Abstract
Purpose
Respiratory distress syndrome (RDS), also known as hyaline membrane disease, is the most common clinical syndrome encountered among preterm infants, and the complications of the disease account for substantial mortality. Diagnosis of RDS is based on the clinical status of patients in correlation with laboratory parameters and chest X-ray. Lung ultrasound despite its wide use still is not incorporated into diagnostic algorithms. The aim of the study was to evaluate the diagnostic ability of lung ultrasound in diagnosing respiratory distress syndrome as well as in the monitoring of the response to treatment. A secondary aim was to propose a modified ultrasound grading scale.
Methods
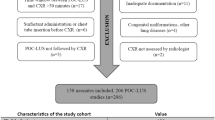
The prospective study included 150 neonates with clinical and radiographic signs of neonatal respiratory distress syndrome within the first 24 h of life, with different gestational age (≤ 35 weeks). Lung ultrasound was performed by two radiologists and correlated with a chest X-ray. Two gradation scales (ultrasound and X-ray) were compared and each scale was correlated with the patient’s clinical data.
Results
In comparison between ultrasound findings and X-ray results showed a statistically significant difference in a favor of ultrasound. Based on the presence of subpleural consolidations, further differentiation of ultrasound profiles were made into subgroups and new ultrasound classification have been proposed.
Conclusion
Our study showed that lung ultrasound enables the diagnosing of respiratory distress syndrome in premature neonates and also shows a significant correlation with chest X-ray, which is considered as a radiological method of choice for the diagnosis of RDS.




















Similar content being viewed by others
References
Jeenakeri R, Drayton M (2009) Management of respiratory distress syndrome. Paediatr Child Health (Oxf) 19(4):158–164. https://doi.org/10.1016/j.paed.2008.12.004
Euro-Peristat Project (2018) Core indicators of the health and care of pregnant women and babies in Europe in 2015. Eur Perinat Heal Rep. https://doi.org/10.1080/03639045.2017.1415927
Fogg MF, Drorbaugh JE (2015) Respiratory distress in the newborn infant. Am J Nurs 56(10):1559–1562
Horbar JD, Soll RF, Edwards WH (2010) The Vermont Oxford Network: a community of practice. Clin Perinatol 37(1):29–47. https://doi.org/10.1016/J.CLP.2010.01.003
Ezz- Eldin ZM, Abdel Hamid TA, Labib Youssef MR, Nabil HED (2015) Clinical risk index for babies (CRIB II) scoring system in prediction of mortality in premature babies. J Clin Diagn Res 9(6):SC08-SC11. https://doi.org/10.7860/JCDR/2015/12248.6012
Singh Y, Tissot C, Fraga MV et al (2020) International evidence-based guidelines on Point of Care Ultrasound (POCUS) for critically ill neonates and children issued by the POCUS Working Group of the European Society of Paediatric and Neonatal Intensive Care (ESPNIC). Crit Care 24(1):1–16. https://doi.org/10.1186/s13054-020-2787-9
Lovrenski J (2020) Pediatric lung ultrasound—pros and potentials. Pediatr Radiol 50(3):306–313. https://doi.org/10.1007/s00247-019-04525-y
Bouhemad B, Zhang M, Lu Q, Rouby JJ (2007) Clinical review: bedside lung ultrasound in critical care practice. Crit Care 11(1):1–9. https://doi.org/10.1186/cc5668
Man MA, Dantes E, Hancu BD et al (2019) Correlation between transthoracic lung ultrasound score and HRCT features in patients with interstitial lung diseases. J Clin Med. https://doi.org/10.3390/jcm8081199
El-Malah HEDGM, Hany S, Mahmoud MK, Ali AM (2015) Lung ultrasonography in evaluation of neonatal respiratory distress syndrome. Egypt J Radiol Nucl Med. 46(2):469–474. https://doi.org/10.1016/j.ejrnm.2015.01.005
M.C. L, E.Y. L. Neonatal lung disorders: Pattern recognition approach to diagnosis. Am J Roentgenol. 2018;210(5):964–975. doi:https://doi.org/10.2214/AJR.17.19231 LK. http://sfx.metabib.ch/sfx_uzh?sid=EMBASE&sid=EMBASE&issn=15463141&id=doi:10.2214%2FAJR.17.19231&atitle=Neonatal+lung+disorders%3A+Pattern+recognition+approach+to+diagnosis&stitle=Am.+J.+Roentgenol.&title=American+Journal+of+Roentgenology&volume=210&issue=5&spage=964&epage=975&aulast=Liszewski&aufirst=Mark+C.&auinit=M.C.&aufull=Liszewski+M.C.&coden=AJROA&isbn=&pages=964-975&date=2018&auinit1=M&auinitm=C.
