Abstract
Purpose
The SCOFF questionnaire was designed as a simple, memorable screening tool to raise suspicion that a person might have an eating disorder. It is over 20 years since the creation of the SCOFF, during which time it has been widely used. Considering this, we wish to review the use of the SCOFF in peer-reviewed scientific journals, and to assess whether it is being used appropriately in the manner in which it was originally devised and tested.
Methods
The Preferred Reporting Items for a Systematic Review and Meta-analysis (PRISMA) guidelines were followed, and all search strategies and methods were determined before the onset of the study. PubMed and Wiley Online Library were searched using the terms SCOFF and eating. Two reviewers were involved in the reviewing process. Criteria for appropriate use of the SCOFF were formalised with the tool’s original authors.
Results
180 articles were included in the final review. 48 articles had used the SCOFF appropriately, 117 articles inappropriately and 15 articles had been mixed in the appropriateness of their use.
Conclusion
This systematic review highlights the inappropriate use of the SCOFF in diverse languages and settings. When used correctly the SCOFF has made a significant contribution to the understanding of eating disorders and its simplicity has been applauded and led to widespread use. However in over two-thirds of studies, the use of the SCOFF was inappropriate and the paper highlights how and in what way it was misused, Guidelines for the appropriate use of the SCOFF are stated. Future validation and avenues of research are suggested.
Level of evidence
Level I.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Early detection and treatment of eating disorders (EDs) can improve prognosis and likelihood of recovery [1], however their presence can often be overlooked or misdiagnosed initially by clinicians [2]. With an estimated 55.5 million people affected [3] and rates appearing to be on the rise [4, 5], the use of tools to assist in the timely identification and access to support for ED sufferers is important.
The SCOFF questionnaire, first published in 1999, was designed as a simple, memorable screening tool to raise suspicion that an ED might exist [6]. It was developed in response to a lack of robust short screening measures, particularly for use in primary care [7]. The questionnaire was intended to suggest a likely case, rather than to diagnose an ED, and to be followed up by a thorough assessment with a trained clinician prior to diagnosis [6]. It was validated against the DSM-IV diagnostic criteria for anorexia nervosa (AN) and bulimia nervosa (BN) [6]. The measure has been used widely since its conception in both clinical and research settings and has gained traction in popular culture with features in publications such as Teen Vogue [8] and GQ magazine [9]. However, we have become aware of some examples of the inappropriate use of the SCOFF as a diagnostic rather than screening tool; for example, it was recently employed as part of the NHS Health Survey for England to estimate the prevalence of EDs in the country [10].
It is over 20 years since the SCOFF was devised and tested and we, the original developers, conscious of its widespread use in many countries and languages, feel it timely to review its use in peer-reviewed scientific journals. This paper reviews a large sample of the available literature and assesses the appropriateness of the SCOFF’s use in each publication. The review will not be addressing the SCOFF’s misuse amongst non-research settings (e.g. public health campaigns), however it will aim to clarify the guidelines of using the SCOFF, thereby benchmarking the future use of the SCOFF. To the authors’ knowledge, there have not been similar reviews assessing the appropriate use of the SCOFF questionnaire.
Method
Search strategy and inclusion criteria
The Preferred Reporting Items for a Systematic Review and Meta-analysis (PRISMA) guidelines [11] were followed in preparing this systematic review and all search strategies and methods were determined before the onset of the study. The review was not registered. The intention to conduct the review was announced at a national and an international conference and it was agreed by the original authors and the editor of a potential journal. The intention was stated on the UK ED specialist website to avoid unnecessary duplication.
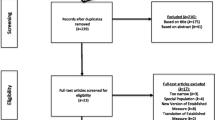
For the literature search, PubMed and Wiley Online Library were employed. The publication timeframe was limited to 1999 (the year the questionnaire was developed) through to the date of the search. The search terms SCOFF and eating were searched for in the title and/or abstract. It was felt these search terms captured the breadth of the literature whilst excluding many publications which used the term ‘scoff’ in the colloquial sense. The results from the search are given in Fig. 1.
Two reviewers (ACo and ACl) were involved in the search process and the results were considered in two steps. Initially, the titles and abstracts of each article were reviewed, by either ACo or ACl, using the following inclusion criteria: (1) a journal article published in an academic journal; (2) the article was written in English and/or a translation was available; (3) the article was related to eating and/or mental health. The full text of those articles included were then examined. During the full review articles were required to meet the initial inclusion criteria and, in addition, demonstrate use of the SCOFF questionnaire as a primary focus within their research (i.e. not simply as a reference). To avoid conflicts of interest, articles authored by the original SCOFF authors in relation to the development of the tool were excluded. Full text articles were reviewed twice—once by each reviewer to ensure the review was robust and objective. Finally, articles included in the final review were assessed to be either appropriate or inappropriate in their use of the SCOFF. It was felt that a subsection of articles were less clear cut in the appropriateness of their use of the measure. These articles tended to have used the SCOFF appropriately, however could have ideally used more caution in their interpretation of the results or been more clear and consistent in their description of the measure and/or results. As such, these were classified as ‘mixed’ use. The classification of each article was cross-checked by each reviewer independently. Any uncertainties at any stage of the review process were resolved by the SCOFF’s original authors.
Data extraction and quality assessment
The reviewers (ACo and ACl) used a data collection tracker to extract data on the title, database extracted from, author(s), year of publication, research study design, aim of the study, the use of the SCOFF questionnaire, and the appropriateness of its use. Criteria for appropriate use—which were developed with the tool’s original authors—are shown in Table 1.
The quality of the research articles included in this systematic review was not analysed, beyond looking at the appropriate use of the SCOFF, as it was important for articles of all quality to be included to assess the full breadth of research.
Results
A full overview of the articles reviewed and details of the findings can be found in the supplementary table (Supplementary Information). One hundred and eighty articles met the criteria for inclusion in the review (Fig. 1). Forty-eight articles had used the SCOFF tool appropriately [12,13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30,31,32,33,34,35,36,37,38,39,40,41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57,58,59], 117 articles had used the SCOFF inappropriately [60,61,62,63,64,65,66,67,68,69,70,71,72,73,74,75,76,77,78,79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105,106,107,108,109,110,111,112,113,114,115,116,117,118,119,120,121,122,123,124,125,126,127,128,129,130,131,132,133,134,135,136,137,138,139,140,141,142,143,144,145,146,147,148,149,150,151,152,153,154,155,156,157,158,159,160,161,162,163,164,165,166,167,168,169,170,171,172,173,174,175,176] and 15 articles had been mixed in their use [177,178,179,180,181,182,183,184,185,186,187,188,189,190,191]. The review found 16 translations of the SCOFF, including Italian, Brazilian-Portuguese, Arabic and Chinese (more information can be found in the Supplementary Information). Table 2 gives a summary of the usage errors in the ‘not appropriate’ and ‘mixed’ categories. A subsection of articles fell under multiple usage errors (see Supplementary Information for further details).
Discussion
Early detection of EDs is an important factor for improved prognosis [1]. The SCOFF questionnaire was developed primarily for use, as a screening tool in primary care, to facilitate early detection of EDs [7]. This review examined the widespread use of the SCOFF questionnaire in the academic field. Its use has assisted in expanding knowledge and the understanding of eating disorders. However, it is clear from this review that the original function of the tool, that is, to raise suspicion that an eating disorder may be present, has in many cases been lost. Researchers, clinicians and peer-reviewed journals need to be more rigorous in only accepting data when the SCOFF is used as described in the original studies which reported its efficacy and reliability. This should not preclude, however, encouraging some exciting avenues of the SCOFF’s use which require further research, such as the validation of SCOFF for DSM-V criteria for EDs, and the use of the SCOFF to assess risk of future EDs. To assist, we have provided guidelines for appropriate use of the SCOFF in Table 1.
