Abstract
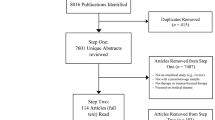
This study is an attempt to explore war-related trauma, its stressful effects, and the coping strategies of Saudi schoolchildren. The authors hypothesized that children exposed to war-related trauma will show higher levels of PTSD, and that those with higher levels of PTSD symptoms use more maladaptive coping strategies. The study describes the correlation between traumatic events and posttraumatic stress disorder (PTSD) as well as coping strategies. Five hundred twenty-seven intermediate and high school students, 12 to 18 years old, living in the conflict zone in southern Saudi Arabia completed three standardized self-reported scales: the War Zone Traumatic Events Checklist, the Child PTSD Symptom Scale, and the Children’s Coping Strategies Checklist. Each participating student was randomly chosen. Analysis was based on two groups: the high-PTSD symptoms group (182 children) and the low-PTSD symptoms group (345 children). The study was conducted between September 2020 and April 2022 while the war was ongoing as part of an ongoing larger study. Children exposed to war-related traumatic events exhibited greater prevalence rates for PTSD. The children reported high levels of PTSD symptoms and applied a variety of coping strategies to manage related stress. Participants rarely reported that psychological or educational interventions had been used to manage the war-related traumatic experiences and PTSD or to improve related coping styles. The results are discussed in the context of mental health services needed for children in the conflict zone. To bridge the gap between health care services and the needs of children with PTSD, and for better understanding and interventions, health professionals are invited to develop a biopsychosocial model that identifies the risks of PTSD related to exposure to war-related traumatic events in school-aged children and, hence, provide a multidisciplinary intervention program that educates, encourages, and supports teachers and parents in following medical recommendations and goals.
Similar content being viewed by others
References
Abdelaziz, T., Abdulla, T., & Vostanis, P. (2013). Coping strategies of children and adolescents exposed to war conflict. Arabpsynet E Journal, 39(40), 289–295. https://refugeeresearch.net/wp-content/uploads/2017/06/Coping-strategies-of-children-and-adolescents-exposed-to-war-conflict.pdf.
Ahmad, A., Sofi, M. A., Sundelin-Wahlsten, V., & von Knorring, A. L. (2000). Posttraumatic stress disorder in children after the military operation Anfal in Iraqi Kurdistan. European Child & Adolescent Psychiatry, 9(4), 235–243. https://doi.org/10.1007/s007870070026.
Ahmed, S., & Amer, M. M. (Eds.). (2013). Counseling muslims: Handbook of mental health issues and interventions. Routledge.
Al-Ammar, F. (2018). Post-traumatic stress disorder among Yemeni children as a consequence of the ongoing war CARPO. https://carpo-bonn.org/wp-content/uploads/2018/03/10_carpo_brief_final.pdf.
Alghamdi, M. (2020). Resilience and trauma in the Southern Border conflict region of Saudi Arabia. Mediterranean Journal of Clinical Psychology, 8(2). https://doi.org/10.6092/2282-1619/mjcp-2386.
Allwood, M. A., Bell-Dolan, D., & Husain, S. A. (2002). Children’s trauma and adjustment reactions to violent and nonviolent war experiences. Journal of the American Academy of Child & Adolescent Psychiatry, 41(4), 450–457. https://doi.org/10.1097/00004583-200204000-00018.
Amnesty International. (21 (October, 2013). Will I be next? US drone strikes in Pakistan. https://www.amnestyusa.org/reports/willi-be-next-us-drone-strikes-in-pakistan/.
An, Y., Fu, F., Wu, X., Lin, C., & Zhang, Y. (2013). Longitudinal relationships between neuroticism, avoidant coping, and posttraumatic stress disorder symptoms in adolescents following the 2008 Wenchuan earthquake in China. Journal of Loss and Trauma, 18(6), 556–571. https://doi.org/10.1080/15325024.2012.719351.
Arega, N. T. (2023). March). Mental health and psychosocial support interventions for children affected by armed conflict in low-and middle-income countries: A systematic review. Child & Youth Care Forum, 52, 1431–1456. https://doi.org/10.1007/s10566-023-09741-0.
Attanayake, V., McKay, R., Joffres, M., Singh, S., Burkle, F. Jr., & Mills, E. (2009). Prevalence of mental disorders among children exposed to war: A systematic review of 7,920 children. Medicine Conflict and Survival, 25(1), 4–19. https://doi.org/10.1080/13623690802568913.
