Abstract
Purpose
Air pollution is an environmental stimulus that may predispose pregnant women to gestational diabetes mellitus (GDM). This systematic review and meta-analysis were conducted to investigate the relationship between air pollutants and GDM.
Methods
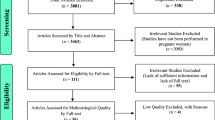
PubMed, Web of Science, and Scopus were systematically searched for retrieving English articles published from January 2020 to September 2021, investigating the relationship of exposure to ambient air pollution or levels of air pollutants with GDM and related parameters, including fasting plasma glucose (FPG), insulin resistance, and impaired glucose tolerance. Heterogeneity and publication bias were evaluated using I-squared (I2), and Begg’s statistics, respectively. We also performed the subgroup analysis for particulate matters (PM2.5, PM10), Ozone (O3), and sulfur dioxide (SO2) in the different exposure periods.
Results
A total of 13 studies examining 2,826,544 patients were included in this meta-analysis. Compared to non-exposed women, exposure to PM2.5 increases the odds (likelihood of occurrence outcome) of GDM by 1.09 times (95% CI 1.06, 1.12), whereas exposure to PM10 has more effect by OR of 1.17 (95% CI 1.04, 1.32). Exposure to O3 and SO2 increases the odds of GDM by 1.10 times (95% CI 1.03, 1.18) and 1.10 times (95% CI 1.01, 1.19), respectively.
Conclusions
The results of the study show a relationship between air pollutants PM2.5, PM10, O3, and SO2 and the risk of GDM. Although evidence from various studies can provide insights into the linkage between maternal exposure to air pollution and GDM, more well-designed longitudinal studies are recommended for precise interpretation of the association between GDM and air pollution by adjusting all potential confounders.
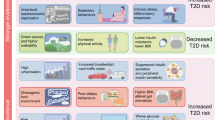
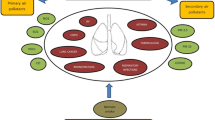
Graphical abstract







Similar content being viewed by others
Data availability
All data relevant to the study are included in the article or uploaded as supplementary information.
References
Buchanan TA, Xiang AH, Page KA (2012) Gestational diabetes mellitus: risks and management during and after pregnancy. Nat Rev Endocrinol 8(11):639–649
Association AD (2003) Gestational diabetes mellitus. Diabetes care 26:S103–S105
Gadgil MD, Oza-Frank R, Kandula NR, Kanaya AM (2017) Type 2 diabetes after gestational diabetes mellitus in south Asian women in the United States. Diabetes Metab Res Rev 33(5):e2891
McIntyre HD, Catalano P, Zhang C, Desoye G, Mathiesen ER, Damm P (2019) Gestational diabetes mellitus. Nat Rev Dis Primers 5(1):1–19
Hu Q, Wang D, Yue D, Xu C, Hu B, Cheng P et al (2021) Association of ambient particle pollution with gestational diabetes mellitus and fasting blood glucose levels in pregnant women from two Chinese birth cohorts. Sci Total Environ 762:143176
Chodick G, Tenne Y, Barer Y, Shalev V, Elchalal U (2020) Gestational diabetes and long-term risk for dyslipidemia: a population-based historical cohort study. BMJ Open Diabetes Res Care 8(1):e000870
Bellamy L, Casas J-P, Hingorani AD, Williams D (2009) Type 2 diabetes mellitus after gestational diabetes: a systematic review and meta-analysis. Lancet 373(9677):1773–1779
Fraser A, Almqvist C, Larsson H, Långström N, Lawlor DA (2014) Maternal diabetes in pregnancy and offspring cognitive ability: sibling study with 723,775 men from 579,857 families. Diabetologia 57(1):102–109
Zhang C, Rawal S, Chong YS (2016) Risk factors for gestational diabetes: is prevention possible? Diabetologia 59(7):1385–1390
Chiefari E, Arcidiacono B, Foti D, Brunetti A (2017) Gestational diabetes mellitus: an updated overview. J Endocrinol Invest 40(9):899–909
Hu C-Y, Gao X, Fang Y, Jiang W, Huang K, Hua X-G et al (2020) Human epidemiological evidence about the association between air pollution exposure and gestational diabetes mellitus: systematic review and meta-analysis. Environ Res 180:108843