This review shows that the use of the SCOFF has grown globally and has been translated into many different languages. Overall, the translation of the SCOFF was executed well with the use of back-translation methods, or similar, and for most translations the modified version was further validated. The vast translation and global use of the SCOFF reflects its memorability and simplicity.
The authors found that the level of caution used when reporting and interpreting the SCOFF results was insufficient and/or inconsistent in a large number of articles. Researchers must remain mindful as to the screening nature of the SCOFF and report their results in line with this. It is paramount that the reader is clear the SCOFF merely raises the suspicion that an ED may exist, as opposed to confirming its presence as a diagnostic fact.
The SCOFF was at times employed to assess a persons’ future risk of developing an ED, which is distinctly different to assessing the likelihood that an ED may exist currently. The items on the SCOFF tool address the core features of AN and BN. To measure a person’s future risk of developing an ED, greater focus on risk factors is needed [192]. Additionally, the SCOFF has not been validated against future risk and as such this use should be avoided until further validation has been completed. Some articles mistakenly interpreted a negative SCOFF result as indicating ‘no risk of ED’, while others were imprecise or unclear in their use of the terminology around risk. Other articles presented the ‘risk of EDs’ for their whole sample group—this is effectively prevalence, and reflects SCOFF being used inappropriately in a diagnostic tool.
There is perhaps a more philosophical question around the meaningfulness of studies looking for correlates or predictors of being screened positive on SCOFF (i.e. using an endpoint of ‘positive/negative screen’ or ‘at higher risk of having an ED/not higher risk’). Even when sufficient caveats were provided on the exact meaning of being SCOFF positive, in most cases it seemed that this was being presented as a proxy for having an eating disorder. The use of SCOFF (or indeed any screening tool) to define an endpoint in its own right goes beyond its original purpose and requires careful consideration in studies planning such use.
The SCOFF was also widely used to assess disordered eating (DE). DE is generally considered to refer to abnormal eating behaviour that does not meet the criteria for a clinically diagnosable ED [193]. Although the SCOFF is designed to be supplemented by further clinical assessment, it was developed in line with the core features of AN and BN and was validated against DSM-IV diagnostic guidelines [6]. As such, the SCOFF has not been validated to assess eating behaviour that does not meet the diagnostic threshold. From the articles included in this review, there does not appear to have been a robust validation of the SCOFF for assessment of DE, however this would be an exciting avenue of research and would further strengthen the tool’s use for early detection within primary care.
The use of the SCOFF to assess ED symptoms was also present in a subsection of the articles reviewed. A number of these articles analysed the individual items of the SCOFF separately to explore specific ED symptoms. Others analysed the SCOFF as a continuous measure (i.e. a higher score indicated more ED symptoms). Again, authors must remain mindful as to the screening nature of the SCOFF. Consisting of just five items, the SCOFF should be taken as a whole, categorical measure to maintain the specificity and sensitivity of the tool. In addition, the original purpose of the tool must be maintained—that is, to raise suspicion that an ED may exist as opposed to assessing the level or presence of symptomatology.
When the SCOFF is used outside of the parameters of its validity and reliability there is a far higher probability of the outcomes being misinterpreted and overstated—as was the case with the media’s coverage of the NHS Health Survey for England [194]. Thus, it is important to ensure the measure is being used appropriately. Nonetheless, it is promising to see an easily accessible screening tool, such as the SCOFF, used so widely within academia and an ever-growing body of research into EDs. There are some exciting avenues of research to explore expanding the scope of the SCOFF. However, in the absence of further validation, the authors of this review, and the original authors of the SCOFF, propose the criteria for appropriate use of the questionnaire detailed in the methodology of this review (Table 1) be used at present to preserve its function as a screening tool.
Strengths and limitations
The primary strength of this review is the number of articles included due to the wide scope of the search strategy. In addition, the inclusion of a secondary reviewer ensured a robust methodology and limited the subjectivity of the results. Due to the vast amount of research employing the SCOFF and the limited manpower of this review, the decision was made to limit the search to just two databases and not to conduct further stages of the search process such as manually searching reference lists. In addition, due to access rights, the reviewers were limited in the databases they were able to search, hence why PubMed and Wiley Online Library were selected. The authors acknowledge that, as such, a subsection of relevant articles may have been missed, however it is felt that the objective of the review was achieved nevertheless, and the review remained systematic in nature due to the methods employed.
Conclusion
This paper reviewed and assessed the use of the SCOFF questionnaire in a large sample of academic papers. In two-thirds of cases, researchers used the SCOFF inappropriately and this paper highlights how and in what way it was misused, However, when used correctly (using the guidelines given in Table 1), the SCOFF remains a relevant, valid and reliable tool for the screening of possible ED cases. Its use within the research field and beyond is indicative of the ever-growing exploration into and understanding of these disorders. There are exciting avenues of future research identified in this review which the authors encourage, including validation of the SCOFF against updated DSM-5 criteria, its ability to assess future risk, and its efficacy in screening for DE.
What is already known on this subject?
The use of the SCOFF is commonplace within academic literature. The original article detailing the development of the SCOFF outlined its intended use.
What this study adds?
This review shows that in many peer-reviewed papers, the SCOFF is used inappropriately and the paper details how and in what way it is misused. The paper re-establishes guidelines for the SCOFF’s appropriate use.
Data availability
Detailed data availability is in the supplementary table available on the online version.
