paper documentation, and/or communication via telephone and fax. The most common outcomes reported were length of stay (n = 17 studies) and time to medication (n = 6 studies), followed by time to order, time to provider, and time from result to disposition. Reported effects of the interventions were generally inconsistent, showing either improvements, delays, or no change in examined outcomes.
Conclusions
Additional research is needed to determine how electronic medical information may be used in the ED to improve timeliness of care. Findings from this review can be used to inform future systematic reviews that evaluate the impact of these systems and tools on specific quality of care measures.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
The emergency department (ED) is often the most crucial and busiest unit within a hospital, as it is where urgent medical care is delivered to patients in need of immediate attention; it also commonly serves individuals experiencing difficulty accessing primary care [1, 2]. However, delivering high-quality and timely care in the ED may be limited by available resources, such as beds, medical personnel, nursing staff, laboratories, and imaging facilities [3].
Many hospitals have implemented an electronic medical information system (EMIS), which is defined as technology used to collect, organize, store, analyze, and report health information [4, 5], in an attempt to optimize the delivery of ED care [6, 7]. In addition, hospitals have also adopted the use of specific EMIS tools, such as push notifications to alert of specific events, dashboards to assist with the coordination of care services, and real-time analytics to predict the likelihood of defined outcomes (such as admission or revisit) [8, 9]. To date, existing literature on EMIS use in the ED has primarily focused on perceived benefits and downfalls of implemented technologies [10,11,12]; reported findings specific to timeliness of care and patient outcomes are diverse and sometimes conflicting.
Although use of an EMIS in ED settings may improve time-based patient outcomes, such as time to treatment, time to diagnosis, and length of stay [13,14,15], there remains a paucity of information on this topic and additional research is required to determine the effects of these technologies on time-based ED metrics. Therefore, the primary objective of our scoping review was to identify and describe interventions aimed at improving timeliness of ED care that are based on the use of an EMIS. Our secondary objective was to summarize the effects of examined interventions on the timeliness of ED care.
2 Methods
Our review complies with the Preferred Reporting Items for Systematic reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) Checklist [16].
2.1 Studies and participants
Primary studies examining the effects of an electronic medical information system (EMIS) or EMIS tool (individually and collectively referred to as EMIS hereafter) on the timeliness of patient care in the emergency department (ED) were eligible for inclusion in this review. This consisted of observational studies, pre-post studies, time-series trials, and randomized control trials (RCTs). Systematic reviews, case series, case reports, anecdotal reports of provider experiences, commentaries, and letters to the editors were excluded. Eligible participants comprised all patients receiving care at an ED. Participants were not restricted by age, sex/gender, diagnosis, or ED characteristics (such as location, size, or type).
2.2 Eligible interventions and comparison/control
Examined interventions included the use of an EMIS, which may comprise of electronic medical record (EMR) systems and/or specific programs, modules, or applications within an EMIS. Interventions had to have been compared with non-use, or to the use of a different EMIS. Studies that compared EMIS upgrades relative to an existing EMIS (without the upgrade) were also eligible for inclusion, since such studies allow for the measurement of effects of specific EMIS upgrades on timeliness of ED care.
2.3 Outcome measures
Outcomes of interest were quantitative measures of timeliness of care in the ED. These included, but were not limited to, time to triage, first physician assessment, first procedure or medication, or discharge. Studies reporting solely on outcomes that are not explicit measures of ED care timeliness were not included in this review.
2.4 Electronic searches
We searched the following four bibliographic databases to identify all potentially eligible studies: MEDLINE, PubMed, Web of Science, and the Cochrane Database of Systematic Reviews. Searches were designed with the assistance of a research librarian and executed on August 25, 2021; search results were limited to English language studies published after 2014 to capture the most relevant reports of time-based outcomes in the ED. Our search strategies are presented in Appendix 1 of the Supplementary Material.
2.5 Selection of studies
Citations retrieved from database searches were imported into DistillerSR (Evidence Partners Incorporated, Ottawa, Canada). Following the removal of duplicates, the title and abstracts of remaining citations were screened by two independent reviewers. Inclusion of the citation by at least one reviewer at this stage was necessary in order for the citation to advance to full-text screening. Full-text screening was performed by two independent reviewers. Disagreements regarding study eligibility at this stage were resolved via consensus and/or through consultation with a third, independent reviewer.
