Abstract
Schistosomiasis, a neglected tropical disease, affects millions of lives and accounts for thousands of deaths each year. The Schistosoma parasites depend on two hosts during their lifecycle: snails as intermediate hosts and human beings as definitive hosts. Therefore, to control and ultimately eliminate schistosomiasis relies on the reduction of snail populations as well as the prevention and treatment of schistosomiasis infections. Praziquantel is the primary drug for prevention and treatment, and although it is considered safe and efficacious, concerns exist regarding emerging drug resistance due to mass drug administration. For this reason, novel antischistosomal drugs are in need and the genus Artemisia might be a promising source. Notably, Artemisia species not only have been evaluated for their antischistosomal effects against Schistosoma parasites, but also for their molluscicidal effects against the snail vectors. Extracts of Artemisia afra seem to be the most active, with IC50 values comparable with the positive control, praziquantel. The antimalarial drug artemisinin, obtained from A. annua, and its semisynthetic derivatives artemether, artesunate, and artemisone have also been evaluated against both schistosomes and snail vectors. Artemether and artesunate have been found to be notably active against the adult and juvenile stages of schistosomes, whereas artemisone was shown to be effective in treating hosts harboring juvenile schistosomes. Artemisinin on the other hand in combination with praziquantel presents as a good lead combination in curing schistosomiasis.
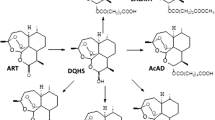
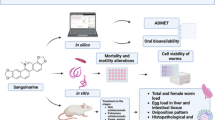
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Schistosomiasis, more commonly known as snail fever or bilharzia, is an infectious acute and chronic disease caused by trematode parasites belonging to the genus Schistosoma (Colley et al. 2014; WHO 2022; Saber et al. 2022). This disease is considered to be one of the most devastating neglected tropical diseases (NTDs), which globally affects approximately 240 million individuals (de Moraes et al. 2014; Center for Disease Control and Prevention 2018; WHO 2022). Annually, this disease accounts for approximately 200,000 deaths, and those at risk of becoming infected with schistosomiasis exceeds 700 million, as estimated by the World Health Organization (WHO) (Verjee 2020; WHO 2022). This NTD occurs in low- and middle-income countries in the tropical and sub-tropical regions of the world (Li et al. 2019; WHO 2022). In Africa, the Middle East, South America, the Caribbean, and Asia, schistosomiasis remains a major cause of mortality and morbidity (Ross et al. 2017). Transmission of schistosomiasis has been reported in more than 70 countries, and due to increased tourism and migration, this disease is spreading to what once were uninfected areas (Enk et al. 2003; Boissier et al. 2015; Murta et al. 2016; Lingscheid et al. 2017; Bekana et al. 2022; WHO 2022).
Schistosoma Species and Their Lifecycle
The three most common Schistosoma species that cause human disease are S. mansoni, S. japonicum, and S. haematobium (Caffrey 2007; Colley et al. 2014; Center for Disease Control and Prevention 2018; McManus et al. 2018). Other Schistosoma species less likely to cause human disease include S. intercalatum, S. guineensis, and S. mekongi (Center for Disease Control and Prevention 2018; Verjee 2020). The geographical distribution of these Schistosoma species is mainly defined by the habitat of the specific intermediate snail host required for maintenance of the parasite’s lifecycle (Colley et al. 2014) (Table S1). Urogenital and intestinal pathologies of schistosomiasis are also dependent on which Schistosoma species causes infection (Center for Disease Control and Prevention 2019; WHO 2022; Ojo et al. 2021).
Two different hosts are required during the lifecycle of the Schistosoma species (Fig. 1), an intermediate host snail and a human being as the final host (Li et al. 2019). In freshwater, snail hosts become infected with free-swimming miracidia (immature schistosome larvae), which multiply asexually inside the snail for up to 6–8 weeks to produce cercariae, the infectious form for humans. Cercariae then return to the water source, from where they penetrate the skin of the human host and transform into schistosomula (maturing larvae). These schistosomula migrate through the vascular system to the final maturation site, the perivesicular venous system for S. haematobium, and mesenteric and hepatic portal venous systems for S. mansoni, S. japonicum, and the others. They then mature over 5–7 weeks into adult female and male worms. These worms then mate and produce fertilized eggs that are either cast back into the environment through urine (S. haematobium) or feces (S. mansoni, S. japonicum, and the others) or retained inside the body (bladder or intestines), leading to inflammation and ultimately morbidity (urogenital or intestinal schistosomiasis). The excreted eggs reaching freshwater sources hatch and produce free-swimming miracidia, from which a new lifecycle starts (Caffrey 2007; Colley et al. 2014; Center for Disease Control and Prevention 2019).
Schistosoma species life cycle. (1) Eggs are eliminated with feces or urine from infected human. (2) The eggs hatch and release miracidia, which swim and penetrate specific snail intermediate hosts (3). The stages in the snail include two generations of sporocysts (4) and the production of cercariae (5). Upon release from the snail, the infective cercariae swim, penetrate the skin of the human host (6), and shed their forked tails, becoming schistosomulae (7). The schistosomulae migrate via venous circulation (8) to lungs, then to the heart, and then develop in the liver, exiting the liver via the portal vein system when mature (9). Male and female adult worms copulate and reside in the mesenteric venules of the bowel and rectum (10). Reproduced from Center for Disease Control and Prevention https://www.cdc.gov/parasites/schistosomiasis/biology.html
Clinical Manifestations
The basis for morbidity due to schistosomiasis is the reaction by the body to the schistosome eggs in the infected body tissue, and not by the adult Schistosoma worms themselves (Colley et al. 2014). For the most part, infections are usually asymptomatic. However, a cutaneous hypersensitive reaction may occur at the site where the cercariae penetrate the skin (Center for Disease Control and Prevention 2019). In schistosomiasis-endemic regions, immigrants or travellers may develop acute schistosomiasis (Katayama syndrome) weeks to months after being exposed to infested water sources for the first time. Those with Katayama syndrome may present with malaise, headache, fatigue, eosinophilia, abdominal pain, and a sudden onset of fever that lasts for 2 to 10 weeks (Colley et al. 2014).
Chronic schistosomiasis, the most prevalent form of this disease, arises after repeated exposure to the parasites (Colley et al. 2014). The two main infection areas associated with urogenital and intestinal schistosomiasis are either the urinary tract or the intestines. Haematuria (urine containing blood) is the first sign of an acute urogenital infection. Other possible acute symptoms may include nodules in the vulva, vaginal bleeding, genital lesions, and painful sexual intercourse in women, while in men the pathology of the prostate, seminal vesicles, and other organs may be affected. Chronic urogenital schistosomiasis leads to complications including ureter and bladder fibrosis, kidney damage, as well as bladder carcinoma and infertility. On the other hand, bloody stools, pain in the abdomen, and diarrhoea are significant symptoms of intestinal schistosomiasis that often are associated with hepatosplenomegaly, abdominal blood vessel hypertension, and fluid accumulation in the peritoneal cavity (Colley et al. 2014; WHO 2022).