References
Treasure J, Russell G (2011) The case for early intervention in anorexia nervosa: theoretical exploration of maintaining factors. Br J Psychiatry 199:5–7. https://doi.org/10.1192/bjp.bp.110.087585
Mehler P, Andersen A (2010) Eating disorders: a quick guide to medical care and complications, 2nd edn. John Hopkins University Press, Baltimore
Santomauro DF, Melen S, Mitchison D et al (2021) The hidden burden of eating disorders: an extension of estimates from the global burden of disease study 2019. Lancet Psychiatry 8:320–328. https://doi.org/10.1016/S2215-0366(21)00040-7
NHS England (2022) NHS treating record number of young people for eating disorders. In: NHS England. https://www.england.nhs.uk/2022/03/nhs-treating-record-number-of-young-people-for-eating-disorders/. Accessed 15 June 2022
Devoe DJ, Han A, Anderson A et al (2023) The impact of the COVID-19 pandemic on eating disorders: a systematic review. Int J Eat Disord 56:5–25. https://doi.org/10.1002/eat.23704
Morgan JF, Reid F, Lacey JH (1999) The SCOFF questionnaire: assessment of a new screening tool for eating disorders. BMJ 319:1467–1468. https://doi.org/10.1136/bmj.319.7223.1467
Luck AJ, Morgan JF, Reid F et al (2002) The SCOFF questionnaire and clinical interview for eating disorders in general practice: comparative study. BMJ 325:755–756. https://doi.org/10.1136/bmj.325.7367.755
Benoit A (2016) This is the test doctors use to determine if you might have an eating disorder. In: Teen Vogue. https://www.teenvogue.com/story/eating-disorder-test-used-by-doctors. Accessed 15 June 2022
Barwise A (2017) Everything you need to know about eating disorders in men. In: GQ. https://www.gq-magazine.co.uk/article/eating-disorders-in-men. Accessed 15 June 2022
Marcheselli F, Light R (2020) Health survey for England 2019 eating disorders
Page MJ, McKenzie JE, Bossuyt PM et al (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ. https://doi.org/10.1136/bmj.n71
Aoun A, Garcia FD, Mounzer C et al (2013) War stress may be another risk factor for eating disorders in civilians: a study in Lebanese university students. Gen Hosp Psychiatry 35:393–397. https://doi.org/10.1016/j.genhosppsych.2013.02.007
Aoun A, Azzam J, ElJabbour F et al (2015) Validation of the Arabic version of the SCOFF questionnaire for the screening of eating disorders. East Mediterr Health J 21:326–331. https://doi.org/10.26719/2015.21.5.326
Bryant E, Miskovic-Wheatley J, Touyz SW et al (2021) Identification of high risk and early stage eating disorders: first validation of a digital screening tool. J Eat Disord 9:1–10. https://doi.org/10.1186/s40337-021-00464-y
Burke NL, Hazzard VM, Karvay YG et al (2021) Eating disorder prevalence among multiracial US undergraduate and graduate students: is multiracial risk different than the sum of each identity? Eat Behav 41:101501. https://doi.org/10.1016/j.eatbeh.2021.101501
Castellon P, Sudres JL, Voltzenlogel V (2020) Self-defining memories in female patients with anorexia nervosa. Eur Eat Disord Rev 28:513–524. https://doi.org/10.1002/erv.2739
Chan CW, Leung SF (2015) Validation of the eating disorder examination questionnaire: an online version. J Hum Nutr Diet 28:659–665. https://doi.org/10.1111/jhn.12275
Cotton M-A, Ball C, Robinson P (2003) Four simple questions can help screen for eating disorders. J Gen Intern Med 18:53–56
Dooley-Hash S, Lipson SK, Walton MA, Cunningham RM (2013) Increased emergency department use by adolescents and young adults with eating disorders. Int J Eat Disord 46:308–315. https://doi.org/10.1002/eat.22070
Evans J, Horn K, Cowan D, Brunero S (2020) Development of a clinical pathway for screening and integrated care of eating disorders in a rural substance use treatment setting. Int J Ment Health Nurs 29:878–887. https://doi.org/10.1111/inm.12722
Fairburn CG, Rothwell ER (2015) Apps and eating disorders: a systematic clinical appraisal. Int J Eat Disord 48:1038–1046. https://doi.org/10.1002/EAT.22398
Forbush KT, Wildes JE, Hunt TK (2014) Gender norms, psychometric properties, and validity for the eating pathology symptoms inventory. Int J Eat Disord 47:85–91. https://doi.org/10.1002/eat.22180
Fursland A, Watson HJ (2014) Eating disorders: a hidden phenomenon in outpatient mental health? Int J Eat Disord 47:422–425. https://doi.org/10.1002/eat.22205
Ganson KT, Murray SB, Nagata JM (2021) Associations between eating disorders and illicit drug use among college students. Int J Eat Disord 54:1127–1134. https://doi.org/10.1002/eat.23493
Garcia FD, Grigioni S, Chelali S et al (2010) Validation of the French version of SCOFF questionnaire for screening of eating disorders among adults. World J Biol Psychiatry 11:888–893. https://doi.org/10.3109/15622975.2010.483251
Garcia FD, Grigioni S, Allais E et al (2011) Detection of eating disorders in patients: validity and reliability of the French version of the SCOFF questionnaire. Clin Nutr 30:178–181. https://doi.org/10.1016/j.clnu.2010.09.007
Garcia-Campayo J, Sanz-Carrillo C, Ibañez JA et al (2005) Validation of the Spanish version of the SCOFF questionnaire for the screening of eating disorders in primary care. J Psychosom Res 59:51–55. https://doi.org/10.1016/j.jpsychores.2004.06.005
Hosoda Y, Ohtani T, Hanazawa H et al (2021) Establishment of a Japanese version of the sick, control, one stone, fat, and food (SCOFF) questionnaire for screening eating disorders in university students. BMC Res Notes. https://doi.org/10.1186/s13104-021-05549-0
Jugale PV, Pramila M, Murthy AK, Rangath S (2014) Oral manifestations of suspected eating disorders among women of 20–25 years in Bangalore City, India. J Health Popul Nutr 32:46–50
Kotyuk E, Farkas J, Magi A et al (2019) The psychological and genetic factors of the addictive behaviors (PGA) study. Int J Methods Psychiatr Res 28:e1748. https://doi.org/10.1002/mpr.1748
Koyanagi A, Stickley A, Haro JM (2016) Psychotic-like experiences and disordered eating in the English general population. Psychiatry Res 241:26–34. https://doi.org/10.1016/j.psychres.2016.04.045
Lähteenmäki S, Aalto-Setälä T, Suokas JT et al (2009) Validation of the Finnish version of the SCOFF questionnaire among young adults aged 20 to 35 years. BMC Psychiatry 9:1–8. https://doi.org/10.1186/1471-244X-9-5
Leung SF, Lee KL, Lee SM et al (2009) Psychometric properties of the SCOFF questionnaire (Chinese version) for screening eating disorders in Hong Kong secondary school students: a cross-sectional study. Int J Nurs Stud 46:239–247. https://doi.org/10.1016/j.ijnurstu.2008.09.004
Lichtenstein MB, Haastrup L, Johansen KK et al (2021) Validation of the eating disorder examination questionnaire in Danish eating disorder patients and athletes. J Clin Med 10:3976. https://doi.org/10.3390/jcm10173976
Lichtenstein MB, Hemmingsen SD, Støving RK (2017) Identification of eating disorder symptoms in Danish adolescents with the SCOFF questionnaire. Nord J Psychiatry 71:340–347. https://doi.org/10.1080/08039488.2017.1300322
Liu CY, Tseng MCM, Chen KY et al (2015) Sex difference in using the SCOFF questionnaire to identify eating disorder patients at a psychiatric outpatient clinic. Compr Psychiatry 57:160–166. https://doi.org/10.1016/j.comppsych.2014.11.014
Maguen S, Hebenstreit C, Li Y et al (2018) Screen for disordered eating: improving the accuracy of eating disorder screening in primary care. Gen Hosp Psychiatry 50:20–25. https://doi.org/10.1016/j.genhosppsych.2017.09.004
