Abstract
Background
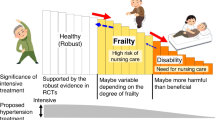
Frailty and hypertension are interrelated, but it remains unclear whether this relationship is modified by antihypertensive drugs.
Methods and results
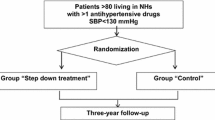
A systematic review of PubMed and Web of Science databases was performed to review the influence of hypertension management on preventing the occurrence or progression of frailty in older people aged 65 and over. Studies providing information on this association regardless of the study setting, or definition of hypertension and frailty were included. Among the initial 2298 articles identified, 7 were included in the review. Three observational studies assessed the association between frailty and hypertension. Two of them reported no relationship between Aldosterone Antagonists use and frailty prevention. No relationship between BP and incidence frailty after adjustment for hypertension treatment was observed in two other articles. An indirect relationship was reported in the RCTs included. Higher AT11RaAb levels (control group), can lead to a generalized weakness/frailty risk shown by a decrease in grip strength (r = –0.57, p < 0.005) and walking speed (r = – 0.47, p < 0.005). No significant differences between int-hypertensive intervention and control were observed in frailty status after a 12-weeks follow-up after applying three different frailty measurement tools in the other RCT.
Conclusions
Based on the results of this systematic review we conclude that BP and frailty occur together but whether the treatment with anti-hypertensive drugs modifies this relationship remains unclear and needs to be further investigated.


Similar content being viewed by others
Availability of data and materials
Not applicable.
References
United Nations Department of Economic and Social Affairs, Population Division (2020) World Population Ageing 2020 Highlights: Living arrangements of older persons (ST/ESA/SER.A/451)
Clegg A, Young J, Iliffe S, Rikkert MO et al (2013) Frailty in elderly people. Lancet 381:752–762
Vetrano DL, Palmer KM, Galluzzo L, Giampaoli S, Marengoni A, Bernabei R, Onder G, Joint Action ADVANTAGE, WP4 group, (2018) Hypertension and frailty: a systematic review and meta-analysis. BMJ 8:e024406
World Health Organization Clinical Consortium on Healthy Ageing (2017) Report of consortium meeting 1–2 December 2016. World Health Organization, Geneva
Cesari M, Prince M, Thiyagarajan JA et al (2016) Frailty: An Emerging Public Health. J Am Med Dir Assoc 17:188–192
Ma L, Zhang L, Sun F, Li Y et al (2018) Frailty in chinese older adults with hypertension: prevalence, associated factors, and prediction for long-term mortality. J Clin Hypertens (Greenwich) 20:1595–1602
Aprahamian I, Sassaki E, Dos Santos MF et al (2018) Hypertension and frailty in older adults. J Clin Hypertens (Greenwich) 20:186–192
Jankowska-Polańska B, Dudek K, Szymanska-Chabowska A, Uchmanowicz I (2016) The influence of frailty syndrome on medication adherence among elderly patients with hypertension. Clin Interv Aging 11:1781–1790
Warwick J, Falaschetti E, Rockwood K, Mitnitski A et al (2015) No evidence that frailty modifies the positive impact of antihypertensive treatment in very elderly people: an investigation of the impact of frailty upon treatment effect in the HYpertension in the Very Elderly Trial (HYVET) study, a double-blind, placeb. BMC Med 13:78
Fattori A, Santimaria MR, Alves RM, Guariento ME et al (2013) Influence of blood pressure profile on frailty phenotype in community-dwelling elders in Brazil - FIBRA study. Arch Gerontol Geriatr 56:343–349
World Health Organization. Hypertension. https://www.who.int/health-topics/hypertension/#tab=tab_1. Accessed 12 Aug 2022
Benetos A, Petrovic M, Strandberg T (2020) Hypertension management in older and frail older patients. Circ Res 124:1045–1060
Graciani AG-EE, López-García E, Banegas JR et al (2020) Ideal cardiovascular health and risk of frailty in older adults. Circulat Cardiovasc Qual Outcomes 9:239–245
Whelton PK, Carey RM, Aronow WS et al (2018) 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults: Executive Summary: A Report of the American College of Cardiology/American Heart Association Task F. Hypertension 71:1269–1324
Iadecola C, Duering M, Hachinski V et al (2019) Vascular cognitive impairment and dementia: JACC scientific expert panel. J Am Coll Cardiol 73:3326–3344
Mone P, Gambardella J, Pansini A et al (2021) Cognitive impairment in frail hypertensive elderly patients: role of hyperglycemia. Cells 10:2115
Satizabal C, Beiser AS, Seshadri S (2016) Incidence of dementia over three decades in the framingham heart study. N Engl J Med 375:93–94
Panza F, Seripa D, Solfrizzi V et al (2015) Targeting cognitive frailty: clinical and neurobiological roadmap for a single complex phenotype. J Alzheimers Dis 47:793–813
Elias PK, Elias MF, Robbins MA et al (2004) Blood pressure-related cognitive decline: does age make a difference? Hypertension 44:631–636
Ma L, Chan P (2020) Understanding the physiological links between physical frailty and cognitive decline. Aging Dis 11:405–418
