Abstract
Vascular adhesion protein-1 (VAP-1) is a bifunctional protein that has the ability to catalyze the deamination of primary amines and is involved in the production of hydrogen peroxide, aldehydes, and advanced glycation end products (AGEs). VAP-1 is usually stored in intracellular vesicles of endothelial cells, smooth muscles, and adipocytes. It is responsible for leukocyte transmigration and adhesion. Overexpression of VAP-1 exacerbates oxidative stress and modulates a variety of inflammatory mediators linked with diabetic complications. Numerous studies have suggested the association of increased insulin levels with serum VAP-1 (sVAP-1). Preclinical research evidence suggests the increased activity of sVAP-1 in type 1 and 2 diabetes. Scientific reports on VAP-1 inhibitors have shown a reduction in severity in diabetic animal models. VAP-1 is a potential target of a therapeutically effective line of treatment for diabetes and diabetic complications such as nephropathy and retinopathy. The primary focus of this review is the role of VAP-1 in diabetes and its associated microvascular complications.
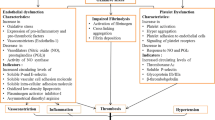
Graphical abstract

Similar content being viewed by others
Abbreviations
- ACR:
-
Acrolein
- AGE:
-
Advanced glycation end product
- AOC/SSAO:
-
Amine oxidase/semicarbazide-sensitive amine oxidase
- AOC:
-
Amine oxidase copper containing
- AOC1:
-
Amine oxidase copper containing 1
- AOC2:
-
Amine oxidase copper containing 2
- AOC3:
-
Amine oxidase copper containing 3
- AOC3KI:
-
AOC3 gene mutated
- AOC3KO:
-
AOC3 gene knock-out
- DM:
-
Diabetes mellitus
- DR:
-
Diabetic retinopathy
- ESRD:
-
End stage renal disease
- FPG:
-
Fasting plasma glucose
- GSH:
-
Glutathione
- HEV:
-
High endothelial venules
- ICAM-1:
-
Intercellular adhesion molecule-1
- IDF:
-
International diabetes federation
- IL-1β:
-
Interleukin 1-beta
- IL-6:
-
Interleukin-6
- LOX:
-
Lysyl oxidase
- mAb:
-
Monoclonal antibody
- MMP:
-
Matrix metalloproteinase
- NADPH:
-
Nicotinamide adenine dinucleotide phosphate
- NOD:
-
Non obese diabetic
- PDR:
-
Proliferative diabetic retinopathy
- sVAP-1:
-
Serum vascular adhesion protein-1
- T2DM:
-
Type II diabetes mellitus
- TNF-α:
-
Tumor necrosis factor-alpha
- TPQ:
-
Topaquinone
- VAP-1:
-
Vascular adhesion protein-1
- VEGF:
-
Vascular endothelial growth factor
References
Jalkanen S, Salmi M. A novel endothelial cell molecule mediating lymphocyte binding in humans. Behring Inst Mitt. 1993;92:36–43. PMID: 8250815
Merinen M, Irjala H, Salmi M, Jaakkola I, Hänninen A, Jalkanen S. Vascular adhesion protein-1 is involved in both acute and chronic inflammation in the mouse. Am J Pathol. 2005;166:793–800. https://doi.org/10.1016/S0002-9440(10)62300-0.
Yu PH, Wright S, Fan EH, Lun ZR, Gubisne-Harberle D. Physiological and pathological implications of semicarbazide-sensitive amine oxidase. Biochim Biophys Acta Proteins Proteom. 2003;1647:193–9. https://doi.org/10.1016/S1570-9639(03)00101-8.
Kaitaniemi S, Elovaara H, Grön K, Kidron H, Liukkonen J, Salminen T, et al. The unique substrate specificity of human AOC2, a semicarbazide-sensitive amine oxidase. Cell Mol Life Sci. 2009;66:2743–57. https://doi.org/10.1007/s00018-009-0076-5.
Finney J, Moon HJ, Ronnebaum T, Lantz M, Mure M. Human copper-dependent amine oxidases. Arch Biochem Biophys. 2014;546:19–32. https://doi.org/10.1016/j.abb.2013.12.022.