Mond JM, Myers TC, Crosby RD et al (2008) Screening for eating disorders in primary care: EDE-Q versus SCOFF. Behav Res Ther 46:612–622. https://doi.org/10.1016/j.brat.2008.02.003
Castro AM, Beltrán-Barrios T, Mercado-Lara M (2021) Assessment of the frequency of sleep complaints and menopausal symptoms in climacteric women using the Jenkins sleep scale. Sleep Sci 14:92–100. https://doi.org/10.5935/1984-0063.20200041
Pannocchia L, Di Fiorino M, Giannini M, Vanderlinden J (2011) A psychometric exploration of an Italian translation of the SCOFF questionnaire. Eur Eat Disord Rev 19:371–373. https://doi.org/10.1002/erv.1105
Parker SC, Lyons J, Bonner J (2005) Eating disorders in graduate students: exploring the SCOFF questionnaire as a simple screening tool. J Am Coll Health 54:103–107. https://doi.org/10.3200/JACH.54.2.103-107
Phillips L, Kemppainen JK, Mechling BM et al (2015) Eating disorders and spirituality in college students. J Psychosoc Nurs 53:30–37
Prnjak K, Mitchison D, Griffiths S et al (2020) Further development of the 12-item EDE-QS: identifying a cut-off for screening purposes. BMC Psychiatry. https://doi.org/10.1186/s12888-020-02565-5
Estecha Querol S, Fernández Alvira JM, Mesana Graffe MI et al (2016) Nutrient intake in Spanish adolescents SCOFF high-scorers: the AVENA study. Eat Weight Disord 21:589–596. https://doi.org/10.1007/s40519-016-0282-8
Rai D, Kerr MP, McManus S et al (2012) Epilepsy and psychiatric comorbidity: a nationally representative population-based study. Epilepsia 53:1095–1103. https://doi.org/10.1111/j.1528-1167.2012.03500.x
Sánchez-Armass O, Drumond-Andrade FC, Wiley AR et al (2012) Evaluation of the psychometric performance of the SCOFF questionnaire in a Mexican young adult sample. Salud Publica Mex 54:375–382. https://doi.org/10.1590/S0036-36342012000400007
Saßmann H, Albrecht C, Busse-Widmann P et al (2015) Psychometric properties of the German version of the diabetes eating problem survey-revised: additional benefit of disease-specific screening in adolescents with type 1 diabetes. Diabet Med 32:1641–1647. https://doi.org/10.1111/dme.12788
Shaikh MA, Kayani A (2014) Detection of eating disorders in 16–20 year old female students—perspective from Islamabad, Pakistan. J Pak Med Assoc 64:334–336
Siervo M, Boschi V, Papa A et al (2005) Application of the SCOFF, eating attitude test 26 (EAT 26) and eating inventory (TFEQ) questionnaires in young women seeking diet-therapy. Eat Weight Disord 10:76–82. https://doi.org/10.1007/BF03327528
Simioni N, Cottencin O (2016) Screening for eating disorders in outpatient smoking cessation: feasibility, pertinence, and acceptance of referral to specific treatment. Int J Eat Disord 49:1018–1022. https://doi.org/10.1002/eat.22564
Solmi F, Hatch SL, Hotopf M et al (2015) Validation of the SCOFF questionnaire for eating disorders in a multiethnic general population sample. Int J Eat Disord 48:312–316. https://doi.org/10.1002/eat.22373
Teixeira AA, Roque MA (2021) The Brazilian version of the SCOFF questionnaire to screen eating disorders in young adults: cultural adaptation and validation study in a university population. Braz J Psychiatry 43:613–616. https://doi.org/10.1590/1516
Trott M, Johnstone J, McDermott DT et al (2022) The development and validation of the secondary exercise addiction scale. Eat Weight Disord Stud Anorex Bulim Obes 27:1427–1436. https://doi.org/10.1007/s40519-021-01284-4
Tseng MCM, Chen KY, Chang CH et al (2016) Variables influencing presenting symptoms of patients with eating disorders at psychiatric outpatient clinics. Psychiatry Res 238:338–344. https://doi.org/10.1016/j.psychres.2016.02.013
Van Dyke N, Drinkwater EJ (2022) Intuitive eating is positively associated with indicators of physical and mental health among rural Australian adults. Aust J Rural Health 30:468–477. https://doi.org/10.1111/ajr.12856
Wan Wahida WMZ, Lai PSM, Abdul Hadi H (2017) Validity and reliability of the English version of the sick, control, one stone, fat, food (SCOFF) in Malaysia. Clin Nutr ESPEN 18:55–58. https://doi.org/10.1016/j.clnesp.2017.02.001
Zickgraf HF, Hazzard VM, O’Connor SM (2022) Food insecurity is associated with eating disorders independent of depression and anxiety: findings from the 2020–2021 healthy minds study. Int J Eat Disord 55:354–361. https://doi.org/10.1002/eat.23668
Goldstone AP, Prechtl De Hernandez CG, Beaver JD et al (2009) Fasting biases brain reward systems towards high-calorie foods. Eur J Neurosci 30:1625–1635. https://doi.org/10.1111/j.1460-9568.2009.06949.x
Khalil RB, Dagher R, Zarzour M et al (2022) The impact of lockdown and other stressors during the COVID-19 pandemic on depression and anxiety in a Lebanese opportunistic sample: an online cross-sectional survey. Curr Psychol. https://doi.org/10.1007/s12144-021-02644-0
Azzouzi N, Ahid S, Bragazzi NL et al (2019) Eating disorders among Moroccan medical students: cognition and behavior. Psychol Res Behav Manag 12:129–135. https://doi.org/10.2147/PRBM.S165114
Bizri M, Geagea L, Kobeissy F, Talih F (2020) Prevalence of eating disorders among medical students in a Lebanese medical school: a cross-sectional study. Neuropsychiatr Dis Treat 16:1879–1887. https://doi.org/10.2147/NDT.S266241
Di Lodovico L, Dubertret C, Ameller A (2018) Vulnerability to exercise addiction, socio-demographic, behavioral and psychological characteristics of runners at risk for eating disorders. Compr Psychiatry 81:48–52. https://doi.org/10.1016/j.comppsych.2017.11.006
Esteban-Gonzalo L, Veiga OL, Gómez-Martínez S et al (2014) Length of residence and risk of eating disorders in immigrant adolescents living in Madrid; the AFINOS study. Nutr Hosp 29:1047–1053. https://doi.org/10.3305/nh.2014.29.5.7387
Fragkos KC, Frangos CC (2013) Assessing eating disorder risk: the pivotal role of achievement anxiety, depression and female gender in non-clinical samples. Nutrients 5:811–828. https://doi.org/10.3390/nu5030811
Ganson KT, Nagata JM (2021) Associations between vaping and eating disorder diagnosis and risk among college students. Eat Behav 43:101566. https://doi.org/10.1016/j.eatbeh.2021.101566
Garrido-Miguel M, Torres-Costoso A, Martínez-Andrés M et al (2019) The risk of eating disorders and bone health in young adults: the mediating role of body composition and fitness. Eat Weight Disord 24:1145–1154. https://doi.org/10.1007/s40519-017-0458-x
Hazzard VM, Simone M, Borg SL et al (2020) Disparities in eating disorder risk and diagnosis among sexual minority college students: findings from the national healthy minds study. Int J Eat Disord 53:1563–1568. https://doi.org/10.1002/eat.23304
Chan MMH, Zarate-Lopez N, Martin L (2022) Group education on the low FODMAP diet improves gastrointestinal symptoms but neither anxiety or depression in irritable bowel syndrome. J Hum Nutr Diet 35:425–434. https://doi.org/10.1111/jhn.12951
Mari A, Hosadurg D, Martin L et al (2019) Adherence with a low-FODMAP diet in irritable bowel syndrome: are eating disorders the missing link? Eur J Gastroenterol Hepatol 31:178–182. https://doi.org/10.1097/MEG.0000000000001317
Memon AA, Adil SE-E-R, Siddiqui EU et al (2012) Eating disorders in medical students of Karachi, Pakistan—a cross-sectional study. BMC Res Notes 5:84. https://doi.org/10.1186/1756-0500-5-84
