Abstract
Introduction
Avoidable mortality is widely used by public health researchers to measure population health, and many related methodologies have been proposed for doing so. This scoping review presents a comprehensive view of global peer-reviewed and grey literature exploring the association between socioeconomic status (SES) and avoidable mortality.
Methods
We searched Ovid Medline, Scopus, and Web of Science to find articles that investigated SES inequalities in avoidable mortality. We limited our review to articles in English published between 2000 and 2020. For grey literature, we searched leading global and Canadian health information websites. We extracted data on different study characteristics, avoidable mortality definition, SES indicator, method of analysis of the association between avoidable mortality and SES, and main findings of the studies.
Results
We identified 34 articles to review, including 29 scientific papers and 5 grey literature documents. The findings of the selected articles consistently indicate a negative association between SES and avoidable mortality rates. Studies have not all used the same definitions of avoidable mortality or SES nor operationalized them in the same way.
Conclusion
Our review highlights the absence of a globally standard definition in avoidable mortality health equity research. Additional work to establish a standardized definition is crucial for supporting global comparability.
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Avoid common mistakes on your manuscript.
1 Introduction
Addressing health inequities requires improved measurement, monitoring, and reporting of population health status and its association with social determinants of health [1,2,3]. Avoidable mortality, a subset of premature mortality, is widely used by public health researchers to measure population health, and many related methodologies have been proposed for doing so. This scoping review presents a comprehensive view of global peer-reviewed and grey literature exploring the association between socioeconomic status (SES) and avoidable mortality. The studies tend to vary not only in how they define avoidable mortality but also in how they measure SES and the association between them. We also report on how these studies do or do not standardize their results for age and sex and encapsulate their main findings with respect to SES inequalities. Our aim is to facilitate a more widespread and in-depth analysis of inequities in avoidable mortality by consolidating these resources in one location.
Avoidable mortality is a relatively new concept, with corresponding methodologies still under refinement. In 1976, the Working Group on Preventable and Manageable Diseases, chaired by Rutstein, introduced the new concept of “unnecessary untimely death” as a health outcome indicator designed to evaluate the quality of medical care [4]. Subsequently, an American research group empirically applied this concept to “demonstrate the usefulness of this approach” as a measure of healthcare quality [5, 6]. The term “avoidable mortality” came into use following a study by Charlton et al. investigating geographical variation in mortality across England and Wales [7]. While premature death is defined as mortality that happens before a certain age, for example, before 75 years of age [8], “avoidable mortality” refers to premature deaths that could have been avoided in the presence of timely and effective health and social policies and public health interventions aimed at addressing the social determinants of health or reducing risk factors contributing to ill health [8]. Nevertheless, researchers do not adopt a uniform approach to conceptualizing “avoidable mortality,” and it is not always clear whether the terms “avoidable,” “amenable,” “preventable,” and “unnecessary” causes of death are being used interchangeably in the literature [9, 10]. Over time, researchers have refined and updated the list of avoidable causes of death used to classify mortality events as avoidable to suit the situational context of their research [8, 11,12,13,14,15,16]. Recently, there have been efforts to propose standardized global definitions of avoidable mortality, as seen in the work of the Organization for Economic Co-operation and Development (OECD) and the Office for National Statistics (ONS) [17,18,19]. These standardized definitions are pivotal for reliable comparison of health indicators within or between countries [20].
Avoidable mortality is an important summary measure of overall population health status [8], and one of its many applications has been as an indicator of health equity [5, 21]. Researchers have used avoidable mortality to investigate health inequity with the goal of informing political decisions trying to address health inequity [11, 22,23,24,25,26]. Socioeconomic status (SES) is one of the most important “fundamental causes” of disparities in morbidity and mortality [27, 28]. People with lower SES have access to a limited range of resources, such as money, knowledge, prestige, social capital, and power, which could affect their health through many pathways; lack of these resources exposes individuals to a higher risk of mortality [27]. These deaths could be avoided by appropriate means such as timely and effective treatment or the application of health and social policies.