2.6 Data extraction and charting
Data extraction was performed by two independent reviewers using a custom piloted form. Data extracted from each study included: (1) study characteristics (such as authors, title, date of publication, study design, and setting); (2) population characteristics (such as size, mean and/or median age, and sex distribution); (3) intervention and comparator characteristics (such as details about the EMIS); (4) timeliness of care outcome(s) (such as mean or median time to receipt of care or discharge); and (5) reported study limitations. A 20% sample of included studies was extracted in duplicate by both reviewers and compared to ensure data integrity. Following extraction form validation, the remaining study data were extracted by a single reviewer.
Study characteristics and key findings of included studies were reported. Where possible, reported outcomes were grouped by similarity and summarized using descriptive statistics.
3 Results
3.1 Search results
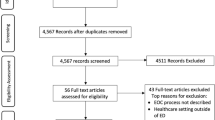
The database search identified a total of 9043 citations. After removal of duplicates, a total of 4386 citations were subject to title and abstract screening (Fig. 1). Of these, 114 studies underwent full-text review and were assessed for eligibility. Twenty-five studies reporting on the effects of an EMIS on the timeliness of patient care in the ED met the eligibility criteria.
3.2 Excluded studies
A list of the 89 studies that were excluded following full-text review is provided in Supplementary Table 1. Overall, studies were excluded for not satisfying the following inclusion criteria: population (23), intervention (27), comparison (10), outcome (20), or study type (9).
3.3 Characteristics of included studies
Key characteristics of included studies are provided in Table 1. The majority of studies were single-centre studies, with six multicentre studies that recruited participants from EDs located in Canada, the United States, Germany, South Korea, and Japan [17,18,19,20,21,22]. Studies were published between 2015 and 2021. Participants included both males and females, with few restrictions according to age or severity of visit.
3.4 Types of studies
Of the 25 studies included in this review, 13 were retrospective studies, seven were pre-post studies, three were randomized controlled trials (RCTs), one was a crossover study, and one was a time series trial.
3.5 Types of interventions and comparisons
Interventions reported by all studies were directly related to the implementation of an EMIS. They included evaluations of a new or updated EMIS [23,24,25,26,27,28], EMIS tools related to disease diagnosis and/or management [17, 19, 20, 22, 29,30,31,32,33,34,35,36], electronic triage tools [37,38,39], result availability alerts [18, 40], health information exchange systems [41], and computerized provider order entry tools [21]. Included studies compared interventions with relevant comparator groups, such as prior versions of an EMIS, absence of an EMIS, pen-and-paper documentation, and/or communication via telephone and fax.
3.6 Outcomes assessed
Reported time-based outcomes varied among included studies and were categorized into six distinct groups: (1) time to provider (n = 3 studies); (2) time to order (n = 4 studies); (3) time to medication (n = 6 studies); (4) time from result to disposition (n = 2 studies); (5) ED length of stay (n = 17 studies); and (6) other time-based outcomes (n = 3 studies) (Table 2). Ten studies reported on multiple time-based outcomes of interest.
3.7 Time to provider
Three studies examined the effects of an EMIS on the time to care provider [21, 26, 37]. Two of the three studies suggest that the implementation of an EMIS increased the length of time that patients waited for a healthcare provider [21, 37]. An emergency severity index tool within the EMIS used during triage of sickle cell disease patients slightly increased both door-to-nurse and door-to-attending time by approximately one minute [37]. Similarly, the implementation of computerized provider order entry increased the wait time for first physician assessment to 83 min in comparison with 78 min with paper-based order entry [21]. In contrast, a single study comparing an EMIS to paper documentation reported a slightly shorter wait time to first physician assessment from 4.2 min pre-EMIS to three min post-EMIS [26].