Prevention and Control
Use of vaccines historically has been considered the most economical way to prevent infectious diseases. However, no vaccine for human schistosomiasis is currently available (Molehin 2020). The prevention and control of this disease primarily relies on alternative measures such as avoiding water sources infested with Schistosoma parasites and eliminating the snail population through use of molluscicides (Inobaya et al. 2014; De Albuquerque et al. 2020). In endemic regions, the avoidance of water sources is not always possible. Therefore, the WHO recommends the use of preventative chemotherapy to control this disease through mass drug administration of the anthelmintic drug praziquantel (Inobaya et al. 2014; WHO 2022).
Treatment Options
The WHO estimated that 236 million people required treatment for bilharzia in 2019. Roughly 90% of these people live in Africa. The primary treatment option available consists of a racemic mixture of (\(\pm )\)-praziquantel, which was approved in 1982 in the USA, and is sold under the brand name Biltricide. The activity of praziquantel is based almost exclusively on R-praziquantel (1) and that neither S-praziquantel nor the metabolites significantly contribute to the therapeutic effect (Meister et al. 2014). Praziquantel is efficacious against all etiological Schistosoma species (Summers et al. 2022). Two alternatives, (\(\pm )\)-oxamniquine (2) and metrifonate (3), however, are active only against S. haematobium and S. mansoni, respectively (Xiao et al. 2018). Besides their restricted bioactivity, drawbacks including ineffectiveness and emerging drug resistance for oxamniquine (da Silva et al. 2017), and logistical, including toxicity, problems for metrifonate led to the removal of the latter from the WHO’s list of essential medicines, and doubt exists for the future use of the former (Fenwick and Utzinger 2017).

Praziquantel has thus become the first-line treatment for schistosomiasis and is now recorded on the WHO’s list of essential medicines (Liu et al. 2011; WHO 2019). It is generally seen as a safe and effective medication and is therefore included in various control programmes (Center for Disease Control and Prevention 2018; McManus et al. 2018). The main disadvantage of praziquantel is its ineffectiveness against the immature and egg phases of the flatworms (Xiao et al. 2018; WHO 2019). Even though it is considered the safest among all anthelmintic drugs, the potential for the emergence of drug resistance and its ineffectiveness against the immature and egg phases of the parasite warrant a search for new drugs that will be effective against all stages (Cioli et al. 2014).
Over the years, medicinal plants have served as traditional remedies for treating various ailments, including parasitic diseases (Kingston and Cassera 2022). One such plant species without a doubt is Artemisia annua L., Asteraceae, or sweet wormwood, which has been used to treat malaria in the form of tea, pressed juice, or an infusion (Mueller et al. 2000; Sadiq et al. 2013; Septembre-Malaterre et al. 2020). However, A. annua is not only against malaria (Mesa et al. 2015; Feng et al. 2020) but also displays activity against various parasitic diseases such as leishmaniasis (Machín et al. 2021), trypanosomiasis (Naβ and Efferth 2018), and schistosomiasis (Gruessner et al. 2019). Artemisinin, the antimalarial compound explicitly isolated from A. annua leaves, has also shown antischistosomal activity and its derivatives artemether and artesunate are approved for use as prophylactic schistosomal drugs by the Chinese Ministry of Health (Liu et al. 2011; Bergquist and Elmorshedy 2018).
The aim of the present review was, therefore, to provide a comprehensive overview on in vitro and in vivo studies conducted with Artemisia species against schistosomiasis, as well as artemisinin (4) and its derivatives tested for antischistosomal activities. A systematic review is presented where all available information regarding scientific research that has been conducted on Artemisia species, artemisinin, and its derivatives against Schistosoma as well as the snail vectors is discussed.
Search Strategy
This literature review was compiled by searching five scientific databases: Elsevier ScienceDirect, Scopus, Web of Science, Google Scholar, and PubMed were search using the terms “Artemisia AND Schistosomiasis” and “artemisinin AND Schistosomiasis”. Literature published in English from 2012 until August 2022 were also considered to include the most recently conducted studies. The titles and abstracts of all retrieved publications were first reviewed for relevance. Then, the full text of the selected papers was further consulted. All duplicates were excluded. All papers that included preclinical studies that have been conducted with Artemisia species and schistosomiasis, as well as artemisinin and its derivatives against schistosomiasis, were considered.
Discussion
The Genus Artemisia
The Artemisia genus, Asteraceae, comprises around 600 species distributed across all continents except Antarctica (Funk et al. 2005; Vallès et al. 2011). The species in this genus serves multiple purposes, such as being used as ornamentals, spices, and most importantly, traditional remedies in treating various ailments. The two best known species are Artemisia absinthium L., “wormwood”, and A. annua L., “Qinghao” in traditional Chinese medicine, whereby the former is used for treating gastrointestinal disorders and controlling pain during childbirth, and the latter for treating cough, cold, diarrhoea, fever, and malaria (Nigam et al. 2019).
Asia has the greatest number of Artemisia spp., with around 150 species found in China, 50 species in Japan, and approximately 174 species in Russia (Taleghani et al. 2020). In Africa, A. afra Jacq. is prevalent and is distributed across Kenya, Tanzania, Uganda, and as far north as Ethiopia. It is a very common plant and is widely distributed throughout South Africa, Namibia, and Zimbabwe (Liu et al. 2009; Kane et al. 2019). A few species are also found in South America (Abad et al. 2012). Species of this genus may be perennial, biennial, or annual herbs, subshrub or shrubs and are usually quite fragrant, with upright or ascending, sometimes decumbent stems (Taleghani et al. 2020).
Scientific studies on Artemisia species have led to the identification of many compounds (Abad et al. 2012), with roughly six hundred compounds from A. annua alone having been identified (Brown 2010). This genus contains chemical constituents from various chemical classes such as terpenoids, phenolics, coumarins, steroids, flavonoids, monoterpenoids, triterpenoids, sesquiterpenoids, and sesquiterpene lactones (Shahrajabian et al. 2020). As can be expected, the chemical constituents differ between the different Artemisia species, as well as within the same species depending on time of collection, and collection sites, among other factors (Bilia 2014; Zhang et al. 2017). The distinct difference in chemical profiles enables the same species to be used for different purposes in different locations (Zhang et al. 2017).