2 Methods
We used Arksey and O’Malley’s framework [29] to conduct this scoping review in five stages:
2.1 Identification of studies
Our central question in this review was “How have avoidable mortality and inequalities therein been defined and operationalized in studies investigating SES inequalities in avoidable mortality?” To answer this question, we developed a search strategy (see Additional file: Appendix A) to find relevant articles by searching Ovid Medline, Scopus, and Web of Science, narrowing down the results to English language and publication dates from 2000 to 2020. We omitted PubMed in our search since the Ovid Medline interface allows a more focused search, excluding citations such as “in process” and “ahead of print” articles [30], which were not of interest to the current review. All the searches were conducted on June 18th, 2020. For grey literature, first, we searched several leading international websites, including Google, Google Scholar, The World Health Organization (WHO) [31], United Nations [32], and Organization for Economic Co-operation and Development (OECD) [33]. We expanded our search by choosing Canada as a sample for a more thorough grey-literature search since our research team is located in Canada. We searched leading Canadian health information websites, including Public Health Agency of Canada (PHAC) [34] restricting our review to the first 5 pages, with 10 results on each page. The following websites were also searched with no restriction on page numbers of the search results: Canadian Institute for Health Information (CIHI) [35]; National Collaborating Center for Determinants of Health [36]; and Ontario Public Health Libraries Association (OPHLA)-Custom Search Engine for Canadian Public Health information [37]. For this study we also partnered with the Urban Public Health Network (UPHN), an association of urban local public health units in Canada; in order to ensure coverage of their membership, we also included their websites in our grey literature search (see Additional file: Appendix B) with no restriction on the page numbers of the search results. The keywords searched to capture relevant grey literature included “avoidable mortality,” “avoidable death,” “preventable mortality,” “preventable death,” “amenable mortality,” and “amenable death.” We did not include the keyword “premature death” as we were focused on avoidable mortality.
2.2 Screening and identifying relevant studies
All the articles were imported into Rayyan® for deduplication and title and abstract screening. The first author reviewed the articles by title and abstract to find relevant studies using the inclusion–exclusion criteria in Table 1. We were only interested in articles investigating socioeconomic status indicators as they are amongst those most frequently implicated as a contributor to inequities in health [38]. Although there is debate about how and whether SES can be measured [39], researchers often consider factors such as income, education, employment, and occupation to assess SES, analyzing them either individually or combining them into a single indicator. These indicators are usually measured at the household or area level so that they can relate to children’s health outcomes as well. We excluded articles investigating a specific cause of death or premature mortality since they are different from indicators of avoidable mortality. As we were interested in studies investigating the entire avoidable mortality at-risk population (aged 0 to 65 or 75), we excluded articles that limited their analysis to only a subset of this population, such as one sex, race, or children. The strict inclusion–exclusion criteria and minimal risk of misclassifying articles led us to use a single reviewer for screening and selecting the articles.
2.3 Selecting eligible studies
After screening the titles and abstracts, the selected articles were transferred from Rayyan® to Paperpile® for in-depth, full-text review. At this stage, the first author evaluated the complete texts using the inclusion–exclusion criteria, determining the final article selection. Once all articles from the searched databases were assessed, the first author applied the criteria outlined in Table 1 to evaluate results from the grey literature search and decide on their inclusion in the review. Finally, the reference lists of all chosen articles were examined to identify any additional pertinent studies.
2.4 Charting the data
We created a spreadsheet to catalog characteristics and data from the chosen articles and grey literature. This form captured details such as the study's timeframe, design, region examined, unit of analysis, population, SES indicators, definition of avoidable mortality, upper age boundaries, avoidable mortality measurement methods, and techniques used to analyze the relationship between avoidable mortality and SES. Additionally, we documented findings regarding the association between SES and avoidable mortality, the International Classification of Diseases (ICD) codes employed to identify avoidable deaths, and the classification of Ischaemic Heart Disease (IHD).
2.5 Collating, summarizing, and reporting the results
Finally, we compiled, summarized, and presented the gathered data. We highlighted the definitions of avoidable mortality used across the articles and determined whether Ischaemic Heart Disease was considered an avoidable cause of death. We summarized the insights from the articles regarding SES disparities in avoidable mortality and identified the SES indicators employed. Moreover, we compared the list of avoidable mortalities of a sample of five articles that used different definitions of avoidable mortality to identify avoidable deaths.
3 Results
3.1 Search results
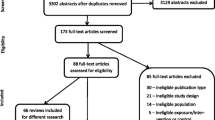
In total, we identified 2457 articles. Of these, 2436 articles were obtained by searching the three predetermined databases using our tailored syntax (see Additional file: Appendix A). From grey literature, we found 16 articles, and 5 more articles were identified by examining the reference lists of the included studies. The database search yielded 810 articles from Ovid Medline, 669 from Web of Science, and 957 from Scopus. After removing duplicates, 1393 potential records underwent title and abstract screening. Of these, 1301 were deemed irrelevant to our research and consequently excluded. This left 92 articles for a full-text review. From these, 58 were further excluded with the reasons for exclusion documented. Figure 1 offers a PRISMA flowchart detailing the selection process of this scoping review.
The grey literature search results were as follows: the World Health Organization (0 records); Public Health Agency of Canada (0 records); United Nations (1 record found and excluded after screening); OECD (1 record found and excluded after screening); CIHI (2 records found, 1 was included after screening); National Collaborating Center for Determinants of Health (1 record found and excluded after screening); OPHLA-Custom Search Engine for Canadian Public Health information (6 records found and 3 were included after screening). Additionally, we identified 5 records from the UPHN members' websites, of which one report was considered suitable for inclusion after the screening process.
In conclusion, 34 articles were selected for detailed review and data extraction, comprising 29 scientific papers and 5 grey literature documents.
