Abstract
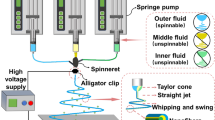
Current electrospun membranes used for pulp capping still lack the sustained-release capability and long-term anti-inflammatory effects that are favorable for dental pulp regeneration. In this work, a single-layered poly(lactic acid) (PLA) electrospun membrane loaded with amorphous calcium phosphate (ACP) and aspirin (PLA/ACP/Aspirin membrane, i.e., PAA membrane) is sandwiched between two poly(lactic-co-glycolic acid) (PLGA) electrospun membranes as a novel sandwich-structured PLGA and PAA composite electrospun membrane (PLGA-PAA membrane) to resolve the need for sustained-release design and anti-inflammatory effects. Contact angle measurements indicate that the PLGA-PAA membrane is more hydrophilic than the PAA membrane. An in vitro release study reveals that PLGA membranes coated on PAA membrane could slightly slow down ion release, while significantly prolonging aspirin release. We also co-cultured membranes with dental pulp stem cells (DPSCs) and human monocytic THP-1 cells to evaluate their osteogenic ability and anti-inflammatory effects, respectively. Compared with the PAA membrane, the PLGA-PAA membrane promotes cell adhesion, proliferation, and osteogenic differentiation. A prolonged anti-inflammatory effect of up to 18 days is also observed in the PLGA-PAA group. The results suggest a promising strategy for fabricating an electrospun membrane system with controlled release capabilities and long-term anti-inflammatory effects for use as pulp-capping material for regeneration of the dentin-pulp complex.
Graphic abstract







Similar content being viewed by others
References
Tort H, Oktay EA, Tort S et al (2017) Evaluation of ornidazole-loaded nanofibers as an alternative material for direct pulp capping. J Drug Deliv Sci Technol 41:317–324. https://doi.org/10.1016/j.jddst.2017.07.010
Lee W, Oh JH, Park JC et al (2012) Performance of electrospun poly(epsilon-caprolactone) fiber meshes used with mineral trioxide aggregates in a pulp capping procedure. Acta Biomater 8(8):2986–2995. https://doi.org/10.1016/j.actbio.2012.04.032
Wang J, Liu X, Jin X et al (2010) The odontogenic differentiation of human dental pulp stem cells on nanofibrous poly(L-lactic acid) scaffolds in vitro and in vivo. Acta Biomater 6(10):3856–3863. https://doi.org/10.1016/j.actbio.2010.04.009
Lee LW, Hsiao SH, Hung WC et al (2015) Clinical outcomes for teeth treated with electrospun poly(epsilon-caprolactone) fiber meshes/mineral trioxide aggregate direct pulp capping. J Endod 41(5):628–636. https://doi.org/10.1016/j.joen.2015.01.007
Choung HW, Lee DS, Lee JH et al (2016) Tertiary dentin formation after indirect pulp capping using protein CPNE7. J Dent Res 95(8):906–912. https://doi.org/10.1177/0022034516639919
Peycheva K (2015) Pulp-capping with mineral trioxide aggregate. Acta Med Bulgarica 42(2):23–29. https://doi.org/10.1515/amb-2015-0014
Furey A, Hjelmhaug J, Lobner D (2010) Toxicity of flow line, durafill vs, and dycal to dental pulp cells: effects of growth factors. J Endod 36(7):1149–1153. https://doi.org/10.1016/j.joen.2010.03.013
Parirokh M, Torabinejad M, Dummer PMH (2018) Mineral trioxide aggregate and other bioactive endodontic cements: an updated overview—part I: vital pulp therapy. Int Endod J 51(2):177–205. https://doi.org/10.1111/iej.12841
da Rosa WLO, Cocco AR, da Silva TM et al (2018) Current trends and future perspectives of dental pulp capping materials: a systematic review. J Biomed Mater Res B 106(3):1358–1368. https://doi.org/10.1002/jbm.b.33934
Brizuela C, Ormeno A, Cabrera C et al (2017) Direct pulp capping with calcium hydroxide, mineral trioxide aggregate, and biodentine in permanent young teeth with caries: a randomized clinical trial. J Endod 43(11):1776–1780. https://doi.org/10.1016/j.joen.2017.06.031
Torabinejad M, Parirokh M (2010) Mineral trioxide aggregate: a comprehensive literature review-part II: leakage and biocompatibility investigations. J Endod 36(2):190–202. https://doi.org/10.1016/j.joen.2009.09.010
