Abstract
Introduction
Animal experiments have shown that anti-GBM antibodies play a pathogenic role in anti-GBM disease. However, the relationship between anti-GBM antibody levels and kidney outcomes in patients with anti-GBM disease is unclear.
Methods
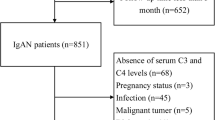
We performed a retrospective analysis of 110 patients diagnosed with anti-GBM disease. We compared their baseline characteristics stratifying on different anti-GBM antibody levels, and used Cox regression analysis to analyze the correlation between antibody levels and kidney survival. We further selected 69 patients to evaluate the modification of antibody titers over 14 days of treatment, then compared kidney survival of patients in the group with antibody level decrease < 48% to those with antibody decrease ≥ 48%.
Results
The 110 patients had a median follow-up of 27.1 (Q1–Q3: 7.9–80.1) months, and among them 90 (81.8%) developed kidney failure. Multivariate analysis suggested that anti-GBM antibody level was an independent risk factor for progression to kidney failure in patients with anti-GBM disease (HR 1.08, 95% CI 1.01–1.16). The patients who reduced the antibodies levels quickly had better kidney survival than those who did not, and multivariate analysis also indicated that antibody decrease rate was related to kidney outcomes.
Conclusions
Anti-GBM antibody level is closely related to kidney outcomes in patients with anti-GBM disease, and short-term reduction of antibodies can be beneficial to improving kidney outcomes.
Graphical abstract




Similar content being viewed by others
Availability of data and material
The datasets collected and analyzed in the current study are available from the corresponding author on reasonable request.
References
Lerner RA, Glassock RJ, Dixon FJ (1967) The role of anti-glomerular basement membrane antibody in the pathogenesis of human glomerulonephritis. J Exp Med 126(6):989–1004. https://doi.org/10.1084/jem.126.6.989
Saus J, Wieslander J, Langeveld JP, Quinones S, Hudson BG (1988) Identification of the Goodpasture antigen as the alpha 3(IV) chain of collagen IV. J Biol Chem 263(26):13374–13380
Turner N, Mason PJ, Brown R, Fox M, Povey S, Rees A, Pusey CD (1992) Molecular cloning of the human Goodpasture antigen demonstrates it to be the alpha 3 chain of type IV collagen. J Clin Invest 89(2):592–601. https://doi.org/10.1172/JCI115625
Hellmark T, Burkhardt H, Wieslander J (1999) Goodpasture disease. Characterization of a single conformational epitope as the target of pathogenic autoantibodies. J Biol Chem 274(36):25862–25868. https://doi.org/10.1074/jbc.274.36.25862
Lockwood CM, Rees AJ, Pearson TA, Evans DJ, Peters DK, Wilson CB (1976) Immunosuppression and plasma-exchange in the treatment of Goodpasture’s syndrome. Lancet 1(7962):711–715. https://doi.org/10.1016/s0140-6736(76)93089-0
Peters DK, Rees AJ, Lockwood CM, Pusey CD (1982) Treatment and prognosis in antibasement membrane antibody-mediated nephritis. Transplant Proc 14(3):513–521
Lockwood CM, Boulton-Jones JM, Lowenthal RM, Simpson IJ, Peters DK (1975) Recovery from Goodpasture’s syndrome after immunosuppressive treatment and plasmapheresis. Br Med J 2(5965):252–254. https://doi.org/10.1136/bmj.2.5965.252
Cui Z, Zhao J, Jia XY, Zhu SN, Jin QZ, Cheng XY, Zhao MH (2011) Anti-glomerular basement membrane disease: outcomes of different therapeutic regimens in a large single-center Chinese cohort study. Medicine (Baltimore) 90(5):303–311. https://doi.org/10.1097/MD.0b013e31822f6f68
Huart A, Josse AG, Chauveau D, Korach JM, Heshmati F, Bauvin E, Cointault O, Kamar N, Ribes D, Pourrat J, Faguer S (2016) Outcomes of patients with Goodpasture syndrome: a nationwide cohort-based study from the French Society of Hemapheresis. J Autoimmun 73:24–29. https://doi.org/10.1016/j.jaut.2016.05.015