Artemisinin and Derivatives
In 1972, the bioactive compound artemisinin (4), a sesquiterpene lactone with a 1,2,4-trioxane ring, was first isolated from A. annua and it was shown to have powerful antimalarial properties. This compound and its semisynthetic derivatives are now used worldwide for the treatment of malaria. Artemisinin is still mainly obtained by isolation from A. annua, with Vietnam and China roughly producing 80% of the global supply. However, the production of artemisinin is not sufficient to meet global requirements, and demand continues to outstrip supply. This problem will be aggravated once artemisinin and its derivatives are adopted for treatment of other diseases including cancer, other parasitic diseases such as bilharzia, and viral infections. The semisynthetic derivatives currently used are dihydroartemisinin (5), artemether (6), and artesunate (7) that were first prepared by Chinese scientists from artemisinin. Because of their short pharmacological half-lives, they are used in fixed-dose artemisinin combination therapies (ACTs) with longer half-life antimalarial medications such as mefloquine, piperaquine, and pyronaridine, among others (Wells 2010; Angus 2014; Meiyi and Guoqiao 2017).

New hybrids derived from praziquantel/artemisinin derivatives with dual action represent an interesting strategy in the development of new and more effective schistosomicidal agents with reduced risk of drug resistance (Duan et al. 2012). Derivative DW-3-15 (8) was prepared by binding the artesunate to praziquantel by inserting a hydroxyl group at position C-10 in praziquantel. Its activity against the young worms is comparable to that of artesunate, but significantly higher than praziquantel. More importantly, the derivative has the same effectiveness as praziquantel against adult S. japonicum (Dong et al. 2014).

Antischistosomal and Molluscicidal Activities
Extracts and Infusions
Methanolic extracts prepared from 45 Egyptian plant species, including A. monosperma Delile, were screened for their in vitro antischistosomal and antimicrobial activities against adult S. mansoni worms and microorganisms, respectively. The A. monosperma extract, at a concentration of 200 µg/ml, showed moderate antischistosomal activity after a 24-h incubation period (Abdel-Hameed et al. 2008).
Extracts of Solanum villosum Mill. (syn. S. sinaicum Boiss), Solanaceae, and A. judaica Lour. have been screened for their molluscicidal potencies against Biomphalaria alexandrina snails (S. mansoni–specific intermediate hosts) and their eggs (Bakry et al. 2011). The most toxic to the snails were the ethanolic extracts of S. siniacum (LC50 14.8 ppm), while A. judaica required twice the concentration for its lethal dose (LC50 38 ppm). These two extracts were further subjected to tests against the snails’ reproduction rate (R0), fecundity (Mx), and S. mansoni miracidia infectivity. A significant reduction in snail reproduction (73.69%), survival (52%), and fecundity (12.2 eggs/snail) rates were observed after B. alexandrina snails were exposed to LC25 (32 ppm) of an ethanolic extract of A. judaica. Also, a considerable reduction (46.15%) in the snails infected with S. mansoni miracidia was observed. Also, a reduction in the number of cercariae per snail (710 ± 11.1), prepatent period (22.7 ± 2.2 days), and shedding duration (6.2 ± 1.23 days) were observed. The authors of the study concluded that LC25 (32 ppm) of A. judaica ethanolic extract could be useful in snail control.
Crude extracts of A. absinthium L. and Tanacetum parthenium Sch.Bip. were assayed for their schistosomicidal activities in vitro against adult S. mansoni worms at concentrations of 12.5, 25, 50, 100, and 200 µg/ml. After incubation periods of 24, 48, and 72 h, A. absinthium at 200 µg/ml caused 100% mortality of all S. mansoni worms, as well as a significant reduction in motor activity and tegumental alterations in all worms. The same effects were also observed at 50 µg/ml and 100 µg/ml concentrations of A. absinthium after 48- and 72-h incubations. Extracts of A. absinthium submitted to chromatographic fractionation provided two pure compounds, artemetin and hydroxypelenolide. However, assay of the compounds against S. mansoni adult worms at 100 µM indicated that these were inactive (de Almeida et al. 2016).
An ethanolic extract of the leaves of A. dubia Wall. was screened in vitro for its molluscicidal activity against juvenile and mature Oncomelania hupensis quadrasi (S. japonicum–specific intermediate snail host) (Tercinõ et al. 2020). Different concentrations of the ethanolic extract were used in the molluscicidal assay against mature and juvenile snails. Even though the exact method of sample preparation and dilution was not apparent, they reported that the highest concentration (6.3%) of the A. dubia ethanolic extract against the mature snails displayed a mortality rate of 92%, which was statistically comparable with the positive control, niclosamide (p > 0.05). For the juvenile snails, mortality rates of 94, 95, and 98% were obtained with concentrations of 10, 11.22, and 12.59% of the A. dubia ethanolic extract, respectively. These results were also statistically comparable with the positive control (p > 0.05). The ethanolic A. dubia extract was also profiled for its secondary metabolites, which revealed tannins, saponins, and terpenoids. The molluscicidal activity of the ethanolic A. dubia extract may thus be attributed to these secondary metabolites, either independently or in combination.
Methanolic and aqueous extracts of A. annua were evaluated for their mortality effects on Biomphalaria pfeifferi (S. mansoni–specific intermediate snail host) and inhibitory effects against the shedding of S. mansoni cercariae after 24 h of exposure. Inhibitory effects at the highest concentrations were 63.06% ± 1.84 at 1.77 mg/µl and 55.75% ± 1.94 at 2.73 mg/µl for the methanolic and aqueous extract, respectively. Inhibitions of 22.41% ± 2.17 and 21.80% ± 1.45 were obtained, respectively, for the lowest concentrations of the methanolic (0.12 mg/µl) and aqueous (0.23 mg/µl) extracts. The effects on cercariae in B. pfeifferi snails were concentration dependent, and a substantial difference (p < 0.05) existed between the mean of the treatment group and that of the control group (Ado et al. 2021).
The prophylactic effects of traditional A. annua extract and artemisinin itself were evaluated in experimental mice infected with S. japonicum cercariae (40 ± 1). Mice were given 300 mg/kg A. annua extract once a week for a total of 4 weeks, commencing at day 7 post-infection. The mice in the artemisinin prevention group were treated the same as those in the A. annua extract group. The artemisinin content in the A. annua extract was roughly 20%, measured by HPLC. Both artemisinin and the A. annua extract had extremely significant (p < 0.0001) worm and egg reduction rates. Artemisinin reduced worms and liver eggs by 95.65 and 98.40%, respectively, and the A. annua extract by 98.26 and 100%, respectively. No pathological changes were detected in the treated mice, and their physiological indexes were consistent with the normal control group’s mice, which indicates the efficacy of artemisinin and the A. annua extract in curing and preventing schistosomiasis (Yang et al. 2022).
