Abstract
Purpose
Digital interventions that consider end-user needs, preferences, and concerns may address suboptimal rates of e-health uptake, usage, and engagement. We explored target-user perspectives of e-health treatment and prevention programs for eating disorders (EDs), with a focus on investigating (1) perceived advantages and barriers of e-health; (2) help-seeking intentions; and (3) preferences for different digital functionality, device types, and content-delivery formats.
Methods
Survey data were analysed from 722 community-based participants. Participants were categorized into one of four groups based on symptom presentation and severity, ranging from low risk to probable bulimia nervosa or binge-eating disorder.
Results
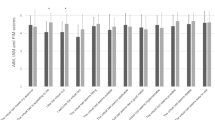
e-health advantages that received the highest endorsement (~ 84%) were “always there in times of need” and “travel not required”. e-health barriers that received the highest endorsement (~ 50%) were concerns about data privacy and the accuracy of content presented. Nearly three-quarters reported an intention to use an e-health platform for preventing or treating EDs. Preference ratings were highest for programs to be available on all digital devices (relative to restricting the program to one type of device) and for content to be presented via graphics and video tutorials (rather than audio-based). e-health functionality that received highest preference ratings (~ 80%) were added clinician support, tailored feedback, strategies to change unhelpful ED thoughts, screening scales to assess symptoms, ED psychoeducation, and just-in-time intervention prompts. Preference and intention ratings were strikingly similar across all subgroups.
Conclusion
Findings may inform the development and design of e-health platforms that meet the needs of people at different stages of an ED.
Level of evidence
Level V, cross-sectional descriptive study.


Similar content being viewed by others
Code availability
Syntax can be provided upon request.
References
Klump KL, Bulik CM, Kaye WH, Treasure J, Tyson E (2009) Academy for eating disorders position paper: eating disorders are serious mental illnesses. Int J Eat Disord 42(2):97–103
Linardon J, Fairburn CG, Fitzsimmons-Craft EE, Wilfley DE, Brennan L (2017) The empirical status of the third-wave behaviour therapies for the treatment of eating disorders: a systematic review. Clin Psychol Rev 58:125–140. https://doi.org/10.1016/j.cpr.2017.10.005
Linardon J, Wade T, De la Piedad GX, Brennan L (2017) The efficacy of cognitive-behavioral therapy for eating disorders: a systematic review and meta-analysis. J Consult Clin Psychol 85:1080–1094. https://doi.org/10.1037/ccp0000245
Weissman RS, Rosselli F (2017) Reducing the burden of suffering from eating disorders: unmet treatment needs, cost of illness, and the quest for cost-effectiveness. Behav Res Ther 88:49–64. https://doi.org/10.1016/j.brat.2016.09.006
Kazdin AE, Fitzsimmons-Craft EE, Wilfley DE (2017) Addressing critical gaps in the treatment of eating disorders. Int J Eat Disord 50:170–189. https://doi.org/10.1002/eat.22670
Andersson G (2016) Internet-delivered psychological treatments. Annu Rev Clin Psychol 12:157–179. https://doi.org/10.1146/annurev-clinpsy-021815-093006
Linardon J, Cuijpers P, Carlbring P, Messer M, Fuller-Tyszkiewicz M (2019) The efficacy of app-supported smartphone interventions for mental health problems: a meta-analysis of randomized controlled trials. World Psychiatry 18:325–336. https://doi.org/10.1002/wps.20673
Loucas CE, Fairburn CG, Whittington C, Pennant ME, Stockton S, Kendall T (2014) E-therapy in the treatment and prevention of eating disorders: a systematic review and meta-analysis. Behav Res Ther 63:122–131. https://doi.org/10.1016/j.brat.2014.09.011
Linardon J, Shatte A, Messer M, Firth J, Fuller-Tyszkiewicz M (2020) E-mental health interventions for the treatment and prevention of eating disorders: an updated systematic review and meta-analysis. J Consult Clin Psychol. https://doi.org/10.1037/ccp0000575