Ayers, T. A., & Sandler, I. N. (1999). Manual for the children’s coping strategies Checklist & the how I coped under pressure scale. Arizona State University. https://www.yumpu.com/en/document/read/12240213/manual-for-the-childrens-coping-strategies-checklist.
Babicka-Wirkus, A., Wirkus, L., Stasiak, K., & Kozłowski, P. (2021). University students’ strategies of coping with stress during the coronavirus pandemic: Data from Poland. PloS ONE, 16(7), e0255041. https://doi.org/10.1371/journal.pone.0255041.
Bartone, P. T., & Homish, G. G. (2020). Influence of hardiness, avoidance coping, and combat exposure on depression in returning war veterans: A moderated-mediation study. Journal of Affective Disorders, 265, 511–518. https://doi.org/10.1016/j.jad.2020.01.127.
Benuto, L. T., Yang, Y., Bennett, N., & Lancaster, C. (2022). Distress tolerance and emotion regulation as potential mediators between secondary traumatic stress and maladaptive coping. Journal of Interpersonal Violence, 37(13–14), NP11557–NP11581. https://doi.org/10.1177/0886260520967136.
Black, J. M., & Hoeft, F. (2015). Utilizing biopsychosocial and strengths-based approaches within the field of child health: What we know and where we can grow. New Directions for Child and Adolescent Development, 2015(147), 13–20. https://doi.org/10.1002/cad.20089.
Bürgin, D., Anagnostopoulos, D., Vitiello, B., Sukale, T., Schmid, M., FegertJM, & Board and Policy Division of ESCAP. (2022). Impact of war and forced displacement on children’s mental health-multilevel, needs-oriented, and trauma-informed approaches. European Child & Adolescent Psychiatry, 31(6), 845–853. https://doi.org/10.1007/s00787-022-01974-z.
Catani, C. (2018). Mental health of children living in war zones: A risk and protection perspective. World Psychiatry, 17(1), 104–105. https://doi.org/10.1002/wps.20496.
Cénat, J. M., McIntee, S. E., & Blais-Rochette, C. (2020). Symptoms of posttraumatic stress disorder, depression, anxiety and other mental health problems following the 2010 earthquake in Haiti: A systematic review and meta-analysis. Journal of Affective Disorders, 273, 55–85. https://doi.org/10.1016/j.jad.2020.04.046.
Chun, C. A., Moos, R. H., & Cronkite, R. C. (2006). Culture: A fundamental context for the stress and coping paradigm. In P. T. P. Wong & L. C. J. Wong (Eds.), Handbook of multicultural perspectives on stress and coping (pp. 29–53). Spring Publications. https://doi.org/10.1007/0-387-26238-5_2.
Diab, M., Peltonen, K., Qouta, S. R., Palosaari, E., & Punamäki, R. L. (2019). Can functional emotion regulation protect children’s mental health from war trauma? A Palestinian study. International Journal of Psychology, 54(1), 42–52. https://doi.org/10.1002/ijop.12427.
Ehntholt, K. A., & Yule, W. (2006). Practitioner review: Assessment and treatment of refugee children and adolescents who have experienced war-related trauma. Journal of Child Psychology and Psychiatry, 47(12), 1197–1210. https://doi.org/10.1111/j.1469-7610.2006.01638.x.
El Hatw, M. M., Taher, E., El Hamidi, A. A., A., & Alturkait, F. A. (2015). The association of exposure to the 2009 south war with the physical, psychological, and family well-being of Saudi children. Saudi Medical Journal, 36(1), 73–81. https://doi.org/10.15537/smj.2015.1.9494.
El-Khodary, B., & Samara, M. (2019). The mediating role of trait emotional intelligence, prosocial behaviour, parental support and parental psychological control on the relationship between war trauma, and PTSD and depression. Journal of Research in Personality, 81, 246–256. https://doi.org/10.1016/j.jrp.2019.06.004.
El-Khodary, B., Samara, M., & Askew, C. (2020). Traumatic events and PTSD among Palestinian children and adolescents: The effect of demographic and socioeconomic factors. Frontiers in Psychiatry, 11, 4. https://doi.org/10.3389/fpsyt.2020.00004.
Eltanamly, H., Leijten, P., Jak, S., & Overbeek, G. (2021). Parenting in times of war: A meta-analysis and qualitative synthesis of war exposure, parenting, and child adjustment. Trauma. Violence & Abuse, 22(1), 147–160. https://doi.org/10.1177/1524838019833001.
