Abstract
Background
Immense attention has been given to the outcome of COVID-19 infection. However, comprehensive studies based on large populational cohort with long-term follow-up are still lacking. This study aimed to investigate the risk of various short-term comorbidities (within one month) and long-term sequelae (above one month) after COVID-19 infection.
Methods
In this large prospective cohort study with 14 months follow-up information based on UK biobank, we included 16,776 COVID-19-positive participants and 58,281 COVID-19-negative participants matched for comparison. The risk of each comorbidity and sequela was evaluated by multivariable logistic regression analysis and presented as hazard ratio (HR) and 95% confidence interval (95% CI).
Results
COVID-19-positive individuals had a higher risk of 47 types of comorbidities within one month following COVID-19 infection, especially those who were older, male, overweight/obese, ever-smoked, with more pre-existing comorbidities and hospitalized. About 70.37% of COVID-19 patients with comorbidities had more than one co-occurring comorbidities. Additionally, only 6 high-risk sequelae were observed after one month of COVID-19 infection, and the incidence was relatively low (< 1%).
Conclusion
In addition to long-term sequelae following COVID-19 infection, plenty of comorbidities were observed, especially in patients with older age, male gender, overweight/obese, more pre-existing comorbidities and severe COVID-19, indicating that more attention should be given to these susceptible persons within this period.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Over the past 3 years, corona virus disease 2019 (COVID-19) has spread globally and has become a growing public health concern, posing a serious threat to human survival. As of November 2022, over 637 million cases of COVID-19 have been confirmed globally, of which about 1.04% have died [1]. In the context of widespread infection, the possible systemic comorbidities and sequelae of COVID-19 may cause panic.
It has been previously reported that patients with COVID-19 may experience various adverse and persistent symptoms during hospitalization (comorbidity) and after recovery (sequelae or post-acute COVID-19 syndrome), including dyspnea, pain, respiratory diseases, cardiovascular diseases, digestive diseases, neurological disorders, renal failure, diabetes, musculoskeletal diseases, anxiety and depression, etc. [2,3,4,5,6,7,8,9,10,11,12,13,14,15,16] However, the prevalence and severity of COVID-19-related comorbidities and sequelae remain controversial. Large-scale and long-term cohort studies are still needed to demonstrate the incidence of COVID-19-related comorbidities and sequelae, as well as individual differences in susceptibility, which is of great significance for clinical strategy determination.
The aim of this study is to perform a comprehensive outcome-wide association analysis of COVID-19 comorbidities (short-term) and sequelae (long-term), and individual susceptibilities based on the large prospective UK Biobank (UKB) cohort.
2 Material and Methods
2.1 Study Design and Data Source
This prospective population-based outcome-wide association study was conducted in the UKB, which is a national prospective cohort that recruited over 500,000 participants aged 40–69 years from 22 assessment centers across the United Kingdom between 2006 and 2010. UKB obtained ethical approval from the North West Multicenter Research Ethics Committee [17], and has collected extensive detailed baseline and long-term follow-up data, including real-time updated extensive clinical records. SARS-CoV-2 testing results were obtained from Public Health England (PHE), Public Health Scotland (PHS) and Secure Anonymized Information Linkage (SAIL). Hospitalization information of participants from England, Scotland, and Wales were acquired from Hospital Episode Statistics, the Scottish Morbidity Record, and the Patient Episode Database for Wales, respectively. Mortality data were extracted from the National Health Service (NHS) Digital and NHS Central Register.
2.2 Participants and Exposure
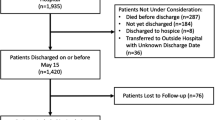
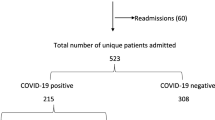
A total of 106,760 UKB participants who were tested for SARS-CoV-2 during March 2020 and February 2021 were included. Among the 17,832 participants with at least one positive SARS-CoV-2 test (COVID-19-positve participants), those who were tested with positive result after 2021-2-23 (had limited follow-up time, n = 1041), or withdrew during follow-up (n = 15) were excluded. We further defined the severity of COVID-19 according to the presence of death or hospitalization due to COVID-19. For these 88,928 participants without any positive SARS-CoV-2 test result (COVID-19-negative participants), we excluded those who were reported to die or hospitalize due to COVID-19 (n = 303), died before the pandemic of COVID-19 (2020-1-31, n = 1,095) or withdrew during follow-up (n = 14). Then for each COVID-19-positive participant, we matched up to 4 COVID-19-negative participants according to birth year, sex, and Townsend deprivation index (TDI) by propensity scores. Finally, we excluded COVID-19-negative participants who died before the SARS-CoV-2 test date of their matched COVID-19-positive counterparts. These inclusion and exclusion criteria, and matching process resulted in a final cohort of 16,776 COVID-19-positive participants and 58,281 COVID-19-negative participants (Supplementary Figs. 1–2).