3.8 Time to order
Four studies evaluated the effects of implementing an EMIS on time to order [17, 18, 24, 31]. These articles evaluated a variety of time intervals and generally found that a reduction of time to order may be attributed to the implementation of an EMIS compared with the absence of an EMIS. Koziatek et al. [18] reported an eight-minute decrease in median order time between pre-implementation and post implementation cohorts when comparing an EMIS with notifications to those without. Another study found that implementing an EMIS containing Wells score criteria decreased time to order a venous duplex ultrasound from 226 min pre-implementation to 165 min post-implementation [31]. Furthermore, time from ED arrival to X-ray order was considerably decreased from 36.5 min to four minutes when searchable chief complaint, best practice advisory, and order sheet features were added to an EMIS for children presenting to the ED with coin-shaped foreign body ingestion [24]. When evaluating time to hydrocortisone order, a decrease of 13.2 min was observed for the critical information note-present group compared with the critical information note-absent group [17]. Lastly, Koziatek et al. [18] reported no meaningful decrease in time from hemoglobin result availability to the administration of a blood transfusion following the implementation of notifications within an EMIS.
3.9 Time to medication
Six studies reported on outcomes related to the timely administration of medication in the ED [17, 30, 34,35,36,37]. Most concluded that a tool embedded within an EMIS decreased time to medication, with improvements ranging from 30.5 to 91 min. For instance, three studies implemented some version of a tool within an EMIS to aid in the early detection and management of sepsis [30, 34, 36]. Collectively, findings demonstrated improved time to antibiotics and time to a bolus of fluid, as well as a greater proportion of patients receiving antibiotics within the target time of 60 min [30, 34, 36]. Another study implemented electronic pediatric asthma guidelines in the EMIS and found that time to steroid administration was reduced from 196 min pre-intervention to 105 min post-intervention [35]. In contrast, two of the six studies did not report any notable improvements in timeliness of patient care [17, 37]. The incorporation of an outpatient critical information note within an EMIS minimally decreased time to the administration of hydrocortisone for pediatric adrenal insufficiency from 121.9 to 112.7 min [17]. Furthermore, the implementation of a triage tool actually led to a slight increase in time to analgesia, from 106.7 to 115.2 min, for sickle cell disease patients presenting to the ED in vaso-occlusive crisis [37].
3.10 Time from result to disposition
Two studies reported on the time from result to disposition [18, 40]. Both concluded that there was a decrease in median time from result availability to physician decision-making owing to the implementation of an alert system within an EMIS. One of these studies reported on four distinct results relating to this primary outcome [18]. When evaluating time from chest X-ray result availability to disposition, there was a 24-min decrease in median time among the push-notification cohort (56 min) compared with the no push-notification cohort (80 min). Similarly, the median time from various laboratory results to physician decision was shortened considerably following the addition of the push-notifications to the EMIS. For example, median time from basic metabolic panel, urinalysis, and respiratory pathogen panel results to disposition decreased by 12, 10, and 43 min, respectively. Moreover, Verma et al. [40] reported that the median time from last troponin result to discharge was decreased from 94.3 to 68.5 min when push notifications for all troponin results were added to an existing EMIS.
3.11 Length of stay
We found that ED length of stay (LOS) was the most commonly examined time-based outcome within included studies. Seventeen distinct studies reported on outcomes related to LOS and yielded highly variable results [17, 19,20,21,22,23, 25,26,27,28,29, 33, 37,38,39,40,41]. The majority of studies reported an increase in ED LOS following the implementation of an updated EMIS. Three of these studies explored the effects of a tool embedded within an EMIS and reported modest increases in LOS ranging from five to 18 min [17, 21, 29]. Two other studies involved the implementation of an emergency severity index triage tool and reported an overall increase in LOS of 12.1 min and 18 min, respectively [37, 39]. However, the latter study also reported decreased triage time and a greater number of high acuity patients seen within recommended timeframes [39]. Following the introduction of a new or updated EMIS, four studies reported an increase in ED LOS ranging from 1.8 min to 35 min [23, 25, 26, 28]. A post-hoc analysis performed by one of these studies showed that LOS decreased by four minutes for patients admitted to hospital [28].