3.2 Study designs and distribution by region and timeline
Studies of avoidable mortality heavily rely on having access to previously collected death data. Analyzing and disseminating this data demands time, so the study coverage years might not always match their publication dates. Figure 2 contrasts these trends, showcasing the years studied in blue and publication years in orange. A noteworthy observation is that a significant portion (7 out of 34 articles) were unveiled in 2019, with 4 classified as grey literature. Moreover, there's been a rising trend in the frequency of data collection annually from 1971 to 2016. Regarding the region of study, our findings indicate that the majority of the chosen articles originated from European nations, specifically England, Finland, Spain, France, Switzerland, and Hungary.
Most of the selected studies adopted quantitative observational approaches. To explore disparities in avoidable mortality, researchers employed a myriad of designs such as population-based, ecological, longitudinal, cross-sectional, prospective cohort surveys, exploratory spatial analysis, and official reports. The majority established an upper age threshold of 75 years. However, three distinct studies concentrated solely on deaths before age 65, covering the spans of 1971–2008, 1997–2001, and the 1990s, respectively [40,41,42].
3.3 Unit of analysis
The “unit of analysis” pertains to the level of grouping at which researchers measured avoidable mortality, subsequently stratifying these measurements based on SES to examine disparities. Most studies used small areas as their unit of analysis although the size of these areas varies between concepts and countries. These areas include the Lower Super Output Area (LSOA) in England [43, 44], Dissemination Area (DA) [8, 21, 44,45,46,47], health region [48], and Census Tract (CT) in Canada [49] and Spain [23, 24], commune and canton in France [41, 42], Local Government Area (LGA) [26, 50] and Statistical Local Area (SLA) [51, 52] in Australia, meshblock in New Zealand [53], districts in Brazil [54], neighborhoods [25, 55,56,57], and other small areas [11, 22, 58].
Only two studies used individual-level data for their analysis [59, 60]. A study carried out in Taiwan examined inequality between townships (city districts) [40], and three articles investigated SES inequality in avoidable mortality at the municipal level [61, 62]. Surenjav et al. examined both provincial and municipal (capital) data [63], and Neethling et al. compared provinces and population groups in their analysis [64]. Table 2 presents a summary of the selected articles' characteristics.
3.4 Avoidable mortality definitions and terminology
Researchers have used various definitions of avoidable mortality as the foundation for their studies and referred to it using different terminology. Table 3 displays the definitions adopted within the selected articles. While numerous studies adopted definitions proposed by other researchers or established organizations, several articles introduced their own distinct definitions of avoidable mortality, drawing from pertinent literature and consultations with expert panels.
There is a difference in how researchers phrase and conceptualize the type of mortality deemed avoidable. The term “amenable mortality” is mainly used to describe deaths that could have been averted through medical interventions. This term is often used interchangeably with “treatable mortality” in the literature [12, 65, 66]. A definition by Nolte and Mckee, which is widely used in the selected articles (cited in 11 studies when identifying avoidable deaths,) characterizes “amenable mortality” as premature deaths that could have been avoided through timely and effective health care (i.e., secondary and tertiary prevention) [12]. Consequently, their list of amenable causes does not include deaths preventable via public health policy interventions [12] which are referred to as “preventable mortality” and assessed by other researchers [46, 47, 67].
Conversely, certain definitions, such as the one tailored for the Canadian setting, do not use the term “amenable mortality” [8]. The Canadian Institute for Health Information (CIHI) categorizes “potentially avoidable mortality” into preventable and treatable mortality. Here, “preventable mortality” refers to deaths before the age of 75 that could have been potentially avoided through public health initiatives (i.e., primary prevention.) Meanwhile, “treatable mortality” pertains to premature deaths that could have been potentially avoided through health care interventions and treatments (i.e., secondary and tertiary prevention) [8].
Another important definition, which was published after our search, is that offered by the OECD [17]. In 2022, the OECD and Eurostat partnered to create joint lists of “avoidable” causes of death [17]. This definition builds upon the lists developed by Nolte and McKee [12], Eurostat [68], and CIHI [8], categorizing avoidable mortality into “preventable” and “treatable” mortalities. These categories are aligned with CIHI's definitions [17]. Within this framework, the term “amenable” from the prior Eurostat list has been rephrased as “treatable.” Similarly, the NHS Outcome Framework [69] along with the Australian and New Zealand Atlas of Avoidable Mortality [66] classify avoidable deaths into “amenable” and “preventable” categories, resonating with CIHI's definition of “treatable” and “preventable” mortality.
Simonato et al. [13] and Tobias and Jackson [11] use unique terminology to define avoidable mortality. They partition avoidable mortality into three categories, each attributed to a set of mortalities that could be averted through one of the levels of prevention (i.e., primary, secondary, and tertiary levels). A detailed breakdown of the commonly used definitions in the selected articles is provided in Table 4.