Palma PJ, Marques JA, Falacho RI et al (2019) Six-month color stability assessment of two calcium silicate-based cements used in regenerative endodontic procedures. J Funct Biomater 10(1):14. https://doi.org/10.3390/jfb10010014
Hilton TJ (2009) Keys to clinical success with pulp capping: a review of the literature. Oper Dent 34(5):615–625. https://doi.org/10.2341/09-132-0
Sanaei-rad P, Jamshidi D, Adel M et al (2021) Electrospun poly(L-lactide) nanofibers coated with mineral trioxide aggregate enhance odontogenic differentiation of dental pulp stem cells. Polym Adv Technol 32(1):402–410. https://doi.org/10.1002/pat.5095
Daghrery A, Aytac Z, Dubey N et al (2020) Electrospinning of dexamethasone/cyclodextrin inclusion complex polymer fibers for dental pulp therapy. Colloids Surf B Biointerface 191:111011. https://doi.org/10.1016/j.colsurfb.2020.111011
Thakor J, Ahadian S, Niakan A et al (2020) Engineered hydrogels for brain tumor culture and therapy. Bio-Des Manuf 3(3):203–226. https://doi.org/10.1007/s42242-020-00084-6
Ma PX (2004) Scaffolds for tissue fabrication. Mater Today 7(5):30–40. https://doi.org/10.1016/S1369-7021(04)00233-0
Song JQ, Zhu GL, Gao HC et al (2018) Origami meets electrospinning: a new strategy for 3D nanofiber scaffolds. Bio-Des Manuf 1(4):254–264. https://doi.org/10.1007/s42242-018-0027-9
Gao Q, Zhao P, Zhou RJ et al (2019) Rapid assembling organ prototypes with controllable cell-laden multi-scale sheets. Bio-Des Manuf 2(1):1–9. https://doi.org/10.1007/s42242-019-00032-z
Li Z, Du T, Ruan C et al (2021) Bioinspired mineralized collagen scaffolds for bone tissue engineering. Bioact Mater 6(5):1491–1511. https://doi.org/10.1016/j.bioactmat.2020.11.004
Song W, Chen L, Seta J et al (2017) Corona discharge: a novel approach to fabricate three-dimensional electrospun nanofibers for bone tissue engineering. ACS Biomater Sci Eng 3(6):1146–1153. https://doi.org/10.1021/acsbiomaterials.7b00061
Kost B, Svyntkivska M, Brzezinski M et al (2020) PLA/beta-CD-based fibres loaded with quercetin as potential antibacterial dressing materials. Colloids Surf B Biointerface. https://doi.org/10.1016/j.colsurfb.2020.110949
Konwarh R (2019) Can the venerated silk be the next-generation nanobiomaterial for biomedical-device designing, regenerative medicine and drug delivery? Prospects and hitches. Bio-Des Manuf 2(4):278–286. https://doi.org/10.1007/s42242-019-00052-9
Niu X, Liu Z, Hu J et al (2016) Microspheres assembled from chitosan-graft-poly(lactic acid) micelle-like core-shell nanospheres for distinctly controlled release of hydrophobic and hydrophilic biomolecules. Macromol Biosci 16(7):1039–1047. https://doi.org/10.1002/mabi.201600020
Loi F, Cordova LA, Pajarinen J et al (2016) Inflammation, fracture and bone repair. Bone 86:119–130. https://doi.org/10.1016/j.bone.2016.02.020
Claes L, Recknagel S, Ignatius A (2012) Fracture healing under healthy and inflammatory conditions. Nat Rev Rheumatol 8(3):133–143. https://doi.org/10.1038/nrrheum.2012.1
Sun L, Li X, Xu M et al (2020) In vitro immunomodulation of magnesium on monocytic cell toward anti-inflammatory macrophages. Regen Biomater 7(4):391–401. https://doi.org/10.1093/rb/rbaa010
Mahon OR, Browe DC, Gonzalez-Fernandez T et al (2020) Nano-particle mediated M2 macrophage polarization enhances bone formation and MSC osteogenesis in an IL-10 dependent manner. Biomaterials 239:119833. https://doi.org/10.1016/j.biomaterials.2020.119833
Yang F, Niu X, Gu X et al (2019) Biodegradable magnesium-incorporated poly(L-lactic acid) microspheres for manipulation of drug release and alleviation of inflammatory response. ACS Appl Mater Interface 11(26):23546–23557. https://doi.org/10.1021/acsami.9b03766
Tamaddon M, Wang L, Liu Z et al (2018) Osteochondral tissue repair in osteoarthritic joints: clinical challenges and opportunities in tissue engineering. Bio-Des Manuf 1(2):101–114. https://doi.org/10.1007/s42242-018-0015-0
Niu X, Liu Z, Tian F et al (2017) Sustained delivery of calcium and orthophosphate ions from amorphous calcium phosphate and poly(L-lactic acid)-based electrospinning nanofibrous scaffold. Sci Rep. https://doi.org/10.1038/srep45655