2.3 Outcome and Covariates
Comorbidities and sequelae, defined using 3-digit ICD-10 codes (International Classification of Diseases, 10th revision, excluding codes used for special purposes, injury, poisoning and certain other consequences of external causes, factors influencing health status and contact with health services, as well as external causes of morbidity and mortality) from medical records, referred to newly onset illnesses < 1 month and ≥ 1 month after the diagnosis of COVID-19, respectively [18,19,20]. We then reclassified the eligible (hazard ratio [HR] > 1, p < 0.05, and case number > 10) diseases into more broadly defined comorbidities and sequelae (Supplementary Tables 1–2). In the case of multiple identical records for the same individual, the date of diagnosis was derived from the earliest record. Ethnicity, body mass index (BMI), smoking status, and Charlson comorbidity index (CCI, without age calculation, Supplementary Table 3) were included as covariates [21,22,23]. In subgroup analysis, we also defined another covariate, current age, as the age on January 31st, 2020.
2.4 Follow-Up
The start date of follow-up was the test date for COVID-19-positive participants. For COVID-19-negative participants, it was the same as that for their matched counterparts. Follow-up ended on the day of (1) specific disease diagnosis, (2) death, or (3) end of follow-up (March 31st, 2021), whichever came first. The longest follow-up duration was 14 months.
2.5 Statistics Analyses
Student’s t-tests and Chi-square tests were performed as appropriate to assess the differences among groups. Univariable conditional Cox proportional hazards models were performed to identify eligible diseases for comorbidity and sequela reclassification, and outcome-wide association analyses for the risk of COVID-19-related comorbidities and sequelae were conducted using multivariable conditional Cox proportional hazards models adjusting for ethnicity, BMI, smoking status, and CCI [24]. In the specific analysis of each disease, participants diagnosed with corresponding disease before COVID-19 were excluded. In the analysis of death in COVID-19-positive participants, we also excluded individuals who died on the day of diagnosis. To explore the impact of severity of COVID-19 on COVID-19-related sequelae, we additionally adjusted for age, sex, and TDI. In subgroup analyses, participants were stratified by current age (< 65 and ≥ 65 years), sex (female and male), BMI (< 25 kg/m2 and ≥ 25 kg/m2), smoking status (ever-smoker and never-smoker), and CCI (≤ 1 and ≥ 2).
All analyses were performed using R software (version 3.6.3, https://www.r-project.org/), and a two-tailed p < 0.05 was considered statistically significant.
3 Results
3.1 Participant Characteristics
A total of 16,776 COVID-19-positive participants were included and 58,281 COVID-19-negative participants were matched for comparison (1:4). A total of 2670 participants were hospitalized due to COVID-19, and 1169 participants died of COVID-19. Compared with COVID-19-negative participants, COVID-19-positive participants were younger (64.6 vs. 65.8, p < 0.001), more deprived (TDI: − 0.7 ± 3.3 vs. − 0.9 ± 3.3) and more overweight/obese (normal BMI: 25.5% vs 30.1%, p < 0.001, Supplementary Table 4).
3.2 Descriptive Analysis of COVID-19-Related Comorbidity Burdens
We observed that compared with COVID-19-negative participants, 121 types of comorbidities showed significantly higher incidences in participants with COVID-19 (HR > 1 and p < 0.05, Supplementary Table 5). In the outcome-wide association analysis adjusting for ethnicity, BMI, CCI and smoking status, 47 out of the 51 reclassified comorbidities showed higher risks in COVID-19-positive participants (HR > 1 and p < 0.05, Table 1). Representative comorbidities included lower respiratory infection (incidence: 5.93%, HR = 48.32, p < 0.001), respiratory failure (incidence: 2.02%, HR = 103.02, p < 0.001), electrolyte imbalance (incidence: 2.00%, HR = 9.41, p < 0.001), renal failure (incidence: 1.51%, HR = 8.8, p < 0.001), hypertension (incidence: 1.25%, HR = 2.49, p < 0.001) and other heart disease (incidence: 1.05%, HR = 3.92, p < 0.001, Table 1). However, the incidence rates of the other remaining 40 types of COVID-19-related comorbidities were less than 1%. Besides, among all COVID-19-positive participants who developed COVID-19-related comorbidities, 70.37% of them were reported to have two or more co-occurring comorbidities, and the most common form of co-occurrence was respiratory failure plus lower respiratory infection (Fig. 1 and Supplementary Fig. 3).