3.5 Operationalization of avoidable mortality measures
Measures of avoidable mortality vary with respect to their operationalization using ICD codes (e.g., whether IHD is classified as avoidable). We evaluated the list of avoidable mortalities from five articles chosen at random and found significant variances. Table 5 presents these five articles, each tagged with a unique article code. These article codes serve as references when comparing their respective lists of avoidable mortality by ICD codes, as detailed in Additional file: Appendix C. These differences largely arise from the adoption of varied definitions of avoidable mortality. Another contributing factor is the timeframe in which these lists were created; perceptions of avoidability evolve over time due to advancements in healthcare services and public health.
Despite the diverse views on which causes of death are deemed avoidable across the selected articles (see Additional file: Appendix C) Ischemic Heart Disease (IHD) remains a focal point in discussions about avoidability and its measurement. Among the chosen articles, there is no consensus on whether death due to IHD should be labelled as an avoidable cause. Numerous studies subdivide IHD into two [8, 21, 56, 57, 70] or even three [11, 50] subsets of avoidable mortality. Several studies included only half of the IHD mortality in their calculation of amenable mortality rates as proposed by Nolte and McKee [12, 25, 53, 55, 58]. Additionally, some articles opted out of classifying IHD as an avoidable cause, excluding it from their calculations of avoidable mortality rates [22, 24, 42]. (See Additional file: Appendix D for the number of studies that followed each approach). Taking note of these various approaches is particularly important in health inequality research as IHD is known to be one of the leading conditions in health inequality [71, 72].
3.6 Socioeconomic status indicator
We classified the articles based on the type of indicator used for socioeconomic status (SES) into four categories, namely index, income, education, and employment. The index category includes any article using a predefined index for SES, such as the Ontario Marginalization Material Deprivation Index (ON-Marg) [44, 56], Index of Relative Socioeconomic Disadvantage (IRSD) [26, 50, 51], and Index of Multiple Deprivation (IMD) [43, 44]. Some authors constructed a variable representing SES in a population using indicators such as income and education [23, 24]. We placed these studies in the index group as well. To decide whether to include or exclude an article that used an SES index, we carefully examined the index to ensure that at least one of our indicators of interest (i.e., education, income, and employment/occupation) was taken into account in its construction. One study in South Africa used apartheid classifications (Africans, Whites, Asians, and Coloureds) as a proxy for socioeconomic status, arguing that income and education disparities continued to persist in the population even after apartheid was ended [64].
Most of the articles (n = 20) used an index to investigate SES inequality in avoidable mortality. This number was 13 for income indicators, 4 for education, and 2 for employment. If a study examined more than one category in its analysis, we counted each category separately. For example, if an article examined income and education inequality in avoidable mortality separately, we counted this article once for the income category and once for the education category.
3.7 Standardization for age and sex
Most of the included articles used directly age-standardized mortality rates to assess avoidable mortality. In some cases, mortality rates were also standardized by sex. However, some studies applied unique methodologies. For example, one study estimated smoothed standardized mortality rates using the Bayesian model proposed by Besag et al. [73], to address the problem of age standardization in small areas [22]. A Hungarian study calculated mortality amenable to health care ratios using full hierarchical Bayesian methods. In doing so, the authors calculated smoothed indirectly standardized mortality ratios using sex- and age-specific rates for the Hungarian population [62]. A Canadian study calculated the age-standardized expected years of life lost (SEYLL) rate instead of the mortality rate, using the life expectancies of the richest income quintile as the standard [49]. Another methodology examined the contribution of different groups of mortality, including death amenable to health care and death amenable to health policy, to life expectancy at age 35 and partial life expectancy between 35 and 75 [59]. Doing so, Manderbacka et al. were able to assess the impact of health policy and care on income disparities in life expectancy in Finland [59]. In a study conducted by Masters et al. the authors tested the central claims of Fundamental Cause Theory (FCT) and then performed a retrospective cohort study to examine the association between preventable mortality and educational attainment [60]. An ecological study conducted in France calculated the standardized mortality ratio by dividing the observed mortality in a spatial unit by the corresponding expected mortality [41].
3.8 Association between SES and avoidable mortality
The findings of the selected articles consistently indicate a negative relationship between SES and avoidable mortality rates, where the avoidable mortality rate is higher among those with lower socioeconomic status. This aligns with the substantial body of knowledge indicating the role of SES in population health [2, 3, 27, 74, 75]. Khan et al. found a similar trend among immigrants and long-term residents, with a downward gradient in age-adjusted avoidable mortality rates as income quintiles increase [45]. However, a study conducted in Mongolia reported no significant relationship between avoidable mortality rate and the percentage of poor households [63]. This could be due to the lack of individual or neighborhood-level data in this study, which focused on the capital and provincial levels [76]. Nevertheless, the study revealed higher amenable mortality rates in remote western provinces in Mongolia, characterized by harsh weather conditions, high poverty rates, lack of human resources for health, and poor infrastructure [63]. Details on the findings of the selected articles are provided in Table 2.