Zhang H, Wang Q, He S, Wu K, Ren M, Dong H et al (2020) Ambient air pollution and gestational diabetes mellitus: a review of evidence from biological mechanisms to population epidemiology. Sci Total Environ 719:137349
Hu H, Ha S, Henderson BH, Warner TD, Roth J, Kan H et al (2015) Association of atmospheric particulate matter and ozone with gestational diabetes mellitus. Environ Health Perspect 123(9):853–859
Rammah A, Whitworth KW, Symanski E (2020) Particle air pollution and gestational diabetes mellitus in Houston. Texas Environ Res 190:109988
Jo H, Eckel SP, Chen J-C, Cockburn M, Martinez MP, Chow T et al (2019) Associations of gestational diabetes mellitus with residential air pollution exposure in a large Southern California pregnancy cohort. Environ Int 130:104933
Robledo CA, Mendola P, Yeung E, Männistö T, Sundaram R, Liu D et al (2015) Preconception and early pregnancy air pollution exposures and risk of gestational diabetes mellitus. Environ Res 137:316–322
Malmqvist E, Jakobsson K, Tinnerberg H, Rignell-Hydbom A, Rylander L (2013) Gestational diabetes and preeclampsia in association with air pollution at levels below current air quality guidelines. Environ Health Perspect 121(4):488–493
Pedersen M, Olsen SF, Halldorsson TI, Zhang C, Hjortebjerg D, Ketzel M et al (2017) Gestational diabetes mellitus and exposure to ambient air pollution and road traffic noise: a cohort study. Environ Int 108:253–260
Yao M, Liu Y, Jin D, Yin W, Ma S, Tao R et al (2020) Relationship betweentemporal distribution of air pollution exposure and glucose homeostasis during pregnancy. Environ Res 185:109456
Zhang H, Dong H, Ren M, Liang Q, Shen X, Wang Q et al (2020) Ambient air pollution exposure and gestational diabetes mellitus in Guangzhou, China: a prospective cohort study. Sci Total Environ 699:134390
Bai W, Li Y, Niu Y, Ding Y, Yu X, Zhu B et al (2020) Association between ambient air pollution and pregnancy complications: a systematic review and meta-analysis of cohort studies. Environ Res 185:109471
Tang X, Zhou J-B, Luo F, Han Y, Heianza Y, Cardoso MA et al (2020) Air pollution and gestational diabetes mellitus: evidence from cohort studies. BMJ Open Diabetes Res Care 8(1):e000937
Elshahidi MH (2019) Outdoor air pollution and gestational diabetes mellitus: a systematic review and meta-analysis. Iran J Public Health 48(1):9
Moher D, Liberati A, Tetzlaff J, Altman DG, Group P (2009) Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. PLoS Med 6(7):e1000097
Stroup DF, Berlin JA, Morton SC, Olkin I, Williamson GD, Rennie D et al (2000) Meta-analysis of observational studies in epidemiology: a proposal for reporting. JAMA 283(15):2008–2012
Stang A (2010) Critical evaluation of the Newcastle-Ottawa scale for the assessment of the quality of nonrandomized studies in meta-analyses. Eur J Epidemiol 25(9):603–605
Ye B, Zhong C, Li Q, Xu S, Zhang Y, Zhang X et al (2020) The associations of ambient fine particulate matter exposure during pregnancy with blood glucose levels and gestational diabetes mellitus risk: a prospective cohort study in Wuhan. Chin Am J Epidemiol 189(11):1306–1315
Yu G, Ao J, Cai J, Luo Z, Martin R, van Donkelaar A et al (2020) Fine particular matter and its constituents in air pollution and gestational diabetes mellitus. Environ Int 142:105880
Hehua Z, Yang X, Qing C, Shanyan G, Yuhong Z (2021) Dietary patterns and associations between air pollution and gestational diabetes mellitus. Environ Int 147:106347
Zheng Y, Wen X, Bian J, Lipkind H, Hu H (2021) Associations between the chemical composition of PM2.5 and gestational diabetes mellitus. Environ Res 198:110470
Zhang H, Zhao Y (2021) Ambient air pollution exposure during pregnancy and gestational diabetes mellitus in Shenyang, China: a prospective cohort study. Environ Sci Pollut Res 28(7):7806–7814