In addition, the mortality of COVID-19-positive participants was significantly higher than COVID-19-negative participants regardless of COVID-19 severity (COVID-19-positive vs. COVID-19-negative: 7.09% vs. 0.91%, HR = 10.6, p < 0.001; mild COVID-19-positive vs. COVID-19-negative: 1.47% vs. 0.80%, HR = 2.11, p < 0.001; severe COVID-19-positive vs. COVID-19-negative: 37.36% vs. 1.43%, HR = 44.15, p < 0.001, Supplementary Table 6).
3.3 Burden of Comorbidities by COVID-19 Severity
Compared with mild COVID-19 patients (non-hospitalized), severe COVID-19 patients (hospitalized) were more likely to be male, older, deprived, obese, ever-smokers and had higher CCI scores (Supplementary Table 7). As expected, they had higher comorbidity burdens (Supplementary Table 8). Compared with COVID-19-negative participants, severe COVID-19 patients had significantly higher risks of having 48/51 types of COVID-19-related comorbidities, among which the incidence rates of lower respiratory infection (61.68%, HR = 12,351.54, p < 0.001), electrolyte imbalance (13.88%, HR = 54.76, p < 0.001), respiratory failure (13.83%, HR = 1394.47, p < 0.001), hypertension (11.04%, HR = 32.55, p < 0.001) and renal failure (10.86%, HR = 81.82, p < 0.001) were relatively higher. Notably, only severe COVID-19 patients were at an increased risk of hearing loss (incidence: 0.59%, HR = 7.57, p = 0.001). In contrast, mild COVID-19 patients only had 11/51 types of comorbidities with incidence rates less than 0.5%: septicaemia (HR = 2.89, p = 0.020), vitamin deficiency (HR = 2.14, p = 0.043), delirium (HR = 3.66, p < 0.001), lower respiratory infection (HR = 2.41, p < 0.001), respiratory failure (HR = 3.32, p = 0.031), rash and dermatitis (HR = 3.31, p = 0.031), decubitus ulcer (HR = 34.6, p = 0.004), cough (HR = 5.55, p = 0.001), dyspnea and asphyxia (HR = 2.36, p = 0.013), disorientation (HR = 2.18, p = 0.033) and emotional state symptoms and signs (HR = 4.68, p = 0.020, Table 2, and Supplementary Fig. 4). Besides, severe COVID-19 patients had more co-occurrence comorbidities, with lower respiratory infection plus respiratory failure being the most common form. On the other hand, the incidence of co-occurring comorbidities in mild COVID-19 patients was relatively lower, and renal failure plus electrolyte imbalance was the commonest (Fig. 1B ~ C and Supplementary Fig. 3B ~ C).
3.4 Subgroup Analyses of COVID-19-Related Comorbidities by Age, Sex, BMI, Smoking Status and CCI
To understand whether the burden of COVID-19-related comorbidities differed among various populations, we further carried out subgroup analyses stratified by current age, sex, BMI, smoking status and CCI, respectively (Fig. 2).
Differences in adjusted hazards ratio of clinical comorbidities among COVID-19-positive participants compared with COVID-19-negative participants stratified by age, sex, BMI, smoking status, and CCI, respectively. Note: Only the top 20 comorbidities in terms of incidence were shown. Analyses were adjusted for ethnicity, BMI, smoking status and CCI as appropriate. COVID-19 corona virus disease 2019, BMI body mass index, CCI Charlson comorbidity index
In terms of subgroup analysis for current age, older COVID-19-positive participants (> 65 years) were at a significantly higher risk of 48/51 clinical comorbidities, whereas only 26/51 comorbidities were significant in younger COVID-19 patients (Table 3). Specifically, among younger participants, COVID-19-positive individuals had a higher risk of respiratory failure (HR = 99.05, p < 0.001), vitamin deficiency (HR = 66.51, p = 0.004), delirium (HR = 51.65, p = 0.006), septicaemia (HR = 50.86, p = 0.026), etc. However, the incidences of these comorbidities were less than 1%, except for respiratory failure (incidence: 1.23%). In contrast, 16 out of the 48 comorbidities in elderly COVID-19-positive patients had an incidence greater than 1%, e.g., lower respiratory infection (9.22%), electrolyte imbalance (3.72%), respiratory failure (3.00%), renal failure (2.79%), etc.