Studies in vitro and in vivo evaluated the antischistosomal activities of crude aqueous extracts of A. annua, Nigella sativa L., Ranunculaceae, and Allium sativum L., Amaryllidaceae, against Egyptian strains of S. mansoni (Fadladdin 2022). The in vitro study included the evaluation of different concentrations of aqueous plant extracts against adult S. mansoni worms of both sexes. The mating, motility rate, and mortality of the treated worms were monitored and recorded at certain time points throughout a 48-h incubation period. The A. annua extract at concentrations of 125, 250, and 500 μg/ml showed a slight decrease in the worms’ motility. Regarding mating, about 89% of worms were separated in the first 2 h at the highest concentrations (250 and 500 μg/ml) of the A. annua extract. At concentrations of 125 and 62.5 μg/ml, 77% were separated after 4 h, and 55% were separated after 12 h at the lowest concentration (31.25 μg/ml) of the A. annua extract. The mortality effects of the extracts were directly dependent on the concentrations used and the duration of incubation. One hundred percent of the adult S. mansoni worms were killed after 6, 12, and 24 h of incubation with 500, 250, and 125 μg/ml of the A. annua extract, respectively. The A. annua extract was the most effective extract compared to the effects of the other extracts on the adult worms. The in vivo study involved 30 adult S. mansoni–infected hamsters, which were divided into 6 treatment groups. The hamsters in the A. annua treatment group received an oral dose of 300 mg/kg aqueous A. annua extract. After treatment, the hamsters were slaughtered, and their kidneys, livers, and spleens were examined for granulomas. After treatment with all plant extracts, including A. annua, the hamsters’ tissues revealed calcification, a reduction in the size of granulomas, as well as damage to the eggs of the S. mansoni worms in the spleen and liver.
Crude aqueous, methanol, hexane, and acetone extracts of seven traditional Kenyan medicinal plants, including A. annua, were screened against newly transformed schistosomula (NTS) and adult S. mansoni worms at 100 μg/ml. After a 24-h exposure, the A. annua acetone extracts compared to the negative control exhibited a remarkable 97.9% decrease in the viability of S. mansoni NTS. Moreover, adult S. mansoni worm exposure to A. annua acetone extracts resulted in a 48% reduction in worm viability at 24 h, which increased by ± 10% at 48 h. Far lower killing activity against NTS were exerted by the methanol and hexane A. annua extracts, which were thus excluded from the adult worm assay. Terpenoids, steroids, and anthraquinones were identified by chemical analysis as the main compounds present in the A. annua acetone extracts (Ndegwa et al. 2022). These results signify that the acetone A. annua possesses potent S. mansoni NTS mortality activity.
Traditional aqueous infusions, dichloromethane (DCM), and hexane extracts, as well as organic extracts of the infusions of A. afra and A. annua, were tested against NTS and mature S. mansoni worms in vitro (Taljaard et al. 2022). Overall, the aqueous infusions as well as the organic extracts (DCM and hexane) of both Artemisia spp. exhibited good activity against NTS at 100 µg/ml, after a 72-h treatment period. The organic extracts of A. afra exhibited potent IC50 values of 1.8 µg/ml (hexane) and 1.7 µg/ml (DCM) against NTS. Compared to praziquantel (IC50 1.5 µg/ml), both of these organic extracts were remarkably active against NTS. Infusions and extracts of A. afra were also submitted to assays with mature S. mansoni worms. After 24, 48, and 72 h of treatment, both organic extracts of A. afra showed total clearance (100% inhibition) of mature worms at 100 µg/ml. Moderate IC50 values of 10.4 µg/ml and 8.9 µg/ml were also obtained for the A. afra hexane and DCM extracts, respectively.
Antischistosomal Activity
In Vitro and In Vivo Activities
Immunomodulation and inflammation are responses to many infectious diseases, including schistosomiasis (Gruessner et al. 2019). Immunomodulation directly influences the pathogenesis of this disease, as it is responsible for activating changes in the profile of humoral and cellular immune responses in the human host via triggering complex mechanisms, which are dependent on the sensitization of CD4 + T cells (Schwartz and Fallon 2018). Artemisinin alone has demonstrated a potent anti-inflammatory activity (Zhu et al. 2012; Kim et al. 2015; Shi et al. 2015; Wang et al. 2017). This anti-inflammatory capacity is the result of the inhibition of pro-inflammatory cytokine expression, such as TNF-α and IL-6, by blocking the NF-κB and MAPK signaling cascades (Zhu et al. 2012; Wang et al. 2017), as illustrated in Fig. 2.
Artemisinin inhibition of inflammation through NF-κB and MAPK signaling cascades in human host cells after parasite infection. Abbreviations: TNF-α tumor necrosis factor alpha, NF-kB nuclear factor kappa-light-chain-enhancer of activated B cells, MAPK mitogen-activated protein kinases, IKK I kappa B kinase, IkB-alpha inhibitor of kappa B alpha, Ub ubiquitin, Yellow p’s indicate phosphorylation of protein, ERK extracellular signal-regulated kinases, JNK c-Jun N-terminal kinases. Reproduced from Gruessner et al. 2019 with permission by Springer
Artesunate (7) has been evaluated for its effects on schistosome cytochrome-C peroxidase (CcP) and thioredoxin glutathione reductase (TGR). The inhibition of these two defensive enzymes makes the parasite vulnerable during its different stages to the attack by the host generated reactive oxygen species (Abdin et al. 2013). In an in vivo study with Swiss albino mice infected with S. mansoni, 4 groups of 50 mice each comprising a control group, an artesunate treatment group, a praziquantel treatment group, and a group treated with artesunate followed by praziquantel were used. The artesunate and praziquantel monotherapy groups revealed a much lower decrease in total worm count than the combined AS-praziquantel treatment group. Furthermore, the combined artesunate-praziquantel therapy also remarkably eliminated all tissue eggs, whereas reduction rates of 68.4% and 95.4% were recorded in the praziquantel and artesunate treatment groups, respectively. A significant reduction in expression of schistosome CcP and TGR was revealed by semiquantitative rt-PCR values in mice treated with artesunate compared to those in the control group. In this context, the present results revealed that praziquantel had no effect on expression of schistosome TGR and CcP; however, praziquantel has been established to cause intense muscular paralysis due to a rapid influx of calcium ions in the parasites. Therefore, this combination therapy comprising artesunate and praziquantel may completely cure schistosomiasis (Abdin et al. 2013).