Niu X, Chen S, Tian F et al (2017) Hydrolytic conversion of amorphous calcium phosphate into apatite accompanied by sustained calcium and orthophosphate ions release. Mater Sci Eng C 70:1120–1124. https://doi.org/10.1016/j.msec.2016.04.095
Kotsakis GA, Thai A, Ioannou AL et al (2015) Association between low-dose aspirin and periodontal disease: results from the continuous national health and nutrition examination survey (NHANES) 2011–2012. J Clin Periodontol 42(4):333–341. https://doi.org/10.1111/jcpe.12380
Xu X, Zhang K, Zhao L et al (2016) Aspirin-based carbon dots, a good biocompatibility of material applied for bioimaging and anti-inflammation. ACS Appl Mater Interface 8(48):32706–32716. https://doi.org/10.1021/acsami.6b12252
Kidoaki S, Kwon IK, Matsuda T (2005) Mesoscopic spatial designs of nano- and microfiber meshes for tissue-engineering matrix and scaffold based on newly devised multilayering and mixing electrospinning techniques. Biomaterials 26(1):37–46. https://doi.org/10.1016/j.biomaterials.2004.01.063
Laha A, Sharma CS, Majumdar S (2017) Sustained drug release from multi-layered sequentially crosslinked electrospun gelatin nanofiber mesh. Mater Sci Eng C 76:782–786. https://doi.org/10.1016/j.msec.2017.03.110
Okuda T, Tominaga K, Kidoaki S (2010) Time-programmed dual release formulation by multilayered drug-loaded nanofiber meshes. J Contr Release 143(2):258–264. https://doi.org/10.1016/j.jconrel.2009.12.029
Kim K, Yu M, Zong XH et al (2003) Control of degradation rate and hydrophilicity in electrospun non-woven poly(D, L-lactide) nanofiber scaffolds for biomedical applications. Biomaterials 24(27):4977–4985. https://doi.org/10.1016/s0142-9612(03)00407-1
Tang Y, Singh J (2008) Controlled delivery of aspirin: effect of aspirin on polymer degradation and in vitro release from PLGA based phase sensitive systems. Int J Pharm 357(1–2):119–125. https://doi.org/10.1016/j.ijpharm.2008.01.053
Zheng L, Zhang L, Chen L et al (2018) Static magnetic field regulates proliferation, migration, differentiation, and YAP/TAZ activation of human dental pulp stem cells. Tissue Eng Regen Med 12(10):2029–2040. https://doi.org/10.1002/term.2737
Wei D, Qiao R, Dao J et al (2018) Soybean lecithin-mediated nanoporous PLGA microspheres with highly entrapped and controlled released BMP-2 as a stem cell platform. Small. https://doi.org/10.1002/smll.201800063
Cui W, Zhu X, Yang Y et al (2009) Evaluation of electrospun fibrous scaffolds of poly(DL-lactide) and poly(ethylene glycol) for skin tissue engineering. Mater Sci Eng C 29(6):1869–1876. https://doi.org/10.1016/j.msec.2009.02.013
Ru C, Wang F, Pang M et al (2015) Suspended, shrinkage-free, electrospun PLGA nanofibrous scaffold for skin tissue engineering. ACS Appl Mater Interface 7(20):10872–10877. https://doi.org/10.1021/acsami.5b01953
Acknowledgements
The authors gratefully acknowledge the financial support from the National Natural Science Foundation of China (Nos. 11872097, 82074463, 11827803, and U20A20390), the National Key R&D Program of China (No. 2020YFC0122204), the 111 Project (No. B13003), and the International Joint Research Center of Aerospace Biotechnology and Medical Engineering, Ministry of Science and Technology of China.
Author information
Authors and Affiliations
Contributions
FHY and XFN contributed to conceptualization; FHY, JXW, XYL, and ZZJ contributed to methodology; FHY contributed to investigation; FHY contributed to writing—original draft; QW, DZY, JYL, and XFN contributed to writing—review & editing; XFN contributed to funding acquisition; XFN provided the resources; JYL and XFN contributed to supervision.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest.
Ethical approval
This study does not contain any studies with human or animal subjects performed by any of the authors.
Rights and permissions
About this article
Cite this article
Yang, F., Wang, J., Li, X. et al. Electrospinning of a sandwich-structured membrane with sustained release capability and long-term anti-inflammatory effects for dental pulp regeneration. Bio-des. Manuf. 5, 305–317 (2022). https://doi.org/10.1007/s42242-021-00152-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42242-021-00152-5