Abstract
Purpose
Our aim was to study patients with diabetes mellitus and SARS-CoV-2-infection diagnosed during the first pandemic wave in Greece.
Methods
Cases were retrieved from the national database of SARS-CoV-2 infections.
Results
We studied 2624 SARS-CoV-2 infected cases, including 157 with diabetes. Patients with diabetes more often had other comorbidities (68.8 vs. 24.1%; p-value < 0.001). Among patients with diabetes, 149 (94.9%) developed symptomatic disease (COVID-19) compared to 1817 patients (73.7%) without diabetes (p-value < 0.001). A total of 126 patients with diabetes and COVID-19 were hospitalized and 41 died (27.5% case-fatality rate compared to 7.5% among patients without diabetes; p-value < 0.001). Patients with diabetes more often were hospitalized, developed complications, were admitted to the intensive care unit (ICU), received invasive mechanical ventilation, and died compared to patients without diabetes (p-values < 0.001 to 0.002 for all comparisons). Multivariate logistic regression analyses revealed that diabetes, having other comorbidities, and older age were significantly associated with higher risk for hospitalization, ICU admission, invasive mechanical ventilation, and death, and that obesity was significantly associated with higher risk for hospitalization, ICU admission, and mechanical intubation, while female gender protected against these outcomes.
Conclusion
COVID-19 is associated with increased rates of serious morbidity and adverse outcome in patients with diabetes and represents a severe illness for them.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In late 2019, a new betacoronavirus named severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) emerged and spread globally causing a pandemic of respiratory illness named coronavirus disease 2019 (COVID-19). According to the World Health Organization, as of May 25, 2021, more than 166 million laboratory-confirmed cases and nearly 3.5 million deaths have been recorded globally [1]. Studies have shown that patients with comorbidities, including diabetes mellitus (hereafter referred to as diabetes), have higher COVID-19-associated hospitalization rates and case fatality rates compared to patients without comorbidities [2,3,4,5]. As the pandemic evolves, it is of utmost importance to study the epidemiological and clinical profile of patients with severe COVID-19-associated morbidity and outcomes at the country level so as to guide interventions both at host level and at the levels of public health. In our recent study, we showed that increased age, male gender, presence of comorbidities, and number of comorbidities were significantly associated with severe COVID-19 or a fatal outcome [6]. Herein we explore the role of diabetes in patients with SARS-CoV-2 infection during the first pandemic wave in Greece based on data from the national database of SARS-CoV-2 infected cases.
Methods
SARS-CoV-2 infection is notifiable in Greece. Case-based data are collected from laboratories diagnosing SARS-CoV-2 infections through real-time reverse-transcriptase polymerase chain reaction (RT-PCR). In addition, physicians notify laboratory-confirmed SARS-CoV-2 cases via the mandatory notification form. A passive comprehensive system for hospitalized COVID-19 cases is also in place, collecting data daily about admission to the intensive care unit (ICU), invasive mechanical ventilation, complications, and outcome. For every COVID-19 case admitted to the ICU and every COVID-19-associated death, relevant information is collected actively via a phone interview with the physician in charge. Testing for SARS-CoV-2 infection, regardless of symptoms, is also performed for containment purposes.
This is an observational epidemiological study. The study period extended from February 26, 2020, through May 3, 2020 (first pandemic wave of SARS-CoV-2 infections in Greece). We retrieved data from the national database of SARS-CoV-2 infected cases. Data on clinical course, hospitalization, and outcome of patients were updated on September 30, 2020. Only cases with a recorded outcome (hospitalization, ICU admission, invasive mechanical ventilation, and death) were included in the statistical analysis. Patients with diabetes were contacted by telephone in order to collect data about type of diabetes, insulin therapy, and level of glycated hemoglobin A1c (HbA1c) at the time of diagnosis of SARS-CoV-2 infection.
