Abstract
The number of reported cases of rib osteomyelitis is very infrequent. Magnetic resonance is generally the best test in these cases, due to its high sensitivity and specificity. However, given this technique has some drawbacks, it is usually restricted to cases of bad evolution. A relevant, easy to perform, bedside imaging test is the point of care ultrasound. We present the case of a 2-month-old infant with a rib osteomyelitis detected by point-of-care ultrasound in the context of sepsis after abdominal surgery. The thoracic ultrasound revealed a lesion adjacent to the right sixth rib and round extra-parenchymal collection in the right costophrenic sinus. Chest computed tomography confirmed the presence of a hypodense collection at the costochondral junction of the right seventh rib with pleural thickening and an increase in soft tissues, compatible with osteomyelitis. Our ultrasound finding in the absence of specific clinical data of rib osteomyelitis led us to a change in the duration of the antibiotic treatment already established and therefore likely led to an improvement in the patient’s prognosis. The ultrasound has gained increasing prominence due to its usefulness in diagnosis and monitoring, especially in pediatric intensive care, given the ease of use at the patient’s bedside.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
It is important to acknowledge that osteomyelitis is a serious disease with a mortality rate of up to 5% of affected cases [1]. This pathology is however difficult to diagnose due to the absence of specific signs and symptoms. Early diagnosis is essential to avoid complications, to properly direct antibiotic treatment and to reduce the need for surgical intervention [2]. Medical imaging tests, such as radiography, ultrasound, magnetic resonance imaging (MRI), single-photon emission computed tomography (SPECT) and positron emission tomography (PET), are often used to diagnose osteomyelitis. In a systematic review of imaging tests for the detection of osteomyelitis, it revealed in adults that MRI, SPECT and PET had similar diagnostic performance, whilst CT, radiography (Rx) and scintigraphy all had a generally inferior diagnostic accuracy. In children, there was not enough evidence to reach a clear conclusion [3].
In the case of a critically ill infant or child, the main challenge is achieving an accurate diagnosis of osteomyelitis at the bedside, without having to transfer the patient to the radiology department. It is accepted that sonography and MRI imaging have the best sensitivity for detection of acute osteomyelitis and septic arthritis in children [4]. With ultrasound, the first sign that presents, even before the periosteal reaction, is swelling and oedema of the deep soft tissues surrounding the bone, as well as thickening and increased echogenicity of subcutaneous fat, and loss of differentiation between fat and dermis. Ultrasound could be used to monitor the evolution of the disease and to detect collections [5].
Clinical Case
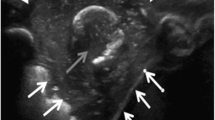
We present the case of a 2-month-old infant with rib osteomyelitis detected by ultrasound, in the context of sepsis after abdominal surgery. One month prior to this finding, his parents presented at the emergency department for significant irritability and abdominal distension. Upon admission, a poor general condition was observed with hemodynamic instability and severe lactic acidosis. In the abdominal ultrasound, intestinal loop distention and abundant free fluid were observed. Laparotomy was performed, finding intestinal malrotation with volvulus. One month after the surgical correction, the patient began to have a fever and irritability, so it was necessary to proceed with empirical antibiotic therapy. Methicillin-sensitive Staphylococcus aureus (MSSA) was isolated in several hemocultures and the central venous catheter tip. Catheter-related bacteremia was diagnosed, and antibiotic therapy was indicated according to the antibiogram. Coinciding with bacteremia, the patient developed pulmonary oedema and respiratory failure, due to fluid overload. In the pulmonary ultrasound performed at the bedside, B lines were observed, compatible with interstitial oedema due to increased pulmonary fluid. Diuretics and high-flow oxygen therapy were added to the therapy. In the following days, a progressive improvement was observed in the ultrasound findings as well as in the respiratory failure. However, in one of the ultrasounds performed, a 3 × 3 cm round extraparenchymal collection with a heterogeneous appearance in the right costophrenic sinus was detected (Fig. 1, 2, 3, video 1, video 2, video 3). No alteration was observed in skin or subcutaneous tissue or in the contralateral hemithorax (video 4). The chest radiograph confirmed the image of lung consolidation accompanied by a lytic lesion at the costochondral junction of the right seventh rib, with an associated periosteal reaction (Fig. 4). Chest CT confirmed the presence of a hypodense collection at the costochondral junction of the right seventh rib with pleural thickening and an increase in soft tissues, compatible with osteomyelitis (Fig. 5). As a result, antibiotic therapy was maintained, and echocardiography was performed to rule out endocarditis lesions. The follow-up thoracic ultrasounds showed a progressive decrease in the heterogeneous extraparenchymal collection in the right costophrenic sinus (Fig. 6, Video 5), which subsequently disappeared.
