Abstract
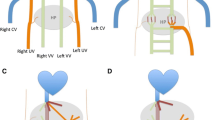
Congenital extrahepatic portosystemic shunt (CEPS), also known as Abernethy malformation, is a rare condition in which the splenomesenteric blood drains directly into a systemic vein, bypassing the liver through a complete or partial shunt. The diagnosis is frequently made during childhood in the setting of neonatal cholestasis, hypergalactosemia, failure to thrive, mental retardation or other congenital defects. In adulthood, CEPS is usually found incidentally during diagnostic work-up for abdominal pain, liver test abnormalities, liver nodules, portopulmonary hypertension, portopulmonary syndrome or portosystemic encephalopathy. The diagnosis depends on imaging and portal venography, but sometimes only liver biopsy can be resolutive, demonstrating the absence of venules within the portal areas. Here we report four recent cases of Abernethy malformation diagnosed in young adults, in which ultrasound (US) was the initial imaging technique and allowed to suspect the diagnosis. Furthermore, we reviewed clinical presentations, associated anomalies and treatment of the 310 cases of CEPS previously reported in the literature.
Sommario
Lo shunt portosistemico extraepatico congenito (CEPS), anche noto come malformazione di Abernethy, è una rara condizione patologica in cui il sangue venoso refluo dal distretto spleno-mesenterico drena direttamente nel circolo venoso sistemico, bypassando il fegato attraverso un shunt completo o parziale. La diagnosi viene posta frequentemente durante l’infanzia in presenza di colestasi neonatale, ipergalattosemia, scarso accrescimento o altri difetti congeniti. Durante l’età adulta la diagnosi di CEPS è spesso incidentale nel corso di accertamenti diagnostici per dolore addominale, alterazioni degli indici di funzionalità epatica, riscontro di lesioni focali epatiche, ipertensione porto-polmonare, sindrome porto-polmonare ed encefalopatia porto-sistemica. Le tecniche di imaging o la porto-venografia consentono solitamente di porre la diagnosi, ma in alcuni casi solo la biopsia epatica risulta dirimente, documentando l’assenza di strutture venose a livello degli spazi portali. Nel presente lavoro vengono presentati 4 casi di malformazione di Abernethy diagnosticati in giovani adulti, nei quali l’ultrasonografia (US) è stata la prima tecnica di immagine utilizzata consentendo di porre il sospetto diagnostico. Inoltre, abbiamo analizzato la presentazione clinica, le anomalie associate e le opzioni terapeutiche dei 310 casi di CEPS riportati in letteratura.




Similar content being viewed by others
References
Abernethy J (1793) Account of two instances of uncommon formation in the viscera of the human body. Phil Trans R Soc Lond B Biol Sci 83:295–299
Hao Y, Hong X, Zhao X (2015) Congenital absence of the portal vein associated with focal nodular hyperplasia of the liver and congenital heart disease (Abernethy malformation): a case report and literature review. Oncol Lett 9(2):695–700
Morgan BG, Superina R (1994) Congenital absence of the portal vein: two cases and a proposed classification system for portosystemic vascular anomalies. J Pediatr Surg 29:1239–1241
Kobayashi N, Niwa T, Kirikoshi H et al (2010) Clinical classification of congenital extrahepatic portosystemic shunts. Hepatol Res 40:585
Lautz TB, Tantemsapya N, Rowell E et al (2011) Management and classification of type II congenital portosystemic shunts. J Pediatr Surg 46(2):308–314
Kanazawa H, Nosaka S, Miyazaki O et al (2015) The classification based on intrahepatic portal system for congenital portosystemic shunts. J Pediatr Surg 50(4):688–695
