Abstract
Purpose
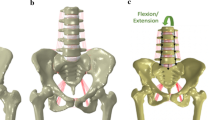
The fusion of the sacroiliac joint (SIJ) is the last treatment option for chronic pain resulting from sacroiliitis. With the various implant systems available, there are different possible surgical strategies in terms of the type and number of implants and trajectories. The aim was to quantify the effect of the number of cylindrical threaded implants on SIJ stabilization.
Methods
Six cadaveric pelvises were embedded in resin simulating a double-leg stance. Compression loads were applied to the sacral plate. The pelvises were tested non-instrumented and instrumented progressively with up to three cylindrical threaded implants (12-mm diameter, 60-mm length) with a posterior oblique trajectory. Vertical (VD) and angular (AD) displacements of the SIJ were measured locally using high-precision cameras and digital image correlation.
Results
Compared to the non-instrumented initial state, instrumentation with one implant significantly decreased the VD (− 24% ± 15%, p = 0.028), while the AD decreased on average by − 9% (± 15%; p = 0.345). When compared to the one-implant configuration, adding a second implant further statistically decreased VD (− 10% ± 7%, p = 0.046) and AD (− 19% ± 15, p = 0.046). Adding a third implant did not lead to additional stabilization for VD nor AD (p > 0.5).
Conclusion
Compared to the non-instrumented initial state, the two-implant configuration reduces both vertical and angular displacements the most, while minimizing the number of implants.



Similar content being viewed by others
Availability of data and materials
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
Code availability
Not applicable.
References
Cohen SP, Chen Y, Neufeld NJ (2013) Sacroiliac joint pain: a comprehensive review of epidemiology, diagnosis and treatment. Expert Rev Neurother 13:99–116. https://doi.org/10.1586/ern.12.148
Smith AG, Capobianco R, Cher D, Rudolf L, Sachs D, Gundanna M, Kleiner J, Mody MG, Shamie AN (2013) Open versus minimally invasive sacroiliac joint fusion: a multi-center comparison of perioperative measures and clinical outcomes. Ann Surg Innov Res 7:14. https://doi.org/10.1186/1750-1164-7-14
Claus CF, Lytle E, Kaufmann A, Tong D, Bahoura M, Garmo L, Richards B, Soo TM, Houseman C (2019) Minimally invasive sacroiliac joint fusion using triangular titanium versus cylindrical threaded implants: a comparison of patient-reported outcomes. World Neurosurg. https://doi.org/10.1016/j.wneu.2019.09.150
Sachs D, Kovalsky D, Redmond A, Limoni R, Meyer SC, Harvey C, Kondrashov D (2016) Durable intermediate-to long-term outcomes after minimally invasive transiliac sacroiliac joint fusion using triangular titanium implants. Med Devices (Auckland, NZ) 9:213–222. https://doi.org/10.2147/mder.s109276
Polly DW, Swofford J, Whang PG, Frank CJ, Glaser JA, Limoni RP, Cher DJ, Wine KD, Sembrano JN, the ISG (2016) Two-year outcomes from a randomized controlled trial of minimally invasive sacroiliac joint fusion vs non-surgical management for sacroiliac joint dysfunction. Int J Spine Surg 10:28. https://doi.org/10.14444/3028
Cross WW, Delbridge A, Hales D, Fielding LC (2018) Minimally invasive sacroiliac joint fusion: 2-year radiographic and clinical outcomes with a principles-based SIJ fusion system. Open Orthop J 12:7–16. https://doi.org/10.2174/1874325001812010007
Rajpal S, Burneikiene S (2019) Minimally invasive sacroiliac joint fusion with cylindrical threaded implants using intraoperative stereotactic navigation. World Neurosurg 122:e1588–e1591. https://doi.org/10.1016/j.wneu.2018.11.116
Lindsey DP, Parrish R, Gundanna M, Leasure J, Yerby SA, Kondrashov D (2018) Biomechanics of unilateral and bilateral sacroiliac joint stabilization: laboratory investigation. J Neurosurg Spine 28:326–332. https://doi.org/10.3171/2017.7.spine17499