Pustivšek S, Hadzić V, Dervišević E, Carruthers J (2020) Risk for eating disorders and body composition among adolescent female and male athletes and non-athlete controls. Int J Adolesc Med Health 32:20170190. https://doi.org/10.1515/ijamh-2017-0190
Pustivšek S, Hadžić V, Derviševic E (2015) Risk factors for eating disorders among male adolescent athletes. Zdr Varst 54:58–65. https://doi.org/10.1515/sjph-2015-0008
Tavolacci MP, Grigioni S, Richard L et al (2015) Eating disorders and associated health risks among university students. J Nutr Educ Behav 47:412-420.e1. https://doi.org/10.1016/j.jneb.2015.06.009
Vila-Martí A, Elío I, Sumalla-Cano S (2021) Eating behavior during first-year college students, including eating disorders—RUVIC-RUNEAT-TCA project. Protocol of an observational multicentric study. Int J Environ Res Public Health 18:9457. https://doi.org/10.3390/ijerph18189457
Zeeni N, Doumit R, Kharma JA, Sanchez-Ruiz M-J (2018) Media, technology use, and attitudes: associations with physical and mental well-being in youth with implications for evidence-based practice. Worldviews Evid Based Nurs 15:304–312. https://doi.org/10.1111/wvn.12298
Adelantado-Renau M, Beltran-Valls MR, Toledo-Bonifás M et al (2018) The risk of eating disorders and academic performance in adolescents: DADOS study. Nutr Hosp 35:1201–1207. https://doi.org/10.20960/nh.1778
Aoun A, Joundi J, El Gerges N (2019) Prevalence and correlates of a positive screen for eating disorders among Syrian refugees. Eur Eat Disord Rev 27:263–273. https://doi.org/10.1002/erv.2660
Bou Khalil R, Bou-Orm IR, Tabet Y et al (2020) Disgust and fear: common emotions between eating and phobic disorders. Eat Weight Disord 25:79–86. https://doi.org/10.1007/s40519-018-0512-3
Czegledi E, Szabo K (2016) Hungarian experiences with the beliefs about attractiveness scale. Clin Neurosci 69:98–105. https://doi.org/10.18071/isz.69.0098
Jantzer V, Groß J, Stute F et al (2013) Risk behaviors and externalizing behaviors in adolescents dealing with parental cancer—a controlled longitudinal study. Psychooncology 22:2611–2616. https://doi.org/10.1002/pon.3327
Kroplewski Z, Szcześniak M, Furmańska J, Gójska A (2019) Assessment of family functioning and eating disorders—the mediating role of self-esteem. Front Psychol 10:407456. https://doi.org/10.3389/fpsyg.2019.00921
Leung SF, Joyce Ma LC, Russell J (2013) An open trial of self-help behaviours of clients with eating disorders in an online programme. J Adv Nurs 69:66–76. https://doi.org/10.1111/J.1365-2648.2012.05988.X
Lichtenstein MB, Griffiths MD, Hemmingsen SD, Støving RK (2018) Exercise addiction in adolescents and emerging adults—validation of a youth version of the exercise addiction inventory. J Behav Addict 7:117–125. https://doi.org/10.1556/2006.7.2018.01
Martínez-Gómez D, Veses AM, Gómez-Martínez S et al (2015) Television viewing time and risk of eating disorders in Spanish adolescents: AVENA and AFINOS studies. Pediatr Int 57:455–460. https://doi.org/10.1111/ped.12662
Muros JJ, Ávila-Alche Á, Knox E, Zabala M (2020) Likelihood of suffering from an eating disorder in a sample of Spanish cyclists and triathletes. J Eat Disord. https://doi.org/10.1186/s40337-020-00350-z
Robert M, Buscail C, Allès B et al (2020) Dispositional optimism is associated with weight status, eating behavior, and eating disorders in a general population-based study. Int J Eat Disord 53:1696–1708. https://doi.org/10.1002/eat.23347
Sharifian MJ, Pohjola V, Kunttu K, Virtanen JI (2021) Association between dental fear and eating disorders and body mass index among Finnish university students: a national survey. BMC Oral Health 21:93. https://doi.org/10.1186/s12903-021-01449-8
Veses AM, Martínez-Gõmez D, Gõmez-Martínez S et al (2014) Physical fitness, overweight and the risk of eating disorders in adolescents. The AVENA and AFINOS studies. Pediatr Obes 9:1–9. https://doi.org/10.1111/j.2047-6310.2012.00138.x
Veses AM, Gómez-Martínez S, de Heredia FP et al (2015) Cognition and the risk of eating disorders in Spanish adolescents: the AVENA and AFINOS studies. Eur J Pediatr 174:229–236. https://doi.org/10.1007/s00431-014-2386-3
Vijayalakshmi P, Thimmaiah R, Reddy SSN et al (2017) Gender differences in body mass index, body weight perception, weight satisfaction, disordered eating and weight control strategies among Indian medical and nursing undergraduates. Invest Educ Enferm 35:276–284. https://doi.org/10.17533/udea.iee.v35n3a04
Vijayalakshmi P, Thimmaiah R, Gandhi S, BadaMath S (2018) Eating attitudes, weight control behaviors, body image satisfaction and depression level among Indian medical and nursing undergraduate students. Community Ment Health J 54:1266–1273. https://doi.org/10.1007/s10597-018-0333-x
Andreeva VA, Tavolacci MP, Galan P et al (2019) Sociodemographic correlates of eating disorder subtypes among men and women in France, with a focus on age. J Epidemiol Community Health 73:56–64. https://doi.org/10.1136/jech-2018-210745
Bächle C, Lange K, Stahl-Pehe A et al (2015) Symptoms of eating disorders and depression in emerging adults with early-onset, long-duration type 1 diabetes and their association with metabolic control. PLoS ONE 10:e0131027. https://doi.org/10.1371/journal.pone.0131027
Bénard M, Bellisle F, Kesse-Guyot E et al (2019) Impulsivity is associated with food intake, snacking, and eating disorders in a general population. Am J Clin Nutr 109:117–126. https://doi.org/10.1093/ajcn/nqy255
Coffino JA, Hormes JM (2018) A default option to enhance nutrition within financial constraints: a randomized, controlled proof-of-principle trial. Obesity 26:961–967. https://doi.org/10.1002/oby.22151
Damiri B, Safarini OA, Nazzal Z et al (2021) Eating disorders and the use of cognitive enhancers and psychostimulants among university students: a cross-sectional study. Neuropsychiatr Dis Treat 17:1633–1645. https://doi.org/10.2147/NDT.S308598
Dooley-Hash S, Adams M, Walton MA et al (2019) The prevalence and correlates of eating disorders in adult emergency department patients. Int J Eat Disord 52:1281–1290. https://doi.org/10.1002/eat.23140
Falvey SE, Hahn SL, Anderson OS et al (2021) Diagnosis of eating disorders among college students: a comparison of military and civilian students. Mil Med 186:975–983. https://doi.org/10.1093/milmed/usab084
Farrow CV, Blissett JM (2005) Is maternal psychopathology related to obesigenic feeding practices at 1 year? Obes Res 13:1999–2005. https://doi.org/10.1038/oby.2005.245
Ganson KT, Cunningham ML, Murray SB, Nagata JM (2022) Use of appearance and performance enhancing drugs and substances is associated with eating disorder symptomatology among U.S. college students. Eat Weight Disord Stud Anorex Bulim Obes 27:2245–2250. https://doi.org/10.1007/s40519-022-01364-z
Grüneis V, Schweiger K, Galassi C et al (2021) Sweetness perception is not involved in the regulation of blood glucose after oral application of sucrose and glucose solutions in healthy male subjects. Mol Nutr Food Res 65:2000472. https://doi.org/10.1002/mnfr.202000472
Herpertz-Dahlmann B, Dempfle A, Konrad K et al (2015) Eating disorder symptoms do not just disappear: the implications of adolescent eating-disordered behaviour for body weight and mental health in young adulthood. Eur Child Adolesc Psychiatry 24:675–684. https://doi.org/10.1007/s00787-014-0610-3