While some studies adopted a descriptive approach and compared the avoidable mortality rates between different SES groups, many articles examined SES inequality in avoidable mortality using various types of analysis, including Poisson regression models, calculating Slope Index of Inequality (SII) and Relative Index of Inequality (RII), disparity rate ratio, incidence rate difference, random coefficient growth curve modeling approach, ecological regression, among other analytical methods.
The majority of findings from the captured studies indicate a decline in avoidable mortality rates over time while socioeconomic disparities persisted [43, 54, 56]. A study conducted in South Africa found that the socioeconomic disparity widened from 2000 to 2005 and narrowed thereafter until 2012 [64]. Similar patterns were observed in France, with a 40% higher avoidable mortality rate for the fifth deprivation quintile communes compared to the first quintile in 1988–92, and 78% higher in 1997–2001 [42]. A study conducted in Taiwan reported a faster decline in avoidable mortality from 1971 to 2008 in affluent townships compared to less affluent townships [40]. Similarly, an Australian study found a larger decline in avoidable mortality rates in higher socioeconomic groups, with increasing relative inequality and decreasing absolute inequality between 1986 and 2002 [52].
4 Discussion and conclusion
The findings of this review highlight the variability in terminology and definition for the concept of avoidable mortality used in health inequality research. Using common indicator definitions are essential for reliable comparison of health indicators within or between countries [20]. Recently, an OECD working group created a harmonized avoidable mortality definition to be used internationally [17, 77]. This definition can potentially address the gap we identified in the literature concerning the lack of consensus among researchers regarding the measurement of avoidable mortality. However, while there's a pressing need for standardized terminology and definition for avoidable mortality, it is important to recognize that a single, universal list of avoidable causes of death applicable in all countries and contexts is not likely feasible. The avoidability of specific causes of death may vary across countries with different levels of advancement in medical sciences. Therefore, it is crucial to consider the contextual factors and available healthcare technologies when developing lists of avoidable causes of death, acknowledging the variations across low-, middle-, and high-income countries. Nonetheless, this should not deter the establishment of a standardized definition, which is pivotal for supporting global comparability in this area of research.
The majority of studies captured in our scoping review were conducted in high-income countries, with Europe having the highest number of publications, followed by Australia and New Zealand. This trend may be attributed to the presence of national or regional standard definitions for avoidable mortality in these countries, such as the well-established list of avoidable causes proposed for use in the Australian [66] and European [78] contexts. Nonetheless, it is worth noting that the availability of the list of avoidable causes of death primarily designed for high-income countries may hinder the conduction of avoidable mortality research in lower-income countries.
The absence of an established list of avoidable causes of death can be one reason for the low number of research conducted in low-income countries as compared to high-income countries. This difference in the number of studies can also be explained by numerous other factors, including the unequal distribution of money, power, and other resources between low- and high-income countries. Nevertheless, the impact of the absence of an established list of avoidable causes of death on the number of studies can also be observed in high-income countries like Canada. The introduction of Canada’s first list of potentially avoidable causes of death in 2012 by CIHI [8] has led to a significant increase in inequality research on avoidable mortality in the Canadian literature [8, 21, 56, 57, 70]. Four out of five Canadian governmental reports included in this review were published in 2019. These findings underscore the crucial role played by established definitions and lists of avoidable causes of death in promoting research on SES-related inequalities in avoidable mortality.
Furthermore, it should be noted that our data collection took place during the early stages of the COVID-19 pandemic. Consequently, the literature captured and discussed in this scoping review does not include the subsequent debates regarding the consideration of COVID-19 as an avoidable mortality and its association with SES. Since then, organizations such as CIHI [79] and OECD/Eurostat [17], have revised and updated their lists of avoidable causes of death to incorporate COVID-19.
4.1 Study limitations
A potential limitation of this scoping review is that only one reviewer screened the articles. However, given the rigorous inclusion–exclusion criteria we used, we are confident that the risk of misclassification of articles remains minimal. In addition, this scoping review focused on studies of avoidable mortality that included analysis of SES-related inequalities. However, there exists a body of literature exploring inequality in avoidable mortality in terms of social determinants of health other than socioeconomic status, such as ethnicity. For instance, in their study of avoidable mortality in South Africa, Debbie Bradshaw and colleagues used apartheid classifications as a proxy for socioeconomic status. While we decided to include this particular study in our scoping review, we acknowledge that studies not considering SES indicators in assessing inequalities and those that did not investigate disparities may have used additional conceptualizations and definitions of avoidable mortality.
Data availability
This study used publicly available data from published articles and reports. All the studies used in this scoping review can be found in the reference list.
References
HIR. Key health inequalities in Canada: a national portrait. Pan-Canadian Health Inequalities Reporting Initiative (HIR). 2018.
CSDH. Closing the gap in a generation: health equity through action on the social determinants of health. Final Report of the Commission on Social Determinants of Health, World Health Organization. 2008.