Lindsey DP, Kiapour A, Yerby SA, Goel VK (2015) Sacroiliac joint fusion minimally affects adjacent lumbar segment motion: a finite element study. Int J Spine Surg 9:64. https://doi.org/10.14444/2064
Joukar A, Chande RD, Carpenter RD, Lindsey DP, Erbulut DU, Yerby SA, Duhon B, Goel VK (2019) Effects on hip stress following sacroiliac joint fixation: a finite element study. JOR Spine 2:e1067. https://doi.org/10.1002/jsp2.1067
Lindsey DP, Perez-Orribo L, Rodriguez-Martinez N, Reyes PM, Newcomb A, Cable A, Hickam G, Yerby SA, Crawford NR (2014) Evaluation of a minimally invasive procedure for sacroiliac joint fusion—an in vitro biomechanical analysis of initial and cycled properties. Med Devices (Auckland, NZ) 7:131–137. https://doi.org/10.2147/MDER.S63499
Soriano-Baron H, Lindsey DP, Rodriguez-Martinez N, Reyes PM, Newcomb A, Yerby SA, Crawford NR (2015) The effect of implant placement on sacroiliac joint range of motion: posterior versus transarticular. Spine 40:E525-530. https://doi.org/10.1097/brs.0000000000000839
Shih YC, Beaubien BP, Chen Q, Sembrano JN (2018) Biomechanical evaluation of sacroiliac joint fixation with decortication. Spine J. https://doi.org/10.1016/j.spinee.2018.02.016
Jeong JH, Leasure JM, Park J (2018) Assessment of biomechanical changes after sacroiliac joint fusion by application of the 3-dimensional motion analysis technique. World Neurosurg 117:e538–e543. https://doi.org/10.1016/j.wneu.2018.06.072
Dubé-Cyr R, Aubin C, Villemure I, Bianco RJ, Godio-Raboutet Y, Arnoux PJ (2020) Biomechanical analysis of two insertion sites for the fixation of the sacroiliac joint via an oblique lateral approach. Clin Biomech (Bristol, Avon) 74:118–123. https://doi.org/10.1016/j.clinbiomech.2020.02.010
Joukar A (2017) Gender specific sacroiliac joint biomechanics: a finite element study. The University of Toledo, Toledo
Lindsey DP, Kiapour A, Yerby SA, Goel VK (2018) Sacroiliac joint stability: finite element analysis of implant number, orientation, and superior implant length. World J Orthop 9:14–23. https://doi.org/10.5312/wjo.v9.i3.14
Larson AN, Polly DW Jr, Ackerman SJ, Ledonio CG, Lonner BS, Shah SA, Emans JB, Richards BS 3rd (2016) What would be the annual cost savings if fewer screws were used in adolescent idiopathic scoliosis treatment in the US? J Neurosurg Spine 24:116–123. https://doi.org/10.3171/2015.4.spine131119
Bruna-Rosso C, Arnoux PJ, Bianco RJ, Godio-Raboutet Y, Fradet L, Aubin CE (2016) Finite element analysis of sacroiliac joint fixation under compression loads. Int J Spine Surg 10:16. https://doi.org/10.14444/3016
Dall BE, Eden SV, Cho W, Karkenny A, Brooks DM, Hayward GM 2nd, Moldavsky M, Yandamuri S, Bucklen BS (2019) Biomechanical analysis of motion following sacroiliac joint fusion using lateral sacroiliac screws with or without lumbosacral instrumented fusion. Clin Biomech (Bristol, Avon) 68:182–189. https://doi.org/10.1016/j.clinbiomech.2019.05.025
Klima S, Grunert R, Ondruschka B, Scholze M, Seidel T, Werner M, Hammer N (2018) Pelvic orthosis effects on posterior pelvis kinematics an in-vitro biomechanical study. Sci Rep 8:15980. https://doi.org/10.1038/s41598-018-34387-7
Hammer N, Scholze M, Kibsgard T, Klima S, Schleifenbaum S, Seidel T, Werner M, Grunert R (2019) Physiological in vitro sacroiliac joint motion: a study on three-dimensional posterior pelvic ring kinematics. J Anat 234:346–358. https://doi.org/10.1111/joa.12924
Joukar A, Kiapour A, Elgafy H, Erbulut DU, Agarwal AK, Goel VK (2020) Biomechanics of the sacroiliac joint: surgical treatments. Int J Spine Surg 14:355–367. https://doi.org/10.14444/7047
Cher DJ, Reckling WC, Capobianco RA (2015) Implant survivorship analysis after minimally invasive sacroiliac joint fusion using the iFuse Implant System(®). Med Devices (Auckland, NZ) 8:485–492. https://doi.org/10.2147/MDER.S94885