Hochkogler CM, Rohm B, Hojdar K et al (2014) The capsaicin analog nonivamide decreases total energy intake from a standardized breakfast and enhances plasma serotonin levels in moderately overweight men after administered in an oral glucose tolerance test: a randomized, crossover trial. Mol Nutr Food Res 58:1282–1290. https://doi.org/10.1002/mnfr.201300821
Hochkogler CM, Lieder B, Rust P et al (2017) A 12-week intervention with nonivamide, a TRPV1 agonist, prevents a dietary-induced body fat gain and increases peripheral serotonin in moderately overweight subjects. Mol Nutr Food Res 61:1600731. https://doi.org/10.1002/mnfr.201600731
Kenny TE, Carter JC (2018) I weigh therefore I am: implications of using different criteria to define overvaluation of weight and shape in binge-eating disorder. Int J Eat Disord 51:1244–1251. https://doi.org/10.1002/eat.22956
Kenny TE, Van Wijk M, Singleton C, Carter JC (2018) An examination of the relationship between binge eating disorder and insomnia symptoms. Eur Eat Disord Rev 26:186–196. https://doi.org/10.1002/ERV.2587
Kenny TE, Singleton C, Carter JC (2017) Testing predictions of the emotion regulation model of binge-eating disorder. Int J Eat Disord 50:1297–1305. https://doi.org/10.1002/eat.22787
Kronfol Z, Khalifa B, Khoury B et al (2018) Selected psychiatric problems among college students in two Arab countries: comparison with the USA. BMC Psychiatry 18:1–9. https://doi.org/10.1186/s12888-018-1718-7
Leung SF, Ma J, Russell J (2013) Enhancing motivation to change in eating disorders with an online self-help program. Int J Ment Health Nurs 22:329–339. https://doi.org/10.1111/j.1447-0349.2012.00870.x
Maïmoun L, Guillaume S, Lefebvre P et al (2018) Effects of the two types of anorexia nervosa (binge eating/purging and restrictive) on bone metabolism in female patients. Clin Endocrinol 88:863–872. https://doi.org/10.1111/cen.13610
McBride O, McManus S, Thompson J et al (2013) Profiling disordered eating patterns and body mass index (BMI) in the English general population. Soc Psychiatry Psychiatr Epidemiol 48:783–793. https://doi.org/10.1007/s00127-012-0613-7
Melchior C, Desprez C, Riachi G et al (2019) Anxiety and depression profile is associated with eating disorders in patients with irritable bowel syndrome. Front Psychiatry 10:928. https://doi.org/10.3389/fpsyt.2019.00928
Patmore J, Meddaoui B, Feldman H (2019) Cultural considerations for treating Hispanic patients with eating disorders: a case study illustrating the effectiveness of CBT in reducing bulimia nervosa symptoms in a Latina patient. J Clin Psychol 75:2006–2021. https://doi.org/10.1002/jclp.22860
Romo L, Ladner J, Kotbagi G et al (2018) Attention-deficit hyperactivity disorder and addictions (substance and behavioral): prevalence and characteristics in a multicenter study in France. J Behav Addict 7:743–751. https://doi.org/10.1556/2006.7.2018.58
Rothschild-Yakar L, Goshen D, Enoch-Levy A et al (2022) General mentalizing, emotional theory of mind and interpersonal mistrust in anorexia nervosa: the validation of the Hebrew version of the Cambridge mindreading face-task. Clin Psychol Psychother 29:240–249. https://doi.org/10.1002/cpp.2626
Safer M, Zemni I, Mili M et al (2020) Eating disorders: prevalence and associated factors among health occupation students in Monastir university (Tunisia). Tunis Med 98:895–912
Spillebout A, Dechelotte P, Ladner J, Tavolacci MP (2019) Mental health among university students with eating disorders and irritable bowel syndrome in France. Rev Epidemiol Sante Publique 67:295–301. https://doi.org/10.1016/j.respe.2019.04.056
Tavolacci MP, Gillibert A, Zhu Soubise A et al (2019) Screening four broad categories of eating disorders: suitability of a clinical algorithm adapted from the SCOFF questionnaire. BMC Psychiatry 19:1–7. https://doi.org/10.1186/s12888-019-2338-6
Tavolacci MP, Déchelotte P, Ladner J (2020) Eating disorders among college students in France: characteristics, help-and care-seeking. Int J Environ Res Public Health 17:1–11. https://doi.org/10.3390/ijerph17165914
Tavolacci MP, Ladner J, Déchelotte P (2021) Sharp increase in eating disorders among university students since the covid-19 pandemic. Nutrients 13:3415. https://doi.org/10.3390/nu13103415
Tavolacci MP, Ladner J, Dechelotte P (2021) COVID-19 pandemic and eating disorders among university students. Nutrients 13:4294. https://doi.org/10.3390/nu13124294
Wróblewska B, Szyc AM, Markiewicz LH et al (2018) Increased prevalence of eating disorders as a biopsychosocial implication of food allergy. PLoS ONE 13:e0198607. https://doi.org/10.1371/journal.pone.0198607
Alcaraz-Ibáñez M, Paterna A, Griffiths MD, Sicilia Á (2020) Examining the role of social physique anxiety on the relationship between physical appearance comparisons and disordered eating symptoms among Spanish emerging adults. Scand J Psychol 61:803–808. https://doi.org/10.1111/sjop.12663
Ammann S, André Berchtold B, Barrense-Dias Y et al (2018) Disordered eating: the young male side. Behav Med 44:289–296. https://doi.org/10.1080/08964289.2017.1341383
Bächle C, Stahl-Pehe A, Rosenbauer J (2016) Disordered eating and insulin restriction in youths receiving intensified insulin treatment: results from a nationwide population-based study. Int J Eat Disord 49:193–198. https://doi.org/10.1002/eat.22463
Baechle C, Castillo K, Straßburger K et al (2014) Is disordered eating behavior more prevalent in adolescents with early-onset type 1 diabetes than in their representative peers? Int J Eat Disord 47:342–352. https://doi.org/10.1002/eat.22238
Baechle C, Hoyer A, Stahl-Pehe A et al (2019) Course of disordered eating behavior in young people with early-onset type 1 diabetes: prevalence, symptoms, and transition probabilities. J Adolesc Health 65:681–689. https://doi.org/10.1016/j.jadohealth.2019.05.016
Berger U, Schaefer JM, Wick K et al (2014) Effectiveness of reducing the risk of eating-related problems using the German school-based intervention program, “Torera”, for preadolescent boys and girls. Prev Sci 15:557–569. https://doi.org/10.1007/s11121-013-0396-4
Elran-Barak R, Bromberg M, Shimony T et al (2020) Disordered eating among Arab and Jewish youth in Israel: the role of eating dinner with the family. Isr J Health Policy Res 9:1–11. https://doi.org/10.1186/s13584-020-00388-z
Feng T, Abebe DS (2017) Eating behaviour disorders among adolescents in a middle school in Dongfanghong, China. J Eat Disord. https://doi.org/10.1186/s40337-017-0175-x
Hansson E, Daukantaité D, Johnsson P (2015) SCOFF in a general Swedish adolescent population. J Eat Disord. https://doi.org/10.1186/s40337-015-0087-6
Hansson E, Daukantaitė D, Johnsson P (2016) Typical patterns of disordered eating among Swedish adolescents: associations with emotion dysregulation, depression, and self-esteem. J Eat Disord 4:28. https://doi.org/10.1186/s40337-016-0122-2
Hansson E, Daukantaité D, Johnsson P (2017) Disordered eating and emotion dysregulation among adolescents and their parents. BMC Psychol. https://doi.org/10.1186/s40359-017-0180-5
Herpertz-Dahlmann B, Wille N, Hölling H et al (2008) Disordered eating behaviour and attitudes, associated psychopathology and health-related quality of life: results of the BELLA study. Eur Child Adolesc Psychiatry 17:82–91. https://doi.org/10.1007/s00787-008-1009-9