The antischistosomal efficacies of different dosing protocols of the artemisinin-naphthoquine phosphate (ANP) combination against S. mansoni in its juvenile and adult stages were evaluated (El-Beshbishi et al. 2013a). Infected mice treated with a single oral dose of 400 mg/kg ANP on the 7th day post-infection (p.i.) had a 95.07% reduction in worms. No eggs could be found in the liver and the intestines after mice were treated with 600 mg/kg on the 21st day p.i., due to the mortality of all female worms. Mice treated with the same dose (600 mg/kg) on the 42nd day p.i. revealed 94.17 and 93.36% reductions in female and total worm burdens, respectively. For intestinal and hepatic tissue egg loads, 76.73 and 80.18% reductions, respectively, were observed with ANP combination treatment.
In a separate study, ANP was evaluated in vitro against adult S. mansoni worms (Egyptian strain), free larvae, and B. alexandrina snails (El-Beshbishi et al. 2015). The dose effect of ANP in response to time was assessed, resulting in 100% mortality of all S. mansoni worms at 40 and 20 µg/ml ANP after incubation periods of 48 and 72 h, respectively. The molluscicidal effects at a LC50 value of 16.8 µg/ml caused complete mortality of S. mansoni cercariae and miracidia after 15 and 90 min, respectively. After a 24-h incubation, all adult B. alexandrina snails exposed to 40 µg/ml ANP were killed and therefore shows promising antischistosomicidal and molluscicidal potential.
Likewise, the antischistosomal activity of artemether against the early juvenile stages and mature stages of S. mansoni in infected mice was evaluated (El-Beshbishi et al. 2013b). A single oral dose of 400 mg/kg artemether was administered to the mice at three time points (days 7, 21, and 49 p.i.). After the first treatment point (day 7 p.i.), the mean worm burden was reduced by 85.94%. The most significant reductions were obtained after the second treatment point (day 21 p.i.), where 90.57 and 91.52% of female and mean worm burdens were reduced, respectively. Lower reduction rates of 66.51 and 55.17% were obtained for the female and mean worm burdens, respectively, at the last treatment point (day 49 p.i.). Additionally, artemether treatment also led to a significant decrease in tissue egg load and altered the oogram patterns within the mice, while killing more eggs and reducing the numbers of juvenile eggs. The authors concluded that artemether possessed significant schistosomicidal activities, especially against schistosomulae older than 21 days.
The immunomodulatory action of artemether compared to that of praziquantel in mice infected with S. mansoni has been evaluated by administration of a single intramuscular dose of 50 mg/kg artemether at 7, 14, 21, and 45 days p.i. (Madbouly et al. 2015). Optimal effects were observed during the interference of artemether treatment with schistosomula that were 14 or 21 days old. It was concluded that artemether causes a reduction in worm burden and therefore is a promising lead in the control of schistosomiasis.
The elimination of S. mansoni in infected mice by slow release of artemisone (9), an artemisinin derivative with an amino-substituted group at C-10, has been demonstrated (Gold et al. 2017). Various dosage regimes were evaluated, namely, artemisone suspension administered by (i) gavage (400–450 mg/kg); (ii) subcutaneous injection of a gel containing artemisone (115–120 mg/kg); (iii) subcutaneous insertion of artemisone incorporated in a solid polymer (56–60 mg/kg); and (iv) intraperitoneal injection of artemisone solubilized in DMSO (115–120 mg/kg). Strong antischistosomal effects of 73.1 and 95.9% reduction in mice treated with artemisone in gel 7 and 14, and 21, 28 and 35 days p.i. were found. The results indicate that artemisone has potent antischistosomal activity and seems effective in treating hosts harboring juvenile schistosomes, before egg-deposition and induction of deleterious immune responses.

Perspectives and Future Directions
Schistosomiasis affects millions of lives mainly in tropical regions and accounts for many deaths each year. In combination with other neglected tropical diseases, it not only causes human suffering, but it is also having a profound negative impact on economic activity in these regions. Therefore, controlling and/or eliminating schistosomiasis will have to focus on the reduction of snail populations as well as the development of safer and more effective treatment options. Novel antischistosomal drugs are needed, and the genus Artemisia, as presented in this review, seems to be a promising source. Work published within the last few years has revealed several promising results regarding Artemisia species (Table S2) and their constituents, and especially with artemisinin and its derivatives (Table S3) against either the snail vectors, adult worms, or developing larvae of Schistosoma species. Given the remarkable antiparasitic activity of artemisinin and its derivatives, it is of concern that so little research has been conducted on Artemisia spp. as a possible source for new drug leads for the treatment of neglected diseases. Interestingly, it does appear that A. afra seems to be more active than A. annua and/or artemisinin (Taljaard et al. 2022). It is known that A. afra does not contain the compound artemisinin, and clearly one or more compounds possessing antiparasitic activity are biosynthesised by A. afra. It is of importance to identify these compound(s) in A. afra and further investigate other Artemisia spp. for bioactivity against schistosomiases.
Conclusions
Artemisia afra, A. annua, and artemisinin derivatives seem to be the most promising avenue for further scientific investigation, but it must be noted that only six Artemisia species, out of the approximately 600 species distributed worldwide, have been tested for activity against schistosomiasis or its vectors. It can therefore be concluded that this promising genus, which has already yielded the valuable antiparasitic compound artemisinin, is completely understudied and deserves more intense scientific scrutiny in order to identify possible new effective and safe treatment options for schistosomiases.
Data Availability
The data that supports the findings of this study are available upon request.
