Abstract
Background
Non-thyroidal illness (NTI) is frequent in hospitalized patients. Its recovery is characterized by a raise in TSH levels. However, the clinical significance of high TSH levels at admission in hospitalized elderly patients with NTI remains uncertain.
Aim
To explore the relevance of baseline TSH evaluation in hospitalized elderly patients with NTI.
Methods
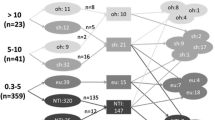
We examined the participants with NTI (n = 123) from our previous study (Sforza, 2017). NTI was defined as: low T3 (< 80 ng/dL) and normal or low total T4 in the presence of TSH values between 0.1 and 6.0 mU/L. Thyroid function tests were performed on day 1 and day 8 of the hospital stay. Positive TSH changes (+ ΔTSH) were considered when the day-8 TSH value increased more than the reference change value for TSH (+ 78%). Multiple logistic regression was used to evaluate the independent association of baseline TSH, sex, clinical comorbidities (by ACE-27) and medications with + ΔTSH.
Results
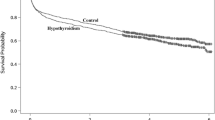
Out of 123 patients (77 ± 8 years, 52% female), 34 showed a + ΔTSH. These patients had a lower TSH at admission (p < 0.001) and intra-hospital mortality (p = 0.003) than the others. In multiple logistic regression, TSH > 2.11 mU/L at baseline was associated with reduced odds to show + ΔTSH [odds ratio (95 CI) 0.29 (0.11–0.75); p = 0.011] in a model adjusted by age, sex and ACE-27.
Discussion
Inappropriately higher TSH levels at admission in hospitalized elderly patients were associated with a reduced ability to raise their TSH levels later on. The present results confront the idea that TSH levels at admission are irrelevant in this clinical context.
Similar content being viewed by others
References
Van den Berghe G, De Zegher F, Bouillon R (1998) Acute and prolonged critical illness as different neuroendocrine paradigms. J Clin Endocrinol Metab 83(6):1827–1834
Wartofsky L, Burman KD (1982) Alterations in thyroid function in patients with systemic illness: the “euthyroid sick syndrome”. Endocr Rev 3(2):164–217
Bianco AC, Salvatore D, Gereben B, Berry MJ, Larsen PR (2002) Biochemistry, cellular and molecular biology, and physiological roles of the iodothyronine selenodeiodinases. Endocr Rev 23(1):38–89
Rothwell PM, Lawler PG (1995) Prediction of outcome in intensive care patients using endocrine parameters. Crit Care Med 23(1):78–83
Docter R, Krenning E, Jong M, Hennemann G (1993) The sick euthyroid syndrome: changes in thyroid hormone serum parameters and hormone metabolism. Clin Endocrinol 39(5):499–518
De Vries E, Fliers E, Boelen A (2015) The molecular basis of the non-thyroidal illness syndrome. J Endocrinol 225(3):67–81. https://doi.org/10.1530/joe-15-0133
Mingote E, Meroño T, Rujelman R, Marquez A, Fossati P, Gurfinkiel M, Schnitman M, Brites F, Faingold C, Brenta G (2012) High TSH and low T4 as prognostic markers in older patients. HORMONES 11(3):350–355
Fliers E, Bianco A, Langouche L, Boelen A (2015) Thyroid function in critically ill patients. Lancet Diabetes Endocrinol 3(10):816–825. https://doi.org/10.1016/s2213-8587(15)00225-9
Iglesias P, Munoz A, Prado F, Guerrero MT, Macias MC, Ridruejo E, Tajada P, Diez JJ (2009) Alterations in thyroid function tests in aged hospitalized patients: prevalence, aetiology and clinical outcome. Clin Endocrinol 70(6):961–967. https://doi.org/10.1111/j.1365-2265.2008.03421.x
McIver B, Gorman C (1997) Euthyroid sick syndrome: an overview. Thyroid 7(1):125–132
Warner M, Beckett G (2010) Mechanisms behind the non-thyroidal illness syndrome: an update. J Endocrinol 205(1):1–13. https://doi.org/10.1677/joe-09-0412
Ayaz T, Sahin SB, Sahin OZ, Bilir O, Rakici H (2014) Factors affecting mortality in elderly patients hospitalized for nonmalignant reasons. J Aging Res 2014:584315. https://doi.org/10.1155/2014/584315
Maldonado LS, Murata GH, Hershman JM, Braunstein GD (1992) Do thyroid function tests independently predict survival in the critically ill? Thyroid 2(2):119–123
Plikat K, Langgartner J, Buettner R, Bollheimer LC, Woenckhaus U, Scholmerich J, Wrede CE (2007) Frequency and outcome of patients with nonthyroidal illness syndrome in a medical intensive care unit. Metabolism 56(2):239–244. https://doi.org/10.1016/j.metabol.2006.09.020
Tognini S, Marchini F, Dardano A, Polini A, Ferdeghini M, Castiglioni M, Monzani F (2010) Non-thyroidal illness syndrome and short-term survival in a hospitalised older population. Age Ageing 39(1):46–50. https://doi.org/10.1093/ageing/afp197
Delpont B, Aboa-Eboule C, Durier J, Petit JM, Daumas A, Legris N, Daubail B, Giroud M, Bejot Y (2016) Associations between thyroid stimulating hormone levels and both severity and early outcome of patients with ischemic stroke. Eur Neurol 76(3–4):125–131. https://doi.org/10.1159/000449055