Females had higher risks of 36/51 types of COVID-19-related comorbidities, whereas males were at higher risks of having 37/51 types of COVID-19-related comorbidities (Supplementary Table 9). Notably, blood cell disease (incidence: 0.65%, HR = 5.42, p < 0.001), obesity (incidence: 0.61%, HR = 2.34, p = 0.028), hypertension (incidence: 1.95%, HR = 2.77, p < 0.001), cerebrovascular diseases (incidence: 0.13%, HR = 4.74, p = 0.027), vascular disease (incidence: 0.20%, HR = 3.53, p = 0.042), COPD/emphysema (incidence: 0.64%, HR = 1732.86, p = 0.030) and rash and dermatitis (incidence: 0.31%, HR = 33.8, p = 0.006) were observed as significant comorbidities only in males but not in females.
In addition, individuals who were overweight/obese, ever-smoker, or with more comorbidities at baseline (CCI score ≥ 2) had more COVID-19-related comorbidities than their counterparts, respectively (Supplementary Tables 10–12).
3.5 Descriptive Analysis of COVID-19-Related Sequelae Burden
We observed that 14 types of sequelae were positively associated with the infection of COVID-19 (HR > 1 and p < 0.05, Supplementary Table 13). In the outcome-wide association analysis adjusting for ethnicity, BMI, CCI and smoking status, only 6 out of the 11 reclassified more broadly defined sequelae were observed in COVID-19-positive participants, including lower respiratory infection (incidence: 0.10%, HR = 8.33, p < 0.001), immobility (incidence: 0.10%, HR = 4.82, p = 0.001), interstitial pulmonary disease (incidence: 0.12%, HR = 2.4, p = 0.018), fecal abnormalities (incidence: 0.13%, HR = 2.24, p = 0.011), decubitus ulcer (incidence: 0.17%, HR = 1.96, p = 0.020) and urinary incontinence (incidence: 0.21%, HR = 1.81, p = 0.010, Supplementary Table 14), etc. The incidence rates of all these COVID-19-related sequelae were less than 1%.
4 Discussion
In this prospective cohort study, we conducted comprehensive outcome-wide association analyses to identify COVID-19-related comorbidities and sequelae in a large population. Overall, 47 types of COVID-19 related comorbidities that occurred within one month after COVID-19 infection were identified, by incidence from high to low, including lower respiratory infection, respiratory failure, electrolyte imbalance, renal failure, hypertension and other heart disease, etc. We also observed that COVID-19-related comorbidities tended to co-occur, especially in severe COVID-19 patients. Besides, older age, male gender, obese/overweight, smoking history, higher CCI scores and severe COVID-19 were risk factors for experiencing more types of comorbidities. Meanwhile, we identified 6 types of COVID-19 related sequelae that began to appear after one month following COVID-19 infection, such as lower respiratory infection, immobility, interstitial pulmonary disease, fecal abnormalities, decubitus ulcer and urinary incontinence. Nonetheless, the incidence rates of these COVID-19-related sequelae were all relatively low (< 1%). Therefore, the public should be urged not to worry too much about these low-morbidities and low-seriousness sequelae.
Previous studies showed that COVID-19 patients had a higher risk of having sequelae, such as myalgia, sexual dysfunction, hearing loss and disturbances of smell and taste [25,26,27,28], however, these sequelae were not prominent in our results, as we only observed 6 types of COVID-19-related sequelae with low incidences. However, we observed plenty of comorbidities involving multiple organs after COVID-19 infection, such as respiratory, neurological, circulatory and urinary systems. Besides, the majority of COVID-19 patients developing comorbidities showed more than one comorbidity. Thus, comorbidity was a more prominent issue for COVID-19 patients.
It has been established that SARS-CoV-2 can upregulate the expression of the type 2 angiotensin converting enzyme (ACE-2), and can bind ACE-2 receptors on the surface of the host cells for cell entrance in many organs, which may explain the comorbidities we observed in COVID-19 patients, such as hypertension, diabetes and COPD [29,30,31]. COVID-19 is associated with a high inflammatory burden and SARS-CoV-2 can affect the myocardium and cardiac biomarker level and lead to myocarditis and heart failure [32,33,34,35]. Moreover, interleukin-mediated modulation of phosphokinases and phosphatases, NOD-like receptor thermal protein domain associated protein 3 (NLRP3) inflammasome-mediated inflammation and pathological accumulation of amyloid-β are associated with COVID-19 related neurological disorder. Several studies have found abnormalities in brain structures in COVID-19 patients, such as reduced grey matter thickness, tissue-contrast in the cortex and gyrus, and reduced overall brain size [36,37,38,39]. In addition, the activation of the RAS, hemodynamic changes and secondary infection of the urinary tract following COVID-19 infection are associated with the comorbidities and sequelae of urinary system in COVID-19 patients [40,41,42]. Hearing loss was found in the comorbidities of severe COVID-19 patients, which may be associated with brainstem dysfunction resulting from neuroinflammatory mechanisms. Cytokine storm after COVID-19 infection could damage the auditory glial cells and might play a role in hearing loss [43].