References
Abad MJ, Bedoya LM, Apaza L, Bermejo P (2012) The Artemisia L. genus: a review of bioactive essential oils. Molecules 17:2542–2566. https://doi.org/10.3390/molecules17032542
Abdel-Hameed ES, El-Nahas HA, Abo-Sedera SA (2008) Antischistosomal and antimicrobial activities of some Egyptian plant species. Pharm Biol 46:626–633. https://doi.org/10.1080/13880200802179543
Abdin AA, Dalia SA, Shoheib ZS (2013) Artesunate effect on schistosome thioredoxin glutathione reductase and cytochrome c peroxidase as new molecular targets in Schistosoma mansoni-infected mice. Biomed Environ Sci 26:953-61. https://doi.org/10.3967/bes2013.030
Ado IM, Ali ZA, Dogara MM, Abdullahi K, Luka SA, Nock HI, Ndams IS, Madara AA (2021) Mortality and inhibitory effects of aqueous and methanolic extracts of Artemisia annua L. on Biomphalaria pfeifferi (Krauss) and shedding of cercariae. Niger J Parasitol 42:25–30. https://doi.org/10.4314/njpar.v42i1.4
Angus B (2014) Novel anti-malarial combinations and their toxicity. Expert Rev Clin Pharmacol 7:299–316. https://doi.org/10.1586/17512433.2014.907523
Bakry FA, Mohamed RT, El-Hommossany K (2011) Biological and biochemical responses of Biomphalaria alexandrina to some extracts of the plants Solanum siniacum and Artemisia judaica L. Pestic Biochem Physiol 99:174–180. https://doi.org/10.1016/j.pestbp.2010.12.001
Bekana T, Abebe E, Mekonnen Z, Tulu B, Ponpetch K, Liang S, Erko B (2022) Parasitological and malacological surveys to identify transmission sites for Schistosoma mansoni in Gomma District, south-western Ethiopia. Sci Rep 12:17063. https://doi.org/10.1038/s41598-022-21641-2
Bergquist R, Elmorshedy H (2018) Artemether and praziquantel: origin, mode of action, impact, and suggested application for effective control of human schistosomiasis. Trop Med Infect Dis 3:125. https://doi.org/10.3390/tropicalmed3040125
Bilia AR (2014) Science meets regulation. J Ethnopharmacol 158:487–494. https://doi.org/10.1016/j.jep.2014.06.036
Boissier J, Moné H, Mitta G, Bargues MD, Molyneux D, Mas-Coma S (2015) Schistosomiasis reaches Europe. Lancet Infect Dis 15:757–758. https://doi.org/10.1016/s1473-3099(15)00084-5
Brown GD (2010) The biosynthesis of artemisinin (qinghaosu) and the phytochemistry of Artemisia annua L. (qinghao). Molecules 15:7603–7698. https://doi.org/10.3390/molecules15117603
Caffrey CR (2007) Chemotherapy of schistosomiasis: present and future. Curr Opin Chem Biol 11:433–439. https://doi.org/10.1016/j.cbpa.2007.05.031
Centers for Disease Control and Prevention (2018) Parasites - schistosomiasis. https://www.cdc.gov/parasites/schistosomiasis/treatment.html. Accessed 11 Oct 2022
Centers for Disease Control and Prevention (2019) DPDx – laboratory identification of parasites of public health concern, schistosomiasis, parasite Biology. https://www.cdc.gov/dpdx/schistosomiasis/index.html. Accessed 13 Sept 2022
Cioli D, Pica-Mattoccia L, Basso A, Guidi A (2014) Schistosomiasis control: praziquantel forever? Mol Biochem Parasitol 195:23–29. https://doi.org/10.1016/j.molbiopara.2014.06.002
Colley DG, Bustinduy AL, Secor WE, King CH (2014) Human schistosomiasis. Lancet 383:2253–2264. https://doi.org/10.1016/s0140-6736(13)61949-2
da Silva VBR, Campos BR, de Oliveira JF, Decout JL, de Lima MD (2017) Medicinal chemistry of antischistosomal drugs: praziquantel and oxamniquine. Bioorg Med Chem 25:3259–3277. https://doi.org/10.1016/j.bmc.2017.04.031
de Albuquerque RDDG, Mahomoodally MF, Lobine D, Suroowan S, Rengasamy KR (2020) Botanical products in the treatment and control of schistosomiasis: recent studies and distribution of active plant resources according to affected regions. Biology 9:223. https://doi.org/10.3390/biology9080223
de Almeida LMS, Carvalho LSA, de Gazolla MC, Pinto PLS, Silva MPN, de Moraes J, Da Silva Filho AA (2016) Flavonoids and sesquiterpene lactones from Artemisia absinthium and Tanacetum parthenium against Schistosoma mansoni worms. Evid-Based Compl Alt Med 2016:9521349. https://doi.org/10.1155/2016/9521349
de Moraes J, de Oliveira RN, Costa JP, Junio ALG, de Sousa DP, Freitas RM, Allegretti SM, Pinto PLS (2014) Phytol, a diterpene alcohol from chlorophyll, as a drug against neglected tropical disease Schistosomiasis mansoni. PLoS Negl Trop Dis 8:2617. https://doi.org/10.1371/journal.pntd.0002617
Dong L, Duan W, Chen J, Sun H, Qiao C, Xia C (2014) An artemisinin derivative of praziquantel as an orally active antischistosomal agent. PLoS ONE 9:e112163. https://doi.org/10.1371/journal.pone.0112163
Duan W, Qiu S, Zhao Y, Sun H, Qiao C, Xia C (2012) Praziquantel derivatives exhibit activity against both juvenile and adult Schistosoma japonicum. Bioorg Med Chem Lett 22:1587–1590. https://doi.org/10.1016/j.bmcl.2011.12.133
El-Beshbishi SN, Taman A, El-Malky M, Azab MS, El-Hawary AK, El-Tantawy DA (2013a) In vivo effect of single oral dose of artemether against early juvenile stages of Schistosoma mansoni Egyptian strain. Exp Parasitol 135:240–245. https://doi.org/10.1016/j.exppara.2013.07.006
El-Beshbishi SN, Taman A, El-Malky M, Azab MS, El-Hawary AK, El-Tantawy DA (2013b) First insight into the effect of single oral dose therapy with artemisinin-naphthoquine phosphate combination in a mouse model of Schistosoma mansoni infection. Int J Parasitol 43:521–530. https://doi.org/10.1016/j.ijpara.2013.01.007
El-Beshbishi SN, El Bardicy S, Tadros M, Ayoub M, Taman A (2015) Spotlight on the in vitro effect of artemisinin-naphthoquine phosphate on Schistosoma mansoni and its snail host Biomphalaria alexandrina. Acta Trop 4:37–45. https://doi.org/10.1016/j.actatropica.2014.09.018
Enk MJ, Amorim A, Schall VT (2003) Acute schistosomiasis outbreak in the metropolitan area of Belo Horizonte, Minas Gerais: alert about the risk of unnoticed transmission increased by growing rural tourism. Mem Inst Oswaldo Cruz 98:745–750. https://doi.org/10.1590/s0074-02762003000600006