SARS-CoV-2 infection was defined as a laboratory-confirmed infection with SARS-CoV-2 regardless of symptoms. COVID-19 was defined as a case with signs and symptoms compatible with COVID-19 and laboratory-confirmed SARS-CoV-2 infection. Laboratory-confirmed SARS-CoV-2 infection was defined as a case tested positive through RT-PCR. Fever was defined as a temperature of ≥ 37.5 °C twice within 24 h. A COVID-19-associated death was defined as a death in a COVID-19-classified case with no period of complete recovery between the illness and death and in the absence of a clear alternative cause of death. Diabetes and comorbidities were defined as notified by the physicians in charge or were self-reported by the patients. Comorbidities other than diabetes include chronic cardiovascular disease, hypertension, chronic pulmonary disease, chronic renal disease, chronic neurological disease, chronic neuromuscular disease, chronic hepatic disease, malignancy, immunosuppression, obesity, and high-risk pregnancy.
Descriptive statistics were used. Medians and means were calculated to describe the distribution of continuous variables and frequencies, and percentages were used for categorical variables. Comparisons between groups were performed by using the chi-square test for categorical variables and the t-test for continuous variables with normal distribution or the Mann–Whitney U test for non-parametric data. P-values of 0.05 or less were considered statistically significant. Logistic regression analyses were conducted to explore the factors that predict hospitalization, admission to ICU, mechanical ventilation, and death by using as independent variables the following factors: age, sex, diabetes, other comorbidities, and obesity. Adjusted odds ratio (OR) and confidence intervals (CIs) were estimated in order to control for confounders. We ran a missing values analysis and found no pattern among them, given that missing values were completely at random. The statistical analysis was conducted using the IBM-SPSS software version 26.0 for Windows, Armonk, NY, USA.
Written consent was not required given that the data were collected within the framework of national epidemiological surveillance. Data were managed in accordance with the national and European Union laws. The study was approved by the Ethics Committee of the National Public Health Organization.
Results
During the study period, a total of 2625 cases with SARS-CoV-2 infection were notified in Greece. One case was excluded because of unknown outcome. Therefore, 2624 cases were included in the analysis. Of these, 157 cases (6%) had diabetes. Table 1 shows the characteristics of the 157 patients with diabetes compared to patients without diabetes. Patients with diabetes in comparison to those without diabetes were significantly older (mean age 68.03 years vs. 46.78 years; p-value < 0.001), were more often males (65.6 vs. 54.7%; p-value = 0.008), and more often had other comorbidities (68.8 vs. 24.1%; p-value < 0.001).
In terms of type of diabetes, 59 out of 72 patients (81.9%) with diabetes for whom this information was available had diabetes type 2 and 13 (18.1%) had diabetes type 1. In addition, 20 out of 70 patients (28.6%) with diabetes for whom this information was available were on insulin therapy (13 with type 1 and 7 with type 2). Patients with diabetes had a mean HbA1c of 6.5% (range 5.8–14.0%) at the time of diagnosis of SARS-CoV-2 infection. Patients with type 1 diabetes had higher levels of HbA1c compared to patients with type 2 diabetes (mean value 8.4 vs. 6.3%).
Of the 157 patients with diabetes, 149 (94.9%) developed COVID-19 compared to 1817 patients (73.7%) without diabetes (p-value < 0.001). There was no significant difference between patients with and without diabetes with COVID-19 in terms of the mean time interval that elapsed between the onset of symptoms and testing (5.39 days vs. 5.77 days; p-value = 0.312).
Most patients with diabetes had fever at diagnosis (136 patients, 86.6%), followed by cough (70 patients, 44.6%), dyspnea (52 patients, 33.1%), weakness (38 patients, 24.2%), myalgias (22 patients, 14%), and diarrhea (16 patients, 10.2%); loss of taste and/or smell was reported in eight cases (5.1%).