We observed that participants with advanced age, male sex, smoking status or excessive obesity were at higher risks of COVID-19-related comorbidities. Old and obese participants were usually characterized by more pre-existing comorbidities, weaker immune defense, and higher levels of proinflammatory cytokines, which may contribute to their more comorbidities [44, 45]. Besides, the discrepancy of COVID-19 related outcomes between male and female participants could be attributed to the differences in sex hormones, expression levels of ACE2 and Transmembrane protease serine 2 (TMPRSS2), and lifestyles [46]. Moreover, smoking is associated with a higher expression level of ACE2 in airway epithelial cells, which may induce the occurrence of COVID-19 related comorbidities and sequelae [47]. These populations should be paid special attention as they were more susceptible to COVID-19-related comorbidities.
Although the advent of our study provided new insight into the comorbidities and sequelae of COVID-19 patients, a few limitations still existed. First, due to the data limitation, we defined the severity of COVID-19 according to the hospitalization status or death cause, which may lead to partial bias but was acceptable [48]. Second, due to the limited data on COVID-19 medications, we could not assess the effect of COVID-19 medications on COVID-19-related outcomes. Third, our observations were mainly of comorbidities and sequelae associated with the SARS-CoV-2 Alpha variant, which was the main strain in the UK between January 31, 2020 and March 31, 2021, but not the Delta and Omicron variants of SARS-CoV-2, which began to emerged and spread in the UK from March and October 2021, respectively. The SARS-CoV-2 Alpha variant was considered relatively more pathogenic but less infectious than Delta and Omicron variant, therefore, the incidence and severity of sequelae of Delta and Omicron variants might be lower than, also be different from, those of Alpha variants [49,50,51,52]. Unfortunately, to date, we are unable to obtain the lagging comorbidities and sequelae data of Delta and Omicron variant for analysis.
In conclusion, 47 types of high-risk comorbidities might occur within one month after COVID-19 infection, especially in patients with older age, overweight/obese, more pre-existing comorbidities and severe COVID-19. And only 6 types of COVID-19-related sequelae appeared after one month following COVID-19 infection, indicating that more attention and health care should be given to these susceptible populations after COVID-19 infection.
Availability of Data and Materials
UKB data are available in a public, open access repository. This research has been conducted using the UKB Resource under Application Number 80787 and 69718. The UKB data are available on application to the UKB (http://www.ukbiobank.ac.uk/).
Abbreviations
- COVID-19:
-
Corona virus disease 2019
- HR:
-
Hazard ratio
- 95% CI:
-
95% confidence interval
- UKB:
-
UK Biobank
- PHE:
-
Public Health England
- PHS:
-
Public Health Scotland
- SAIL:
-
Secure Anonymized Information Linkage
- NHS:
-
National Health Service
- TDI:
-
Townsend deprivation index
- ICD:
-
International Classification of Diseases
- BMI:
-
Body mass index
- CCI:
-
Charlson comorbidity index
- COPD:
-
Chronic obstructive pulmonary disease
- ACE-2:
-
Type 2 angiotensin converting enzyme
- NLRP3:
-
NOD-like receptor thermal protein domain associated protein 3
- TMPRSS2:
-
Transmembrane protease serine 2
- SARS-CoV-2:
-
Severe acute respiratory syndrome coronavirus 2
References
Coronavirus disease (COVID-19) weekly epidemiological updates and monthly operational updates. Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/situation-reports. Accessed 7 Dec 2022.
Lee S-H, Yeoh ZX, Sachlin ISA, et al. Self-reported symptom study of COVID-19 chemosensory dysfunction in Malaysia. Sci Rep. 2022;12(1):2111. https://doi.org/10.1038/s41598-022-06029-6.
Lassen MCH, Skaarup KG, Lind JN, et al. Recovery of cardiac function following COVID-19—ECHOVID-19: a prospective longitudinal cohort study. Eur J Heart Fail. 2021;23(11):1903–12. https://doi.org/10.1002/ejhf.2347.
Robey RC, Kemp K, Hayton P, et al. Pulmonary sequelae at 4 months after COVID-19 infection: a single-centre experience of a COVID follow-up service. Adv Ther. 2021;38(8):4505–19. https://doi.org/10.1007/s12325-021-01833-4.
