Abstract
Study design
Multicenter retrospective.
Objective
To determine the long-term complication rate associated with surgical treatment of spondylolisthesis in adolescents.
Summary of background data
There is limited information on the complication rate associated with posterior spinal fusion (PSF) of spondylolisthesis in the pediatric and adolescent population.
Methods
Patients who underwent PSF for spondylolisthesis between 2004 and 2015 at four spine centers, < 21 years of age, were included. Exclusion criteria were < 2 years of follow-up or anterior approach. Charts and radiographs were reviewed.
Results
50 patients had PSF for spondylolisthesis, 26 had PSF alone, while 24 had PSF with trans-foraminal lumbar interbody fusion (TLIF). Mean age was 13.9 years (range 9.6–18.4). Mean follow-up was 5.5 years (range 2–15). Mean preoperative slip was 61.2%. 20/50 patients (40%) experienced 23 complications requiring reoperation at a mean of 2.1 years (range 0–9.3) for the following: implant failure (12), persistent radiculopathy (3), infection (3), persistent back pain (2), extension of fusion (2), and hematoma (1). In addition, there were 22 cases of radiculopathy (44%) that were transient. Rate of implant failure was related to preoperative slip angle (p = 0.02). Reoperation rate and rates of implant failure were not associated with preoperative % slip (reoperation: p = 0.42, implant failure: p = 0.15), postoperative % slip (reoperation: p = 0.42, implant failure: p = 0.99), postoperative kyphosis of the lumbosacral angle (reoperation: p = 0.81, implant failure: p = 0.48), change in % slip (reoperation: p = 0.30, implant failure: p = 0.12), change in slip angle (reoperation: p = 0.42, implant failure: p = 0.40), graft used (reoperation: p = 0.22, implant failure: p = 0.81), or addition of a TLIF (reoperation: p = 0.55, implant failure: p = 0.76).
Conclusion
PSF of spondylolisthesis in the adolescent population was associated with a 40% reoperation rate and high rate of post-operative radiculopathy. Addition of a TLIF did not impact reoperation rate or rate of radiculopathy.

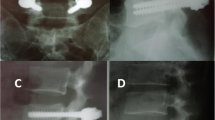
Reproduced with Permission from the Children’s Orthopaedic Center, Los Angeles