Jalkanen S, Salmi M. Cell surface monoamine oxidases enzymes in search of a function. EMBO. 2001;20:3893–901. https://doi.org/10.1093/emboj/20.15.3893
Unzeta M, Hernàndez-Guillamon M, Sun P, Solé M. Ssao/vap-1 in cerebrovascular disorders: a potential therapeutic target for stroke and alzheimer’s disease. Int J Mol Sci. 2021;22:1–30. https://doi.org/10.3390/ijms22073365.
Gharanei S, Fishwick K, Peter Durairaj R, Jin T, Siamantouras E, Liu KK, et al. Vascular adhesion protein-1 determines the cellular properties of endometrial pericytes. Front Cell Dev Biol. 2021;8:1–11. https://doi.org/10.3389/fcell.2020.621016.
Smith DJ, Vainio PJ. Targeting vascular adhesion protein-1 to treat autoimmune and inflammatory diseases. Ann N Y Acad Sci. 2007;1110:382–8. https://doi.org/10.1196/annals.1423.040.
Aalto K, Autio A, Kiss EA, Elima K, Nymalm Y, Veres TZ, et al. Siglec-9 is a novel leukocyte ligand for vascular adhesion protein-1 and can be used in PET imaging of inflammation and cancer. Blood. 2011;118(13):3725–33. https://doi.org/10.1182/blood-2010-09-311076.
Kivi E, Elima K, Aalto K, Nymalm Y, Auvinen K, Koivunen E, et al. Human Siglec-10 can bind to vascular adhesion protein-1 and serves as its substrate. Blood. 2009;114:5385–92. https://doi.org/10.1182/blood-2009-04-219253.
Enrique-Tarancon G, Castan I, Morin N, Marti L, Abella A, Camps M, et al. Substrates of semicarbazide-sensitive amine oxidase co-operate with vanadate to stimulate tyrosine phosphorylation of insulin-receptor-substrate proteins, phosphoinositide 3-kinase activity and GLUT4 translocation in adipose cells. Biochem J. 2000;350:171–80. https://doi.org/10.1042/0264-6021:3500171.
Koskinen K, Nevalainen S, Karikoski M, Hänninen A, Jalkanen S, Salmi M. VAP-1-deficient mice display defects in mucosal immunity and antimicrobial responses: implications for antiadhesive applications. J Immunol. 2007;179:6160–8. https://doi.org/10.4049/jimmunol.179.9.6160.
Toivonen R, Vanhatalo S, Hollmén M, Munukka E, Keskitalo A, Pietilä S, et al. Vascular adhesion protein 1 mediates gut microbial flagellin-induced inflammation, leukocyte infiltration, and hepatic steatosis. Sci. 2021;3:13. https://doi.org/10.3390/sci3010013.
Ferjančič Š, Gil-Bernabé AM, Hill SA, Allen PD, Richardson P, Sparey T, et al. VCAM-1 and VAP-1 recruit myeloid cells that promote pulmonary metastasis in mice. Blood. 2013;121:3289–97. https://doi.org/10.1182/blood-2012-08-449819.
Gerussi A, Carbone M, Invernizzi P. sVAP-1: a novel potential therapeutic target and marker for risk stratification in primary sclerosing cholangitis. J Lab Precis Med. 2017;2:72–72. https://doi.org/10.21037/jlpm.2017.09.04.
Shepherd EL, Karim S, Newsome PN, Lalor PF. Inhibition of vascular adhesion protein-1 modifies hepatic steatosis in vitro and in vivo. World J Hepatol. 2020;12:931–48. https://doi.org/10.4254/wjh.v12.i11.931.
Weston CJ, Shepherd EL, Claridge LC, Rantakari P, Curbishley SM, Tomlinson JW, et al. Vascular adhesion protein-1 promotes liver inflammation and drives hepatic fibrosis. J Clin Invest. 2015;125:501–20. https://doi.org/10.1172/JCI73722.
Becchi S, Buson A, Foot J, Jarolimek W, Balleine BW. Inhibition of semicarbazide-sensitive amine oxidase/vascular adhesion protein-1 reduces lipopolysaccharide-induced neuroinflammation. Br J Pharmacol. 2017;174:2302–17. https://doi.org/10.1111/bph.13832.
Jargaud V, Bour S, Tercé F, Collet X, Valet P, Bouloumié A, et al. Obesity of mice lacking VAP-1/SSAO by Aoc3 gene deletion is reproduced in mice expressing a mutated vascular adhesion protein-1 (VAP-1) devoid of amine oxidase activity. J Physiol Biochem. 2021;77:141–54. https://doi.org/10.1007/s13105-020-00756-y.