Engel, G. L. (1977). The need for a new medical model: A challenge for biomedicine. Science, 196(4286), 129–136. https://www.urmc.rochester.edu/MediaLibraries/URMCMedia/medical-humanities/documents/Engle-Challenge-to-Biomedicine-Biopsychosicial-Model.pdf.
Feldman, R., & Vengrober, A. (2011). Posttraumatic stress disorder in infants and young children exposed to war-related trauma. Journal of the American Academy of Child & Adolescent Psychiatry, 50(7), 645–658. https://doi.org/10.1016/j.jaac.2011.03.001.
Fino, E., Mema, D., & Russo, P. M. (2020). War trauma exposed refugees and posttraumatic stress disorder: The moderating role of trait resilience. Journal of Psychosomatic Research, 129, 109905. https://doi.org/10.1016/j.jpsychores.2019.109905.
Foa, E. B., Asnaani, A., Zang, Y., Capaldi, S., & Yeh, R. (2018). Psychometrics of the child PTSD Symptom Scale for DSM-5 for trauma-exposed children and adolescents. Journal of Clinical Child & Adolescent Psychology, 47(1), 38–46. https://doi.org/10.1080/15374416.2017.1350962.
Garcia, F. E., Barraza-Pena, C. G., Wlodarczyk, A., Alvear-Carrasco, M., & Reyes-Reyes, A. (2018). Psychometric properties of the Brief-COPE for the evaluation of coping strategies in the Chilean population. Psicologia Reflexao E Critica, 31(1), 22. https://doi.org/10.1186/s41155-018-0102-3.
Gil-Rivas, V., Silver, R. C., Holman, E. A., McIntosh, D. N., & Poulin, M. (2007). Parental response and adolescent adjustment to the September 11, 2001 terrorist attacks. Journal of Traumatic Stress, 20(6), 1063–1068. https://doi.org/10.1002/jts.20277.
Hijazi, A. M., Ferguson, C. J., Ferraro, R., Hall, F., Hovee, H., M., & Wilcox, S. L. (2019). Psychological dimensions of drone warfare. Current Psychology, 38(5), 1285–1296. https://doi.org/10.1007/s12144-017-9684-7.
Jiang, H., Jin, L., Qian, X., Xiong, X., La, X., Chen, W., Yang, X., Yang, F., Zhang, X., Abudukelimu, N., Li, X., Xie, Z., Zhu, X., Zhang, X., Zhang, L., Wang, L., Li, L., & Li, M. (2021). Maternal mental health status and approaches for accessing antenatal care information during the COVID-19 epidemic in China: Cross-sectional study. Journal of Medical Internet Research, 23(1), e18722. https://doi.org/10.2196/18722.
Kandemir, H., Karataş, H., Çeri, V., Solmaz, F., Kandemir, S. B., & Solmaz, A. (2018). Prevalence of war-related adverse events, depression and anxiety among Syrian refugee children settled in Turkey. European Child & Adolescent Psychiatry, 27(11), 1513–1517. https://doi.org/10.1007/s00787-018-1178-0.
Karam, E. G., Fayyad, J., Karam, A. N., Melhem, N., Mneimneh, Z., Dimassi, H., & Tabet, C. C. (2014). Outcome of depression and anxiety after war: A prospective epidemiologic study of children and adolescents. Journal of Traumatic Stress, 27(2), 192–199. https://doi.org/10.1002/jts.21895.
Kilmer, R. P., & Gil-Rivas, V. (2010). Exploring posttraumatic growth in children impacted by Hurricane Katrina: Correlates of the phenomenon and developmental considerations. Child Development, 81(4), 1211–1227. https://doi.org/10.1111/j.1467-8624.2010.01463.x.
Kuehn, P. D. (2013). Cultural coping strategies and their connection to grief therapy modalities for children: An investigation into current knowledge and practice [Master’s thesis, University of St. Thomas, Minnesota]. https://ir.stthomas.edu/cgi/viewcontent.cgi?article=1213&context=ssw_mstrp
Kuo, B. C. (2013). Collectivism and coping: Current theories, evidence, and measurements of collective coping. International Journal of Psychology, 48(3), 374–388. https://doi.org/10.1080/00207594.2011.640681.
Llabre, M. M., Hadi, F., La Greca, A. M., & Lai, B. S. (2015). Psychological distress in young adults exposed to war-related trauma in childhood. Journal of Clinical Child & Adolescent Psychology, 44(1), 169–180. https://doi.org/10.1080/15374416.2013.828295.