A total of 126 patients with diabetes who developed COVID-19 were hospitalized (84.6% of all patients with diabetes and COVID-19 and 80.2% of all SARS-CoV-2-infected patients with diabetes). Overall, 75 patients with diabetes [out of 126 hospitalized patients (59.5%) with diabetes] developed at least one complication, including pneumonia (64 cases out of 126 hospitalized patients with diabetes, 50.8%), acute respiratory distress syndrome (49 cases out of 126 hospitalized patients, 38.9%), renal failure (nine cases out of 126 hospitalized patients, 7.1%), cardiovascular complications (five cases out of 126 hospitalized patients, 3.9%), and multiorgan failure (two cases out of 126 hospitalized patients, 1.8%). Forty-one of the 149 patients with diabetes who had COVID-19 died, which corresponds to a 27.5% case-fatality rate compared to 7.5% among non-diabetic patients with COVID-19 (p-value < 0.001) and an overall 32.5% in-hospital COVID-19-associated case fatality rate in the former group. Table 2 summarizes the morbidity and outcome of patients with COVID-19. Patients with diabetes more often were hospitalized, developed complications, were admitted to the ICU, received invasive mechanical ventilation, and died compared to non-diabetic patients (p-values < 0.001 for all comparisons). In particular, patients with diabetes accounted for 7.6% of all COVID-19 cases, 12.1% of all hospitalized cases, 18.1% of all cases admitted to the ICU, 18.7% of all cases on mechanical ventilation, and 23.2% of all fatal cases. Patients with and without diabetes did not differ significantly in terms of duration of hospitalization, duration of admission to the ICU, and duration of invasive mechanical ventilation (data not shown). In addition, there was no difference between patients with type 1 and type 2 diabetes regarding rates of hospitalization, ICU admission, invasive mechanical ventilation, and death (data not shown). However, patients with type 2 diabetes had significantly prolonged ICU stay compared to patients with type 1 diabetes (mean of 8.03 days vs. 1 day; p-value = 0.021), as well as significantly prolonged intubation period (mean of 8.7 days compared to 1 day; p-value = 0.019). Moreover, compared to patients with an HbA1c value of < 7%, patients with an HbA1c value of ≥ 7% significantly more frequently were admitted to ICU and were on mechanical ventilation (40 vs. 17.6% for both comparisons; p-values = 0.023). There was no statistically significant difference between patients with an HbA1c value of ≥ 7% and those with a value of < 7% in terms of rate of hospitalization, complications, or death (data not shown). Finally, among male patients without comorbidities, we found that only those with diabetes were more frequently hospitalized (65.3 vs. 43.2%; p-value = 0.003), were admitted to ICU (24.5 vs. 10.7%; p-value = 0.004), were on mechanical ventilation (22.4 vs. 9.8%; p-value = 0.006), and/or died (10.2 vs. 3.9%; p-value = 0.043) compared to patients without diabetes.
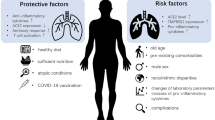
Table 3 summarizes the results of the multivariate logistic regression analyses. Diabetes, having at least one other comorbidity, and older age were significantly associated with an increased probability for hospitalization, ICU admission, invasive mechanical ventilation and death, while female gender consistently protected against all abovementioned outcomes. Finally, obesity was significantly associated with increased risk for hospitalization, ICU admission, and mechanical ventilation.
