Abstract
Objective
Serum albumin level is not only one of the protein-energy wasting criteria but also a powerful marker of mortality in patients on haemodialysis (HD) treatment. The study aimed to assess the effect of a protein-enriched snack given during HD treatment on serum albumin level.
Design and methods
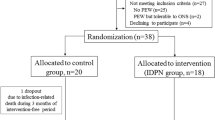
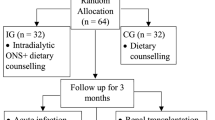
This prospective, single-centre, observational, non-randomized 16-month study was sub-divided into four 4-month periods. Patients on hemodialysis for more than three months and receiving a regular standard snack (8.8 g of protein) during the HD session were included and assigned during four four-month periods to receive either the standard snack or a protein-enriched snack (28.7 g). Patients were not selected based on nutritional criteria.
Results
Sixty-six patients completed the study. Serum albumin levels significantly increased, from 3.43 ± 0.28 g/dl in the first period (standard snack) to 3.62 ± 0.32 g/dl (p < 0.0001) in the second period (enriched snack). In the third period (standard snack), albumin levels remained stable (3.61 ± 0.35 g/dl). After the fourth period (enriched snack), serum albumin levels further increased significantly (3.69 ± 0.30 g/dl; p = 0.05 and p = 0.007, respectively). Weight and normalized protein nitrogen appearance remained stable during the 16-month study period.
Conclusions
This study suggests that the intake of a protein-enriched snack during HD treatment, independently from baseline serum albumin level, could significantly increase their serum albumin levels. Serum albumin level is a powerful predictor of mortality; therefore, this simple and effective action could be of real interest to improve patients’ outcomes.




Similar content being viewed by others
References
Kalantar-Zadeh K, Fouque D (2017) Nutritional management of chronic kidney disease. N Eng J Med 377:1765–1776
de Mutsert R, Grootendorst DC, Axelsson J, Boeschoten EW, Krediet RT, Dekker FW et al (2008) Excess mortality due to interaction between protein-energy wasting, inflammation and cardiovascular disease in chronic dialysis patients. Nephrol Dial Transpl 23:2957–2964
Pupim LB, Caglar K, Hakim RM, Shyr Y, Ikizler TA (2004) Uremic malnutrition is a predictor of death independent of inflammatory status. Kidney Int 66:2054–2060
Lacson E Jr, Wang W, Hakim RM, Teng M, Lazarus JM (2009) Associates of mortality and hospitalization in hemodialysis: potentially actionable laboratory variables and vascular access. Am J Kidney Dis 53:79–90
Rocco MV, Paranandi L, Burrowes JD, Cockram DB, Dwyer JT, Kusek JW et al (2002) Nutritional status in the HEMO Study cohort at baseline. Hemodial Am J Kidney Dis 39:245–256
Kistler BM, Benner D, De Burrowes JD, Campbell KL, Fouque D, Garibotto G et al (2018) Eating during hemodialysis traitement: a consensus statement from the international Society of Renal Nutrition and Metabolism. J Ren Nut 28(1):4–12
Rhee CM, You AS, Koontz Parsons T et al (2017) Effect of high-protein meals during hemodialysis combined with lanthanum carbonate in hypoalbuminemic dialysis patients: findings from the FrEDI randomized controlled trial. Nephrol Dial Transpl 32:1233–1243
Tomayko EJ, Kistler BM, Fitschene PJ, Wilmund KR (2015) Intradialytic protein supplementation reduces inflammation and improves physical function in maintenance hemodialysis patients. J Ren Nutr 25:276–283
Caetano C, Valente A, Silva FJ, Antunes J, Gargaraza C (2017) Effect of an intradialytic protein-rich meal intake in nutritional and body composition parameters on hemodialysis patients. Clin Nutr ESPEN 20:29–33
Vilay AM, Mueller BA (2013) Intradialytic oral nutritional supplements improve quality of life. Am J Kidney Dis 61:349
Ikizler TA, Pupim LB, Brouillette JR, Levenhagen DK, Farmer K, Hakim RM et al (2002) Hemodialysis stimulates muscle and whole-body protein loss and alters substrate oxidation. Am J Physiol Endocrinol Metab 282:E107–E116
Pupim LB, Majchrzak KM, Flakoll PJ, Ikizler TA (2006) Intradialytic oral nutrition improves protein homeostasis in chronic hemodialysis patients with deranged nutritional status. J Am Soc Nephrol 17:3149–3157
Pupim LB, Flakoll PJ, Brouillette JR, Levenhagen DK, Hakim RM, Ikizler TA (2002) Intradialytic parenteral nutrition improves protein and energy homeostasis in chronic hemodialysis patients. J Clin Invest 110:483–492
Pupim LB, Flakoll PJ, Levenhagen DK, Ikizler TA (2004) Exercise augments the acute anabolic effects of intradialytic parenteral nutrition in chronic hemodialysis patients. Am J Physiol Endocrinol Metab 286:E589–E597