Discussion
Acute osteomyelitis is usually unifocal and prefers the metaphysis of the long bones (femur, tibia and humerus, in this order). Rib osteomyelitis is very infrequently reported. Typically, it has an incidence of approximately eight cases per 100,000 children per year, with a higher prevalence in those under 5 years old. However, in the recent years, an increase in the number of incidences has been observed [6]: the number of cases of acute osteomyelitis has risen by 2.8 times in the last 20 years [7]. Most infections are produced by the haematogenous route, with Staphylococcus aureus being the most common causative microorganism in all ages [5]. Severity of the course of osteomyelitis in children has been reported to be rising, possibly due to more frequent presence of more aggressive MRSA and PVL gene (Panton-Valentine leukocidin), where prompt and accurately targeted therapy is vital for favourable outcome [8].
In the diagnosis of acute osteomyelitis, imaging tests play an important role. A study comparing different diagnostic methods showed that magnetic resonance and bone scintigraphy are most valuable methods at the onset of the illness [9].
Conventional radiographs are diagnostic in less than 20% of acute osteomyelitis in the early stages of the disease; at the same time, they are useful in distinguishing conditions as trauma or potentially tumour. The sensitivity of conventional X-ray increases in late diagnosis. Sensitivity and specificity of ultrasound modality have been stated around 50% [9].
Magnetic resonance (MR) imaging is generally the best test in these cases, due to its high sensitivity and specificity. However, this technique has some drawbacks such as less availability, having to transfer the children to the radiology department and the requirement of sedation during the procedure. For all these reasons, it is usually restricted to cases of torpid evolution. Other relevant imaging tests are bedside ultrasound, plain radiography, CT and bone scintigraphy [4]. CT was used in our case as it has good specificity and adequate sensitivity (69.7% sensitivity, 95% CI 40.1 to 88.7%; 90.2% specificity (57.6 to 98.4%) [5].
The use of ultrasound has gained increasing prominence due to its usefulness in diagnosis and monitoring given the ease of use at the patient’s bedside. The most frequent early sonographic findings are intra-articular fluid collections and/or subperiosteal abscess formation that precedes radiographic changes by several days. It can detect superficial cortical erosion and even intramedullary. Point-of-care ultrasound (POCUS) is a very helpful tool for establishing the correct diagnosis in osteomyelitis and for reducing the frequency of additional imaging studies. In a pediatric study, Riebel et al. [10] found that typical ultrasound patterns of osteomyelitis precede to radiographic images by several days in most cases. In the first 48–72 h after infection, ultrasound can detect soft tissue inflammation followed by periosteal elevation due to fluid accumulation, subsequent subperiosteal collection and, finally, erosion of the cortical bone that appears between 2 and 4 weeks of evolution. If necessary, it can be helpful in guiding the puncture of a bone or abscess. With Doppler ultrasound, an increase in vascular flow can be found in the early phases, a common finding in the diagnosis of osteomyelitis [10]. Therefore, ultrasound is a technique of considerable significance and use in osteomyelitis. Tayal et al. [11] found that the use of ultrasound in this instance changes the management of patients in approximately half of the cases.
Ultrasound seems to be a safer, advantageous, quick and easy to use method compared to an MRI despite its relatively low specificity and sensitivity. Sensitivity and specificity of the ultrasound might be potentially modifiable factor by operator experience. Since the ultrasound imaging has become frequently used method in the intensive care units or emergency department settings, operators’ experience has been broadening. The advantages of ultrasound have been broadly recognised by medical society. The ultrasound technique is easy to use, an investigation is possible to repeat at any time and as many times as patient tolerates, allows comparison of both sides, does not introduce a burden for a patient (e.g. radiation or pain) and is very cost-effective.
As we show in this case, ultrasound can be useful for an early detection of osteomyelitis in children although an MRI will still be required for a more thorough assessment. Ultrasound is able to detect very early in course of the illness:
-
Soft tissue swelling seen as areas of fluid collection and hypervascularity around the affected bone on colour Doppler.
-
Periostal thickening and subperiostal collection seen as periostal elevation with an underlying fluid collection.
-
The collection might be assessed using dynamic nature of ultrasound and allow for needle aspiration if required.
-
Scanning the cortical bone surface and periosteum can be helpful in distinguishing between infection, tumour and trauma [12].
In conclusion, there is no doubt that ultrasound detects signs of acute osteomyelitis in children earlier than standard radiography, hence is very useful as a screening method. Being rapid, cheap, easily available and accurate diagnostic modality, it is very useful guide allowing to plan more thorough investigations and target the therapy with minimal burden to a patient. The article contributes to the broadening evidence that ultrasound is becoming the method of choice for assessment of patients, especially in intensive care or emergency medicine settings bringing faster and more accurate diagnostic, hopping to improve patients experience and outcome.