Reproduced with Permission from the Children’s Orthopaedic Center, Los Angeles

Reproduced with Permission from the Children’s Orthopaedic Center, Los Angeles

Reproduced with Permission from the Children’s Orthopaedic Center, Los Angeles
Similar content being viewed by others
References
Schoenleber SJ, Shufflebarger HL, Shah SA (2015) The assessment and treatment of high-grade lumbosacral spondylolisthesis and spondyloptosis in children and young adults. JBJS Rev 3(12)
Boxall D et al (1979) Management of severe spondylolisthesis in children and adolescents. J Bone Jt Surg Am 61(4):479–495
Bourassa-Moreau E et al (2013) Quality of life of patients with high-grade spondylolisthesis: minimum 2-year follow-up after surgical and nonsurgical treatments. Spine J 13(7):770–774
Maurice HD, Morley TR (1989) Cauda equina lesions following fusion in situ and decompressive laminectomy for severe spondylolisthesis. Four case reports. Spine (Phila Pa 1976) 14(2):214–216
Schoenecker PL et al (1990) Cauda equina syndrome after in situ arthrodesis for severe spondylolisthesis at the lumbosacral junction. J Bone Jt Surg Am 72(3):369–377
Lykissas MG et al (2014) Paresis of the L5 nerve root after reduction of low-grade lumbosacral dysplastic spondylolisthesis: a case report. J Pediatr Orthop B 23(5):461–466
Molinari RW et al (1999) Complications in the surgical treatment of pediatric high-grade, isthmic dysplastic spondylolisthesis. A comparison of three surgical approaches. Spine (Phila Pa 1976) 24(16):1701–1711
Bouyer B et al (2014) High-grade lumbosacral spondylolisthesis reduction and fusion in children using transsacral rod fixation. Childs Nerv Syst 30(3):505–513
Burkus JK et al (1992) Long-term evaluation of adolescents treated operatively for spondylolisthesis. A comparison of in situ arthrodesis only with in situ arthrodesis and reduction followed by immobilization in a cast. J Bone Jt Surg Am 74(5):693–704
Fu KM et al (2011) Morbidity and mortality in the surgical treatment of six hundred five pediatric patients with isthmic or dysplastic spondylolisthesis. Spine (Phila Pa 1976) 36(4):308–312
Lundine KM et al (2014) Patient outcomes in the operative and nonoperative management of high-grade spondylolisthesis in children. J Pediatr Orthop 34(5):483–489
DeWald RL et al (1981) Severe lumbosacral spondylolisthesis in adolescents and children. Reduction and staged circumferential fusion. J Bone Jt Surg Am 63(4):619–626
Kasliwal MK et al (2012) Short-term complications associated with surgery for high-grade spondylolisthesis in adults and pediatric patients: a report from the scoliosis research society morbidity and mortality database. Neurosurgery 71(1):109–116
Schwend RM et al (1992) Treatment of severe spondylolisthesis in children by reduction and L4–S4 posterior segmental hyperextension fixation. J Pediatr Orthop 12(6):703–711
O'Brien MFK, Blanke KM, Lenke LG (eds) (2008) Spinal deformity study group radiographic measurement manual. Medtronic Sofamor Danek USA, Inc
Transfeldt EE, Mehbod AA (2007) Evidence-based medicine analysis of isthmic spondylolisthesis treatment including reduction versus fusion in situ for high-grade slips. Spine (Phila Pa 1976) 32(19 Suppl):S126–S129
Ilharreborde B et al (2007) Jackson's intrasacral fixation in the management of high-grade isthmic spondylolisthesis. J Pediatr Orthop B 16(1):16–18
Muschik M, Zippel H, Perka C (1997) Surgical management of severe spondylolisthesis in children and adolescents. Anterior fusion in situ versus anterior spondylodesis with posterior transpedicular instrumentation and reduction. Spine (Phila Pa 1976) 22(17):2036–2042 (discussion 2043)
Poussa M et al (1993) Surgical treatment of severe isthmic spondylolisthesis in adolescents. Reduction or fusion in situ. Spine (Phila Pa 1976) 18(7):894–901
Cook JA, Collins GS (2015) The rise of big clinical databases. Br J Surg 102(2):e93–e101
Yoshihara H, Yoneoka D (2014) Understanding the statistics and limitations of large database analyses. Spine (Phila Pa 1976) 39(16):1311–1312
Shufflebarger HL, Geck MJ (2005) High-grade isthmic dysplastic spondylolisthesis: monosegmental surgical treatment. Spine (Phila Pa 1976) 30(6):S42–48
Lonner BS et al (2007) Reduction of high-grade isthmic and dysplastic spondylolisthesis in 5 adolescents. Am J Orthop (Belle Mead NJ) 36(7):367–373
Lenke LG, Bridwell KH (2003) Evaluation and surgical treatment of high-grade isthmic dysplastic spondylolisthesis. Instr Course Lect 52:525–532
Funding
This study has been carried out with approval from the Institutional Review Board at Children’s Hospital Los Angeles. None of the authors received financial support for this study.
Author information
Authors and Affiliations
Contributions
EN data collection, data analysis, manuscript preparation, final approval of manuscript. LMA study design, manuscript preparation, manuscript review, final approval of manuscript. AS data collection, manuscript preparation, final approval of manuscript. NM data collection, manuscript review, final approval of manuscript. SG study design, manuscript review, final approval of manuscript. MP study design, manuscript review, final approval of manuscript. BKB study design, manuscript review, final approval of manuscript. EF study design, manuscript review, final approval of manuscript. KM study design, manuscript review, final approval of manuscript. BI study design, manuscript review, final approval of manuscript. DLS study design, manuscript review, final approval of manuscript.
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nielsen, E., Andras, L.M., Siddiqui, A.A. et al. 40% reoperation rate in adolescents with spondylolisthesis. Spine Deform 8, 1059–1067 (2020). https://doi.org/10.1007/s43390-020-00121-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43390-020-00121-5