Discussion
We studied the role of diabetes in the clinical course and outcome of 157 patients with SARS-CoV-2 infection out of a total of 2624 SARS-CoV-2 infected cases in Greece. In line with other studies [7,8,9,10,11,12], diabetes was an independent factor for a significant COVID-19-associated morbidity burden and adverse outcome, including the development of complications, hospitalization, ICU admission, invasive mechanical ventilation, and death, an overall case fatality rate of 27.5% and an in-hospital case fatality rate of 32.5%. Similarly, in a nationwide register-based study from England, an in-hospital COVID-19 related fatality rate of 31.4% was estimated among patients with type 2 diabetes [9]. In contrast, a case fatality rate of 16.46% was reported in Lombardy, Italy, during the first pandemic wave [5]. Furthermore, a US cohort study of 4536 patients with SARS-CoV-2 infection reported a 39.7% hospitalization rate among patients with diabetes, which is significantly lower than the 84.5% hospitalization rate in our study [8]. A prospective cohort study conducted in a healthcare network of 137 locations in the US showed an overall 3.35-fold increased risk for COVID-19-associated severity, regardless of type of diabetes [13]. Similarly to ours, a study that analyzed data from the UK Biobank Community Cohort concerning individuals older than 65 years found a 1.73 increased risk for hospitalization and a 3.11 increased risk for death among patients with type II diabetes compared to non-diabetic patients [7]. However, in a single-center study from Hubei, China, patients with diabetes accounted for 24.9% of 193 patients with severe COVID-19, which is a higher rate than ours [11]. A recent systemic review and meta-analysis of 18 studies (16 from China, one from the US, and one from Italy), with a total of 14,558 patients with COVID-19, found that diabetes was an independent risk factor for severe COVID-19 by a risk ratio of 2.11, along with hypertension, cardiovascular disease, chronic obstructive pulmonary disease, and cancer [14]. A recently published meta-analysis by Wu et al. of nine original studies showed that diabetes increases the mortality of patients with COVID-19, with a pooled OR of 1.75, which is similar to ours [15]. Therefore, COVID-19 should be considered as a severe illness for patients with diabetes. However, the COVID-19-associated infection-fatality rates and respective differences across studies should be cautiously interpreted bearing in mind that they represent crude rather than attributed fatality rates. Indeed, other coexisting factors that may influence the outcome of the cases were not considered, including, for example, multidrug-resistant infections. In addition, case fatality rates have improved as the COVID-19 pandemic has evolved and have been lower in subsequent pandemic waves. For instance, the overall infection-fatality rate was estimated at 3.5% at the peak of the third pandemic wave in Greece [6].
In agreement with other studies [7, 8, 11, 14, 16], we noted that male gender, the presence of comorbidities in addition to diabetes, and older age were also significantly associated with higher rates of hospitalization, ICU admission, invasive mechanical ventilation, and death. In a retrospective observational cohort study of 3988 patients (median age 63 years) with COVID-19 requiring treatment in the ICU in Lombardy, Italy, independent risk factors associated with mortality included older age, male gender, high fraction of inspired oxygen and high positive end-expiratory pressure on ICU admission, chronic obstructive pulmonary disease, hypercholesterolemia, and type 2 diabetes (hazard ratios: 1.75, 1.57, 1.14, 1.04, 1.68, 1.25, and 1.18, respectively) [16]. We found an OR of 1.66 for COVID-19-associated death in our patients with diabetes. In our series, approximately two-thirds of patients with diabetes had at least one other comorbidity. Several comorbidities encountered in our patients with diabetes (e.g., chronic cardiovascular disease, chronic renal disease, hypertension, and obesity) may interrelate with each other in the context of diabetes, therefore the impact of each of them on the clinical course and outcome of COVID-19 is not ease to estimate [17]. We also found that older age was independently associated with a poor outcome, as reported by others [7, 8, 16], which is attributed to the age-related dysregulation and decline of the immune system in older adults (immunosenescence). In 2020, people older than 65 years accounted for approximately 20% of the European population [18, 19]. The increase of life expectancy partially accounts for the increased COVID-19-associated case fatality rate and the unprecedented pressure on healthcare systems in several European countries [20]. The demographic and high-risk profile of patients with COVID-19 requiring hospitalization and admission to the ICU should be meticulously examined for the purpose of planning healthcare services to more adequately deal with the ongoing COVID-19 pandemic [21].