Paul M, Ridker M, MPH, Nancy Cook S. (2004) Clinical usefulness of very high and very low levels of c-reactive protein across the full range of framingham risk scores. Circulation 109:1955–1959
Rockwood K, Song X, MacKnight C et al (2005) A global clinical measure of fitness and frailty in elderly people. CMAJ 173:489–495
Page MJ, McKenzie JE, Bossuyt PM et al (2020) Statement: an updated guideline for reporting systematic reviews. BMJ 2021:n71
Ouzzani M, Hammady H, Fedorowicz Z et al (2016) Rayyan-a web and mobile app for systematic reviews. Syst Rev 5:210
National Heart Lung and Blood Institute. Study Quality Assessment Tools. July 2021 [cited 2022 August 12]. https://www.nhlbi.nih.gov/health-topics/study-quality-assessment-tools
Sterne JAC, Savovic J, Page MJ et al (2019) RoB 2: a revised tool for assessing risk of bias in randomised trials. BMJ 366:l4898
Sanders NA, Supiano MA, Lewis EF et al (2018) The frailty syndrome and outcomes in the TOPCAT trial. Eur J Heart Fail 20:1570–1577
Abadir PM, Jain A, Powell LJ, Xue QL et al (2017) Discovery and validation of agonistic angiotensin receptor autoantibodies as biomarkers of adverse outcomes. Circulation 135:449–459
Fried LP,Tangen CM, Walston J et al (2001) CHSCR Frailty in older adults: evidence for a phenotype. J Gerontol A Biol Sci Med Sci 56:M146–M156
Anker D, Santos-Eggimann B, Zwahlen M, Santschi V et al (2019) Blood pressure in relation to frailty in older adults: a population-based study. J Clin Hypertens (Greenwich) 21:1895–1904
Ghazi LY, Yaffe K, Tamura MK, Rahman M et al (2020) Association of 24-hour ambulatory blood pressure patterns with cognitive function and physical functioning in CKD. Clin J Am Soc Nephrol 15:455–464
Gray SL, LaCroix AZ, Aragaki AK, McDermott M, Cochrane BB, Kooperberg CL, Murray AM, Rodriguez B, Black H, Woods NF et al Women's Health Initiative Observational Study (2009) Angiotensin-converting enzyme inhibitor use and incident frailty in women aged 65 and older: prospective findings from the Women’s Health Initiative Observational Study. J Am Geriatr Soc 57:297–303
Wu Z, Zhang Y, Yu Q et al (2017) Association of frailty with morning blood pressure and blood pressure variability in elderly patients with hypertension. Int J Clin Exp Med 10:11172–11178
Sheppard JP, Burt J, Lown M, Temple E et al (2020) Effect of antihypertensive medication reduction vs usual care on short-term blood pressure control in patients with hypertension aged 80 years and older: the optimise randomized clinical trial. JAMA 323:2039–2051
Boyd PJ, Nevard M, Ford JA, Khondoker M et al (2019) The electronic frailty index as an indicator of community healthcare service utilisation in the older population. Age Ageing 48:273–277
Morley JE, Malmstrom TK, Miller DK (2012) A simple frailty questionnaire (FRAIL) predicts outcomes in middle aged African Americans. J Nutr Health Aging 16:601–608
Vella Azzopardi R, Beyer I, Vermeiren S et al (2018) Increasing use of cognitive measures in the operational definition of frailty—a systematic review. Ageing Res Rev 7:10–16
Aprahamian I, Xue QL (2021) Shaping the next steps of research on frailty: challenges and opportunities. BMC Geriatr 21:432
Kojima G, Liljas A, Liffe S (2019) Frailty syndrome: implications and challenges for health care policy. Risk Manag Healthc Policy 12:23–30
Acknowledgements
Members of the Gerontopole Brussels Study group:
Ivan Bautmans (FRIA, VUB) ivan.bautmans@vub.be;
Dominque Verté (Belgian Ageing Studies BAST, VUB) dominique.verte@vub.be;
Ingo Beyer (Geriatric Medicine department, UZ Brussel) ingo.beyer@uzbrussel.be;
Mirko Petrovic (ReFrail, UGent) mirko.petrovic@ugent.be;
Nico De Witte (Belgian Ageing Studies BAST, VUB) nico.de.witte@vub.be;
Tinie Kardol (Leerstoel Bevordering Active Ageing, VUB) mjmkardol@hotmail.com;
Gina Rossi (Clinical and Lifespan Psychology KLEP, VUB) grossi@vub.be;
Peter Clarys (Physical Activity and Nutrition PANU, VUB) pclarys@vub.be;
Aldo Scafoglieri (Experimental Anatomy EXAN, VUB) aldo.scafoglieri@vub.be;
Erik Cattrysse (Experimental Anatomy EXAN, VUB) ecattrys@vub.be;
Paul de Hert (Fundamental Rights and Constitutionalism Research group FRC, VUB) paul.de.hert@vub.be;
Bart Jansen (Department of Electronics and Informatics ETRO, VUB) bart.jansen@vub.be
Funding
This study was funded by an “Interdisciplinary Research Program” grant from the research council of the Vrije Universiteit Brussel (VUB).
Author information
Authors and Affiliations
Consortia
Contributions
Ivan BAUTMANS conceived the review idea, acquired the funding and contribute to the review protocol, selection of the articles, interpretation of the data, and writing and editing of the manuscript. Orgesa QIPO and Aziz DEBAIN performed the literature search, article selection, quality assessment, data extraction and prepared the original draft of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Qipo, O., Debain, A., Bautmans, I. et al. The influence of hypertension management on frailty prevention among older persons aged 65 and over: a systematic review. Aging Clin Exp Res 34, 2645–2657 (2022). https://doi.org/10.1007/s40520-022-02247-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40520-022-02247-0