Duhon BS, Bitan F, Lockstadt H, Kovalsky D, Cher D, Hillen T (2016) Triangular titanium implants for minimally invasive sacroiliac joint fusion: 2-year follow-up from a prospective multicenter trial. Int J Spine Surg 10:13. https://doi.org/10.14444/3013
Cher D, Polly D, Berven S (2014) Sacroiliac joint pain: burden of disease. Med Devices (Auckland, NZ) 7:73–81. https://doi.org/10.2147/mder.s59437
Crandall JR (1994) The preservation of human surrogates for biomechanical studies. PhD thesis, University of Virginia
van Haaren EH, van der Zwaard BC, van der Veen AJ, Heyligers IC, Wuisman PI, Smit TH (2008) Effect of long-term preservation on the mechanical properties of cortical bone in goats. Acta Orthop 79(5):708–716. https://doi.org/10.1080/17453670810016759
Topp T, Müller T, Huss S, Kann PH, Weihe E, Ruchholtz S, Zettl RP (2012) Embalmed and fresh frozen human bones in orthopedic cadaveric studies: which bone is authentic and feasible? Acta Orthop 83(5):543–547. https://doi.org/10.3109/17453674.2012.727079
Acknowledgements
The authors acknowledge the support of Dr Kathia Chaumoître, MD, and the Assistance Publique-Hôpitaux de Marseille, (Hôpital Nord, Marseille, France) for their radiologic expertise.
Funding
This study was financially supported by the Fonds de Recherche du Québec—Nature et Technologies, the A*MIDEX foundation and the Technologies and the Natural Sciences and Engineering Research Council of Canada (Industrial Research Chair program with Medtronic of Canada, IRCPJ 346145-16).
Author information
Authors and Affiliations
Contributions
RD-C: (1) made substantial contributions to the conception of the work, acquisition, analysis and interpretation of data; (2) drafted the work; (3) approved the version to be published; (4) agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. C-ÉA: (1) made substantial contributions to the conception of the work and interpretation of data; (2) revised the work critically for important intellectual content; (3) approved the version to be published; (4) agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. IV: (1) made substantial contributions to the conception of the work and interpretation of data; (2) revised the work critically for important intellectual content; (3) approved the version to be published; (4) agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved. P-JA: (1) made substantial contributions to the conception of the work and interpretation of data; (2) revised the work critically for important intellectual content; (3) approved the version to be published; (4) agreed to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Conflict of interest
Dr. Aubin reports grants from Natural Sciences and Engineering Research Council of Canada (Industrial Research Chair program with Medtronic of Canada), non-financial support from Medtronic, during the conduct of the study; grants from Medtronic, grants from Natural Sciences and Engineering Research Council of Canada, grants from Canada First Research Excellence Funds, outside the submitted work. Dr. Dubé-Cyr has nothing to disclose. Dr. Villemure has nothing to disclose. Dr. Arnoux has nothing to disclose.
Ethics approval
Polytechnique Montreal: CÉR-1617-30.
Consent to participate
Specimens used in this study gave an informed consent to donate their body to science.
Consent for publication
Information is anonymized.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dubé-Cyr, R., Aubin, CÉ., Villemure, I. et al. Biomechanical analysis of the number of implants for the immediate sacroiliac joint fixation. Spine Deform 9, 1267–1273 (2021). https://doi.org/10.1007/s43390-021-00325-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-021-00325-3