Six studies reported a decrease in ED LOS, ranging from 6.7 to 54 min, following the implementation of an updated EMIS [27, 30, 34,35,36, 38]. One of these studies found that incorporating the Korean triage and acuity scale into an existing EMIS decreased LOS by 54 min [38]. Another study implemented a health information exchange system that permitted providers to access patient records from outside the ED. When compared to telephone and fax-based systems for acquiring records, LOS was decreased by 26.9 min [41]. A third study involving smartphone push-alert notifications for troponin results decreased both total ED LOS and time from triage to discharge decision by 17 min [40]. Similarly, when the HEART (history, electrocardiogram, age, risk factors, and initial troponin) pathway accelerated diagnostic protocol was integrated into an EMIS, LOS was decreased by 24 min alongside improvements in hospitalization rates, mortality, and myocardial infarction [20]. Finally, two studies implemented newly updated EMIS and compared their performance with an original EMIS and paper-based documentation [27, 28]. Findings from Inokuchi et al. [27] demonstrated that the new EMIS with advanced electronic features decreased LOS for all patients by 6.7 min. Additional time savings were observed when groups were stratified according to level of urgency. Tall et al. [28] reported that an EMIS decreased LOS by four minutes for patients who were ultimately admitted to hospital from the ED, when compared with paper-based documentation.
Three of the 17 studies examined ED LOS as either a secondary outcome or balancing measure and, despite positive effects observed for primary outcomes, did not report any difference in LOS following implementation of an electronic tool [19, 22, 33]. For instance, Atabaki et al. [33] and Kharbanda et al. [22] reported a reduction in computed tomography use and associated radiation exposure for pediatric head trauma and appendicitis, respectively, while Delahanty et al. [19] demonstrated that use of an electronic tool was considerably more specific and sensitive for the early detection of sepsis.
3.12 Other timeliness outcomes
Three studies reported on six distinct outcomes that are related to timeliness of care, including time to flagging for sepsis, time to electrocardiogram acquisition, triage interval, disposition-to-admit time, door-to-bed time, and provider-to-disposition time [26, 32, 39]. Lloyd et al. [32] reported that, by integrating an electronic sepsis screening tool within an EMIS, the time to flagging for sepsis resulted in sepsis being identified 68 min earlier compared with a paper-based screening tool. Lavin et al. reported a significant decrease in median time from ED arrival to completion of X-ray (from 59 to 41 min) after implementing an EMIS-based intervention targeting children with coin-shaped foreign body ingestion [24]. Another study found that implementing a stepwise triage tool in an EMIS reduced the triage interval from 5.9 to 2.8 min, and slightly increased time to ECG (electrocardiogram) acquisition from two minutes to 4.5 min [39]. Rupp et al. [26] explored the effects of converting from paper charts to an EMIS system on disposition-to-admit time, door-to-bed time, and provider-to-disposition time. Results were variable, with disposition-to-admit time slightly decreased by 7.2 min, door-to-bed time increased by 3.8 min, and provider-to-disposition time increased by 9.8 min.
4 Discussion
We completed a scoping review to identify recent peer-reviewed studies that described the implementation of an EMIS and examined its effects on timeliness of patient care in the ED. Our primary findings were that the nature of EMIS implemented, as well as the timeliness of patient care outcomes examined, varied considerably among the 25 studies included in this review. There were no clear trends on the impact of the EMIS, as reported findings varied for the same time-based outcome and across examined outcomes. Noteworthy secondary findings include: (1) ED LOS was most commonly examined as a timeliness of care outcome, with moderate changes observed in the overall LOS (ranging from 54 min decrease to 35 min increase); (2) a number of studies examined time to medication delivery, with most reporting decreases in overall time to event; and (3) other important markers of timeliness of care studied within ED settings included time to provider consult, time to intervention request (such as imaging, medication, or procedure), and time from test result to discharge.