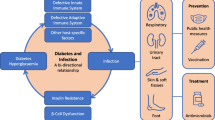
Diabetes and uncontrolled glycemia were reported as significant predictors of severity and deaths in patients infected with different viruses, including the 2009 influenza A/H1N1 pandemic, SARS-Co-V, and the Middle East respiratory syndrome coronavirus [22,23,24]. Similarly, a large population-based cohort study conducted in the UK in patients with diabetes found significantly increased COVID-19-related mortality rates in patients with increased HbA1c values (> 10 vs. < 7%) in patients with type 1 diabetes and in patients with type 2 diabetes mellitus (HbA1c values > 7 vs. < 7% [25]. In our study, we found that an HbAc1 value of ≥ 7 was associated with increased risk for admission to the ICU and mechanical ventilation. Moreover, several pathogenetic mechanisms are potentially implicated in the increased morbidity and mortality of patients with diabetes. These include a compromised immune system, which translates to inefficient immune response against COVID-19 (dysfunction of granulocytes, monocytes/macrophages, natural killer cells, B cells, and T cells), an increased systemic cytokine response (cytokine storm) which may predispose to organ damage, and abnormal angiotensin-converting enzyme 2 (ACE2) expression (receptor of cellular entry of SARS-CoV-2), which translates to increased risk of severe lung injury and uncontrolled hyperglycemia due to dysfunction of the pancreas [10, 26,27,28,29,30]. SARS-CoV-2 can also infect and replicate in human pancreatic islets, while a profound proinflammatory response may also contribute to the injury of pancreatic cells [31]. Furthermore, other comorbidities that are common in patients with diabetes may also predispose to an unfavorable clinical course and outcome: for example, obesity is often associated with a chronic systemic inflammation, insulin resistance, hypertension, coagulopathy, and thrombosis, which additionally contribute to clinical deterioration per se [26, 27, 29, 30]. Indeed, in our study, obesity was an independent factor for increased risk for hospitalization, ICU admission, and invasive mechanical ventilation. Similarly, an observational multi-center study of 90 critically ill patients (median age: 65.5 years) with COVID-19 diagnosed until April 13, 2020 in Greece found that type 2 diabetes and obesity contributed to disease severity and mortality [32].
A limitation of the current study is the fact that the criteria for testing for SARS-CoV-2 infection and hospitalization changed during the study period. Another limitation is the fact that detailed information on the type of diabetes and the need for insulin therapy during hospitalization, the type of antidiabetic therapy, and the duration of diabetes were not available for several patients with diabetes. In addition, it is possible that some patients may have had undiagnosed diabetes and were misclassified as non-diabetic. Overall, the number of studied patients with diabetes and COVID-19 is rather small, which means that definitive conclusions should be avoided. A clear strength of our study is the analysis of 2624 SARS-CoV-2 cases that were retrieved from the national surveillance database. Another strength is the fact that the data were collected prospectively and that we followed the outcome of all our patients, which is not the case in most published series on COVID-19 patients with diabetes.
Conclusions
The current study offers insight into the role of diabetes in SARS-CoV-2 infection in Greece. Diabetes is a major driver of COVID-19-associated severe morbidity and mortality and should therefore be considered a serious illness for patients with diabetes. This risk is particularly pronounced among men, older patients, patients with other comorbidities, and obese patients. These findings should be taken into consideration by policy makers so that they may determine what may be the optimal public health interventions with regard to health system planning and containment measures as well as vaccination policies against COVID-19. Further research is needed in order to elucidate the specific pathogenetic mechanisms of disease severity and unfavorable outcome in this high-risk group of patients.
Data availability
Data are available upon request from the National Public Health Organization.