Silvola J, Virtanen H, Siitonen R, Hellberg S, Liljenbäck H, Metsälä O, et al. Leukocyte trafficking-associated vascular adhesion protein 1 is expressed and functionally active in atherosclerotic plaques. Sci Rep. 2016;6:1–10. https://doi.org/10.1038/srep35089.
Abella A, Garcia-Vicente S, Viguerie N, Ros-Baro A, Campus M, Palacin M, et al. Adipocytes release a soluble form of VAP-1/SSAO by a metalloprotease-dependent process and in a regulated manner. Diabetologia. 2004. https://doi.org/10.1007/s00125-004-1346-2.
Bono P, Jalkanen S, Salmi M. Mouse vascular adhesion protein 1 is a sialoglycoprotein with enzymatic activity and is induced in diabetic insulitis. Am J Pathol. 1999;155:1613–24. https://doi.org/10.1016/S0002-9440(10)65477-6.
Li HY, Lin HA, Nien FJ, Wu VC, Der JY, Chang TJ, et al. Serum vascular adhesion protein-1 predicts end-stage renal disease in patients with type 2 diabetes. PLoS ONE. 2016;11:1–14. https://doi.org/10.1371/journal.pone.0147981.
Li HY, Wei JN, Lin MS, Smith DJ, Vainio J, Lin CH, et al. Serum vascular adhesion protein-1 is increased in acute and chronic hyperglycemia. Clin Chim Acta. 2009;404:149–53. https://doi.org/10.1016/j.cca.2009.03.041.
Artasensi A, Pedretti A, Vistoli G, Fumagalli L. Type 2 diabetes mellitus: a review of multi-target drugs. Molecules. 2020;25:1–20. https://doi.org/10.3390/molecules25081987.
Papatheodorou K, Banach M, Bekiari E, Rizzo M, Edmonds M. Complications of diabetes 2017. J Diabetes Res. 2018;2018:10–3. https://doi.org/10.1155/2018/3086167.
Yraola F, Zorzano A, Albericio F, Royo M. Structure-activity relationships of SSAO/VAP-1 arylalkylamine-based substrates. ChemMedChem. 2009;4:495–503. https://doi.org/10.1002/cmdc.200800393.
Salmi M, Stolen C, Jousilahti P, Yegutkin GG. Insulin-regulated increase of soluble vascular adhesion protein-1 in diabetes. Am J Pathol. 2002;161:2255–62. https://doi.org/10.1016/S0002-9440(10)64501-4
DincgezCakmak B, Dundar B, KetenciGencer F, Yildiz DE, Bayram F, Ozgen G, et al. Assessment of relationship between serum vascular adhesion protein-1 (VAP-1) and gestational diabetes mellitus. Biomarkers. 2019;24:750–6. https://doi.org/10.1080/1354750X.2019.1684562.
Koc-Zorawska E, Malyszko J, Zbroch E, Malyszko J, Mysliwiec M. Vascular adhesion protein-1 and renalase in regard to diabetes in hemodialysis patients. Arch Med Sci. 2012;8:1048–52. https://doi.org/10.5114/aoms.2012.32413.
Kuo CH, Wei JN, Yang CY, Ou HY, Wu HT, Fan KC, et al. Serum vascular adhesion protein-1 is up-regulated in hyperglycemia and is associated with incident diabetes negatively. Int J Obes. 2019;43:512–22. https://doi.org/10.1038/s41366-018-0172-4.
Li HY, Der JY, Chang TJ, Wei JN, Lin MS, Lin CH, et al. Serum vascular adhesion protein-1 predicts 10-year cardiovascular and cancer mortality in individuals with type 2 diabetes. Diabetes. 2011;60:993–9. https://doi.org/10.2337/db10-0607.
Abella A, Marti L, Camps M, Claret M, Fernández-Alvarez J, Gomis R, et al. Semicarbazide-sensitive amine oxidase/vascular adhesion protein-1 activity exerts an antidiabetic action in Goto-Kakizaki rats. Diabetes. 2003;52:1004–13. https://doi.org/10.2337/diabetes.52.4.1004.
Tamura H, Miyamoto K, Kiryu J, Miyahara S, Katsuta H, Hirose F, et al. Intravitreal injection of corticosteroid attenuates leukostasis and vascular leakage in experimental diabetic retina. Investig Ophthalmol Vis Sci. 2005;46:1440–4. https://doi.org/10.1167/iovs.04-0905.