The most frequently examined ED time-based outcome was LOS. Reported findings were highly variable among studies. The range of reported findings varied from a 54-min decrease to a 35-min increase in LOS [23, 38]. Additionally, a number of studies found no change in LOS, but reported improvements in other patient care outcomes such as a reduction in unnecessary radiation exposure [19, 22, 33]. These findings are consistent with those reported in systematic reviews that examined patient care efficiencies and outcomes associated with EMIS implementation [15, 42, 43]. Notable improvement in ED LOS of up to 54.5 min with reductions in unnecessary diagnostic tests and/or imaging have previously been reported [15, 42]. Inconsistencies observed within the literature may be attributed to EMRs and related tools being relatively new, with their implementation accelerating over the last decade [15]. As a result, their use in the ED has yet to be thoroughly explored. Nevertheless, improvements in ED LOS may be attributed to EMIS and related tools providing faster access to patient information, reducing time to diagnosis and management, aiding in the proper distribution of resources, and shortening documentation time [15, 27, 38, 41, 42]. Conversely, increased LOS may be associated with system complexities, steep learning curves, and poor system implementation [21, 23, 25, 26, 28, 29, 39].
Time to medication was the second most commonly reported time-based outcome that we observed within our review of the literature. With the exception of a single study, reported findings suggest that an EMIS substantially decreases time to medication administration, with improvements reaching up to 91 min [35, 37]. Interestingly, all studies reporting a shortened time to medication implemented an EMIS tool, such as a push-alert or management guideline, as an intervention within an existing EMIS [17, 30, 34,35,36]. Our findings are consistent with a prior review examining the effects of automated EMIS alerts on ED personnel response to sepsis [13]. Similarly, we observed evidence for improved process-of-care markers, including decreased time to antibiotic delivery [13]. Future studies are required to determine whether such findings apply to the administration of all ED medications and to determine whether additional time-based efficiencies in the delivery of ED medications may be achieved.
Other time-based outcomes identified from our literature review were diverse and included measures such as time to flagging for sepsis and disposition to admit time. Although findings were generally inconsistent across studies, some consistent timeliness of care benefits were observed for time to provider and time to order outcomes, with time savings ranging from eight to 61 min [26, 31]. These findings suggest that the delivery of essential urgent health services may be improved with the adoption of an EMIS. Future studies are necessary to determine whether observed timeliness benefits in the ED extend to all ED settings and patient health outcomes.
Inconsistencies in time-based indicators of patient flow and departmental performance across EMIS implementations make it challenging to generalize regarding the potential benefits of such systems and tools, which may in-turn adversely affect their respective uptake or perceived utility. As such, it is important to comprehensively understand factors that may account for the observed heterogeneity in reported time-based metrics associated with EMIS deployment. It is reasonable to presume that variations in observed effects are attributed to non-standardized EMIS implementation across hospitals, as well as differences in offered training and overall comfort of ED personnel with new health technology. Furthermore, time-varying hospital-level factors that are difficult to control for, such as the number of vacant beds for admissions from the ED and the availability of nurses and other staff, may partially explain the variability in reported findings to date. It is also possible that the lack of standardized time-based outcome definitions and guidelines regarding when and how best to measure the impact of an implemented EMIS render it difficult for hospitals to report similar findings across comparable outcomes, especially for shorter time-based metrics. Future studies should therefore focus on elucidating the underlying factors that may explain observed differences across EMIS deployments, and aim to standardize research parameters specific to EMIS studies.
Our study has a number of strengths. To our knowledge, our study is the first to complete a scoping review of the literature on the impact of the use of an EMIS on time-based outcomes in the ED. We employed a systematic approach in searching for and identifying eligible studies and did not restrict our findings by geography. As such, this work maps the emerging evidence from studies that have evaluated the impact of implementing electronic tools in ED settings on the timeliness of care. Findings from this review may therefore be used to inform future systematic reviews that seek to quantitatively synthesize the impact of these tools on a specific outcome.
A number of limitations should be considered when interpreting our findings. Since the adoption of an EMIS is relatively new within ED settings, we limited our search to articles published after 2014 in English. Therefore, relevant findings published prior to 2015 or those published in another language are not reflected in our review. Furthermore, “Electronic Medical Information System”, “Electronic Medical Record” and “Emergency Department” are broad terms for which there may be many synonyms. To account for this, our searches were developed in consultation with a research librarian and included select synonyms for these terms; though we may have unintentionally missed some relevant records. Notwithstanding these limitations, our study meaningfully adds to the paucity of information on the effects of an EMIS on the timeliness of ED care.