Bernard O, Franchi-Abella S, Branchereau S et al (2012) Congenital portosystemic shunts in children: recognition, evaluation, and management. Semin Liver Dis 32(4):273–287
Venkat-Raman N, Murphy KW, Ghaus K et al (2001) Congenital absence of portal vein in the fetus: a case report. Ultrasound Obstet Gynecol 17:71–75
Jiang C, Ye W, Liu C et al (2015) Surgical ligation of portosystemic shunt to resolve severe hematuria and hemafecia caused by type II abernethy malformation. Ann Vasc Surg 29(5):1020.e11–1020.e16
Gong Y, Zhu H, Chen J et al (2015) Congenital portosystemic shunts with and without gastrointestinal bleeding—case series. Pediatr Radiol 45(13):1964–1971
Kalifa G, Brunelle F, Chaumont P (1978) Fistule porto-cavale congenitale. Ann Radiol 21:183–186
Morse SS, Taylor KJW, Strauss EB et al (1986) Congenital absence of the portal vein in oculoauriculovertebral dysplasia (Goldenhar syndrome). Pediatr Radiol 16:437–439
Sakamoto S, Shigeta T, Fukuda A et al (2012) The role of liver transplantation for congenital extrahepatic portosystemic shunt. Transplantation 93(12):1282–1287
Bas S, Guran T, Atay Z et al (2015) Premature pubarche, hyperinsulinemia and hypothyroxinemia: novel manifestations of congenital portosystemic shunts (Abernethy Malformation) in Children. Horm Res Paediatr 83(4):282–287
Sokollik C, Bandsma RH, Gana JC et al (2013) Congenital portosystemic shunt: characterization of a multisystem disease. J Pediatr Gastroenterol Nutr 56(6):675–681
Uchino T, Matsuda I, Endo F (1999) The long-term prognosis of congenital portosystemic venous shunt. J Pediatr 135(2 Pt 1):254–256
Ohno T, Muneuchi J, Ihara K et al (2008) Pulmonary hypertension in patients with congenital portosystemic venous shunt: a previously unrecognized association. Pediatrics 121(4):e892–e899
Ohnishi Y, Ueda M, Doi H et al (2005) Successful liver transplantation for congenital absence of the portal vein complicated by intrapulmonary shunt and brain abscess. J Pediatr Surg 40(5):E-3
Alvarez AE, Ribeiro AF, Hessel G et al (2002) Abernethy malformation: one of the etiologies of hepatopulmonary syndrome. Pediatr Pulmonol 34:391–394
Pupulim LF, Vullierme MP, Paradis V et al (2013) Congenital portosystemic shunts associated with liver tumours. Clin Radiol 68(7):e362–e369
Franchi-Abella S, Branchereau S, Lambert V et al (2010) Complications of congenital portosystemic shunts in children: therapeutic options and outcomes. J Pediatr Gastroenterol Nutr 51(3):322–330
Sorkin T, Strautnieks S, Foskett P et al (2016) Multiple β-catenin mutations in hepatocellular lesions arising in Abernethy malformation. Hum Pathol 53:153–158
Lisovsky M, Konstas AA, Misdraji J (2011) Congenital extrahepatic portosystemic shunts (Abernethy malformation): a histopathologic evaluation. Am J Surg Pathol 35(9):1381–1390
Bruckheimer E, Dagan T, Atar E et al (2013) Staged transcatheter treatment of portal hypoplasia and congenital portosystemic shunts in children. Cardiovasc Intervent Radiol 36(6):1580–1585
Kanamori Y, Hashizume K, Kitano Y et al (2003) Congenital extrahepatic portocaval shunt (Abernethy type 2), huge liver mass, and patent ductus arteriosus–a case report of its rare clinical presentation in a young girl. J Pediatr Surg 38(4):E15
Tercier S, Delarue A, Rouault F et al (2006) Congenital portocaval fistula associated with hepatopulmonary syndrome: ligation vs liver transplantation. J Pediatr Surg 41:e1
Iida T, Ogura Y, Doi H et al (2010) Successful treatment of pulmonary hypertension secondary to congenital extrahepatic portocaval shunts (Abernethy type 2) by living donor liver transplantation after surgical shunt ligation. Transpl Int 23(1):105–109