Donkin L, Christensen H, Naismith SL, Neal B, Hickie IB, Glozier N (2011) A systematic review of the impact of adherence on the effectiveness of e-therapies. J Med Internet Res 13:e52. https://doi.org/10.2196/jmir.1772
Linardon J, Fuller-Tyszkiewicz M (2020) Attrition and adherence in smartphone-delivered interventions for mental health problems: a systematic and meta-analytic review. J Consult Clin Psychol 88:1–13. https://doi.org/10.1037/ccp0000459
Tighe J, Shand F, Ridani R, Mackinnon A, De La Mata N, Christensen H (2017) Ibobbly mobile health intervention for suicide prevention in Australian Indigenous youth: a pilot randomised controlled trial. BMJ Open 7:e013518. https://doi.org/10.1136/bmjopen-2016013518
Apolinário-Hagen J, Kemper J, Stürmer C (2017) Public acceptability of e-mental health treatment services for psychological problems: a scoping review. JMIR Mental Health 4(2):e10
Apolinário-Hagen J, Vehreschild V, Alkoudmani RM (2017) Current views and perspectives on e-mental health: an exploratory survey study for understanding public attitudes toward internet-based psychotherapy in Germany. JMIR Mental Health 4:e8. https://doi.org/10.2196/mental.6375
McClay C-A, Waters L, Schmidt U, Williams C (2016) A survey of attitudes towards computerized self-help for eating disorders within a community-based sample. Behav Cognit Psychother 44:65–78
Linardon J, Shatte A, Tepper H, Fuller-Tyszkiewicz M (2020) A survey study of attitudes toward, and preferences for, e-therapy interventions for eating disorder psychopathology. Int J Eat Disord 53:907–916. https://doi.org/10.1002/eat.23268
Apolinário-Hagen J, Harrer M, Kählke F, Fritsche L, Salewski C, Ebert DD (2018) Public attitudes toward guided internet-based therapies: web-based survey study. JMIR Mental Health 5(2):e10735
March S, Day J, Ritchie G, Rowe A, Gough J, Hall T, Yuen CYJ, Donovan CL, Ireland M (2018) Attitudes toward e-mental health services in a community sample of adults: online survey. J Med Internet Res 20(2):e59. https://doi.org/10.2196/jmir.9109
Linardon J, Rosato J, Messer M (2020) Break binge eating: reach, engagement, and user profile of an internet-based psychoeducational and self-help platform for eating disorders. Int J Eat Disord. https://doi.org/10.1002/eat.23356
Carlbring P, Andersson G (2006) Internet and psychological treatment. How well can they be combined? Comput Hum Behav 22(3):545–553
Fairburn CG, Beglin S (1994) Assessment of eating disorders: interview or self-report questionnaire? Int J Eat Disord 16:363–370. https://doi.org/10.1002/1098-108X
American Psychiatric Association (2013) The Diagnostic and Statistical Manual of Mental Disorders, 5th edn. DSM 5. American Psychiatric Association, Virginia
Crow SJ, Stewart Agras W, Halmi K, Mitchell JE, Kraemer HC (2002) Full syndromal versus subthreshold anorexia nervosa, bulimia nervosa, and binge eating disorder: a multicenter study. Int J Eat Disord 32:309–318. https://doi.org/10.1002/eat.10088
Mond J, Hay PJ, Rodgers B, Owen C (2006) Eating disorder examination questionnaire (EDE-Q): norms for young adult women. Behav Res Ther 44:53–62. https://doi.org/10.1016/j.brat.2004.12.003
Lavender JM, De Young KP, Anderson DA (2010) Eating disorder examination questionnaire (EDE-Q): norms for undergraduate men. Eat Behav 11:119–121
Stice E (2002) Risk and maintenance factors for eating pathology: a meta-analytic review. Psychol Bull 128:825–848. https://doi.org/10.1037/0033-2909.128.5.825
Van Straten A, Tiemens B, Hakkaart L, Nolen W, Donker M (2006) Stepped care vs. matched care for mood and anxiety disorders: a randomized trial in routine practice. Acta Psychiatr Scand 113(6):468–476
Richards D, Richardson T (2012) Computer-based psychological treatments for depression: a systematic review and meta-analysis. Clin Psychol Rev 32:329–342. https://doi.org/10.1016/j.cpr.2012.02.004