Podsiadlo D, Richardson S (1991) The timed “Up & Go”: a test of basic functional mobility for frail elderly persons. J Am Geriatr Soc 39:142–148
Kalantar-Zadeh K, Block G, McAllister CJ, Humphreys MH, Kopple JD (2004) Appetite and inflammation, nutrition, anemia, and clinical outcome in hemodialysis patients. AM J Clin Nutr 80:299–307
Li J, Hou G, Sun X, Chen A, Chai Y (2020) A low-cost intradialytic, protein-rich meal improves the nutritional status in Chinese hemodialysis patients. J Ren Nutr 30(2):27–34
Sezer S, Bal Z, Tutal E, Uyar ME, Acar NO (2014) Long-term oral nutrition supplementation improves outcomes in malnourished patients with chronic kidney disease on hemodialysis. JPEN J Parenter Enteral Nutr 38:960–965
Malgorzewicz S, Rutkowski P, Jankowska M, Debska-Slizien A, Rutkowski B, Lysiak-Szydlowska W (2011) Effects of renal-specific oral supplementation in malnourished hemodialysis patients. J Ren Nutr 21:347–353
Sabatino Sabatino A, Regolisti G, Karupaiah T et al (2017) Protein-energy wasting and nutritional supplementation in patients with end-stage renal disease on hemodialysis. Clin Nutr 36(3):663–671
Kalantar-Zadeh K, Kilpatrick RD, Kuwae N, McAllister CJ, Alcorn H Jr, Kopple JD et al (2005) Revisiting mortality predictability of serum albumin in the dialysis population: time dependency, longitudinal changes and population-attributable fraction. Nephrol Dial Transpl 20:1880–1888
Cano NJ, Fouque D, Roth H, Aparicio M, Azar R, Canaud B et al (2007) Intradialytic parenteral nutrition does not improve survival in malnourished hemodialysis patients: a 2-year multicenter, prospective, randomized study. J Am Soc Nephrol 18:2583–2591
Lacson E Jr, Wang W, Zebrowski B, Wingard R, Hakim RM (2012) Outcomes associated with intradialytic oral nutritional supplements in patients undergoing maintenance hemodialysis: a quality improvement report. Am J Kidney Dis 60:591–600
Weiner DE, Tighiouart H, Ladik V, Meyer KB, Zager PG, Johnson DS (2014) Oral intradialytic nutritional supplement use and mortality in hemodialysis patients. Am J Kidney Dis 63:276–285
Cheu C, Pearson J, Dahlerus C, Lantz B, Chowdhury T, Sauer PF et al (2013) Association between oral nutritional supplementation and clinical outcomes among patients with ESRD. Clin J Am Soc Nephrol 8:100–107
Sundell MB, Cavanaugh KL, Wu P, Shintani A, Hakim RM, Ikizler TA (2009) Oral protein supplementation alone improves anabolism in a dose-dependent manner in chronic hemodialysis patients. J Ren Nutr 19:412–421
Marini ACB, Pimentel GD (2019) Is body weight or muscle strength correlated with the Malnutrition Inflammation Score (MIS)? A cross-sectional study in hemodialysis patients. Clin Nutr ESPEN 33:276–278
Chang TI, Ngo V, Streja E, Chou JA, Tortorici AR, Kim TH et al (2017) Association of body weight changes with mortality in incident hemodialysis patients. Nephrol Dial Transpl 32(9):1549–1558
Kalantar-Zadeh K, Kopple JD, Kilpatrick RD, McAllister CJ, Shinaberger CS, Gjertson DW et al (2005) Association of morbid obesity and weight change over time with cardiovascular survival in hemodialysis population. Am J Kidney Dis 46:489–500
Acknowledgements
To Cecile Bonhomme and Lactalis group for their conceptual and material contribution to this study.
Author information
Authors and Affiliations
Contributions
DP: Conception and design; data analysis and interpretation; provision of study patients; manuscript writing; final approval of manuscript. JG: Conception and design; data analysis and interpretation; provision of study patients; manuscript writing; final approval of manuscript. BA-L: Conception and design; data analysis and interpretation; final approval of manuscript. LC: Conception and design; provision of study patients; final approval of manuscript. HJ-M: Conception and design; provision of study patients; final approval of manuscript. MB: Conception and design; provision of study patients; final approval of manuscript. MM: Conception and design; provision of study patients; final approval of manuscript. CC: Conception and design; data analysis and interpretation; provision of study patients; manuscript writing; final approval of manuscript. All authors read and approved the final manuscript.
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Deleaval, P., Guillaume, J., Bernollin, AL. et al. The effect of protein-enriched snacks on serum albumin concentration in non-selected haemodialysis patients. J Nephrol 34, 1291–1299 (2021). https://doi.org/10.1007/s40620-020-00887-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40620-020-00887-x