Prabhu M, Cagino K, Matthews KC, et al. Pregnancy and postpartum outcomes in a universally tested population for SARS-CoV-2 in New York City: a prospective cohort study. BJOG. 2020;127(12):1548–56. https://doi.org/10.1111/1471-0528.16403.
Mattioli F, Stampatori C, Righetti F, et al. Neurological and cognitive sequelae of Covid-19: a four month follow-up. J Neurol. 2021;268(12):4422–8. https://doi.org/10.1007/s00415-021-10579-6.
Méndez R, Balanzá-Martínez V, Luperdi SC, et al. Long-term neuropsychiatric outcomes in COVID-19 survivors: a 1-year longitudinal study. J Intern Med. 2022;291(2):247–51. https://doi.org/10.1111/joim.13389.
Darcis G, Bouquegneau A, Maes N, et al. Long-term clinical follow-up of patients suffering from moderate-to-severe COVID-19 infection: a monocentric prospective observational cohort study. Int J Infect Dis. 2021;109:209–16. https://doi.org/10.1016/j.ijid.2021.07.016.
Karaarslan F, Güneri FD, Kardeş S. Long COVID: rheumatologic/musculoskeletal symptoms in hospitalized COVID-19 survivors at 3 and 6 months. Clin Rheumatol. 2022;41(1):289–96. https://doi.org/10.1007/s10067-021-05942-x.
Noviello D, Costantino A, Muscatello A, et al. Functional gastrointestinal and somatoform symptoms five months after SARS-CoV-2 infection: a controlled cohort study. Neurogastroenterol Motil. 2022;34(2): e14187. https://doi.org/10.1111/nmo.14187.
Nersesjan V, Amiri M, Lebech A-M, et al. Central and peripheral nervous system complications of COVID-19: a prospective tertiary center cohort with 3-month follow-up. J Neurol. 2021;268(9):3086–104. https://doi.org/10.1007/s00415-020-10380-x.
Labarca G, Henríquez-Beltrán M, Lastra J, et al. Analysis of clinical symptoms, radiological changes and pulmonary function data 4 months after COVID-19. Clin Respir J. 2021. https://doi.org/10.1111/crj.13403.
Ko JY, DeSisto CL, Simeone RM, et al. Adverse pregnancy outcomes, maternal complications, and severe illness among US delivery hospitalizations with and without a coronavirus disease 2019 (COVID-19) diagnosis. Clin Infect Dis. 2021;73(Suppl 1):S24–31. https://doi.org/10.1093/cid/ciab344.
Wu X, Liu X, Zhou Y, et al. 3-month, 6-month, 9-month, and 12-month respiratory outcomes in patients following COVID-19-related hospitalisation: a prospective study. Lancet Respir Med. 2021;9(7):747–54. https://doi.org/10.1016/S2213-2600(21)00174-0.
Huang C, Huang L, Wang Y, et al. 6-month consequences of COVID-19 in patients discharged from hospital: a cohort study. Lancet. 2021;397(10270):220–32. https://doi.org/10.1016/s0140-6736(20)32656-8[publishedOnlineFirst:2021/01/12].
Huang L, Yao Q, Gu X, et al. 1-year outcomes in hospital survivors with COVID-19: a longitudinal cohort study. Lancet (London, England). 2021;398(10302):747–58. https://doi.org/10.1016/S0140-6736(21)01755-4.
Sudlow C, Gallacher J, Allen N, et al. UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med. 2015;12(3): e1001779. https://doi.org/10.1371/journal.pmed.1001779.
Fernández-de-Las-Peñas C, Palacios-Ceña D, Gómez-Mayordomo V, et al. Defining post-COVID symptoms (post-acute COVID, long COVID, persistent post-COVID): an integrative classification. Int J Environ Res Public Health. 2021. https://doi.org/10.3390/ijerph18052621.
Nalbandian A, Sehgal K, Gupta A, et al. Post-acute COVID-19 syndrome. Nat Med. 2021;27(4):601–15. https://doi.org/10.1038/s41591-021-01283-z.
Daugherty SE, Guo Y, Heath K, et al. Risk of clinical sequelae after the acute phase of SARS-CoV-2 infection: retrospective cohort study. BMJ (Clin Res Ed). 2021;373: n1098. https://doi.org/10.1136/bmj.n1098.
Charlson ME, Pompei P, Ales KL, et al. A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis. 1987;40(5):373–83.
Kubo Y, Tanaka K, Yamasaki M, et al. Influences of the Charlson Comorbidity Index and nutrition status on prognosis after esophageal cancer surgery. Ann Surg Oncol. 2021;28(12):7173–82. https://doi.org/10.1245/s10434-021-09779-1.