In conclusion, many ED settings have implemented an EMIS in effort to improve timeliness of care outcomes, or plan to do so in the future. The impact of these systems and tools has been evaluated by recent studies, with a particular focus on length of stay. Generally, reported findings are inconsistent and varied within and across time-based outcomes. Despite this, reported findings show promise in improving timeliness of care in the ED, which may ultimately be associated with improved health outcomes for patients. Future studies should explore barriers to the adoption of such systems and tools in the ED, examine the long-term effects of such technologies on important time-based indicators of quality care (such as revisit), and assess provider and patient satisfaction with these ever-changing health information systems.
Data availability
Data sharing is not applicable to this article as no datasets were generated or analysed during the current study. Database search results are available upon request.
References
Chen TL, Wang CC. Multi-objective simulation optimization for medical capacity allocation in emergency department. J Simul. 2016;10(1):50–68.
Health Quality Ontario: health in the North: a report on geography and the health of people in Ontario’s two northern regions. 2017. https://www.publications.gov.on.ca/health-in-the-north-a-report-on-geography-and-the-463health-of-people-in-ontarios-two-northern-regions. Accessed 30 Dec 2022.
Ahsan KB, Alam MR, Morel DG, Karim MA. Emergency department resource optimisation for improved performance: a review. J Ind Eng Int. 2019;15(1):253–66.
Fennelly O, Cunningham C, Grogan L, Cronin H, O’Shea C, Roche M, Lawlor F, O’Hare N. Successfully implementing a national electronic health record: a rapid umbrella review. Int J Med Inform. 2020;144: 104281.
Honavar SG. Electronic medical records—the good, the bad and the ugly. Indian J Ophthalmol. 2020;68(3):417–8.
Ward MJ, Landman AB, Case K, Berthelot J, Pilgrim RL, Pines JM. The effect of electronic health record implementation on community emergency department operational measures of performance. Ann Emerg Med. 2014;63(6):723–30.
Leventhal EL, Schreyer KE. Information management in the emergency department. Emerg Med Clin North Am. 2020;38(3):681–91.
Nguyen Q, Wybrow M, Burstein F, Taylor D, Enticott J. Understanding the impacts of health information systems on patient flow management: a systematic review across several decades of research. PLoS ONE. 2022;17(9): e0274493.
Alexiuk M, Elgubtan H, Tangri N. Clinical decision support tools in the electronic medical record. Kidney Int Rep. 2024;9(1):29–38.
Shin GW, Lee Y, Park T, Cho I, Yun MH, Bahn S, Lee JH. Investigation of usability problems of electronic medical record systems in the emergency department. Work. 2022;72(1):221–38.
Handel DA, Hackman JL. Implementing electronic health records in the emergency department. J Emerg Med. 2010;38(2):257–63.
Daniel GW, Ewen E, Willey VJ, Reese Iv CL, Shirazi F, Malone DC. Efficiency and economic benefits of a payer-based electronic health record in an emergency department. Acad Emerg Med. 2010;17(8):824–33.
Hwang MI, Bond WF, Powell ES. Sepsis alerts in emergency departments: a systematic review of accuracy and quality measure impact. West J Emerg Med. 2020;21(5):1201–10.
Chang F, Gupta N. Progress in electronic medical record adoption in Canada. Can Fam Physician. 2015;61(12):1076–84.
Mullins A, O’Donnell R, Mousa M, Rankin D, Ben-Meir M, Boyd-Skinner C, Skouteris H. Health outcomes and healthcare efficiencies associated with the use of electronic health records in hospital emergency departments: a systematic review. J Med Syst. 2020;44(12):200.
Tricco AC, Lillie E, Zarin W, O’Brien KK, Colquhoun H, Levac D, Moher D, Peters MDJ, Horsley T, Weeks L, et al. PRISMA extension for scoping reviews (PRISMA-ScR): checklist and explanation. Ann Intern Med. 2018;169(7):467–73.