Martsenkovskyi, D., Napryeyenko, O., & Martsenkovsky, I. (2020). Depression in adolescents exposed to war trauma risk factors for development of depression in adolescents exposed to war trauma: Does PTSD matter? Global Psychiatry Archives, 3(2), 227–240. https://doi.org/10.52095/gpa.2020.1379.
Novita, S., Uyun, Q., Witruk, E., & Siregar, J. R. (2019). Children with dyslexia in different cultures: Investigation of anxiety and coping strategies of children with dyslexia in Indonesia and Germany. Annals of Dyslexia, 69(2), 204–218. https://doi.org/10.1007/s11881-019-00179-5.
Novo Navarro, P., Landin-Romero, R., Guardiola-Wanden-Berghe, R., Moreno-Alcázar, A., Valiente-Gómez, A., Lupo, W., García, F., Fernández, I., Pérez, V., & Amann, B. L. (2018). The EMDR therapy protocol, hypotheses of its mechanism of action and a systematic review of its efficacy in the treatment of post-traumatic stress disorder. Revista de Psiquiatría y Salud Mental (English Edition), 11(2), 101–114. https://doi.org/10.1016/j.rpsm.2015.12.002. 25 years of Eye Movement Desensitization and Reprocessing (EMDR).
Ollendick, T. H., Langley, A. K., Jones, R. T., & Kephart, C. (2001). Fear in children and adolescents: Relations with negative life events, attributional style, and avoidant coping. The Journal of Child Psychology and Psychiatry and Allied Disciplines, 42(8), 1029–1034. https://pubmed.ncbi.nlm.nih.gov/11806684/.
Osokina, O., Silwal, S., Bohdanova, T., Hodes, M., Sourander, A., & Skokauskas, N. (2023). Impact of the Russian invasion on mental health of adolescents in Ukraine. Journal of the American Academy of Child & Adolescent Psychiatry, 62(3), 335–343. https://doi.org/10.1016/j.jaac.2022.07.845.
Perkins, J. D., Ajeeb, M., Fadel, L., & Saleh, G. (2018). Mental health in Syrian children with a focus on post-traumatic stress: A cross-sectional study from Syrian schools. Social Psychiatry and Psychiatric Epidemiology, 53(11), 1231–1239. https://doi.org/10.1007/s00127-018-1573-3.
Pfefferbaum, B. (1997). Posttraumatic stress disorder in children: A review of the past 10 years. Journal of the American Academy of Child & Adolescent Psychiatry, 36(11), 1503–1511. https://doi.org/10.1016/S0890-8567(09)66558-8.
Pfefferbaum, B., Noffsinger, M. A., Wind, L. H., & Allen, J. R. (2014). Children’s coping in the context of disasters and terrorism. Journal of Loss and Trauma, ‘9(1), 78–97. https://doi.org/10.1080/15325024.2013.791797.
Pina, A. A., Villalta, I. K., Ortiz, C. D., Gottschall, A. C., Costa, N. M., & Weems, C. F. (2008). Social support, discrimination, and coping as predictors of posttraumatic stress reactions in youth survivors of Hurricane Katrina. Journal of Clinical Child & Adolescent Psychology, 37(3), 564–574. https://doi.org/10.1080/15374410802148228.
Powell, T., Wegmann, K. M., & Backode, E. (2021). Coping and post-traumatic stress in children and adolescents after an acute onset disaster: A systematic review. International Journal of Environmental Research and Public Health, 18(9), 4865. https://doi.org/10.3390/ijerph18094865.
Ressler, K. J., Berretta, S., Bolshakov, V. Y., Rosso, I. M., Meloni, E. G., Rauch, S. L., & Carlezon, W. A. Jr. (2022). Post-traumatic stress disorder: Clinical and translational neuroscience from cells to circuits. Nature Reviews Neurology, 18(5), 273–288. https://doi.org/10.1038/s41582-022-00635-8.
Saudi Gazette (2021, June 14). US leads global condemnation of Houthi drone attack on Asir school. Saudi Gazette. https://saudigazette.com.sa/article/607772.
Silwal, S., Chudal, R., Dybdahl, R., Sillanmäki, L., Lien, L., & Sourander, A. (2021). Post-traumatic stress and depressive symptoms among adolescents after the 2015 earthquake in Nepal: A longitudinal study. Child Psychiatry & Human Development, 1–10. https://doi.org/10.1007/s10578-021-01136-3.