Cui Z, Wang HY, Zhao MH (2006) Natural autoantibodies against glomerular basement membrane exist in normal human sera. Kidney Int 69(5):894–899. https://doi.org/10.1038/sj.ki.5000135
Yang R, Cui Z, Hellmark T, Segelmark M, Zhao MH, Wang HY (2007) Natural anti-GBM antibodies from normal human sera recognize alpha3(IV)NC1 restrictively and recognize the same epitopes as anti-GBM antibodies from patients with anti-GBM disease. Clin Immunol 124(2):207–212. https://doi.org/10.1016/j.clim.2007.05.001
Shoenfeld Y (2004) The idiotypic network in autoimmunity: antibodies that bind antibodies that bind antibodies. Nat Med 10(1):17–18. https://doi.org/10.1038/nm0104-17
Pendergraft WF 3rd, Preston GA, Shah RR, Tropsha A, Carter CW Jr, Jennette JC, Falk RJ (2004) Autoimmunity is triggered by cPR-3(105–201), a protein complementary to human autoantigen proteinase-3. Nat Med 10(1):72–79. https://doi.org/10.1038/nm968
Gilles JG, Saint-Remy JM (1994) Healthy subjects produce both anti-factor VIII and specific anti-idiotypic antibodies. J Clin Invest 94(4):1496–1505. https://doi.org/10.1172/JCI117489
Levy JB, Lachmann RH, Pusey CD (1996) Recurrent Goodpasture’s disease. Am J Kidney Dis 27(4):573–578. https://doi.org/10.1016/s0272-6386(96)90169-9
Levy JB, Turner AN, Rees AJ, Pusey CD (2001) Long-term outcome of anti-glomerular basement membrane antibody disease treated with plasma exchange and immunosuppression. Ann Intern Med 134(11):1033–1042. https://doi.org/10.7326/0003-4819-134-11-200106050-00009
Simpson IJ, Doak PB, Williams LC, Blacklock HA, Hill RS, Teague CA, Herdson PB, Wilson CB (1982) Plasma exchange in Goodpasture’s syndrome. Am J Nephrol 2(6):301–311. https://doi.org/10.1159/000166666
Segelmark M, Hellmark T, Wieslander J (2003) The prognostic significance in Goodpasture’s disease of specificity, titre and affinity of anti-glomerular-basement-membrane antibodies. Nephron Clin Pract 94(3):c59-68. https://doi.org/10.1159/000072022
Cui Z, Zhao MH (2005) Avidity of anti-glomerular basement membrane autoantibodies was associated with disease severity. Clin Immunol 116(1):77–82. https://doi.org/10.1016/j.clim.2005.02.016
Savage CO, Pusey CD, Bowman C, Rees AJ, Lockwood CM (1986) Antiglomerular basement membrane antibody mediated disease in the British Isles 1980–4. Br Med J (Clin Res Ed) 292(6516):301–304. https://doi.org/10.1136/bmj.292.6516.301
Fischer EG, Lager DJ (2006) Anti-glomerular basement membrane glomerulonephritis: a morphologic study of 80 cases. Am J Clin Pathol 125(3):445–450. https://doi.org/10.1309/nptp-4ukv-7ju3-elmq
Zahir Z, Wani AS, Prasad N, Jain M (2021) Clinicopathological characteristics and predictors of poor outcome in anti-glomerular basement membrane disease—a fifteen year single center experience. Ren Fail 43(1):79–89. https://doi.org/10.1080/0886022X.2020.1854301
van Daalen EE, Jennette JC, McAdoo SP, Pusey CD, Alba MA, Poulton CJ, Wolterbeek R, Nguyen TQ, Goldschmeding R, Alchi B, Griffiths M, de Zoysa JR, Vincent B, Bruijn JA, Bajema IM (2018) Predicting outcome in patients with anti-GBM glomerulonephritis. Clin J Am Soc Nephrol 13(1):63–72. https://doi.org/10.2215/CJN.04290417
Funding
This work was supported by the National Key Research and Development Project of China (Grant number 2021YFC2501302).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare no competing interests.
Ethical statement
This study was approved by the ethics committee of Jinling Hospital (2022DZKY-033-01), and was carried out following the principles of the Helsinki Declaration.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhu, M., Wang, J., Le, W. et al. Relationship between anti-GBM antibodies and kidney outcomes in patients with anti-GBM disease. J Nephrol 36, 789–797 (2023). https://doi.org/10.1007/s40620-022-01508-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-022-01508-5