Abstract
Background
It is recognized that low oestrogen status impairs the skeletal response to mechanical loading in elderly women; therefore, oestrogen administration is expected to increase the osteogenic response to mechanical strain.
Objectives
This meta-analysis aimed to evaluate the combined effects of hormone replacement therapy (HRT) and exercise on femoral neck and lumbar spine bone mineral density (BMD) in postmenopausal women, in comparison with the effects of exercise-only intervention.
Methods
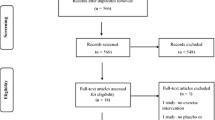
A systematic literature search was conducted in PubMed, Embase, SPORTDiscus and ProQuest up to May 1, 2014, to ascertain the influence of oestrogen administration and exercise on BMD in postmenopausal women. The study quality and potential publication bias of the included trials were evaluated. The primary end point was the change in BMD from baseline to follow-up. The effect sizes were estimated in terms of the standardized mean difference (SMD). Subgroup analysis was conducted on the basis of exercise categories.
Results
Six studies with a total of 764 postmenopausal women (aged between 51.8 ± 2.9 and 68.0 ± 3.0 years) met the inclusion criteria. The included studies had low and high levels of heterogeneity of hip outcomes (I 2 = 0.0 %) and spine outcomes (I 2 = 80.8 %), respectively. Fixed- and random-effects models were used for calculating the effect size estimates. The pooled effect sizes associated with the combined interventions of HRT and exercise were significant for femoral neck BMD (SMD 0.220, 95 % confidence interval [CI] 0.011–0.429, p = 0.039) and lumbar spine BMD (SMD 0.729, 95 % CI 0.186–1.273, p = 0.009) in comparison with the exercise-only intervention. The mixed loading exercise programmes were sensitive to HRT in preventing postmenopausal bone loss in the spine (SMD 1.073, 95 % CI 0.140–2.005, p = 0.024) in comparison with single-mode exercise.
Conclusions
Our findings indicate that oestrogen treatment significantly increases the skeletal response to exercise training in both the hips and the spine in postmenopausal women, which implies that the combination of oestrogen administration and exercise may generate greater effects.





Similar content being viewed by others
References
Lorrain J, Paiement G, Chevrier N, et al. Population demographics and socioeconomic impact of osteoporotic fractures in Canada. Menopause. 2003;10(3):228–34.
Kelley GA, Kelley KS, Kohrt WM. Effects of ground and joint reaction force exercise on lumbar spine and femoral neck bone mineral density in postmenopausal women: a meta-analysis of randomized controlled trials. BMC Musculoskelet Disord. 2012;13:177.
Martyn-St James M, Carroll S. A meta-analysis of impact exercise on postmenopausal bone loss: the case for mixed loading exercise programmes. Br J Sports Med. 2009;43(12):898–908.
Kemmler W, Bebenek M, von Stengel S, et al. Effect of block-periodized exercise training on bone and coronary heart disease risk factors in early post-menopausal women: a randomized controlled study. Scand J Med Sci Sports. 2013;23(1):121–9.
Martyn-St James M, Carroll S. Meta-analysis of walking for preservation of bone mineral density in postmenopausal women. Bone. 2008;43(3):521–31.
Schmitt NM, Schmitt J, Doren M. The role of physical activity in the prevention of osteoporosis in postmenopausal women—an update. Maturitas. 2009;63(1):34–8.
Kemmler W, Engelke K, Weineck J, et al. The Erlangen Fitness Osteoporosis Prevention Study: a controlled exercise trial in early postmenopausal women with low bone density—first-year results. Arch Phys Med Rehabil. 2003;84(5):673–82.
Martyn-St James M, Carroll S. High-intensity resistance training and postmenopausal bone loss: a meta-analysis. Osteoporos Int. 2006;17(8):1225–40.
Snow CM, Shaw JM, Winters KM, et al. Long-term exercise using weighted vests prevents hip bone loss in postmenopausal women. J Gerontol A Biol Sci Med Sci. 2000;55(9):M489–91.
Rhodes EC, Martin AD, Taunton JE, et al. Effects of one year of resistance training on the relation between muscular strength and bone density in elderly women. Br J Sports Med. 2000;34(1):18–22.
Lanyon LE. Using functional loading to influence bone mass and architecture: objectives, mechanisms, and relationship with estrogen of the mechanically adaptive process in bone. Bone. 1996;18(1 Suppl.):37S–43S.
Lee K, Jessop H, Suswillo R, et al. Endocrinology: bone adaptation requires oestrogen receptor-alpha. Nature. 2003;424(6947):389.
Tobias JH. At the crossroads of skeletal responses to estrogen and exercise. Trends Endocrinol Metab. 2003;14(10):441–3.
Ankrom MA, Patterson JA, d’Avis PY, et al. Age-related changes in human oestrogen receptor alpha function and levels in osteoblasts. Biochem J. 1998;333(Pt 3):787–94.
Hahn S, Williamson PR, Hutton JL, et al. Assessing the potential for bias in meta-analysis due to selective reporting of subgroup analyses within studies. Stat Med. 2000;19(24):3325–36.
Damien E, Price JS, Lanyon LE. The estrogen receptor’s involvement in osteoblasts’ adaptive response to mechanical strain. J Bone Miner Res. 1998;13(8):1275–82.