Inoue T, Morita M, Tojo T, Nagashima A, Moritomo A, Miyake H. Novel 1H-imidazol-2-amine derivatives as potent and orally active vascular adhesion protein-1 (VAP-1) inhibitors for diabetic macular edema treatment. Bioorgan Med Chem. 2013;21:3873–81. https://doi.org/10.1016/j.bmc.2013.04.011.
Murata M, Noda K, Fukuhara J, Kanda A, Kase S, Saito W, et al. Soluble vascular adhesion protein-1 accumulates in proliferative diabetic retinopathy. Investig Ophthalmol Vis Sci. 2012;53:4055–62. https://doi.org/10.1167/iovs.12-9857.
Murata M, Noda K, Kawasaki A, Yoshida S, Dong Y, Saito M, et al. Soluble vascular adhesion protein-1 mediates spermine oxidation as semicarbazide-sensitive amine oxidase: possible role in proliferative diabetic retinopathy. Curr Eye Res. 2017;42:1674–83. https://doi.org/10.1080/02713683.2017.1359847.
Matsuda T, Noda K, Murata M, Kawasaki A, Kanda A, Mashima Y, et al. Vascular adhesion protein-1 blockade suppresses ocular inflammation after retinal laser photocoagulation in mice. Investig Ophthalmol Vis Sci. 2017;58:3254–61. https://doi.org/10.1167/iovs.17-21555.
Abu El-Asrar AM, Mohammad G, Nawaz MI, Siddiquei MM, Van Den Eynde K, Mousa A, et al. Relationship between vitreous levels of matrix metalloproteinases and vascular endothelial growth factor in proliferative diabetic retinopathy. PLoS ONE. 2013;8:1–11. https://doi.org/10.1371/journal.pone.0085857.
Noda K, Nakao S, Zandi S, Engelstädter V, Mashima Y, Hafezi-Moghadam A. Vascular adhesion protein-1 regulates leukocyte transmigration rate in the retina during diabetes. Exp Eye Res. 2009;89:774–81. https://doi.org/10.1016/j.exer.2009.07.010.
Tékus V, Horváth ÁI, Csekő K, Szabadfi K, Kovács-Valasek A, Dányádi B, et al. Protective effects of the novel amine-oxidase inhibitor multi-target drug SZV 1287 on streptozotocin-induced beta cell damage and diabetic complications in rats. Biomed Pharmacother. 2021. https://doi.org/10.1016/j.biopha.2020.111105.
Yu PH, Zuo DM. Aminoguanidine inhibits semicarbazide-sensitive amine oxidase activity: implications for advanced glycation and diabetic complications. Diabetologia. 1997;40:1243–50. https://doi.org/10.1007/s001250050816.
Hoefman S, Snelder N, van Noort M, Garcia-Hernandez A, Onkels H, Larsson TE, et al. Mechanism-based modeling of the effect of a novel inhibitor of vascular adhesion protein-1 on albuminuria and renal function markers in patients with diabetic kidney disease. J Pharmacokinet Pharmacodyn. 2021;48:21–38. https://doi.org/10.1007/s10928-020-09716-x.
Wong M, Saad S, Zhang J, Gross S, Jarolimek W, Schilter H, et al. Semicarbazide-sensitive amine oxidase (SSAO) inhibition ameliorates kidney fibrosis in a unilateral ureteral obstruction murine model. Am J Physiol Renal Physiol. 2014;307(8):F908–16. https://doi.org/10.1152/ajprenal.00698.2013.
Wong MYW, Saad S, Wong MG, Stangenberg S, Jarolimek W, Schilter H, et al. Semicarbazide-sensitive amine oxidase inhibition ameliorates albuminuria and glomerulosclerosis but does not improve tubulointerstitial fibrosis in diabetic nephropathy. PLoS ONE. 2020;15:1–20. https://doi.org/10.1371/journal.pone.0234617.
Funding
This work did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
The article was conceptualized by YK and AS. AS wrote the manuscript. YK and AS finalized the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Singh, A.D., Kulkarni, Y.A. Vascular adhesion protein-1 and microvascular diabetic complications. Pharmacol. Rep 74, 40–46 (2022). https://doi.org/10.1007/s43440-021-00343-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43440-021-00343-y