Abstract
Purpose
To evaluate whether there is a mismatch between Risser staging and the proximal humerus ossification system (PHOS); and to analyze the correlation in the skeletal maturity stages between the two humeral epiphyses.
Methods
Data from patients aged 10 to 18 years with adolescent idiopathic scoliosis (AIS) seen between 2018 to 2021 were analyzed.
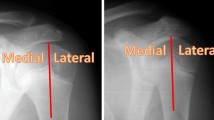
In an anteroposterior (AP) spine radiograph the ossification process was evaluated using the Risser classification method and bilateral PHOS (if both humeral epiphyses were visualized).
A mismatch between methods was defined as a Risser 0–1 (relatively skeletally immature) with a PHOS 4–5 (skeletally mature), or a Risser 2–5 (relatively skeletally mature) with a PHOS 1–3 (skeletally immature). The McNemar test was used to calculate the significance of the mismatch.
Results
A mismatch between Risser and PHOS stages was observed in 28.5% of 105 patients, which was statistically significant (p < 0.001). Of the 49 patients with a Risser 0–1, 55.1% (n = 27) had a PHOS 4–5. None of the patients with a Risser 2–5 had a PHOS 1–3. In the 47 patients in whom both humeri were visualized, the absolute correlation between the left and right PHOS values was 95.7%.
Conclusion
Of AIS patients who are relatively skeletally immature according to Risser staging, more than half may be skeletally mature when measured with PHOS. In patients with a Risser 0–1, it is recommended to measure skeletal maturity in an AP spine radiograph using the PHOS method, which may more accurately guide treatment decision-making, without the need to visualize both humeral epiphyses in this radiographic projection.
Level of evidence
IV.

Similar content being viewed by others
References
Lonstein JE, Carlson JM (1984) The prediction of curve progression in untreated idiopathic scoliosis during growth. J Bone Joint Surg Am 66(7):1061–1071
Ylikoski M (2005) Growth and progression of adolescent idiopathic scoliosis in girls. J Pediatr Orthop B 14(5):320–324. https://doi.org/10.1097/01202412-200509000-00002
Risser JC (1958) The Iliac apophysis; an invaluable sign in the management of scoliosis. Clin Orthop 11:111–119
Little DG, Song KM, Katz D (2000) Relationship of peak height velocity to other maturity indicators in idiopathic scoliosis in girls. J Bone Joint Surg Am 82(5):685–693. https://doi.org/10.2106/00004623-200005000-00009
Reem J, Carney J, Stanley M (2009) Risser sign inter-rater and intra-rater agreement: is the Risser sign reliable? Skeletal Radiol 38(4):371–375. https://doi.org/10.1007/s00256-008-0603-8
Li DT, Cui JJ, DeVries S (2018) Humeral head ossification predicts peak height velocity timing and percentage of growth remaining in children. J Pediatr Orthop 38(9):e546–e550. https://doi.org/10.1097/BPO.0000000000001232
Di Pauli von Treuheim T, Li DT, Mikhail C (2020) Reliable skeletal maturity assessment for an AIS patient cohort: external validation of the proximal humerus ossification system (PHOS) and relevant learning methodology. Spine Deform 8(4):613–620. https://doi.org/10.1007/s43390-020-00105-5.
Vira S, Husain Q, Jalai C (2017) The interobserver and intraobserver reliability of the sanders classification versus the Risser stage. J Pediatr Orthop 37(4):e246–e249. https://doi.org/10.1097/BPO.0000000000000891
Sanders JO, Khoury JG, Kishan S (2008) Predicting scoliosis progression from skeletal maturity: a simplified classification during adolescence. J Bone Joint Surg Am 90(3):540–553. https://doi.org/10.2106/JBJS.G.00004
Sanders JO, Browne RH, McConnell SJ (2007) Maturity assessment and curve progression in girls with idiopathic scoliosis. J Bone Joint Surg Am 89(1):64–73. https://doi.org/10.2106/JBJS.F.00067
Li DT, Linderman GC, Cui JJ (2019) The proximal humeral ossification system improves assessment of maturity in patients with scoliosis. J Bone Joint Surg Am 101(20):1868–1874. https://doi.org/10.2106/JBJS.19.00296
Minkara A, Bainton N, Tanaka M (2020) High risk of mismatch between sanders and Risser staging in adolescent idiopathic scoliosis: are we guiding treatment using the wrong classification? J Pediatr Orthop 40(2):60–64. https://doi.org/10.1097/BPO.0000000000001135
Dimeglio A (2001) Growth in pediatric orthopaedics. J Pediatr Orthop 21(4):549–55.
Charles YP, Daures JP, de Rosa V (2006) Progression risk of idiopathic juvenile scoliosis during pubertal growth. Spine (Phila Pa 1976). 31(17):1933–42. https://doi.org/10.1097/01.brs.0000229230.68870.97.
Funding
The authors declare that they have no competing interests. No conflicts of interest or funding received during the conduct of this study. No funds, grants, or other support was received. The authors have no relevant financial or non-financial interests to disclose.
Author information
Authors and Affiliations
Contributions
JC, NRD, CAT, LP, RR, EG, JPA, MN: Design of study, consulting references, participation in draft manuscript, revise manuscript, and approved the final version of the paper.
Corresponding author
Ethics declarations
IRB
The study was approved by the hospital Institutional Review Board (IRB), because of the retrospective observational nature of the study IRB waived the informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Julián, C., Ricardo, D.N., Rodrigo, R. et al. Adolescent idiopathic scoliosis: is there a relationship between Risser staging and the proximal humerus ossification system?. Spine Deform 12, 629–633 (2024). https://doi.org/10.1007/s43390-023-00812-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-023-00812-9