Halpin KL, Paprocki EL, McDonough RJ. Utilizing health information technology to improve the recognition and management of life-threatening adrenal crisis in the pediatric emergency department: medical alert identification in the 21st century. J Pediatr Endocrinol Metab. 2019;32(5):513–8.
Koziatek C, Swartz J, Iturrate E, Levy-Lambert D, Testa P. Decreasing the lag between result availability and decision-making in the emergency department using push notifications. West J Emerg Med. 2019;20(4):666–71.
Delahanty RJ, Alvarez J, Flynn LM, Sherwin RL, Jones SS. Development and evaluation of a machine learning model for the early identification of patients at risk for sepsis. Ann Emerg Med. 2019;73(4):334–44.
Mahler SA, Lenoir KM, Wells BJ, Burke GL, Duncan PW, Case LD, Herrington DM, Diaz-Garelli JF, Futrell WM, Hiestand BC, et al. Safely identifying emergency department patients with acute chest pain for early discharge: HEART pathway accelerated diagnostic protocol. Circulation. 2018;138(22):2456–68.
Gray A, Fernandes CMB, Van Aarsen K, Columbus M. The impact of computerized provider order entry on emergency department flow. CJEM. 2016;18(4):264–9.
Kharbanda AB, Madhok M, Krause E, Vazquez-Benitez G, Kharbanda EO, Mize W, Schmeling D. Implementation of electronic clinical decision support for pediatric appendicitis. Pediatrics. 2016;137(5): e20151745.
Lucas B, Schladitz P, Schirrmeister W, Pliske G, Walcher F, Kulla M, Brammen D. The way from pen and paper to electronic documentation in a German emergency department. BMC Health Serv Res. 2019;19(1):558.
Lavin JM, Wiedermann J, Sals A, Kato K, Brinson D, Nytko A, Katsogridakis Y, Krug S, Ida J. Electronic medical record-based tools aid in timely triage of disc-shaped foreign body ingestions. Laryngoscope. 2018;128(12):2697–701.
Feblowitz J, Takhar SS, Ward MJ, Ribeira R, Landman AB. A custom-developed emergency department provider electronic documentation system reduces operational efficiency. Ann Emerg Med. 2017;70(5):674-682.e671.
Rupp KJ, Ham NJ, Blankenship DE, Payton ME, Murray KA. Pre and post hoc analysis of electronic health record implementation on emergency department metrics. Baylor Univ Med Cent Proc. 2017;30(2):147–50.
Inokuchi R, Sato H, Iwagami M, Komaru Y, Iwai S, Gunshin M, Nakamura K, Shinohara K, Kitsuta Y, Nakajima S, et al. Impact of a new medical record system for emergency departments designed to accelerate clinical documentation: a crossover study. Medicine. 2015;94(26): e856.
Tall JM, Hurd M, Gifford T. Minimal impact of an electronic medical records system. Am J Emerg Med. 2015;33(5):663–6.
Baker AH, Monuteaux MC, Madden K, Capraro AJ, Harper MB, Eisenberg M. Effect of a sepsis screening algorithm on care of children with false-positive sepsis alerts. J Pediatr. 2021;231:193-199.e191.
Tarabichi Y, Cheng A, Bar-Shain D, McCrate BM, Reese LH, Emerman C, Siff J, Wang C, Kaelber DC, Watts B, et al. Improving timeliness of antibiotic administration using a provider and pharmacist facing sepsis early warning system in the emergency department setting: a randomized controlled quality improvement initiative. Crit Care Med. 2021;50(3):418–27.
Clark RM, Weingardt D, Goff JM Jr, Ketteler ER. Effects of a standardized emergency department protocol on after-hours use of venous duplex ultrasound. J Vasc Surg Venous Lymphat Disord. 2019;7(4):501–6.
Lloyd JK, Ahrens EA, Clark D, Dachenhaus T, Nuss KE. Automating a manual sepsis screening tool in a pediatric emergency department. Appl Clin Inform. 2018;9(4):803–8.
