Abstract
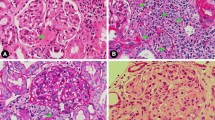
De novo systemic atypical hemolytic uremic syndrome (aHUS) post-kidney transplant is an uncommon entity associated with unfavorable outcome. We herein report a case of systemic and fulminant de novo aHUS accompanied by heart and respiratory failure in a 48-year-old male receiving ABO-incompatible living-related kidney transplant who was successfully treated with the anti-C5 monoclonal antibody eculizumab with complete recovery of allograft function. Genetic testing demonstrated a novel pathogenic heterozygous complement factor H-related 1 gene mutation in both the donor and the recipient. Our study highlights the high risks of post-transplant aHUS due to the complement gene mutations in both donor and recipient in living-related transplantation. Early intervention with eculizumab may be effective for reversing systemic aHUS in kidney transplant recipients.

Similar content being viewed by others
References
Garg N, Rennke HG, Pavlakis M, Zandi-Nejad K (2018) De novo thrombotic microangiopathy after kidney transplantation. Transplant Rev (Orlando) 32(1):58–68
Bu F, Maga T, Meyer NC, Wang K, Thomas CP, Nester CM, Smith RJ (2014) Comprehensive genetic analysis of complement and coagulation genes in atypical hemolytic uremic syndrome. J Am Soc Nephrol 25(1):55–64
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, Grody WW, Hegde M, Lyon E, Spector E, Voelkerding K, Rehm HL; ACMG Laboratory Quality Assurance Committee (2015) Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med 17(5):405–424
Heinen S, Hartmann A, Lauer N, Wiehl U, Dahse HM, Schirmer S, Gropp K, Enghardt T, Wallich R, Hälbich S, Mihlan M, Schlötzer-Schrehardt U, Zipfel PF, Skerka C (2009) Factor H-related protein 1 (CFHR-1) inhibits complement C5 convertase activity and terminal complex formation. Blood 114(12):2439–2447
Bhattacharjee A, Reuter S, Trojnár E, Kolodziejczyk R, Seeberger H, Hyvärinen S, Uzonyi B, Szilágyi Á, Prohászka Z, Goldman A, Józsi M, Jokiranta TS (2015) The major autoantibody epitope on factor H in atypical hemolytic uremic syndrome is structurally different from its homologous site in factor H-related protein 1, supporting a novel model for induction of autoimmunity in this disease. J Biol Chem 290(15):9500–9510
Piras R, Iatropoulos P, Bresin E, Todeschini M, Gastoldi S, Valoti E, Alberti M, Mele C, Galbusera M, Cuccarolo P, Benigni A, Remuzzi G, Noris M (2020) Molecular studies and an ex vivo complement assay on endothelium highlight the genetic complexity of atypical hemolytic uremic syndrome: the case of a pedigree with a null CD46 variant. Front Med (Lausanne) 7:579418
Kobbe R, Schild R, Christner M, Oh J, Loos S, Kemper MJ (2017) Case report—atypical hemolytic uremic syndrome triggered by influenza B. BMC Nephrol 18(1):96
Tasaki M, Saito K, Nakagawa Y, Imai N, Ito Y, Yoshida Y, Ikeda M, Ishikawa S, Narita I, Takahashi K, Tomita Y (2019) Analysis of the prevalence of systemic de novo thrombotic microangiopathy after ABO-incompatible kidney transplantation and the associated risk factors. Int J Urol 26(12):1128–1137
Fakhouri F, Hourmant M, Campistol JM, Cataland SR, Espinosa M, Gaber AO, Menne J, Minetti EE, Provôt F, Rondeau E, Ruggenenti P, Weekers LE, Ogawa M, Bedrosian CL, Legendre CM (2016) Terminal complement inhibitor eculizumab in adult patients with atypical hemolytic uremic syndrome: a single-arm. Open-Label Trial Am J Kidney Dis 68(1):84–93
Legendre CM, Licht C, Muus P, Greenbaum LA, Babu S, Bedrosian C, Bingham C, Cohen DJ, Delmas Y, Douglas K, Eitner F, Feldkamp T, Fouque D, Furman RR, Gaber O, Herthelius M, Hourmant M, Karpman D, Lebranchu Y, Mariat C, Menne J, Moulin B, Nürnberger J, Ogawa M, Remuzzi G, Richard T, Sberro-Soussan R, Severino B, Sheerin NS, Trivelli A, Zimmerhackl LB, Goodship T, Loirat C (2013) Terminal complement inhibitor eculizumab in atypical hemolytic-uremic syndrome. N Engl J Med 368(23):2169–2181
Greenbaum LA, Fila M, Ardissino G, Al-Akash SI, Evans J, Henning P, Lieberman KV, Maringhini S, Pape L, Rees L, van de Kar NC, Vande Walle J, Ogawa M, Bedrosian CL, Licht C (2016) Eculizumab is a safe and effective treatment in pediatric patients with atypical hemolytic uremic syndrome. Kidney Int 89(3):701–711
González CC, López-Jiménez V, Vázquez-Sánchez T, Vázquez-Sánchez E, Cabello M, Hernández-Marrero D (2022) Efficacy and safety of eculizumab in kidney transplant patients with primary atypical hemolytic-uremic syndrome. Transplant Proc 54(1):25–26
Schwartz J, Winters JL, Padmanabhan A, Balogun RA, Delaney M, Linenberger ML, Szczepiorkowski ZM, Williams ME, Wu Y, Shaz BH (2013) Guidelines on the use of therapeutic apheresis in clinical practice-evidence-based approach from the Writing Committee of the American Society for Apheresis: the sixth special issue. J Clin Apher 28(3):1
Funding
This work was supported by a grant from Special Supportive Program for Organ Transplantation by COTDF to Dawei Li (Grant no. 2019JYJH14), and National Natural Science Foundation of China to Jiqiu Wen (Grant no. 81570681) and Wei Wang (Grant no. 82000731).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interests
None declared.
Ethical statement
Written informed consent was obtained from the patient for the publication of this case report and accompanying images.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Li, D., Wang, W., Chen, R. et al. De novo systemic atypical hemolytic uremic syndrome in an ABO-incompatible living kidney transplant recipient with a novel pathogenic CFHR1 gene mutation successfully treated with eculizumab: a case report. J Nephrol 35, 1895–1899 (2022). https://doi.org/10.1007/s40620-022-01391-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-022-01391-0