Solberg, Ø., Nissen, A., Vaez, M., Cauley, P., Eriksson, A. K., & Saboonchi, F. (2020). Children at risk: A nation-wide, cross-sectional study examining post-traumatic stress symptoms in refugee minors from Syria, Iraq and Afghanistan resettled in Sweden between 2014 and 2018. Conflict and Health, 14(1), 1–12. https://doi.org/10.1186/s13031-020-00311-y.
Son, C., Hegde, S., Smith, A., Wang, X., & Sasangohar, F. (2020). Effects of COVID-19 on college students’ mental health in the United States: Interview survey study. Journal of Medical Internet Research, 22(9), e21279. https://doi.org/10.2196/21279.
Stormacq, C., Van den Broucke, S., & Wosinski, J. (2019). Does health literacy mediate the relationship between socioeconomic status and health disparities? Integrative review. Health Promotion International, 34(5), e1–e17. https://doi.org/10.1093/heapro/day062.
Thabet, A. A. M., Abed, Y., & Vostanis, P. (2004). Comorbidity of PTSD and depression among refugee children during war conflict. Journal of Child Psychology and Psychiatry, 45(3), 533–542. https://doi.org/10.1111/j.1469-7610.2004.00243.x.
Thabet, A. A., Tawahina, A. A., El Sarraj, E., & Vostanis, P. (2008). Exposure to war trauma and PTSD among parents and children in the Gaza strip. European Child & Adolescent Psychiatry, 17(4), 191–199. https://doi.org/10.1007/s00787-007-0653-9.
Thabet, A. A., Ibraheem, A. N., Shivram, R., Winter, E. A., & Vostanis, P. (2009). Parenting support and PTSD in children of a war zone. International Journal of Social Psychiatry, 55(3), 226–237. https://doi.org/10.1177/0020764008096100.
Thomassen, Å. G., Hystad, S. W., Johnsen, B. H., Johnsen, G. E., & Bartone, P. T. (2018). The effect of hardiness on PTSD symptoms: A prospective mediational approach. Military Psychology, 30(2), 142–151. https://doi.org/10.1080/08995605.2018.1425065.
Vus, V., Shipley, K., & Lühmann, T. (2023). Mapping and identifying barriers and facilitators to mental health and psychosocial support interventions for war-affected children. Polski Merkuriusz Lekarski, 51(1), 64–73. https://doi.org/10.36740/Merkur202301110.
Walters, W. (2014). Drone strikes, dingpolitik and beyond: Furthering the debate on materiality and security. Security Dialogue, 45(2), 101–118. https://doi.org/10.1177/0967010613519162.
Xu, Y., Farver, J. M., Chang, L., Yu, L., & Zhang, Z. (2006). Culture, family contexts, and children’s coping strategies in peer interactions. In X. Chen, D. French, & B. Schneider (Eds.), Peer relationships in cultural context (pp. 264–280). Cambridge University Press. https://doi.org/10.1017/CBO9780511499739.012.
Yayan, E. H., Düken, M. E., Özdemir, A. A., & Çelebioğlu, A. (2020). Mental health problems of Syrian refugee children: Post-traumatic stress, depression and anxiety. Journal of Pediatric Nursing, 51, e27–e32. https://doi.org/10.1016/j.pedn.2019.06.012.
Yeh, C. J., Arora, A. K., & Wu, K. A. (2006). A new theoretical model of collectivistic coping. In P. T. P. Wong & L. C. J. Wong (Eds.), Handbook of multicultural perspectives on stress and coping (pp. 55–72). Springer. https://doi.org/10.1007/0-387-26238-5_3.
Acknowledgements
The authors thank all participants and parents for their interest and willingness to contribute to the study. We extend our heartfelt appreciation to all the teachers and school professionals who helped us recruit participants. Finally, we are delighted to acknowledge the invaluable contribution of the Saudi National Center for Mental Health Promotion in funding this project.
Funding
This research was funded by the National Center for Mental Health Promotion, Saudi Arabia (https://ncmh.org.sa).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics, Approval, and Consent to Participate
The Research Ethics Committee at Imam Mohammad Ibn Saud Islamic University (Approval Number: 312/2022). Verbal informed consent was obtained from all participants prior to the interviews.
Competing Interests
The authors declare that they have no competing conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alqahtani, M.M.J., Al-Loghbi, A.S., AlSalehi, S.M. et al. Coping Mechanisms and Posttraumatic Stress Exhibited by Children in Areas of Yemen’s Armed Conflict in Southern Saudi Arabia. Journ Child Adol Trauma (2024). https://doi.org/10.1007/s40653-024-00630-9
Accepted:
Published:
DOI: https://doi.org/10.1007/s40653-024-00630-9