Health Disparities Task Group of the Federal/Provincial/Territorial Advisory Committee on Population Health and Health Security, Reducing Health Disparities—Roles of the Health Sector: Discussion Paper, Public Health Agency of Canada. 2004.
Rutstein DD, Berenberg W, Chalmers TC, Child CG, Fishman AP, Perrin EB. Measuring the quality of medical care: a clinical method. N Engl J Med. 1976;294:582.
Pi L, Gauvin F-P, Lavis JN. Issue Brief: building momentum in using the avoidable mortality indicators in Canada. McMaster Health Forum. 2013.
Adler GS. Measuring the quality of medical care. N Engl J Med. 1978;298:574.
Charlton JR, Hartley RM, Silver R, Holland WW. Geographical variation in mortality from conditions amenable to medical intervention in England and Wales. Lancet. 1983;1:691.
CIHI. Health Indicators 2012. Canadian Institute for Health Information (CIHI). 2012.
Castelli A, Nizalova O. Avoidable mortality: what it means and how it is measured. University of York. 2011.
Karanikolos M, McKee M, Nolte E. Revisiting the concept of “preventable mortality”: a scoping review. Eur J Public Health. 2018. https://doi.org/10.1093/eurpub/cky213.501.
Tobias M, Jackson G. Avoidable mortality in New Zealand, 1981–97. Aust N Z J Public Health. 2001;25:12.
Nolte E, McKee M. Does health care save lives? Avoidable mortality revisited. Nuffield Trust. 2004.
Simonato L, Ballard T, Bellini P, Winkelmann R. Avoidable mortality in Europe 1955–1994: a plea for prevention. J Epidemiol Community Health. 1998;52:624.
Mackenbach JP, Looman CW, Kunst AE, Habbema JD, van der Maas PJ. Post-1950 mortality trends and medical care: gains in life expectancy due to declines in mortality from conditions amenable to medical intervention in The Netherlands. Soc Sci Med. 1988;27:889.
Holland W. European community atlas of “avoidable death.” 3rd ed. Oxford: Oxford University Press; 1988.
OECD. Avoidable mortality: OECD/Eurostat List of preventable and treatable causes of death. Organisation for Economic Co-operation and Development. 2019.
OECD. Avoidable mortality: OECD/Eurostat lists of preventable and treatable causes of death. Organisation for Economic Co-operation and Development. 2022.
OECD/Eurostat. Avoidable mortality: OECD/Eurostat lists of preventable and treatable causes of death. Organization for Economic Co-operation and Development. 2019.
ONS. Definition of avoidable mortality, office for national statistics. 2012.
Tolonen H, Reinikainen J, Koponen P, Elonheimo H, Palmieri L, Tijhuis MJ, Joint Action on Health Information (InfAct). Cross-national comparisons of health indicators require standardized definitions and common data sources. Arch Public Health. 2021;79:208.
Rasali D, Kao D, Fong D, Qiyam L. Priority Health Equity Indicators for British Columbia: preventable and treatable mortality, 2009–2013. BC Centre for Disease Control. Provincial Health Services Authority. 2019.
Hoffmann R, et al. Social differences in avoidable mortality between small areas of 15 European cities: an ecological study. Int J Health Geogr. 2014;13:8.
Nolasco A, et al. Preventable avoidable mortality: evolution of socioeconomic inequalities in urban areas in Spain, 1996–2003. Health Place. 2009;15:732.
Nolasco A, et al. Trends in socioeconomic inequalities in preventable mortality in urban areas of 33 Spanish cities, 1996–2007 (MEDEA Project). Int J Equity Health. 2015;14:33.
Weisz D, Gusmano MK, Rodwin VG, Neuberg LG, Weisz D, Gusmano MK, Rodwin VG, Neuberg LG. Population health and the health system: a comparative analysis of avoidable mortality in three nations and their world cities. Eur J Public Health. 2008;18:166.
Piers LS, Carson NJ, Brown K, Ansari Z. Avoidable mortality in Victoria between 1979 and 2001. Aust N Z J Public Health. 2007;31:5.
Phelan JC, Link BG, Diez-Roux A, Kawachi I, Levin B. “Fundamental causes” of social inequalities in mortality: a test of the theory. J Health Soc Behav. 2004;45:265.
Link BG, Phelan J. Social conditions as fundamental causes of disease. J Health Soc Behav. 1995;35:80.
Arksey H, O’Malley L. Scoping studies: towards a methodological framework. Int J Soc Res Methodol. 2005;8:19.
MEDLINE, PubMed, and PMC (PubMed Central): how are they different?. https://www.nlm.nih.gov/bsd/difference.html. Accessed 17 Aug 2023.
WHO. Home. https://www.who.int/. Accessed 19 Dec 2020.
United Nations. United Nations|Peace, Dignity and Equality on a Healthy Planet, https://www.un.org/en/. Accessed 19 Dec 2020.
OECD. OECD. https://www.oecd.org/. Accessed 19 Dec 2020.