Atabaki SM, Jacobs BR, Brown KM, Shahzeidi S, Heard-Garris NJ, Chamberlain MB, Grell RM, Chamberlain JM. Quality improvement in pediatric head trauma with PECARN rules implementation as computerized decision support. Pediatr Qual Saf. 2017;2(3): e019.
Narayanan N, Gross AK, Pintens M, Fee C, MacDougall C. Effect of an electronic medical record alert for severe sepsis among ED patients. Am J Emerg Med. 2016;34(2):185–8.
Walls TA, Hughes NT, Mullan PC, Chamberlain JM, Brown K. Improving pediatric asthma outcomes in a community emergency department. Pediatrics. 2017;139(1): e20160088.
Hayden GE, Tuuri RE, Scott R, Losek JD, Blackshaw AM, Schoenling AJ, Nietert PJ, Hall GA. Triage sepsis alert and sepsis protocol lower times to fluids and antibiotics in the ED. Am J Emerg Med. 2016;34(1):1–9.
Linton E, Souffront K, Gordon L, Loo GT, Genes N, Glassberg J. System level informatics to improve triage practices for sickle cell disease vaso-occlusive crisis: a cluster randomized controlled trial. J Emerg Nurs. 2021;47(5):742–51.
Kwon H, Kim YJ, Jo YH, Lee JH, Lee JH, Kim J, Hwang JE, Jeong J, Choi YJ. The Korean Triage and Acuity Scale: associations with admission, disposition, mortality and length of stay in the emergency department. Int J Qual Health Care. 2019;31(6):449–55.
Villa S, Weber EJ, Polevoi S, Fee C, Maruoka A, Quon T. Decreasing triage time: effects of implementing a step-wise ESI algorithm in an EHR. Int J Qual Health Care. 2018;30(5):375–81.
Verma A, Wang AS, Feldman MJ, Hefferon DA, Kiss A, Lee JS. Push-alert notification of troponin results to physician smartphones reduces the time to discharge emergency department patients: a randomized controlled trial. Ann Emerg Med. 2017;70(3):348–56.
Everson J, Kocher KE, Adler-Milstein J. Health information exchange associated with improved emergency department care through faster accessing of patient information from outside organizations. J Am Med Inform Assoc. 2017;24(e1):e103–10.
Patterson BW, Pulia MS, Ravi S, Hoonakker PLT, SchoofsHundt A, Wiegmann D, Wirkus EJ, Johnson S, Carayon P. Scope and influence of electronic health record-integrated clinical decision support in the emergency department: a systematic review. Ann Emerg Med. 2019;74(2):285–96.
Campanella P, Lovato E, Marone C, Fallacara L, Mancuso A, Ricciardi W, Specchia ML. The impact of electronic health records on healthcare quality: a systematic review and meta-analysis. Eur J Public Health. 2016;26(1):60–4.
Acknowledgements
Not applicable.
Funding
This study was supported by the Northern Ontario Academic Medicine Association (NOAMA) Clinical Innovation Opportunities Fund Award, Project No: C-19-20, the NOSM University Summer Student Research Award Program, and the Northern Ontario Summer Studentship Program.
Author information
Authors and Affiliations
Contributions
DRA and JAGC conceived the study. MLL, ETH, DRA, AC, JAGC, EMM, NF, CB, TSC, SV, LJWL, JJC, and DJK were involved in protocol development and obtaining the ethical waiver for this project. JAGC, NF, MLL, ETH, and EMM completed data analyses. JAGC, NF, MLL, ETH, and EMM wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
JAGC serves as the Principal Health Scientist at TruEffect Inc., a Canadian company that specializes in the provision of professional services for public and private sector clients in the areas of project management, public and population health, epidemiology, statistics, library science, and health risk assessment. NF and DRA serve as the Principal Epidemiologist and Chief Medical Officer, respectively, at TruEffect Inc. TruEffect Inc. has no financial interest in the findings of the present scoping review. All other authors have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Lacasse, M.L., Hendel, E.T., Farhat, N. et al. Electronic medical information systems and timeliness of care in the emergency department: a scoping review. Discov Health Systems 3, 23 (2024). https://doi.org/10.1007/s44250-024-00087-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44250-024-00087-5