Abstract
Introduction
Post-traumatic blister is often encountered in high-energy injuries and following major limb surgeries. Currently, there is very limited evidence concerning blister management resulting in a lack of comprehensive guidelines for their management. The current survey-based study aims to appraise the current consensus in post-traumatic management among the practising orthopaedic surgeons and compare the same with the evidence in the literature.
Materials and Methods
We conducted an online questionnaire-based survey of orthopaedic surgeons concerning post-traumatic blister management practices. The questionnaire mainly focused on antibiotic prophylaxis, local invasive procedures, antiseptics dressings and additional treatment options regarding blister management.
Results
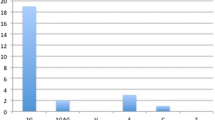
A high prevalence (~ 78%) of systemic antibiotics administration was noticed for post-traumatic blister management. Similarly, large section of respondents (66.4%) advocated for either de-roofing or aspiration of blisters. Approximately 42% of respondents preferred sending blister fluid for cultures. More than half of the respondents used some form of local dressing to cover the blister bed to provide a healing environment. Additional opinions mostly included anti-inflammatory and swelling reducing measures. Few respondents also advocated for oral steroids for inflammation control.
Conclusion
The limited evidence available in literature could be the potential contributing factor for varying clinical practices for post-traumatic blister management. The general measures to reduce soft-tissue oedema have been supported by the literature. However, the use of systemic antibiotics and steroids has not been supported by the literature and should be avoided unless indicated due to other reasons. Further evidence is required to strengthen the recommendations for post-traumatic blister management.



Similar content being viewed by others
Data Availability
Data assessed can be provided on request.
References
McCann, S., & Gruen, G. (1997). Fracture blisters: A review of the literature. Dermatology Nursing, 9(6), 391–398.
Strauss, E. J., Petrucelli, G., Bong, M., Koval, K. J., & Egol, K. A. (2006). Blisters associated with lower-extremity fracture: Results of a prospective treatment protocol. Journal of Orthopaedic Trauma, 20(9), 618–622.
Uebbing, C. M., Walsh, M., Miller, J. B., Abraham, M., & Arnold, C. (2011). Fracture blisters. West. Journal of Emergency Medicine, 12(1), 131.
Giordano, C. P., Scott, D., Koval, K. J., Kummer, F., Atik, T., & Desai, P. (1995). Fracture blister formation: A laboratory study. Journal of Trauma and Acute Care Surgery, 38(6), 907–909.
Borrelli, J., Jr. (2014). Management of soft tissue injuries associated with tibial plateau fractures. The Journal of Knee Surgery, 27(01), 5–10.
Quevedo, D. G., Siles, J. M. S., Tomba, F. R., Mariño, I. T., Bardaji, M. F. B., & Pareja, F. V. (2017). Blisters in ankle fractures: A retrospective cohort study. Journal of Foot and Ankle Surgery, 56(4), 740–743.
Hasegawa, I. G., Livingstone, J. P., & Murray, P. (2018). A novel method for fracture blister management using circumferential negative pressure wound therapy with instillation and dwell. Cureus, 10(10), e3509.
Bleakley, C., McDonough, S., & MacAuley, D. (2004). The use of ice in the treatment of acute soft-tissue injury: A systematic review of randomized controlled trials. American Journal of Sports Medicine, 32(1), 251–261.
Clarkson, R., Mahmoud, S. S., Rangan, A., Eardley, W., & Baker, P. (2017). The use of foot pumps compression devices in the perioperative management of ankle fractures: Systematic review of the current literature. Foot (Edinburgh, Scotland), 31, 61–66.
Matsen, F. A., 3rd., Wyss, C. R., Krugmire, R. B., Jr., Simmons, C. W., & King, R. V. (1980). The effects of limb elevation and dependency on local arteriovenous gradients in normal human limbs with particular reference to limbs with increased tissue pressure. Clinical Orthopaedics and Related Research, 150, 187–195.
Ballo, F., Maroon, M., & Millon, S. J. (1994). Fracture blisters. Journal of the American Academy of Dermatology, 30(6), 1033–1034.
Wallace, G., & Sullivan, J. (1995). Fracture blisters. Clinics in Podiatric Medicine and Surgery, 12, 801–812.
Lal, G., & Bhan, S. (1991). Delayed open reduction for supracondylar fractures of the humerus. International Orthopaedics, 15(3), 189–191.
Varela, C. D., Vaughan, T. K., Carr, J. B., & Slemmons, B. K. (1993). Fracture blisters: Clinical and pathological aspects. Journal of Orthopaedic Trauma, 7(5), 417–427.
Buckley, W. R., & Lobitz, W. C., Jr. (1953). The Fracture Blister. New England Journal of Medicine, 249(1), 11–13.
Wiese, K. R., van Heukelum, M., Lombard, C. J., Ferreira, N., & Burger, M. C. (2021). Randomized controlled trial comparing silver-impregnated fibrous hydrocolloid dressings with silver sulfadiazine cream dressings for the treatment of fracture blisters to determine time to surgical readiness. Journal of Orthopaedic Trauma, 35(8), 442–447.
Tolpinrud, W. L., Rebolledo, B. J., Lorich, D. G., & Grossman, M. E. (2015). A case of extensive fracture bullae: A multidisciplinary approach for acute management. JAAD Case Reports, 1(3), 132.
Bork, K. (1978). Physical forces in blister formation. The role of colloid osmotic pressure and of total osmolality in fluid migration into the rising blister. Journal of Investigative Dermatology, 71(3), 209–212.
Chandanwale, A., Langade, D., Sonawane, D., & Gavai, P. (2017). A randomized, clinical trial to evaluate efficacy and tolerability of trypsin: chymotrypsin as compared to serratiopeptidase and trypsin:bromelain: rutoside in wound management. Advances in Therapy, 34(1), 180–198.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
SS, AK contributed with concept, design, data analysis, manuscript preparation, manuscript editing, and manuscript review. JJ, OAQ contributed with manuscript preparation, and manuscript editing. SK, AM contributed in literature review, manuscript editing, and manuscript review.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors has any conflicts to declare.
Ethical Approval
The study was approved by the institutional review board.
Consent to Participate
Appropriate consents were obtained from the involved participants.
Consent to Publish
Not applicable (No human or animal subjects related information involved).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Sinha, S., Kumar, A., Jameel, J. et al. The Current Consensus on the Management of Post-traumatic Blisters Among Orthopaedic Surgeons. JOIO 56, 1011–1017 (2022). https://doi.org/10.1007/s43465-022-00612-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43465-022-00612-9