Fadladdin YAJ (2022) Evaluation of antischistosomal activities of crude aqueous extracts of Artemisia annua, Nigella sativa, and Allium sativum against Schistosoma mansoni in hamsters. Biomed Res Int 2022:1–14. https://doi.org/10.1155/2022/5172287
Feng X, Cao S, Qiu F, Zhang B (2020) Traditional application and modern pharmacological research of Artemisia annua L. Pharmacol Ther 216:107650. https://doi.org/10.1016/j.pharmthera.2020.107650
Fenwick A, Utzinger J (2017) Helminthic diseases: schistosomiasis. In: International Encyclopedia of Public Health (Second Edition). https://www.sciencedirect.com/science/article/pii/B9780128036785002071. Accessed 16 Nov 2022
Funk VA, Bayer RJ, Keeley S, Chan R, Watson L, Gemeinholzer B (2005) Everywhere but Antarctica: using a supertree to understand the diversity and distribution of the Compositae. Biol Skr 55:343–374
Gold D, Alian M, Domb A, Karawani Y, Jbarien M, Chollet J, Haynes RK, Wong HN, Buchholz V, Greiner A, Golenser J (2017) Elimination of Schistosoma mansoni in infected mice by slow release of artemisone. Int J Parasitol Drugs Drug Resist 7:241–247. https://doi.org/10.1016/j.ijpddr.2017.05.002
Gruessner BM, Cornet-Vernet L, Desrosiers MR, Lutgen P, Towler MJ, Weathers PJ (2019) It is not just artemisinin: Artemisia sp. for treating diseases including malaria and schistosomiasis. Phytochem Rev 18:1509–1527. https://doi.org/10.1007/s11101-019-09645-9
Inobaya MT, Olveda RM, Chau TN, Olveda DU, Ross AG (2014) Prevention and control of schistosomiasis: a current perspective. Res Rep Trop Med 2014:65–75. https://doi.org/10.2147/RRTM.S44274
Kane NF, Kyama MC, Nganga JK, Hassanali A, Diallo M, Kimani FT (2019) Comparison of phytochemical profiles and antimalarial activities of Artemisia afra plant collected from five countries in Africa. S Afr J Bot 125:126–133. https://doi.org/10.1016/j.sajb.2019.07.001
Kim WS, Choi WJ, Lee S, Kim WJ, Lee DC, Sohn UD, Shin HS, Kim W (2015) Anti-inflammatory, antioxidant and antimicrobial effects of artemisinin extracts from Artemisia annua L. Korean J Physiol Pharmacol 19:21–27. https://doi.org/10.4196/kjpp.2015.19.1.21
Kingston DGI, Cassera MB (2022). Antimalarial natural products. In: Kinghorn AD, Falk H, Gibbons S, Asakawa Y, Liu JK, Dirsch VM (eds) Antimalarial natural products. Progress in the Chemistry of Organic Natural Products, vol 117, Springer, Cham, pp 1–106. https://doi.org/10.1007/978-3-030-89873-1_1
Li EY, Gurarie D, Lo NC, Zhu X, King CH (2019) Improving public health control of schistosomiasis with a modified WHO strategy: a model-based comparison study. Lancet Glob Health 7:1414–1422. https://doi.org/10.1016/s2214-109x(19)30346-8
Lingscheid T, Kurth F, Clerinx J, Marocco S, Trevino B, Schunk M, Muñoz J, Gjørup IE, Jelinek T, Develoux M, Fry G (2017) Schistosomiasis in European travelers and migrants: analysis of 14 years TropNet surveillance data. Am J Trop Med Hyg 97:567–574. https://doi.org/10.4269/ajtmh.17-0034
Liu R, Dong H-F, Guo Y, Zhao Q-P, Jiang M-S (2011) Efficacy of praziquantel and artemisinin derivatives for the treatment and prevention of human schistosomiasis: a systematic review and meta-analysis. Parasit Vectors 4:201. https://doi.org/10.1186/1756-3305-4-201
Liu NQ, Van der Kooy F, Verpoorte R (2009) Artemisia afra: a potential flagship for African medicinal plants? S Afr J Bot 75:185–195. https://doi.org/10.1016/j.sajb.2008.11.001
Machín L, Nápoles R, Gille L, Monzote L (2021) Leishmania amazonensis response to artemisinin and derivatives. Parasitol Int 80:102218. https://doi.org/10.1016/j.parint.2020.102218
Madbouly NA, Shalash IR, El Deeb SO, El Amir AM (2015) Effect of artemether on cytokine profile and egg induced pathology in murine Schistosomiasis mansoni. J Adv Res 6:851–857. https://doi.org/10.1016/j.jare.2014.07.003
McManus DP, Dunne DW, Sacko M, Utzinger J, Vennervald BJ, Zhou X-N (2018) Schistosomiasis. Nat Rev Dis Primers 4:13. https://doi.org/10.1038/s41572-018-0013-8
Meister I, Ingram-Sieber K, Cowan N, Todd M, Robertson MN, Meli C, Patra M, Gasser G, Keiser J (2014) Activity of praziquantel enantiomers and main metabolites against Schistosoma mansoni. Antimicrob Agents Chemother 58:5466–5472. https://doi.org/10.1128/AAC.02741-14
Meiyi Z, Guoqiao L (2017) Dihydroartemisinin. In: Li G, Li Y, Li Z, Zeng M (eds) Artemisinin-based and other antimalarials: detailed account of studies by Chinese scientists who discovered and developed them. Academic Press, London, pp 23-24
Mesa LE, Lutgen PP, Velez ID, Segura A, Robledo SM (2015) Artemisia annua L., potential source of molecules with pharmacological activity in human diseases. Am J Phytomed Clin Ther 3:436–450
Molehin AJ (2020) Schistosomiasis vaccine development: update on human clinical trials. J Biomed Sci 27:28. https://doi.org/10.1186/s12929-020-0621-y
Mueller MS, Karhagomba IB, Hirt HM, Wemakor E (2000) The potential of Artemisia annua L. as a locally produced remedy for malaria in the tropics: agricultural, chemical and clinical aspects. J Ethnopharmacol 73:487–493. https://doi.org/10.1016/S0378-8741(00)00289-0
Murta FLG, Massara CL, Nogueira JFC, dos Santos Carvalho O, de Mendonça CLF, Pinheiro VAO Enk MJ (2016) Ecotourism as a source of infection with Schistosoma mansoni in Minas Gerais, Brazil. Trop Dis Travel Med Vaccines 2:3 https://doi.org/10.1186/s40794-016-0019-8
Naß J, Efferth T (2018) The activity of Artemisia spp. and their constituents against Trypanosomiasis. Phytomedicine 47:184–191. https://doi.org/10.1016/j.phymed.2018.06.002
Ndegwa FK, Kondam C, Aboagye SY, Esan TE, Waxali ZS, Miller ME, Gikonyo NK, Mbugua PK, Okemo PO, Williams DL, Hagen TJ (2022) Traditional Kenyan herbal medicine: exploring natural products’ therapeutics against schistosomiasis. J Helminthol 96:16. https://doi.org/10.1017/S0022149X22000074