Public Health Agency of Canada, Public Health Agency of Canada. https://www.canada.ca/en/public-health/services/food-poisoning/campylobacter-jejuni.html. Accessed 19 Dec 2020.
CIHI. Canadian Institute for Health Information, https://www.cihi.ca/en. Accessed 19 Dec 2020.
NCCDH. National Collaborating Centre for Determinants of Health. https://nccdh.ca/. Accessed 19 Dec 2020.
OPHLA. Custom search engine for Canadian Public Health Information. http://www.ophla.ca/p/customsearchcanada.html. Accessed 19 Dec 2020.
Shavers VL. Measurement of socioeconomic status in health disparities research. J Natl Med Assoc. 2007;99:1013.
Antonoplis S. Studying socioeconomic status: conceptual problems and an alternative path forward. Perspect Psychol Sci. 2023;18:275.
Chen BK, Yang YT, Yang C-Y. Trends in amenable deaths based on township income quartiles in Taiwan, 1971–2008: did universal health insurance close the gap? J Public Health. 2016;38:E524.
Rey G, Jougla E, Fouillet A, Hemon D. Ecological association between a deprivation index and mortality in France over the period 1997–2001: variations with spatial scale, degree of urbanicity, age, gender and cause of death. BMC Public Health. 2009;9:33.
Windenberger F, Rican S, Jougla E, Rey G, Windenberger F, Rican S, Jougla E, Rey G. Spatiotemporal association between deprivation and mortality: trends in France during the nineties. Eur J Public Health. 2012;22:347.
Asaria M, Ali S, Doran T, Ferguson B, Fleetcroft R, Goddard M, Goldblatt P, Laudicella M, Raine R, Cookson R. How a universal health system reduces inequalities: lessons from England. J Epidemiol Community Health. 2016;70:637.
Cookson R, Mondor L, Asaria M, Kringos DS, Klazinga NS, Wodchis WP. Primary care and health inequality: difference-in-difference study comparing England and Ontario. PLoS ONE. 2017;12:e0188560.
Khan AM, et al. Socioeconomic gradients in all-cause, premature and avoidable mortality among immigrants and long-term residents using linked death records in Ontario, Canada. J Epidemiol Community Health. 2017;71:625.
Zygmunt A, Kendall CE, James P, Lima I, Tuna M, Tanuseputro P. Avoidable mortality rates decrease but inequity gaps widen for marginalized neighborhoods: a population-based analysis in Ontario, Canada from 1993 to 2014. J Community Health. 2019. https://doi.org/10.1007/s10900-019-00778-8.
Zygmunt A, Tanuseputro P, James P, Lima I, Tuna M, Kendall CE. Neighbourhood-Level marginalization and avoidable mortality in Ontario, Canada: a population-based study. Can J Public Health. 2020;111:169.
Young TK, Chatwood S, Ng C, Young RW, Marchildon GP. The north is not all the same: comparing health system performance in 18 northern regions of Canada. Int J Circumpolar Health. 2019;78:1697474.
James PD, Wilkins R, Detsky AS, Tugwell P, Manuel DG. Avoidable mortality by neighbourhood income in Canada: 25 years after the establishment of universal health insurance. J Epidemiol Community Health. 2007;61:287.
Hayen A, Lincoln D, Moore H, Thomas M. Trends in potentially avoidable mortality in NSW. N S W Public Health Bull. 2002;13:226.
Butler DC, Petterson S, Bazemore A, Douglas KA, Butler DC, Petterson S, Bazemore A, Douglas KA. Use of measures of socioeconomic deprivation in planning primary health care workforce and defining health care need in Australia. Aust J Rural Health. 2010;18:199.
Korda RJ, Butler JRG, Clements MS, Kunitz SJ. Differential Impacts of health care in Australia: trend analysis of socioeconomic inequalities in avoidable mortality. Int J Epidemiol. 2007;36:157.
Tobias M, Yeh LC, Tobias M, Yeh L-C. How much does health care contribute to health gain and to health inequality? Trends in amenable mortality in New Zealand 1981–2004. Aust N Z J Public Health. 2009;33:70.
Grafova IB, Weisz D, Fischetti Ayoub R, Rodwin VG, NeMoyer R, Gusmano MK. Amenable mortality and neighborhood inequality: an ecological study of São Paulo. World Med Health Policy. 2020;12:182.
Feller A, Schmidlin K, Clough-Gorr KM. Trends and socioeconomic inequalities in amenable mortality in Switzerland with international comparisons. Swiss Med Wkly. 2017;147: w14478.
MLHU. Income-related health inequities. http://communityhealthstats.healthunit.com/indicator/social-determinants-health/income-related-health-inequities. Accessed 27 Oct 2020.
MLHU. Preventable mortality. http://communityhealthstats.healthunit.com/indicator/general-health/preventable-mortality. Accessed 27 Oct 2020.
Tobias M, Yeh LC, Tobias M, Yeh L-C. How much does health care contribute to health inequality in New Zealand? Aust N Z J Public Health. 2007;31:207.