Shebeshi DS, Dolja-Gore X, Byles J. Charlson Comorbidity Index as a predictor of repeated hospital admission and mortality among older women diagnosed with cardiovascular disease. Aging Clin Exp Res. 2021;33(10):2873–8. https://doi.org/10.1007/s40520-021-01805-2.
Han X, Hou C, Yang H, et al. Disease trajectories and mortality among individuals diagnosed with depression: a community-based cohort study in UK Biobank. Mol Psychiatry. 2021;26(11):6736–46. https://doi.org/10.1038/s41380-021-01170-6.
Zhang X, Wang F, Shen Y, et al. Symptoms and health outcomes among survivors of COVID-19 infection 1 year after discharge from hospitals in Wuhan, China. JAMA Netw Open. 2021;4(9): e2127403. https://doi.org/10.1001/jamanetworkopen.2021.27403.
Hossain MA, Hossain KMA, Saunders K, et al. Prevalence of long COVID symptoms in Bangladesh: a prospective Inception Cohort Study of COVID-19 survivors. BMJ Glob Health. 2021. https://doi.org/10.1136/bmjgh-2021-006838.
Dasgupta A, Kalhan A, Kalra S. Long term complications and rehabilitation of COVID-19 patients. J Pak Med Assoc. 2020;70(Suppl 35):S131–5. https://doi.org/10.5455/JPMA.32.
Post-COVID-19 global health strategies: the need for an interdisciplinary approach. Aging Clin Exp Res. 2020;32(8):1613–20. https://doi.org/10.1007/s40520-020-01616-x.
Maddaloni E, Buzzetti R. Covid-19 and diabetes mellitus: unveiling the interaction of two pandemics. Diabetes Metab Res Rev. 2020;36(7): e33213321. https://doi.org/10.1002/dmrr.3321.
Qiu H, Tong Z, Ma P, et al. Intensive care during the coronavirus epidemic. Intensive Care Med. 2020;46(4):576–8. https://doi.org/10.1007/s00134-020-05966-y.
Wan Y, Shang J, Graham R, et al. Receptor recognition by the novel coronavirus from Wuhan: an analysis based on decade-long structural studies of SARS coronavirus. J Virol. 2020. https://doi.org/10.1128/JVI.00127-20.
Akhmerov A, Marbán E. COVID-19 and the heart. Circ Res. 2020;126(10):1443–55. https://doi.org/10.1161/CIRCRESAHA.120.317055.
Chang W-T, Toh HS, Liao C-T, et al. Cardiac involvement of COVID-19: a comprehensive review. Am J Med Sci. 2021;361(1):14–22. https://doi.org/10.1016/j.amjms.2020.10.002.
Liu PP, Blet A, Smyth D, et al. The science underlying COVID-19: implications for the cardiovascular system. Circulation. 2020;142(1):68–78. https://doi.org/10.1161/CIRCULATIONAHA.120.047549.
Madjid M, Safavi-Naeini P, Solomon SD, et al. Potential effects of coronaviruses on the cardiovascular system: a review. JAMA Cardiol. 2020;5(7):831–40. https://doi.org/10.1001/jamacardio.2020.1286.
Aghagoli G, Gallo Marin B, Katchur NJ, et al. Neurological involvement in COVID-19 and potential mechanisms: a review. Neurocrit Care. 2021;34(3):1062–71. https://doi.org/10.1007/s12028-020-01049-4.
Douaud G, Lee S, Alfaro-Almagro F, et al. SARS-CoV-2 is associated with changes in brain structure in UK Biobank. Nature. 2022. https://doi.org/10.1038/s41586-022-04569-5.
Heneka MT, Golenbock D, Latz E, et al. Immediate and long-term consequences of COVID-19 infections for the development of neurological disease. Alzheimers Res Ther. 2020;12(1):69. https://doi.org/10.1186/s13195-020-00640-3.
Hingorani KS, Bhadola S, Cervantes-Arslanian AM. COVID-19 and the brain. Trends Cardiovasc Med. 2022. https://doi.org/10.1016/j.tcm.2022.04.004.
Cheng Y, Luo R, Wang K, et al. Kidney disease is associated with in-hospital death of patients with COVID-19. Kidney Int. 2020;97(5):829–38. https://doi.org/10.1016/j.kint.2020.03.005.
Iwasaki M, Saito J, Zhao H, et al. Inflammation triggered by SARS-CoV-2 and ACE2 augment drives multiple organ failure of severe COVID-19: molecular mechanisms and implications. Inflammation. 2021;44(1):13–34. https://doi.org/10.1007/s10753-020-01337-3.