References
World Health Organization (2021) Coronavirus disease (COVID-19) pandemic. https://www.who.int/emergencies/diseases/novel-coronavirus-2019. Accessed 27 May 2021
Yang X, Yu Y, Xu J, Shu H, Xia J, Liu H, Wu Y, Zhang L, Yu Z, Fang M, Yu T, Wang Y, Pan S, Zou S, Yuan S, Shang Y (2020) Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: a single-centered, retrospective, observational study. Lancet Respir Med 8:475–481
Deng X, Yang J, Wang W, Wang X, Zhou J, Chen Z, Li J, Chen Y, Yan H, Zhang J, Zhang Y, Wang Y, Qiu Q, Gong H, Wei X, Wang L, Sun K, Wu P, Ajelli M, Cowling BJ, Viboud C, Yu H (2020) Case fatality risk of the first pandemic wave of novel coronavirus disease 2019 (COVID-19) in China. Clin Infect Dis May 15:ciaa578. https://doi.org/10.1093/cid/ciaa578 (Online ahead of print).
Chen R, Liang W, Jiang M, Guan W, Zhan C, Wang T, Tang C, Sang L, Liu J, Ni Z, Hu Y, Liu L, Shan H, Lei C, Peng Y, Wei L, Liu Y, Hu Y, Peng P, Wang J, Liu J, Chen Z, Li G, Zheng Z, Qiu S, Luo J, Ye C, Zhu S, Liu X, Cheng L, Ye F, Zheng J, Zhang N, Li Y, He J, Li S, Zhong N (2020) Risk factors of fatal outcome in hospitalized subjects with coronavirus disease 2019 from a nationwide analysis in China. Chest 158:97–105
Poletti P, Tirani M, Cereda D, Trentini F, Guzzetta G, Marziano V, Buoro S, Riboli S, Crottogini L, Piccarreta R, Piatti A, Grasselli G, Melegaro A, Gramegna M, Ajelli M, Merler S (2020) Age-specific SARS-CoV-2 infection fatality ratio and associated risk factors, Italy, February to April 2020. Euro Surveill 25:2001383
Maltezou HC, Papadima K, Gkolfinopoulou K, Ferentinos G, Mouratidou E, Andreopoulou A, Pavli A, Magaziotou I, Georgakopoulou T, Mellou K, Vorou R, Antoniadou A, Stathakarou A, Chrysochoou A, Gogos C, Karaiskou A, Kotanidou A, Koutsoukou A, Marangos M, Mentis A, Metallidis S, Papa A, Pefanis A, Tsakris A, Sipsas NV (2021) Coronavirus disease 2019 pandemic in Greece, February 26 – May 3, 2020: the first wave. Trav Med Infect Dis 2021;41:102051
Atkins JL, Masoli JAH, Delgado J, Pilling LC, Kuo CL, Kuchel GA, Melzer D (2020) Preexisting comorbidities predicting COVID-19 and mortality in the UK Biobank community cohort. J Gerontol A Biol Sci Med Sci 75:2224–2230
Jehi L, Ji X, Milinovich A, Erzurum S, Merlino A, Gordon S, Young JB, Kattan MW (2020) Development and validation of a model for individualized prediction of hospitalization risk in 4,536 patients with COVID-19. PLoS One 15;e0237419
Barron E, Bakhai C, Kar P, Weaver A, Bradley D, Ismail H, Knighton P, Holman N, Khunti K, Sattar N, Wareham NJ, Young B, Valabhji J (2020) Associations of type 1 and type 2 diabetes with COVID-19-related mortality in England; a whole-population study. Lancet Diabetes Endocrinol 8:813–822
Vas P, Hopkins D, Feher M, Rubino F, Whyte MB (2020) Diabetes, obesity and COVID-19: a complex interplay. Diabetes Obes Metab 22:1892–1896
Yan Y, Yang Y, Wang F, Ren H, Zhang S, Shi X, Yu X, Dong K (2020) Clinical characteristics and outcomes of patients with severe covid-19 with diabetes. BMJ Open Diabetes Res Care 8;e001343
Dennis JM, Mateen BA, Sonabend R, Thomas NJ, Patel KA, Hattersley AT, Denaxas S, McGovern AP, Vollmer SJ (2021) Type 2 diabetes and COVID-19-related mortality in the critical care setting: a national cohort study in England, March-July 2020. Diabetes Care 44:50–57