In our case, the performance of daily pulmonary ultrasounds to monitor fluid management and assess fluid overload led us to the incidental finding of costal osteomyelitis of probable haematogenous cause. As Marin et al. [13] show, there are many lesions that are not clinically evident, and in these cases, ultrasound may improve the accuracy of the clinical examination.
Our ultrasound finding in the absence of specific clinical data led us to a change in the duration of the antibiotic treatment already established and therefore a likely improvement in the patient’s prognosis [14].
Data Availability
The datasets used during the current study are available from the corresponding author on reasonable request.
Code Availability
No applicable.
References
Zink BJ, Raukar NP. Bone and joint infections. Rosen’s Emergency Medicine.7th edn, Vol. 2. Philadelphia: Mosby-Elsevier; 2010:1816.
Emiley PJ, Kendall JL, Bellows JW. Acute hematogenous osteomyelitis of the rib identified on bedside ultrasound. Ultrasound Emerg Med. 2015;48(1):e15–7.
Llewellyn A, Jones-Diette J, Kraft J, Holton C, Harden M, Simmonds M. Imaging tests for the detection of osteomyelitis: a systematic review. Health Technol Assess. 2019;23(61):1-128.4.
Manz N, Krieg AH, Heininger U, Ritz N. Evaluation of the current use of imaging modalities and pathogen detection in children with acute osteomyelitis and septic arthritis. Eur J Pediatr. 2018;177(7):1071–80.
LeeYJ, Sadigh S, Mankad K, Kapse N, Rajeswaran G. The imaging of osteomyelitis. Quant Imaging Med Surg. 2016;6(2):184–198.
Castellazzi L, Mantero M, Esposito S. Update on the management of pediatric acute osteomyelitis and septic arthritis. Int J Mol Sci. 2016;17(6):855.
Gafur OA, Copley LAB, Hollmig ST, Browne RH, Thornton LA, Crawford SE. The impact of the current epidemiology of pediatric musculoskeletal infection on evaluation and treatment guidelines. J Pediatr Orthop. 2008;28:777–85.
Peltola H, Pääkkönen M. Acute osteomyelitis in children. N Engl J Med. 2014;370:352–60.
Malcius D, Jonkus M, Kuprionis G, et al. The accuracy of different imaging techniques in diagnosis of acute hematogenous osteomyelitis. Medicina. 2009;45(8):624–31.
Riebel TW, Nasir R, Nazarenko O. The value of sonography in the detection of osteomyelitis. Pediatr Radiol. 1996;26(4):291–7.
Tayal VS, Hasan N, Norton HJ, et al. The effect of soft-tissue ultrasound on the management of cellulitis in the emergency department. Acad Emerg Med. 2006;13:384–8.
Dumitriu D, Menten R, Clapuyt P. Ultrasonography of the bone surface in children: normal and pathological findings in the bone cortex and periosteum. Pediatr Radiol. 2022;52:1392–403.
Marin JR, Dean AJ, Bilker WB, et al. Emergency ultrasound-assisted examination of skin and soft tissue infections in the pediatric emergency department. Acad Emerg Med. 2013.
Schleifer J, Liteplo AS, Kharasch S. Point-of-care ultrasound in a child with chest wall pain and rib osteomyelitis. J Emerg Med. 2019;57(4):550–3.
Funding
Funding for open access publishing: Universidad de Córdoba/CBUA.
Author information
Authors and Affiliations
Contributions
MYR, DRL, VJMJ and PNJL participated in obtaining the lung ultrasound images and writing the manuscript. MSS and RSB participated in taking data from the patient. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval
Local ethic committee approved this publication.
Consent to Participate
No applicable.
Consent for Publication
Written informed consent was obtained from the patient´s parents for publication of this case report and accompanying images.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Imaging
Supplementary Information
Below is the link to the electronic supplementary material.
Supplementary file1 (WMV 2676 KB)
Supplementary file2 (WMV 1241 KB)
Supplementary file3 (WMV 1697 KB)
Supplementary file4 (WMV 2451 KB)
Supplementary file5 (WMV 1701 KB)
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Montero-Yéboles, R., Manzanares-Santos, S., Díaz-Rueda, L. et al. Point-of-Care Ultrasound to Identify Rib Osteomyelitis in the Infants: a Case Report. SN Compr. Clin. Med. 5, 90 (2023). https://doi.org/10.1007/s42399-023-01413-3
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-023-01413-3