Abstract
Background
The Self-Efficacy Measure for Sleep Apnea (SEMSA) is a 26-item questionnaire that investigates perceived risks, outcome expectancies and self-efficacy, i.e., the confidence to undertake treatment, in the context of continuous positive airway pressure (CPAP) interventions for sleep apnea syndrome. This questionnaire can be considered too lengthy for clinical practice; therefore, a shortened version is needed.
Methods
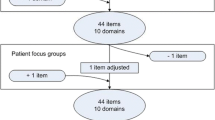
290 adults undergoing CPAP treatment completed the SEMSA-26. An item reduction process took into account both the results of statistical analyses and the expertise of a steering committee. Construct validity, reliability and external validity were tested for a 15-item short version. Additionally, CPAP adherence (usage more than 4 h per night) was collected, and receiver operating characteristics analyses were performed to establish the cut-off point of the SEMSA-15 that would best classify patients depending on their adherence.
Results
The structure of the SEMSA-15 was confirmed by principal components factor analysis. Cronbach’s alpha coefficients ranged from 0.66 to 0.86. The SEMSA-15 dimension scores were highly correlated with their respective SEMSA-26 dimension scores. The self-efficacy sub-score of the SEMSA-15 obtained the best classification performance, with a cut-off point of 2.78 to predict CPAP adherence.
Conclusion
The SEMSA-15 seems to be appropriate for use in clinical practice to investigate beliefs and perception of self-efficacy in CPAP interventions. It is, therefore, a useful tool to predict long-term adherence to treatment.

Similar content being viewed by others
References
Lévy P, Kohler M, McNicholas WT, et al. Obstructive sleep apnoea syndrome. Nat Rev Dis Primer. 2015;1:15015. https://doi.org/10.1038/nrdp.2015.15.
Malhotra A, White DP. Obstructive sleep apnoea. Lancet. 2002;360:237–45. https://doi.org/10.1016/S0140-6736(02)09464-3.
Bhatia M, Singh Y. CPAP compliance in obstructive sleep apnea. Sleep Vigil. 2019. https://doi.org/10.1007/s41782-019-00070-8.
Gay P, Weaver T, Loube D, Iber C. Evaluation of positive airway pressure treatment for sleep related breathing disorders in adults. Sleep. 2006;29:381–401. https://doi.org/10.1093/sleep/29.3.381.
Engleman HM, Wild MR. Improving CPAP use by patients with the sleep apnoea/hypopnoea syndrome (SAHS). Sleep Med Rev. 2003;7:81–99. https://doi.org/10.1053/smrv.2001.0197.
Bandura A. Self-efficacy: the exercise of control. Macmillan; 1997.
Schwarzer R, Fuchs R. Self-efficacy and health behaviours. In: Conner M, Norman P, editors. Predicting health behaviour. Philadelphia: Open University Press; 1996. p. 18.
Philip P, Bioulac S, Altena E, et al. Specific insomnia symptoms and self-efficacy explain CPAP compliance in a sample of OSAS patients. PLoS ONE. 2018;13:e0195343. https://doi.org/10.1371/journal.pone.0195343.
Stepnowsky CJ, Marler MR, Ancoli-Israel S. Determinants of nasal CPAP compliance. Sleep Med. 2002;3:239–47. https://doi.org/10.1016/S1389-9457(01)00162-9.
Micoulaud-Franchi J-A, Monteyrol P-J, Guichard K, et al. Déterminants psychologiques et adhérence au traitement par pression positive continue: des outils pratiques pour une médecine du sommeil intégrative. Médecine Sommeil. 2017;14:99–111. https://doi.org/10.1016/j.msom.2017.04.001.
Micoulaud-Franchi J-A, Coste O, Bioulac S, et al. A French update on the Self-Efficacy Measure for Sleep Apnea (SEMSA) to assess continuous positive airway pressure (CPAP) use. Sleep Breath. 2019;23:217–26. https://doi.org/10.1007/s11325-018-1686-7.
Weaver TE, Maislin G, Dinges DF, et al. Self-efficacy in sleep apnea: instrument development and patient perceptions of obstructive sleep apnea risk, treatment benefit, and volition to use continuous positive airway pressure. Sleep. 2003;26:727–32. https://doi.org/10.1093/sleep/26.6.727.
Ware JE. Improvements in short-form measures of health status: introduction to a series. J Clin Epidemiol. 2008;61:1–5. https://doi.org/10.1016/j.jclinepi.2007.08.008.
Andermann A, Blancquaert I, Beauchamp S, Déry V. Revisiting Wilson and Jungner in the genomic age: a review of screening criteria over the past 40 years. Bull World Health Organ. 2008;86:317–9. https://doi.org/10.1590/S0042-96862008000400018.
Wilson JMG, Jungner G. Principles and practice of screening for disease. Geneva: World Health Organization; 1968.
van der Linden WJ, Hambleton RK. Handbook of modern item response theory. Berlin: Springer; 2013.
Campbell DT, Fiske DW. Convergent and discriminant validation by the multitrait-multimethod matrix. Psychol Bull. 1959;56:81–105. https://doi.org/10.1037/h0046016.
Cronbach LJ, Meehl PE. Construct validity in psychological tests. Psychol Bull. 1955;52:281–302. https://doi.org/10.1037/h0040957.
Steffen M. Universalism, responsiveness, sustainability—regulating the French Health Care System. N Engl J Med. 2016;374:401–5. https://doi.org/10.1056/NEJMp1504547.
Shapiro GK, Shapiro CM. Factors that influence CPAP adherence: an overview. Sleep Breath. 2010;14:323–35. https://doi.org/10.1007/s11325-010-0391-y.
Parish JM, Lyng PJ. Quality of life in bed partners of patients with obstructive sleep apnea or hypopnea after treatment with continuous positive airway pressure. Chest. 2003;124:942–7. https://doi.org/10.1378/chest.124.3.942.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Research involving human participants and/or animals
This study was conducted in accordance with the Declaration of Helsinki and French Good Clinical Practices.
Informed consent
All subjects provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Dupuy, L., Bioulac, S., Coste, O. et al. Proposition of a Shortened Version of the Self-efficacy Measure for Sleep Apnea (SEMSA-15): Psychometric Validation and Cut-Off Score for CPAP Adherence. Sleep Vigilance 4, 17–21 (2020). https://doi.org/10.1007/s41782-020-00083-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s41782-020-00083-8