Soni NJ, Franco R, Velez MI et al (2015) Ultrasound in the diagnosis and management of pleural effusions. J Hosp Med 10(12):811–816. https://doi.org/10.1002/jhm.2434
Mills GH (2005) General ultrasound in the critically ill. Br J Anaesth 95(2):279. https://doi.org/10.1093/bja/aei577
Lichtenstein DA (2009) Lung ultrasound in the critically ill. J Med Ultrasound 17(3):125–142. https://doi.org/10.1016/S0929-6441(09)60120-X
Chiumello D, Froio S, Colombo A, Coppola S (2016) Lung ultrasound in the critically ill patient. Top Issues Anesth Intensive Care 17(3):55–67. https://doi.org/10.1007/978-3-319-31398-6_3
Lichtenstein DA, Mezière GA (2008) Relevance of lung ultrasound in the diagnosis of acute respiratory failure*: the BLUE protocol. Chest 134(1):117–125. https://doi.org/10.1378/chest.07-2800
Liu J, Sorantin E, Cao H. Neonatal lung ultrasonography. 2019. https://doi.org/10.1007/978-94-024-1549-0
Raimondi F, Migliaro F, Sodano A, Vallone G, Ferrara T, Maddaluno S, Coppola C, Capasso L (2013) Point-of-care chest ultrasound in the neonatal intensive care unit. J Pediatr Neonatal Individ Med 2(2):e020214. https://doi.org/10.7363/020214
Hiles M, Culpan AM, Watts C, Munyombwe T, Wolstenhulme S (2017) Neonatal respiratory distress syndrome: chest X-ray or lung ultrasound? A systematic review. Ultrasound 25(2):80–91. https://doi.org/10.1177/1742271X16689374
Santos TM, Franci D, Coutinho CMG et al (2013) A simplified ultrasound-based edema score to assess lung injury and clinical severity in septic patients. Am J Emerg Med 31(12):1656–1660. https://doi.org/10.1016/J.AJEM.2013.08.053
Brat R, Yousef N, Klifa R, Reynaud S, Shankar Aguilera S, De Luca D (2015) Lung ultrasonography score to evaluate oxygenation and surfactant need in neonates treated with continuous positive airway pressure. JAMA Pediatr 169(8):e151797–e151797. https://doi.org/10.1001/jamapediatrics.2015.1797
Lovrenski J (2012) Lung ultrasonography of pulmonary complications in preterm infants with respiratory distress syndrome. Ups J Med Sci 117(1):10–17. https://doi.org/10.3109/03009734.2011.643510
Liu J, Wang Y, Fu W, Yang CS, Huang JJ (2014) Diagnosis of neonatal transient tachypnea and its differentiation from respiratory distress syndrome using lung ultrasound. Medicine (United States) 93(27):23–28. https://doi.org/10.1097/MD.0000000000000197
Kazemi K, Rakhsha M, Pourali L, Ayati S, Boskabadi H, Shakeri MT. Effective maternal and neonatal factors associated with the prognosis of preterm infants A R T I C L E I N F O. 2014;1(Md). http://psj.mums.ac.ir/article_6304_1d0ca0811b289a3d70039f800a98aae0.pdf. .
