Abstract
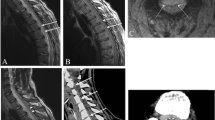
Dural ectasia is a common finding in patients with Marfan syndrome, while many of these patients are on anticoagulants due to prosthetic heart valves. A 44-year-old man was transferred to the ER due to cauda equina syndrome. The patient was on warfarin. His CT scan revealed spontaneous hemorrhage in the lumbosacral region. The patient underwent an urgent laminectomy with subtotal removal of haemorrhagic tissue. Post-operatively, he developed sepsis due to wound leak. Additionally he developed resistance to heparin. The complications were successfully managed, and the patient was discharged 3 months after his admission. People with Marfan syndrome could have significant co-morbidities while their management can be complicated by various issues. We present a case of lumbosacral hemorrhage and cauda equina with the background of dural ectasia and anticoagulants and discuss the relevant set of complications and their management.


Similar content being viewed by others
Availability of Data and Material
“Not applicable”.
Code Availability
“Not applicable”.
References
Kodolitsch Y, Backer J, Schüler H, et al. Perspectives on the revised Ghent criteria for the diagnosis of Marfan syndrome 2015. Appl Clin Genet. 2015;8:137–55.
Xiao Y, Liu X, Guo X, et al. A novel FBN1 mutation causes autosomal dominant Marfan syndrome. Mol Med Rep. 2017;16(5):7321–8.
Lundby R, Rand-Hendriksen S, Hald JK, et al. Dural ectasia in Marfan syndrome: A case control study Am. J Neuroradiol. 2009;30:1534–40.
Arnold P, Teuber J. Marfan syndrome and symptomatic sacral cyst: Report of two cases. J Spinal Cord Med. 2013;36(5):499–503.
Boker T, Vanem TT, Pripp AH, et al. Dural ectasia in Marfan syndrome and other hereditary connective tissue disorders: a 10-year follow-up study The Spine Journal 2019; 1−10
Voermans NC, Hosman AJ, van Alfen N, et al. Radicular dysfunction due to spinal deformities in Marfan syndrome at older age: Three case reports. Eur J Med Genet. 2010;53(1):35–9.
Avivi E, Arzi H, Paz L, Caspi I. Chechik Skeletal manifestations of Marfan syndrome. IMAJ. 2008;10:186–8.
Hollenberg A, Baldwin A, Mesfin A, Silberstein H. Rupture of giant anterior sacral meningocele in a patient with Marfan syndrome: Diagnosis and management. World Neurosurg. 2018;119:137–41.
Stone J, Bergmann L, Takamori R, Donovan DJ. Giant pseudomeningocele causing urinary obstruction in a patient with Marfan syndrome Neurosurg. Spine. 2015;23:77–80.
Gilete-Tejero IJ, Ortega-Martínez M, Mata-Gómez J, et al. Anterior sacral meningocelepresenting as intracystic bleeding. Eur SpineJ. 2017;27:276–80.
Samet J, Johnson PT, Horton KM, Fishman EK. Diverticulitis complicated by fistulous communication of sigmoid colon with anterior sacral meningocele in a patient with Marfan syndrome. Radiology Case Reports (Online). 2012;7:442.
Paisan G, Crandall K, Chen S, Burks S, Sands L, Levi A. Closure of a giant anterior sacral meningocele with an omental flap in a patient with Marfan syndrome: Case report. J Neurosurg Spine. 2018;29:182–6.
Leissinger CA, Blatt PM, Hoots WK, Ewenstein B. Role of prothrombin complex concentrates in reversing warfarin anticoagulation: a review of the literature. Am J Hematol. 2008;83:137–43.
van Aart L, Eijkhout HW, Kamphuis JS, et al. Individualized dosing regimen for prothrombin complex concentrate more effective than standard treatment in the reversal of oral anticoagulant therapy: An open, prospective randomized controlled trial. Thromb Res. 2006;118(3):313–20.
Choudhury M, Kiran U, Saxena N, Saxena R. Heparin resistance and Marfan syndrome: Is there any correlation? J Cardiothorac Vasc Anesth. 2002;16(1):75–9.
Spiess B. Treating heparin resistance with antithrombin or fresh frozen plasma. Ann Thorac Surg. 2008;85:2153–60.
Author information
Authors and Affiliations
Contributions
All authors contributed equally for this work. K. Faropoulos, MD, PhD, has the supervision and is the corresponding author.
Corresponding author
Ethics declarations
Ethics Approval
The work is in accordance with the principles of Nicosia General Hospital, The Scientific Committee, Ethical Board. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent to Participate
A retrospective permission was taken by the “Nicosia General Hospital, The Scientific Committee, Ethical Board.”
Consent for Publication
A retrospective permission was taken by the “Nicosia General Hospital, The Scientific Committee, Ethical Board.”
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Surgery
Rights and permissions
About this article
Cite this article
Gioti, I., Nikolaides, D., Picolas, C. et al. Spontaneously Ruptured Dural Ectasia in a Patient with Marfan Syndrome: a Case Report and Discussion of the Challenges Faced. SN Compr. Clin. Med. 4, 8 (2022). https://doi.org/10.1007/s42399-021-01100-1
Accepted:
Published:
DOI: https://doi.org/10.1007/s42399-021-01100-1