Sharma P, Uppal NN, Wanchoo R, et al. COVID-19-associated kidney injury: a case series of kidney biopsy findings. J Am Soc Nephrol. 2020;31(9):1948–58. https://doi.org/10.1681/ASN.2020050699.
Jafari Z, Kolb BE, Mohajerani MH. Hearing loss, tinnitus, and dizziness in COVID-19: a systematic review and meta-analysis. Can J Neurol Sci. 2022;49(2):184–95. https://doi.org/10.1017/cjn.2021.63.
Gao Y-D, Ding M, Dong X, et al. Risk factors for severe and critically ill COVID-19 patients: a review. Allergy. 2021;76(2):428–55. https://doi.org/10.1111/all.14657.
Sattar N, McInnes IB, McMurray JJV. Obesity is a risk factor for severe COVID-19 infection: multiple potential mechanisms. Circulation. 2020;142(1):4–6. https://doi.org/10.1161/CIRCULATIONAHA.120.047659.
Wolff D, Nee S, Hickey NS, et al. Risk factors for Covid-19 severity and fatality: a structured literature review. Infection. 2021;49(1):15–28. https://doi.org/10.1007/s15010-020-01509-1.
Radzikowska U, Ding M, Tan G, et al. Distribution of ACE2, CD147, CD26, and other SARS-CoV-2 associated molecules in tissues and immune cells in health and in asthma, COPD, obesity, hypertension, and COVID-19 risk factors. Allergy. 2020;75(11):2829–45. https://doi.org/10.1111/all.14429.
Ren J, Pang W, Luo Y, et al. Impact of allergic rhinitis and asthma on COVID-19 infection, hospitalization, and mortality. J Allergy Clin Immunol Pract. 2022;10(1):124–33. https://doi.org/10.1016/j.jaip.2021.10.049.
Dougherty K, Mannell M, Naqvi O, et al. SARS-CoV-2 B.1.617.2 (Delta) variant COVID-19 outbreak associated with a gymnastics facility—Oklahoma, April-May 2021. MMWR Morb Mortal Wkly Rep. 2021;70(28):1004–7. https://doi.org/10.15585/mmwr.mm7028e2.
Karim SSA, Karim QA. Omicron SARS-CoV-2 variant: a new chapter in the COVID-19 pandemic. Lancet (London, England). 2021;398(10317):2126–8. https://doi.org/10.1016/S0140-6736(21)02758-6.
Sheikh A, McMenamin J, Taylor B, et al. SARS-CoV-2 Delta VOC in Scotland: demographics, risk of hospital admission, and vaccine effectiveness. Lancet (London, England). 2021;397(10293):2461–2. https://doi.org/10.1016/S0140-6736(21)01358-1.
Wolter N, Jassat W, Walaza S, et al. Early assessment of the clinical severity of the SARS-CoV-2 omicron variant in South Africa: a data linkage study. Lancet (London, England). 2022;399(10323):437–46. https://doi.org/10.1016/S0140-6736(22)00017-4.
Acknowledgements
We thank all participants in the UK biobank study and the members of the survey teams, as well as the project development and management teams.
Funding
This work was supported by West China Hospital, Sichuan University (ZY, Grant #2019HXFH003, Grant #ZYJC21027). The funders had no role in considering the study design or in the collection, analysis, interpretation of data, writing of the report, or decision to submit the article for publication.
Author information
Authors and Affiliations
Contributions
YYZ, JHL, and LF contributed equally to this work and are joint first authors. WX, YZ and JJR contributed equally to this work and are joint senior authors. YYZ, JHL, LF, YXL, WX, YZ and JJR designed the study. YXL conducted the statistical analysis and YYZ, JHL, LF, YXL, WX, YZ and JJR interpreted the results and wrote the first draft. All other authors had critically revised the manuscript. WX, YZ and JJR are the guarantors of the manuscript and accepts full responsibility for the work and/or the conduct of the study, had access to the data, and controlled the decision to publish. The corresponding author attests that all listed authors meet authorship criteria and that no others meeting the criteria have been omitted.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval and consent to participate
This study was performed under generic ethical approval obtained by UK Biobank from the National Health Service National Research Ethics Service (approval letter ref 11/NW/0382, 17 June 2011). Informed consent was obtained from all individual participants included in the UK Biobank study.
Consent for publication
The authors affirm that human research participants included in the UK Biobank study provided informed consent for publication.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Zhang, Y., Li, J., Feng, L. et al. A Population-Based Outcome-Wide Association Study of the Comorbidities and Sequelae Following COVID-19 Infection. J Epidemiol Glob Health 13, 870–885 (2023). https://doi.org/10.1007/s44197-023-00161-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s44197-023-00161-w