Gregory JM, Slaughter JC, Duffus SH, Smith J, LeStourgeon LM, Jaser SS, McCoy AB, Luther JM, Giovannetti ER, Boeder S, Pettus JH, Moore DJ (2021) COVID-19 severity is tripled in the diabetes community: a prospective analysis of the pandemic’s impact in type 1 and type 2 diabetes. Diabetes Care 44:526–532
Singh AK, Gillies CL, Singh R, Singh A, Chudasama Y, Coles B, Seidu S, Zaccardi F, Davies MJ, Khunti K (2020) Prevalence of co-morbidities and their association with mortality in patients with COVID-19: a systematic review and meta-analysis. Diabetes Obes Metab 22:1915–1924
Wu ZH, Tang Y, Cheng Q (2021) Diabetes increases the mortality of patients with COVID-19: a meta-analysis. Acta Diabetol 58:139–144
Grasselli G, Greco M, Zanella A, Albano G, Antonelli M, Bellani G, Bonanomi E, Cabrini L, Carlesso E, Castelli G, Cattaneo S, Cereda D, Colombo S, Coluccello A, Crescini G, Forastieri Molinari A, Foti G, Fumagalli R, Iotti GA, Langer T, Latronico N, Lorini FL, Mojoli F, Natalini G, Pessina CM, Ranieri VM, Rech R, Scudeller L, Rosano A, Storti E, Thompson BT, Tirani M, Villani PG, Pesenti A, Cecconi M, COVID-19 Lombardy ICU Network (2020) Risk factors associated with mortality among patients with COVID-19 in intensive care units in Lombardy, Italy. JAMA Intern Med 180:1345-1355
Huang Y, Lu Y, Huang YM, Wang M, Ling W, Sui Y, Zhao HL (2020) Obesity in patients with COVID-19: a systematic review and meta-analysis. Metabolism 113: 154378
Eurostat. Population structure by major age groups, EU-28, 2018–2100 (2020). https://ec.europa.eu/eurostat/statistics-explained/images/d/de/Population_structure_by_major_age_groups%2C_EU-28%2C_2018-2100_%28%25_of_total_population%29.png. Accessed 27 May 2021
Hellenic Statistical Authority (2011) Demographic characteristics 2011. https://www.statistics.gr/el/statistics/-/publication/SAM03/. Accessed 27 May 2021 [in Greek]
Verelst F, Kuylen E, Beutels P (2020) Indications for healthcare surge capacity in European countries facing an exponential increase in coronavirus disease (COVID-19) cases, March 2020. Euro Surveill 25:2000323
Hill MA, Sowers JR, Mantzoros CS (2021) COVID-19 and obesity pandemics converge into a syndemic requiring urgent and multidisciplinary action. Metabolism 114:154408
Schoen K, Horvat N, GuerreiroNicolau FC, de Castro Isac, de Giassi Karina S (2019) Spectrum of clinical and radiographic findings in patients with diagnosis of H1N1 and correlation with clinical severity. BMC Infect Dis 19:964
Yang JK, Feng Y, Yuan MY, Yuan SY, Fu HJ, Wu BY, Sun GZ, Yang GR, Zhang XL, Wang L, Xu X, Xu XP, Chan JCN (2006) Plasma glucose levels and diabetes are independent predictors for mortality and morbidity in patients with SARS. Diabet Med 23:623–628
Banik GR, Alqahtani AS, Booy R, Rashid H (2016) Risk factors for severity and mortality in patients with MERS-CoV: analysis of publicly available data from Saudi Arabia. Virol Sin 31:81–84
Holman N, Knighton P, Kar P, O’Keefe J, Curley M, Weaver A, Barron E, Bakhai C, Khunti K, Wareham NJ, Sattar N, Young B, Valabhji J (2020) Risk factors for COVID-19-related mortality in people with type 1 and type 2 diabetes in England: a population-based cohort study. Lancet Diabetes Endocrinol 8:823–833