Jacob L, Haro JM, Koyanagi A (2018) Attention deficit hyperactivity disorder symptoms and disordered eating in the English general population. Int J Eat Disord 51:942–952. https://doi.org/10.1002/eat.22934
Johnston O, Fornai G, Cabrini S, Kendrick T (2007) Feasibility and acceptability of screening for eating disorders in primary care. Fam Pract 24:511–517. https://doi.org/10.1093/fampra/cmm029
Kaluski DN, Natamba B, Goldsmith R et al (2008) Determinants of disordered eating behaviors among Israeli adolescent girls. Eat Disord 16:146–159. https://doi.org/10.1080/10640260801887303
Ko N, Tam DM, Viet NK et al (2015) Disordered eating behaviors in university students in Hanoi, Vietnam. J Eat Disord 3:1–7. https://doi.org/10.1186/s40337-015-0054-2
Lommi S, Viljakainen HT, Weiderpass E, de Oliveira Figueiredo RA (2020) Children’s eating attitudes test (ChEAT): a validation study in Finnish children. Eat Weight Disord 25:961–971. https://doi.org/10.1007/s40519-019-00712-w
Martin E, Dourish CT, Hook R et al (2020) Associations between inattention and impulsivity ADHD symptoms and disordered eating risk in a community sample of young adults. Psychol Med. https://doi.org/10.1017/S0033291720004638
Peat CM, Von Holle A, Watson H et al (2015) The association between internet and television access and disordered eating in a Chinese sample. Int J Eat Disord 48:663–669. https://doi.org/10.1002/EAT.22359
Petisco-Rodríguez C, Sánchez-Sánchez LC, Fernández-García R et al (2020) Disordered eating attitudes, anxiety, self-esteem and perfectionism in young athletes and non-athletes. Int J Environ Res Public Health 17:1–18. https://doi.org/10.3390/ijerph17186754
Philipp J, Zeiler M, Waldherr K et al (2014) The mental health in Austrian teenagers (MHAT)-study: preliminary results from a pilot study. Neuropsychiatrie 28:198–207. https://doi.org/10.1007/s40211-014-0131-9
Richter F, Strauss B, Braehler E et al (2017) Screening disordered eating in a representative sample of the German population: usefulness and psychometric properties of the German SCOFF questionnaire. Eat Behav 25:81–88. https://doi.org/10.1016/j.eatbeh.2016.06.022
Saleh RN, Salameh RA, Yhya HH, Sweileh WM (2018) Disordered eating attitudes in female students of An-Najah National University: a cross-sectional study. J Eat Disord 6:1–6. https://doi.org/10.1186/s40337-018-0204-4
Solmi F, Hatch SL, Hotopf M et al (2014) Prevalence and correlates of disordered eating in a general population sample: the South East London Community Health (SELCoH) study. Soc Psychiatry Psychiatr Epidemiol 49:1335–1346. https://doi.org/10.1007/s00127-014-0822-3
Štefanová E, Bakalár P, Baška T (2020) Eating-disordered behavior in adolescents: associations with body image, body composition and physical activity. Int J Environ Res Public Health 17:6665. https://doi.org/10.3390/ijerph17186665
Strand M, von Hausswolff-Juhlin Y, Fredlund P, Lager A (2019) Symptoms of disordered eating among adult international adoptees: a population-based cohort study. Eur Eat Disord Rev 27:236–246. https://doi.org/10.1002/erv.2653
Watson HJ, Hamer RM, Thornton LM et al (2015) Prevalence of screening-detected eating disorders in Chinese females and exploratory associations with dietary practices. Eur Eat Disord Rev 23:68–76. https://doi.org/10.1002/erv.2334
Yao S, Zhang R, Thornton LM et al (2021) Screen-detected disordered eating and related traits in a large population sample of females in mainland China: China health and nutrition survey. Int J Eat Disord 54:24–35. https://doi.org/10.1002/eat.23409
Zeiler M, Waldherr K, Philipp J et al (2016) Prevalence of eating disorder risk and associations with health-related quality of life: results from a large school-based population screening. Eur Eat Disord Rev 24:9–18. https://doi.org/10.1002/erv.2368
D’Anna G, Lazzeretti M, Castellini G et al (2021) Risk of eating disorders in a representative sample of Italian adolescents: prevalence and association with self-reported interpersonal factors. Eat Weight Disord. https://doi.org/10.1007/s40519-021-01214-4
Galvão PPDO, Valente JY, Almeida MC et al (2021) Being bullied and using drugs are associate with eating disorder symptoms in Brazilian students. Int J Eat Disord 54:445–450. https://doi.org/10.1002/eat.23436
Giel KE, Zipfel S, Schweizer R et al (2013) Eating disorder pathology in adolescents participating in a lifestyle intervention for obesity: associations with weight change, general psychopathology and health-related quality of life. Obes Facts 6:307–316. https://doi.org/10.1159/000354534
Gilon Mann T, Hamdan S, Bar-Haim Y et al (2018) Different attention bias patterns in anorexia nervosa restricting and binge/purge types. Eur Eat Disord Rev 26:293–301. https://doi.org/10.1002/erv.2593
Hautala L, Junnila J, Helenius H et al (2008) Adolescents with fluctuating symptoms of eating disorders: a 1-year prospective study. J Adv Nurs 62:674–680. https://doi.org/10.1111/j.1365-2648.2008.04697.x
Hautala LA, Junnila J, Helenius H et al (2008) Towards understanding gender differences in disordered eating among adolescents. J Clin Nurs 17:1803–1813. https://doi.org/10.1111/j.1365-2702.2007.02143.x
Hautala L, Junnila J, Alin J et al (2009) Uncovering hidden eating disorders using the SCOFF questionnaire: cross-sectional survey of adolescents and comparison with nurse assessments. Int J Nurs Stud 46:1439–1447. https://doi.org/10.1016/j.ijnurstu.2009.04.007
Hautala L, Helenius H, Karukivi M et al (2011) The role of gender, affectivity and parenting in the course of disordered eating: a 4-year prospective case-control study among adolescents. Int J Nurs Stud 48:959–972. https://doi.org/10.1016/j.ijnurstu.2011.01.014
Karukivi M, Hautala L, Korpelainen J et al (2010) Alexithymia and eating disorder symptoms in adolescents. Eat Disord 18:226–238. https://doi.org/10.1080/10640261003719518
Lenk M, Noack B, Weidner K, Lorenz K (2022) Psychopathologies and socioeconomic status as risk indicators for periodontitis: a survey-based investigation in German dental practices. Clin Oral Investig 26:2853–2862. https://doi.org/10.1007/s00784-021-04263-2
Lipson SK, Sonneville KR (2020) Understanding suicide risk and eating disorders in college student populations: results from a national study. Int J Eat Disord 53:229–238. https://doi.org/10.1002/EAT.23188
Noma S, Nakai Y, Hamagaki S et al (2006) Comparison between the SCOFF questionnaire and the eating attitudes test in patients with eating disorders. Int J Psychiatry Clin Pract 10:27–32. https://doi.org/10.1080/13651500500305275
Peters EM, Bowen R, Balbuena L (2019) Mood instability contributes to impulsivity, non-suicidal self-injury, and binge eating/purging in people with anxiety disorders. Psychol Psychother Theory Res Pract 92:422–438. https://doi.org/10.1111/papt.12192
Purcell R, Jorm AF, Hickie IB et al (2015) Transitions study of predictors of illness progression in young people with mental ill health: study methodology. Early Interv Psychiatry 9:38–47. https://doi.org/10.1111/eip.12079
Robert M, Shankland R, Andreeva VA et al (2022) Resilience is associated with less eating disorder symptoms in the NutriNet-Santé cohort study. Int J Environ Res Public Health 19:1471. https://doi.org/10.3390/ijerph19031471