Li H, Ma Z, Xie Y et al (2017) Recurrent hyperammonemia after abernethy malformation type 2 closure: a case report. Ann Hepatol 16(3):460–464
Özden İ, Yavru A, Güllüoğlu M et al (2017) Transplantation for large liver tumors in the setting of Abernethy malformation. Exp Clin Transplant 15(Suppl 2):82–85
Benedict M, Rodriguez-Davalos M, Emre S et al (2017) Congenital extrahepatic portosystemic shunt (Abernethy malformation type Ib) with associated hepatocellular carcinoma. Pediatr Dev Pathol 20(4):354
Brasoveanu V, Ionescu MI, Grigorie R et al (2015) Living donor liver transplantation for unresectable liver adenomatosis associated with congenital absence of portal vein: a case report and literature review. Am J Case Rep. 19(16):637–644
Sanada Y, Mizuta K, Niki T et al (2015) Hepatocellular nodules resulting from congenital extrahepatic portosystemic shunts can differentiate into potentially malignant hepatocellular adenomas. J Hepatobiliary Pancreat Sci 22(10):746–756
Yilmaz C, Onen Z, Farajov R et al (2017) Live donor liver transplantation for a child presented with severe hepatopulmonary syndrome and nodular liver lesions due to Abernethy malformation. Pediatr Transplant. 21(2):e12874
Murray CP, Yoo SJ, Babyn PS (2003) Congenital extrahepatic portosystemic shunts. Pediatr Radiol 33(9):614–620
Ringe K, Schirg E, Melter M et al (2008) Congenital absence of the portal vein (CAPV). Two cases of Abernethy malformation type 1 and review of the literature (in German). Radiologe 48:493–502
Stewart JK, Kuo WT, Hovsepian DM et al (2011) Portal venous remodeling after endovascular reduction of pediatric autogenous portosystemic shunts. J Vasc Interv Radiol 22(8):1199–1205
Mistinova J, Valacsai F, Varga I (2010) Congenital absence of the portal vein–Case report and a review of literature. Clin Anat 23(7):750–758
Athanasiadis A, Karavida A, Chondromatidou S et al (2015) Prenatal diagnosis of Abernethy malformation by three-dimensional ultrasonography. Ultrasound Obstet Gynecol 46(5):638–639
Mi XX, Li XG, Wang ZR et al (2017) Abernethy malformation associated with Caroli’s syndrome in a patient with a PKHD1 mutation: a case report. Diagn Pathol 12(1):61
Draghi F, Rapaccini GL, Fachinetti C et al (2007) Ultrasound examination of the liver: normal vascular anatomy. J Ultrasound 10(1):5–11
Battaglia S, Fachinetti C, Draghi F et al (2010) Ultrasound examination of the liver: variations in the vascular anatomy. J Ultrasound 13(2):49–56
Puccia F, Lombardo V, Giannitrapani L et al (2017) Case report: acute portal vein thrombosis associated with acute cytomegalovirus infection in an immunocompetent adult. J Ultrasound 20(2):161–165
Ricci P, Cantisani V, Biancari F, Drud FM et al (2000) Contrast-enhanced color Doppler US in malignant portal vein thrombosis. Acta Radiol 41(5):470–473
Sidhu PS, Cantisani V, Deganello A et al (2017) Role of contrast-enhanced ultrasound (CEUS) in paediatric practice: an EFSUMB position statement. Ultraschall Med 38(1):33–43
Hwang M, Thimm MA, Guerrerio AL (2018) Detection of cavernous transformation of the portal vein by contrast-enhanced ultrasound. J Ultrasound 21(2):153–157
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Informed consent
Informed consent was obtained from participants included in the study.
Rights and permissions
About this article
Cite this article
Ponziani, F.R., Faccia, M., Zocco, M.A. et al. Congenital extrahepatic portosystemic shunt: description of four cases and review of the literature. J Ultrasound 22, 349–358 (2019). https://doi.org/10.1007/s40477-018-0329-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40477-018-0329-y