Cuschieri S, Grech S (2020) COVID-19 and diabetes: the why, the what and the how. J Diabetes Complications 34:107637
Rajpal A, Rahimi L, Ismail-Beigi F (2020) Factors leading to high morbidity and mortality of COVID-19 in patients with type 2 diabetes. J Diabetes 12:895–908
Hamer M, Gale CR, Batty GD (2020) Diabetes, glycaemic control, and risk of COVID-19 hospitalisation: population-based, prospective cohort study. Metabolism 112:154344. https://doi.org/10.1016/j.metabol.2020.154344 (Online ahead of print)
Trougakos IP, Stamatelopoulos K, Terpos E, Tsitsilonis OE, Aivalioti E, Paraskevis D, Kastritis E, Pavlakis GN, Dimopoulos MA (2021) Insights to SARS-CoV-2 life cycle, pathophysiology, and rationalized treatments that target COVID-19 clinical complications. J Biomed Sci 28:9. https://doi.org/10.1186/s12929-020-00703-5
Gautret P, Million M, Jarrot PA, Camoin-Jau L, Colson P, Fenollar F, Leone M, La Scola B, Devaux C, Gaubert JY, Mege JL, Vitte J, Melenotte C, Rolain JM, Parola P, Lagier JC, Brouqui P, Raoult D (2020) Natural history of COVID-19 and therapeutic options. Exp Rev Clin Immunol 16:1159–1184
Maltezou HC, Pavli A, Tsakris A (2021) Post-COVID syndrome: an insight on its pathogenesis. Vaccines (Basel) 9:497. https://doi.org/10.3390/vaccines9050497
Halvatsiotis P, Kottanidou A, Tzannis K, Jahaj E, Magira E, Theodorakopoulou M, Konstandopoulou G, Gkeka E, Pourzitaki C, Kapravelos N, Papoti S, Sileli M, Gogos C, Velissaris D, Markou N, Stefanatou E, Vlachogianni G, Aimoniotou E, Komnos A, Zafeiridis T, Koulouvaris P, Armaganidis A, Bamias A, Dimopoulos G (2020) Demographic and clinical features of critically ill patients with COVID-19 in Greece: the burden of diabetes and obesity. Diabetes Res Clin Pract 166, 108331
Acknowledgements
We thank the healthcare personnel and especially the Infection Control Committees and the laboratory personnel of the hospitals for their assistance in collecting data. We also thank Anastasia Tedoma for technical assistance. The opinions presented in this article are those of the authors and do not necessarily represent those of their institutions.
Author information
Authors and Affiliations
Contributions
Conceptualization, N.V.S. and N.T.; writing of the research protocol: H.C.M. and A.T.; software, V.R.; formal analysis, P.T, A.P., A.B., K.P. A.T. and M.N.G.; investigation, H.C.M., P.T., A.P., A.B., K.P. and A.A.; data curation, H.C.M., K.P. and A.A.; writing—original draft preparation, H.C.M. and V.R.; review and editing, P.T., A.P, A.B., K.P., A.A., A.T., M.N.G., N.V.S. and N.T.; and supervision, H.C.M., N.V.S. and N.T. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Ethics approval
The study was conducted according to the guidelines of the Declaration of Helsinki, and approved by the Research Committee of the National Public Health Organization.
Informed consent statement
Patient consent was waived given that data were collected within the framework of the national surveillance of SARS-CoV-2 infections.
Conflicts of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Maltezou, H.C., Pavli, A., Tsonou, P. et al. Role of diabetes mellitus in the clinical course and outcome of SARS-CoV-2 infected patients. Hormones 21, 221–227 (2022). https://doi.org/10.1007/s42000-021-00342-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42000-021-00342-x