Navaei F, Aliabady B, Moghtaderi J, Moghtaderi M, Kelishadi R (2010) Early outcome of preterm infants with birth weight of 1500 g or less and gestational age of 30 weeks or less in Isfahan city, Iran. World J Pediatr 6(3):228–232. https://doi.org/10.1007/s12519-010-0204-1
Koller-Smith LI, Shah PS, Ye XY et al (2017) Comparing very low birth weight versus very low gestation cohort methods for outcome analysis of high risk preterm infants. BMC Pediatr 17(1):166. https://doi.org/10.1186/s12887-017-0921-x
Siddiqui A, Cuttini M, Wood R et al (2017) Can the Apgar score be used for international comparisons of newborn health? Paediatr Perinat Epidemiol 31(4):338–345. https://doi.org/10.1111/ppe.12368
Zawada T, Wieczorek A, Garba P (2015) Point of care ultrasound—a way to reduce radiation exposure of patients and medical staff. Intensive Care Med Exp 3(Suppl 1):2197. https://doi.org/10.1186/2197-425X-3-S1-A273
Yu CC (2010) Radiation safety in the neonatal intensive care unit: too little or too much concern? Pediatr Neonatol 51(6):311–319. https://doi.org/10.1016/S1875-9572(10)60061-7
Malone J, Guleria R, Craven C et al (2012) Justification of diagnostic medical exposures: some practical issues. Report of an International Atomic Energy Agency Consultation. Br J Radiol 85(1013):523–538. https://doi.org/10.1259/bjr/42893576
Amis ES, Butler PF, Applegate KE et al (2007) American College of Radiology white paper on radiation dose in medicine. J Am Coll Radiol 4(5):272–284. https://doi.org/10.1016/j.jacr.2007.03.002
Edison P, Chang PS, Toh GH, Lee LN, Sanamandra SK, Shah VA (2017) Reducing radiation hazard opportunities in neonatal unit: quality improvement in radiation safety practices. BMJ Open Qual 6(2):e000128. https://doi.org/10.1136/bmjoq-2017-000128
Lichtenstein D, Axler O (1993) Intensive use of general ultrasound in the intensive care unit. Intensive Care Med 19(6):353–355. https://doi.org/10.1007/BF01694712
Neethling E, Roodt F, Beck C, Swanevelder JLC (2018) Point-of-care and lung ultrasound incorporated in daily practice. S Afr Med J 108(5):376–381. https://doi.org/10.7196/SAMJ.2018.v108i5.13313
Volpicelli G, Elbarbary M, Blaivas M et al (2012) International evidence-based recommendations for point-of-care lung ultrasound. Intensive Care Med 38(4):577–591. https://doi.org/10.1007/s00134-012-2513-4
Raimondi F, Migliaro F, Sodano A et al (2012) Can neonatal lung ultrasound monitor fluid clearance and predict the need of respiratory support? Crit Care 16(6):R220. https://doi.org/10.1186/cc11865
Cattarossi L, Copetti R, Poskurica B, Miserocchi G (2010) Surfactant administration for neonatal respiratory distress does not improve lung interstitial fluid clearance: echographic and experimental evidence. J Perinat Med 38:557. https://doi.org/10.1515/jpm.2010.096
Rodríguez-Fanjul J, Moreno Hernando J, Iriondo Sanz M. PS-375 can lung ultrasound change respiratory distress management in newborns? Abstract PS-375 Table 1. Arch Dis Child. 2014;99(Suppl 2):A247.2–A248. https://doi.org/10.1136/archdischild-2014-307384.674
Corradi F, Via G, Forfori F, Brusasco C, Tavazzi G (2020) Lung ultrasound and B-lines quantification inaccuracy: B sure to have the right solution. Intensive Care Med 46(5):1081–1083. https://doi.org/10.1007/s00134-020-06005-6
Funding
The authors did not receive support from any organization for the submission of the manuscript. No funding was received to assist with the preparation of this manuscript. No funding was received for conducting this study. No funds, grants, or other support was received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose. The authors have no competing interest to declare that are relevant to the content of this article. All authors certify that they no affiliations with or involvement in any organization or entity with any financial interest or non-financial interest in the subject matter or materials discussed in this manuscript. The authors have no financial or proprietary interest in any material discussed in this article.
Ethical approval
Study approved by Ethical committee of Clinical Center University of Sarajevo (no. 0302-19064).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sefic Pasic, I., Riera Soler, L., Vazquez Mendez, E. et al. Comparison between lung ultrasonography and chest X-ray in the evaluation of neonatal respiratory distress syndrome. J Ultrasound 26, 435–448 (2023). https://doi.org/10.1007/s40477-022-00728-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-022-00728-6