Šablatúrová N, Gottfried J, Blinka L et al (2021) Eating disorders symptoms and excessive internet use in adolescents: the role of internalising and externalising problems. J Eat Disord 9:1–8. https://doi.org/10.1186/s40337-021-00506-5
Zarychta K, Luszczynska A, Scholz U (2014) The association between automatic thoughts about eating, the actual-ideal weight discrepancies, and eating disorders symptoms: a longitudinal study in late adolescence. Eat Weight Disord 19:199–207. https://doi.org/10.1007/s40519-014-0099-2
Zeiler M, Philipp J, Truttmann S et al (2021) Psychopathological symptoms and well-being in overweight and underweight adolescents: a network analysis. Nutrients 13:4096. https://doi.org/10.3390/nu13114096
Dooley-Hash S, Banker JD, Walton MA et al (2012) The prevalence and correlates of eating disorders among emergency department patients aged 14–20 years. Int J Eat Disord 45:883–890. https://doi.org/10.1002/eat.22026
Giel KE, Hermann-Werner A, Mayer J et al (2016) Eating disorder pathology in elite adolescent athletes. Int J Eat Disord 49:553–562. https://doi.org/10.1002/eat.22511
Ho AS, Soh NL, Walter G, Touyz S (2011) Comparison of nutrition knowledge among health professionals, patients with eating disorders and the general population. Nutr Diet 68:267–272. https://doi.org/10.1111/j.1747-0080.2011.01549.x
Sidani JE, Shensa A, Hoffman B et al (2016) The association between social media use and eating concerns among US young adults. J Acad Nutr Diet 116:1465–1472. https://doi.org/10.1016/j.jand.2016.03.021
Eisenberg D, Golberstein E, Whitlock JL, Downs MF (2013) Social contagion of mental health: evidence from college roommates. Health Econ 22:965–986. https://doi.org/10.1002/hec.2873
Piacentino D, Sani G, Kotzalidis GD et al (2022) Anabolic androgenic steroids used as performance and image enhancing drugs in professional and amateur athletes: toxicological and psychopathological findings. Hum Psychopharmacol 37:e2815. https://doi.org/10.1002/hup.2815
Piacentino D, Kotzalidis GD, Longo L et al (2017) Body image and eating disorders are common among professional and amateur athletes using performance and image enhancing drugs: a cross-sectional study. J Psychoact Drugs 49:373–384. https://doi.org/10.1080/02791072.2017.1359708
Rodríguez Martín A, Novalbos Ruiz JP, Martínez Nieto JM et al (2004) Epidemiological study of the influence of family and socioeconomic status in disorders of eating behaviour. Eur J Clin Nutr 58:846–852. https://doi.org/10.1038/sj.ejcn.1601884
Rodríguez Martín A, Novalbos Ruiz JP, Martinez Nieto JM et al (2005) Characteristics of eating disorders in a university hospital-based Spanish population. Eur J Clin Nutr 59:459–462. https://doi.org/10.1038/sj.ejcn.1602095
Sanchez-Armass O, Raffaelli M, Andrade FCD et al (2017) Validation of the SCOFF questionnaire for screening of eating disorders among Mexican university students. Eat Weight Disord 22:153–160. https://doi.org/10.1007/s40519-016-0259-7
Toromanyan E, Aslanyan G, Amroyan E et al (2007) Efficacy of Slim339® in reducing body weight of overweight and obese human subjects. Phytother Res 21:1177–1181. https://doi.org/10.1002/ptr.2231
Calcaterra V, Mazzoni C, Ballardini D et al (2020) Disturbed eating behaviors in youth with type 1 diabetes: an exploratory study about challenges in diagnosis. Diagnostics 10:1044. https://doi.org/10.3390/diagnostics10121044
Hefner J, Eisenberg D (2009) Social support and mental health among college students. Am J Orthopsychiatry 79:491–499. https://doi.org/10.1037/a0016918
Hicks TM, Roberts MW, Lee JY et al (2013) Knowledge and practice of eating disorders among a group of adolescent dental patients. J Clin Pediatr Dent 38:39–43. https://doi.org/10.17796/jcpd.38.1.p764642162107355
Barry MR, Sonneville KR, Leung CW (2021) Students with food insecurity are more likely to screen positive for an eating disorder at a large, public university in the Midwest. J Acad Nutr Diet 121:1115–1124. https://doi.org/10.1016/j.jand.2021.01.025
Purcell R, Jorm AF, Hickie IB et al (2015) Demographic and clinical characteristics of young people seeking help at youth mental health services: baseline findings of the transitions study. Early Interv Psychiatry 9:487–497. https://doi.org/10.1111/eip.12133
Wright F, Bewick BM, Barkham M et al (2009) Co-occurrence of self-reported disordered eating and self-harm in UK university students. Br J Clin Psychol 48:397–410. https://doi.org/10.1348/014466509X410343
Conceição EM, Gomes FVS, Vaz AR et al (2017) Prevalence of eating disorders and picking/nibbling in elderly women. Int J Eat Disord 50:793–800. https://doi.org/10.1002/eat.22700
Eisenberg D, Nicklett EJ, Roeder K, Kirz NE (2011) Eating disorder symptoms among college students: prevalence, persistence, correlates, and treatment-seeking. J Am Coll Health 59:700–707. https://doi.org/10.1080/07448481.2010.546461
Moser CM, Terra L, Behenck AdS et al (2020) Cross-cultural adaptation and translation into Brazilian Portuguese of the instruments sick control one stone fat food questionnaire (SCOFF), eating disorder examination questionnaire (EDE-q) and clinical impairment assessment questionnaire (CIA). Trends Psychiatry Psychother 42:267–271. https://doi.org/10.1590/2237-6089-2019-0083
Alcaraz-Ibáñez M, Sicilia Á, Paterna A (2019) Exploring the differentiated relationship between appearance and fitness-related social anxiety and the risk of eating disorders and depression in young adults. Scand J Psychol 60:569–576. https://doi.org/10.1111/sjop.12584
Kabakuş Aykut M, Bilici S (2022) The relationship between the risk of eating disorder and meal patterns in university students. Eat Weight Disord 27:579–587. https://doi.org/10.1007/s40519-021-01179-4
Bakalar JL, Shank LM, Vannucci A et al (2015) Recent advances in developmental and risk factor research on eating disorders. Curr Psychiatry Rep 17:42. https://doi.org/10.1007/s11920-015-0585-x
Nurkkala M, Keränen A-M, Koivumaa-Honkanen H et al (2016) Disordered eating behavior, health and motives to exercise in young men: cross-sectional population-based MOPO study. BMC Public Health 16:483. https://doi.org/10.1186/s12889-016-3162-2
Morrison R (2020) One in six adults in England has a possible eating disorder—including almost a third of women aged 16 to 24, study finds. In: MailOnline
Funding
The authors declare that no funds, grants, or other support were received during the preparation of this manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Data collection and analysis were performed by Amy Coop and Amelia Clark. The first draft of the manuscript was written by Amy Coop and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no relevant financial or non-financial interests to disclose.
Ethical approval
This is a review article and so no ethical approval was required.
Informed consent
This is a review paper and no patients or subjects took part; therefore no informed consent was needed.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Coop, A., Clark, A., Morgan, J. et al. The use and misuse of the SCOFF screening measure over two decades: a systematic literature review. Eat Weight Disord 29, 29 (2024). https://doi.org/10.1007/s40519-024-01656-6
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s40519-024-01656-6