Melody SM, Wills K, Knibbs LD, Ford J, Venn A, Johnston F (2020) Maternal exposure to ambient air pollution and pregnancy complications in Victoria, Australia. Int J Environ Res Public Health 17(7):2572
Kang J, Liao J, Xu S, Xia W, Li Y, Chen S et al (2020) Associations of exposure to fine particulate matter during pregnancy with maternal blood glucose levels and gestational diabetes mellitus: potential effect modification by ABO blood group. Ecotoxicol Environ Saf 198:110673
Zhang M, Wang X, Yang X, Dong T, Hu W, Guan Q et al (2020) Increased risk of gestational diabetes mellitus in women with higher prepregnancy ambient PM2.5 exposure. Sci Total Environ 730:138982
Lin Q, Zhang S, Liang Y, Wang C, Wang C, Wu X et al (2020) Ambient air pollution exposure associated with glucose homeostasis during pregnancy and gestational diabetes mellitus. Environ Res 190:109990
Rajagopalan S, Brook RD (2012) Air pollution and type 2 diabetes: mechanistic insights. Diabetes 61(12):3037–3045
Plows JF, Stanley JL, Baker PN, Reynolds CM, Vickers MH (2018) The pathophysiology of gestational diabetes mellitus. Int J Mol Sci 19(11):3342
Wang B, Xu D, Jing Z, Liu D, Yan S, Wang Y (2014) Effect of long-term exposure to air pollution on type 2 diabetes mellitus risk: a systemic review and meta-analysis of cohort studies. Eur J Endocrinol 171(5):R173–R182
Thiering E, Cyrys J, Kratzsch J, Meisinger C, Hoffmann B, Berdel D et al (2013) Long-term exposure to traffic-related air pollution and insulin resistance in children: results from the GINIplus and LISAplus birth cohorts. Diabetologia 56(8):1696–1704
Liu C, Xu X, Bai Y, Wang T-Y, Rao X, Wang A et al (2014) Air pollution–mediated susceptibility to inflammation and insulin resistance: influence of CCR2 pathways in mice. Environ Health Perspect 122(1):17–26
Achilleos S, Kioumourtzoglou M-A, Wu C-D, Schwartz JD, Koutrakis P, Papatheodorou SI (2017) Acute effects of fine particulate matter constituents on mortality: a systematic review and meta-regression analysis. Environ Int 109:89–100
Calderon-Garciduenas L, Villarreal-Calderon R, Valencia-Salazar G, Henriquez-Roldan C, Gutiérrez-Castrellón P, Torres-Jardon R et al (2008) Systemic inflammation, endothelial dysfunction, and activation in clinically healthy children exposed to air pollutants. Inhalation Toxicol 20(5):499–506
Tamayo T, Rathmann W, Krämer U, Sugiri D, Grabert M, Holl RW (2014) Is particle pollution in outdoor air associated with metabolic control in type 2 diabetes? PLoS ONE 9(3):e91639
Brook RD, Xu X, Bard RL, Dvonch JT, Morishita M, Kaciroti N et al (2013) Reduced metabolic insulin sensitivity following sub-acute exposures to low levels of ambient fine particulate matter air pollution. Sci Total Environ 448:66–71
Sun Q, Yue P, Deiuliis JA, Lumeng CN, Kampfrath T, Mikolaj MB et al (2009) Ambient air pollution exaggerates adipose inflammation and insulin resistance in a mouse model of diet-induced obesity. Circulation 119(4):538–546
Zheng Z, Xu X, Zhang X, Wang A, Zhang C, Hüttemann M et al (2013) Exposure to ambient particulate matter induces a NASH-like phenotype and impairs hepatic glucose metabolism in an animal model. J Hepatol 58(1):148–154
Lee P-C, Roberts JM, Catov JM, Talbott EO, Ritz B (2013) First trimester exposure to ambient air pollution, pregnancy complications and adverse birth outcomes in Allegheny County PA. Matern Child Health J 17(3):545–555
Dinh QN, Drummond GR, Sobey CG, Chrissobolis S (2014) Roles of inflammation, oxidative stress, and vascular dysfunction in hypertension. BioMed Res Int 2014:406960
Dastoorpoor M, Khanjani N, Moradgholi A, Sarizadeh R, Cheraghi M, Estebsari F (2021) Prenatal exposure to ambient air pollution and adverse pregnancy outcomes in Ahvaz, Iran: a generalized additive model. Int Arch Occup Environ Health 94(2):309–324