Nigam M, Atanassova M, Mishra AP, Pezzani R, Devkota HP, Plygun S, Salehi B, Setzer WN, Sharifi-Rad J (2019) Bioactive compounds and health benefits of Artemisia species. Nat Prod Commun 14:1934578X1985035. https://doi.org/10.1177/1934578x19850354
Ojo JA, Adedokun, SA, Akindele AA, Olorunfemi AB, Otutu OA, Ojurongbe TA, Thomas BN, Velavan TP, Ojurongbe O (2021) Prevalence of urogenital and intestinal schistosomiasis among school children in South-west Nigeria. PLoS Negl Trop Dis 15:e0009628. https://doi.org/10.1371/journal.pntd.0009628
Ross AGP, Chau TN, Inobaya MT, Olveda RM, Li Y, Harn DA (2017) A new global strategy for the elimination of schistosomiasis. Int J Infect Dis 54:130–137. https://doi.org/10.1016/j.ijid.2016.09.023
Saber S, Alomar SY, Yahya G (2022) Blocking prostanoid receptors switches on multiple immune responses and cascades of inflammatory signaling against larval stages in snail fever. Environ Sci Pollut Res Int 29:43546–43555. https://doi.org/10.1007/s11356-022-20108-1
Sadiq A, Hayat MQ, Ashraf M (2013) Ethnopharmacology of Artemisia annua L.: a review. In: Aftab T, Ferreira J, Khan M, Naeem M (eds) Artemisia annua - pharmacology and biotechnology. Springer, Berlin, Heidelberg, pp 9–25. https://doi.org/10.1007/978-3-642-41027-7_2
Schwartz C, Fallon PG (2018) Schistosoma “eggs-iting” the host: granuloma formation and egg excretion. Front Immunol 29:2492. https://doi.org/10.3389/fimmu.2018.02492
Septembre-Malaterre A, Lalarizo Rakoto M, Marodon C, Bedoui Y, Nakab J, Simon E, Hoarau L, Savriama S, Strasberg D, Guiraud P, Selambarom J, Gasque P (2020) Artemisia annua, a traditional plant brought to light. Int J Mol Sci 21:4986. https://doi.org/10.3390/ijms21144986
Shahrajabian MH, Wenli S, Cheng Q (2020) Exploring Artemisia annua L., artemisinin and its derivatives, from traditional Chinese wonder medicinal science. Not Bot Horti Agrobot Cluj Napoca 48:1719–1741
Shi C, Li H, Yang Y, Hou L (2015) Anti-inflammatory and immunoregulatory functions of artemisinin and its derivatives. Med Inflamm 2015:435713. https://doi.org/10.1155/2015/435713
Summers S, Bhattacharyya T, Allan F, Stothard JR, Edielu A, Webster BL, Miles MA, Bustinduy AL (2022) A review of the genetic determinants of praziquantel resistance in Schistosoma mansoni: is praziquantel and intestinal schistosomiasis a perfect match? Front Trop Dis 3. https://doi.org/10.3389/fitd.2022.933097
Taleghani A, Emami SA, Tayarani-Najaran Z (2020) Artemisia: a promising plant for the treatment of cancer. Bioorg Med Chem 28:115180. https://doi.org/10.1016/j.bmc.2019.115180
Taljaard L, Probst A, Tornow R, Keiser J, Haynes RK, Van der Kooy F (2022) In vitro antischistosomal activity of Artemisia annua and Artemisia afra extracts. Phytomed Plus 2:100279. https://doi.org/10.1016/j.phyplu.2022.100279
Tercıño CC, Pradera CLM, Bagot MA (2020) Assessment of the molluscicidal activity of wormwood Artemisia dubia, Wallich leaves ethanolic extract on Oncomelania hupensis quadrasi, Möllendorff. Turk J Vet Anim Sci 44:377–381. https://doi.org/10.3906/vet-1907-10
Vallès J, Garcia S, Hidalgo O, Martín J, Pellicer J, Sanz M (2011) Biology, genome evolution, biotechnological issues and reserch including applied perspectives in Artemisia (Asteraceae). In: Kader J, Delseny M (eds) Advances in botanical research vol 60. Academic Press, Burlington, pp 349–419
Verjee MA (2020) Schistosomiasis: still a cause of significant morbidity and mortality. Res Rep Trop Med 10:153–163. https://doi.org/10.2147/rrtm.s204345
Wang KS, Li J, Wang Z, Mi C, Ma J, Piao LX, Xu GH, Li X, Jin X (2017) Artemisinin inhibits inflammatory response via regulating NF-κB and MAPK signaling pathways. Immunopharmacol Immunotoxicol 39:28–36. https://doi.org/10.1080/08923973.2016.1267744
Wells TN (2010) New medicines to improve control and contribute to the eradication of malaria. Malar J 9:I15. https://doi.org/10.1186/1475-2875-9-S2-I15
WHO (2019) World Health Organization Model List of Essential Medicines, 21 st List. World Health Organization, Geneva. https://apps.who.int/iris/rest/bitstreams/1237479/retrieve. Accessed 13 Sept 2022
WHO (2022) Schistosomiasis, World Health Organization. https://www.who.int/news-room/fact-sheets/detail/schistosomiasis. Accessed 13 Sept 2022
Xiao S-H, Sun J, Chen M-G (2018) Pharmacological and immunological effects of praziquantel against Schistosoma japonicum: a scoping review of experimental studies. Infect Dis Poverty 7:9. https://doi.org/10.1186/s40249-018-0391-x
Yang M, Xu Y, Sun J, Guo Y, Jia P, Mi R, Yan H, Zhu C (2022) Preventive effect of Artemisia annua extract on schistosomiasis. Res Sq 1:1–14. https://doi.org/10.21203/rs.3.rs-1579569/v1
Zhang X, Zhao Y, Guo L, Qiu Z, Huang L, Qu X (2017) Differences in chemical constituents of Artemisia annua L from different geographical regions in China. PLoS One 12:9. https://doi.org/10.1371/journal.pone.0183047
Zhu C, Xiong Z, Chen X, Peng F, Hu X, Chen Y, Wang Q (2012) Artemisinin attenuates lipopolysaccharide-stimulated proinflammatory responses by inhibiting NF-κB pathway in microglia cells. PLoS One 7:e35125. https://doi.org/10.1371/journal.pone.0035125
Acknowledgements
The authors are grateful to Pharmacen™, Centre of Excellence for Pharmaceutical Sciences, North-West University, for financial support.
Funding
Open access funding provided by North-West University.
Author information
Authors and Affiliations
Contributions
LT: conceptualisation, data analysis, and collection; writing the initial draft; editing the final draft. RKH: Reviewing and editing, checking of scientific accuracy. F.vdK: conceptualization, student supervision, reviewing and editing.
Corresponding author
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Taljaard, L., Haynes, R.K. & van der Kooy, F. Artemisia Species and Their Active Constituents for Treating Schistosomiasis. Rev. Bras. Farmacogn. 33, 875–885 (2023). https://doi.org/10.1007/s43450-023-00407-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43450-023-00407-5