Kaptein EM, LoPresti JS, Kaptein MJ (2014) Is an isolated TSH elevation in chronic nonthyroidal illness “subclinical hypothyroidism”? J Clin Endocrinol Metab 99(11):4015–4026
Spencer C, Elgen A, Shen D, Duds M, Quails S, Weiss S, Nicoloft J (1987) specificity of sensitive assays of thyrotropin (TSH) used to screen for thyroid disease in hospitalized patients. Clin Chem 33(8):1391–1396
Sforza N, Rosenfarb J, Rujelman R, Rosmarin M, Blanc E, Frigerio C, Fossati P, Caruso D, Faingold C, Merono T, Brenta G (2017) Hypothyroidism in hospitalized elderly patients: a sign of worse prognosis. J Endocrinol Investig 40(12):1303–1310. https://doi.org/10.1007/s40618-017-0690-2
Fraser CG (2001) Biological variation: from principles to practice. American Association of Clinical Chemistry, Washington
Andersen S, Pedersen KM, Bruun NH, Laurberg P (2002) Narrow individual variations in serum T(4) and T(3) in normal subjects: a clue to the understanding of subclinical thyroid disease. J Clin Endocrinol Metab 87(3):1068–1072. https://doi.org/10.1210/jcem.87.3.8165
Iglesias P, Muñoz A, Prado F, Guerrero MT, Macias MC, Ridruejo E, Tajada P, Garcia-Arevalo C, Diez JJ (2010) Serum thyrotropin concentration is an early marker of normalization of low triiodothyronine syndrome in aged hospitalized patients after discharge. J Endocrinol Investig 33(9):607–611. https://doi.org/10.3275/6870, https://doi.org/10.1007/bf03346657
Fliers E, Guldenaar SE, Wiersinga WM, Swaab DF (1997) Decreased hypothalamic thyrotropin-releasing hormone gene expression in patients with nonthyroidal illness. J Clin Endocrinol Metab 82(12):4032–4036
Mendoza A, Hollenberg AN (2017) New insights into thyroid hormone action. Pharmacol Ther 173:135–145. https://doi.org/10.1016/j.pharmthera.2017.02.012
Juarez-Cedillo T, Basurto-Acevedo L, Vega-Garcia S, Sanchez-Rodriguez Martha A, Retana-Ugalde R, Juarez-Cedillo E, Gonzalez-Melendez Roberto C, Escobedo-de-la-Pena J (2017) Prevalence of thyroid dysfunction and its impact on cognition in older mexican adults: (SADEM study). J Endocrinol Investig 40(9):945–952. https://doi.org/10.1007/s40618-017-0654-6
Moon S, Kim MJ, Yu JM, Yoo HJ, Park YJ (2018) Subclinical hypothyroidism and the risk of cardiovascular disease and all-cause mortality: a meta-analysis of prospective cohort studies. Thyroid 28(9):1101–1110. https://doi.org/10.1089/thy.2017.0414
Peeters RP, Wouters PJ, Van Toor H, Kaptein E, Visser TJ, Van den Berghe G (2005) Serum 3,3′,5′-triiodothyronine (rT3) and 3,5,3′-triiodothyronine/rT3 are prognostic markers in critically ill patients and are associated with postmortem tissue deiodinase activities. J Clin Endocrinol Metab 90(8):4559–4565. https://doi.org/10.1210/jc.2005-0535
Acknowledgements
The authors would like to acknowledge all the medical and non-medical staff from the Internal Medicine and Laboratory Departments from the “Dr. César Milstein” Hospital for their cooperation with this study. Noelia Sforza has received additional support from a scholarship granted by the Comisión Nacional Salud Investiga, Ministerio de Salud de la República Argentina.
Author information
Authors and Affiliations
Contributions
DC, CF, TM and GB designed the study and prepared the presentation to the Ethics Review Board of the “Dr. César Milstein” Hospital for approval. JR, NS, RR, AM, CP, and EB were in charge of the recruitment of the patients, performed the clinical evaluations, and registered the medications, the hospital stay and the causes of admission of all the subjects included. DC, CF and GB supervised the protocol development. CF and PF performed the biochemical measurements and filled the study database. TM performed the statistical analyses. JR and NS wrote the manuscript draft. CF, TM and GB reviewed and corrected the manuscript for submission. All the authors approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The author reports no conflicts of interest in this work.
Ethical approval
The study protocol was approved by the Ethics Committee from the Cesar Milstein Hospital. The study was conducted in compliance with the ethical principles for medical research involving human subjects (Declaration of Helsinki).
Informed consent
All the patients, or their relatives, signed the informed consent to participate in the study.
Rights and permissions
About this article
Cite this article
Rosenfarb, J., Sforza, N., Rujelman, R. et al. Relevance of TSH evaluation in elderly in-patients with non-thyroidal illness. J Endocrinol Invest 42, 667–671 (2019). https://doi.org/10.1007/s40618-018-0967-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40618-018-0967-0