Manderbacka K, Peltonen R, Lumme S, Keskimaki I, Tarkiainen L, Martikainen P. The contribution of health policy and care to income differences in life expectancy—a register based cohort study. BMC Public Health. 2013;13:812.
Masters RK, Link BG, Phelan JC. Trends in education gradients of “preventable” mortality: a test of fundamental cause theory. Soc Sci Med. 2015;127:19.
Ronzio CR, Pamuk E, Squires GD. The politics of preventable deaths: local spending, income inequality, and premature mortality in US cities. J Epidemiol Community Health. 2004;58:175.
Nagy C, Juhasz A, Beale L, Paldy A. Mortality amenable to health care and its relation to socio-economic status in Hungary, 2004–08. Eur J Public Health. 2012;22:620.
Surenjav E, Sovd T, Yoshida Y, Yamamoto E, Reyer JA, Hamajima N. Trends in amenable mortality rate in the Mongolian population, 2007–2014. Nagoya J Med Sci. 2016;78:55.
Neethling I, Groenewald P, Schneider H, Bradshaw D. Trends and inequities in amenable mortality between 1997 and 2012 in South Africa. S Afr Med J. 2019;109:597.
OECD. Avoidable mortality (preventable and Treatable). https://www.oecd-ilibrary.org/sites/3b4fdbf2-en/index.html?itemId=/content/component/3b4fdbf2-en. Accessed 30 Oct 2021.
Page A, Tobias M, Glover J, Wright C, Hetzel D, Fisher E. Australian and New Zealand Atlas of Avoidable Mortality, E Public Health Information Development Unit, the University of Adelaide. 2006.
Shahidi FV, Parnia A, Siddiqi A. Trends in socioeconomic inequalities in premature and avoidable mortality in Canada, 1991–2016. CMAJ. 2020;192:E1114.
Eurostat. Archive: amenable and preventable deaths statistics. https://ec.europa.eu/eurostat/statistics-explained/index.php?title=Amenable_and_preventable_deaths_statistics&direction=next&oldid=337528. Accessed 22 Sept 2022.
NHS. The NHS outcomes framework 2012/13, NHS. 2013.
Cui Y, Zinnick S, Henderson A, Dunne L. Winnipeg health region community health assessment 2019. Winnipeg Regional Health Authority. 2019.
Vodden A, Holdroyd I, Bentley C, Marshall L, Barr B, Massou E, Ford J. Evaluation of the national governmental efforts between 1997 and 2010 in reducing health inequalities in England. Public Health. 2023;218:128.
Di Cesare M, et al. Inequalities in non-communicable diseases and effective responses. Lancet. 2013;381:585.
Besag J, York J, Mollié A. Bayesian image restoration, with two applications in spatial statistics. Ann Inst Stat Math. 1991;43:1.
Marmot M. Social determinants of health inequalities. Lancet. 2005;365:1099.
CIHI. Reducing gaps in health: a focus on socio-economic status in Urban Canada. Canadian institute for Health Information. 2008.
Hosseinpoor AR, Bergen N. Area-Based units of analysis for strengthening health inequality monitoring. Bull World Health Organ. 2016;94:856.
ONS. Avoidable mortality in the UK QMI. https://www.ons.gov.uk/peoplepopulationandcommunity/healthandsocialcare/causesofdeath/methodologies/avoidablemortalityinenglandandwalesqmi. Accessed 19 Jan 2024.
Plug I, Hoffmann R, Mackenbach J. Avoidable mortality in the European Union: towards better indicators for the effectiveness of health systems. European Union Health Program. 2011.
CIHI. List of conditions for avoidable mortality and mortality from preventable and treatable causes indicators. Canadian Institute for Health Information. 2022.
Acknowledgements
This paper is based on a part of Anousheh Marouzi’s M.Sc. thesis, and the first author thanks the advisory committee, Maureen Anderson and Sylvia Abonyi, for taking the time to assess her thesis and their insightful comments. The authors also thank Vicky Duncan and Thilina Bandara for reviewing earlier versions of this paper and for their helpful comments.
Funding
This research was funded in part by the Urban Public Health Network. No other financial support was received for the research, authorship, and/or publication of this article.
Author information
Authors and Affiliations
Contributions
Anousheh Marouzi conducted the data collection and analysis and prepared the first draft of the article. Anousheh Marouzi and Charles Plante designed the study and directed its implementation, including quality assurance and control. Charles Plante supervised the data collection and analysis; he also reviewed, edited, and finalized the text. Cordell Neudorf provided the overall guidance and funding for the research project. All authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Marouzi, A., Plante, C. & Neudorf, C. Application of the concept ‘avoidable mortality’ in assessing the socioeconomic status related inequalities in health: a scoping review. Discov Soc Sci Health 4, 12 (2024). https://doi.org/10.1007/s44155-024-00073-5
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s44155-024-00073-5