Melody S, Wills K, Knibbs LD, Ford J, Venn A, Johnston F (2020) Adverse birth outcomes in Victoria, Australia in association with maternal exposure to low levels of ambient air pollution. Environ Res 188:109784
Ben-Haroush A, Yogev Y, Hod M (2004) Epidemiology of gestational diabetes mellitus and its association with Type 2 diabetes. Diabet Med 21(2):103–113
Tumminia A, Milluzzo A, Cinti F, Parisi M, Tata F, Frasca F et al (2018) Abnormal 1-hour post-load glycemia during pregnancy impairs post-partum metabolic status: a single-center experience. J Endocrinol Invest 41(5):567–573
Liu F, Guo Y, Liu Y, Chen G, Wang Y, Xue X et al (2019) Associations of long-term exposure to PM1, PM2.5, NO2 with type 2 diabetes mellitus prevalence and fasting blood glucose levels in Chinese rural populations. Environ Int 133:105213
Lucht SA, Hennig F, Matthiessen C, Ohlwein S, Icks A, Moebus S et al (2018) Air pollution and glucose metabolism: an analysis in non-diabetic participants of the Heinz Nixdorf recall study. Environ Health Perspect 126(4):047001
Qiu H, Schooling CM, Sun S, Tsang H, Yang Y, Lee RS-y et al (2018) Long-term exposure to fine particulate matter air pollution and type 2 diabetes mellitus in elderly: a cohort study in Hong Kong. Environ Int 113:350–6
Ha S, Sundaram R, Louis GMB, Nobles C, Seeni I, Sherman S et al (2018) Ambient air pollution and the risk of pregnancy loss: a prospective cohort study. Fertil Steril 109(1):148–153
Padula AM, Yang W, Lurmann FW, Balmes J, Hammond SK, Shaw GM (2019) Prenatal exposure to air pollution, maternal diabetes and preterm birth. Environ Res 170:160–167
Choe S-A, Eliot MN, Savitz DA, Wellenius GA (2019) Ambient air pollution during pregnancy and risk of gestational diabetes in New York City. Environ Res 175:414–420
Pan S-C, Huang C-C, Lin S-J, Chen B-Y, Chan C-C, Guo Y-LL (2017) Gestational diabetes mellitus was related to ambient air pollutant nitric oxide during early gestation. Environ Res 158:318–323
Shen H-N, Hua S-Y, Chiu C-T, Li C-Y (2017) Maternal exposure to air pollutants and risk of gestational diabetes mellitus in Taiwan. Int J Environ Res Public Health 14(12):1604
Acknowledgements
The authors would like to thank all authors of the primary studies included in this review. They also acknowledge Niusha Bakhtyari for designing the graphic abstract.
Funding
No funding was received to conduct this research.
Author information
Authors and Affiliations
Contributions
Research idea and study design: SN and FRT; data acquisition: SN; data analysis/interpretation: SN, MA and RV; statistical analysis: RV; supervision: FRT; Writing—original draft, SN, MA; Writing—review and editing, FRT, RV had equal contribution with corresponding author. All authors have read and approved the final version for submission.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical approval
The study was approved by the ethical committee of the School of Pharmacy and Nursing & Midwifery- Shahid Beheshti University of Medical Sciences (approval ID: IR.SBMU.ENDOCRINE.REC.1401.005).
Research involving human participants and/or animals
All procedures performed in the study involved human participants in accordance with the ethical standards of the Institutional and National Research Committee. This article does not contain any animal studies conducted by any of the authors.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Informed consent
For this type of study, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Nazarpour, S., Ramezani Tehrani, F., Valizadeh, R. et al. The relationship between air pollutants and gestational diabetes: an updated systematic review and meta-analysis. J Endocrinol Invest 46, 1317–1332 (2023). https://doi.org/10.1007/s40618-023-02037-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-023-02037-z