Wu J, Wang X, Chiba H, et al. Combined intervention of soy isoflavone and moderate exercise prevents body fat elevation and bone loss in ovariectomized mice. Metabolism. 2004;53(7):942–8.
Wu J, Wang XX, Takasaki M, et al. Cooperative effects of exercise training and genistein administration on bone mass in ovariectomized mice. J Bone Miner Res. 2001;16(10):1829–36.
Bassey EJ, Rothwell MC, Littlewood JJ, et al. Pre- and postmenopausal women have different bone mineral density responses to the same high-impact exercise. J Bone Miner Res. 1998;13(12):1805–13.
Going S, Lohman T, Houtkooper L, et al. Effects of exercise on bone mineral density in calcium-replete postmenopausal women with and without hormone replacement therapy. Osteoporos Int. 2003;14(8):637–43.
Kohrt WM, Snead DB, Slatopolsky E, et al. Additive effects of weight-bearing exercise and estrogen on bone mineral density in older women. J Bone Miner Res. 1995;10(9):1303–11.
Kohrt WM, Ehsani AA, Birge SJ Jr. HRT preserves increases in bone mineral density and reductions in body fat after a supervised exercise program. J Appl Physiol (1985). 1998;84(5):1506–12.
Maddalozzo GF, Widrick JJ, Cardinal BJ, et al. The effects of hormone replacement therapy and resistance training on spine bone mineral density in early postmenopausal women. Bone. 2007;40(5):1244–51.
Milliken LA, Going SB, Houtkooper LB, et al. Effects of exercise training on bone remodeling, insulin-like growth factors, and bone mineral density in postmenopausal women with and without hormone replacement therapy. Calcif Tissue Int. 2003;72(4):478–84.
Moher D, Liberati A, Tetzlaff J, et al. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151(4):264–9, W64.
Higgins J, Green S. Cochrane reviewers’ handbook 5.0.1 (updated September 2008). Chichester: Wiley; 2008.
Jadad AR, Moore RA, Carroll D, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17(1):1–12.
Rossouw JE, Anderson GL, Prentice RL, et al. Risks and benefits of estrogen plus progestin in healthy postmenopausal women: principal results from the Women’s Health Initiative randomized controlled trial. JAMA. 2002;288(3):321–33.
Anderson GL, Limacher M, Assaf AR, et al. Effects of conjugated equine estrogen in postmenopausal women with hysterectomy: the Women’s Health Initiative randomized controlled trial. JAMA. 2004;291(14):1701–12.
Banks E, Canfell K. Invited commentary: hormone therapy risks and benefits—the Women’s Health Initiative findings and the postmenopausal estrogen timing hypothesis. Am J Epidemiol. 2009;170(1):24–8.
Gurney EP, Nachtigall MJ, Nachtigall LE, et al. The Women’s Health Initiative trial and related studies: 10 years later. A clinician’s view. J Steroid Biochem Mol Biol. 2014;142:4–11.
Zhang J, Gao R, Cao P, et al. Additive effects of antiresorptive agents and exercise on lumbar spine bone mineral density in adults with low bone mass: a meta-analysis. Osteoporos Int. 2014;25(5):1585–94.
El-Khoury F, Cassou B, Charles MA, et al. The effect of fall prevention exercise programmes on fall induced injuries in community dwelling older adults: systematic review and meta-analysis of randomised controlled trials. BMJ. 2013;347:f6234.
Karinkanta S, Piirtola M, Sievanen H, et al. Physical therapy approaches to reduce fall and fracture risk among older adults. Nat Rev Endocrinol. 2010;6(7):396–407.
Cummings SR, Black DM, Nevitt MC, et al. Bone density at various sites for prediction of hip fractures. The Study of Osteoporotic Fractures Research Group. Lancet. 1993;341(8837):72–5.
Borer KT. Physical activity in the prevention and amelioration of osteoporosis in women: interaction of mechanical, hormonal and dietary factors. Sports Med. 2005;35(9):779–830.
Rubin CT, McLeod KJ. Promotion of bony ingrowth by frequency-specific, low-amplitude mechanical strain. Clin Orthop Relat Res. 1994;298:165–74.
Pildal J, Hrobjartsson A, Jorgensen KJ, et al. Impact of allocation concealment on conclusions drawn from meta-analyses of randomized trials. Int J Epidemiol. 2007;36(4):847–57.
Wood L, Egger M, Gluud LL, et al. Empirical evidence of bias in treatment effect estimates in controlled trials with different interventions and outcomes: meta-epidemiological study. BMJ. 2008;336(7644):601–5.
Ammann P, Rizzoli R. Bone strength and its determinants. Osteoporos Int. 2003;14(Suppl. 3):S13–8.
Acknowledgments
This analysis was based upon work funded by the Zhejiang Provincial Natural Science Foundation of China under Grant No. LY14H070001. The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Zhao, R., Xu, Z. & Zhao, M. Effects of Oestrogen Treatment on Skeletal Response to Exercise in the Hips and Spine in Postmenopausal Women: A Meta-Analysis. Sports Med 45, 1163–1173 (2015). https://doi.org/10.1007/s40279-015-0338-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40279-015-0338-3