Kelders SM, Bohlmeijer ET, Pots WTM, van Gemert-Pijnen JEWC (2015) Comparing human and automated support for depression: fractional factorial randomized controlled trial. Behav Res Ther 72:72–80. https://doi.org/10.1016/j.brat.2015.06.014
Juarascio AS, Parker MN, Lagacey MA, Godfrey KM (2018) Just-in-time adaptive interventions: a novel approach for enhancing skill utilization and acquisition in cognitive behavioral therapy for eating disorders. Int J Eat Disord 51:826–830. https://doi.org/10.1002/eat.22924
Ajzen I (1985) From intentions to actions: a theory of planned behavior. In: Action control. Springer, pp 11–39
Fleming T, Bavin L, Lucassen M, Stasiak K, Hopkins S, Merry S (2018) Beyond the trial: systematic review of real-world uptake and engagement with digital self-help interventions for depression, low mood, or anxiety. J Med Internet Res 20(6):e199
Fairburn CG, Rothwell ER (2015) Apps and eating disorders: a systematic clinical appraisal. Int J Eat Disord 48:1038–1046. https://doi.org/10.1002/eat.22398
Stoyanov SR, Hides L, Kavanagh DJ, Zelenko O, Tjondronegoro D, Mani M (2015) Mobile app rating scale: a new tool for assessing the quality of health mobile apps. JMIR mHealth uHealth 3(1):e27
Torous J, Andersson G, Bertagnoli A, Christensen H, Cuijpers P, Firth J, Haim A, Hsin H, Hollis C, Lewis S (2019) Towards a consensus around standards for smartphone apps and digital mental health. World Psychiatry 18:97–98. https://doi.org/10.1002/wps.20592
Rock Health (2015) Digital health consumer adoption. https://rockhealth.com/reports/digital-health-consumer-adoption-2015/.
Levin ME, Haeger J, An W, Twohig MP (2018) Comparing cognitive defusion and cognitive restructuring delivered through a mobile app for individuals high in self-criticism. Cognit Ther Res. https://doi.org/10.1007/s10608-018-9944-3
Kauer SD, Reid SC, Crooke AH, Khor A, Hearps SJ, Jorm AF, Sanci L, Patton G (2012) Self-monitoring using mobile phones in the early stages of adolescent depression: randomized controlled trial. J Med Internet Res 14(3):e67. https://doi.org/10.2196/jmir.1858
Fairburn CG, Patel V (2017) The impact of digital technology on psychological treatments and their dissemination. Behav Res Ther 88:19–25. https://doi.org/10.1016/j.brat.2016.08.012
Fairburn CG, Harrison PJ (2003) Eating disorders. Lancet 361:407–416
Bowring AL, Peeters A, Freak-Poli R, Lim MS, Gouillou M, Hellard M (2012) Measuring the accuracy of self-reported height and weight in a community-based sample of young people. BMC Med Res Methodol 12(1):175
Neumayr C, Voderholzer U, Tregarthen J, Schlegl S (2019) Improving aftercare with technology for anorexia nervosa after intensive inpatient treatment: a pilot randomized controlled trial with a therapist-guided smartphone app. Int J Eat Disord 52:1191–1201. https://doi.org/10.1002/eat.23152
Funding
No funding was received.
Author information
Authors and Affiliations
Contributions
JL and MM were responsible for conceptualising the research, conducting the statistical analyses and drafting the manuscript. SL and JR were responsible for conceptualising aspects of the research and editing the manuscript. All authors approved the final version of this manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflict of interest.
Ethical approval
This research was approved by the Ethical Board at Deakin University.
Informed consent
All participants provided informed consent to participate.
Availability of data and material
Data are available from the corresponding author on request.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Linardon, J., Messer, M., Lee, S. et al. Perspectives of e-health interventions for treating and preventing eating disorders: descriptive study of perceived advantages and barriers, help-seeking intentions, and preferred functionality. Eat Weight Disord 26, 1097–1109 (2021). https://doi.org/10.1007/s40519-020-01005-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40519-020-01005-3