Abstract
Background
Evidence on the socioeconomic burden associated with childhood visual impairment, severe visual impairment and blindness (VI/SVI/BL) is needed to inform economic evaluations of existing and emerging interventions aimed at protecting or improving vision. This study aimed to evaluate the quantity and quality of literature on resource use and/or costs associated with childhood VI/SVI/BL disorders.
Methods
PubMed, Web of Science (Ovid), the National Health Service (NHS) Economic Evaluation Database and grey literature were searched in November 2020. The PubMed search was rerun in February 2022. Original articles reporting unique estimates of resource use or cost data on conditions resulting in bilateral VI/SVI/BL were eligible for data extraction. Quality assessment (QA) was undertaken using the Drummond checklist adapted for cost-of-illness (COI) studies.
Results
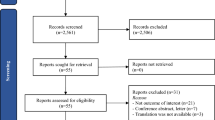
We identified 31 eligible articles, 27 from the peer-reviewed literature and four from the grey literature. Two reported on resource use, and 29 reported on costs. Cerebral visual impairment and optic nerve disorders were not examined in any included studies, whereas retinopathy of prematurity was the most frequently examined condition. The quality of studies varied, with economic evaluations having higher mean QA scores (82%) compared to COI studies (77%). Deficiencies in reporting were seen, particularly in the clinical definitions of conditions in economic evaluations and a lack of discounting and sensitivity analyses in COI studies.
Conclusions
There is sparse literature on resource use or costs associated with childhood visual impairment disorders. The first step in addressing this important evidence gap is to ensure core visual impairment outcomes are measured in future randomised control trials of interventions as well as cohort studies and are reported as a discrete health outcome.


Similar content being viewed by others
Data availability statement
All articles and grey literature can be found using the respective search strategies in supplementary file 1. All data supporting the findings of this study are available within the paper. Quality assessment scores for individual studies are available from the corresponding author on request.
References
Teoh LJ, Solebo AL, Rahi JS, Morton C, Allen L, McPhee D, et al. Visual impairment, severe visual impairment, and blindness in children in Britain (BCVIS2): a national observational study. Lancet Child Adolesc Health [Internet]. 2021;5:190–200.
NICE health technology evaluations: the manual (PMG36). 2022.
Burton MJ, Ramke J, Marques AP, Bourne RRA, Congdon N, Jones I, et al. The Lancet Global Health Commission on global eye health: vision beyond 2020. Lancet Glob Health [Internet]. 2021;9:e489-551.
Cost effectiveness of eye health treatments—The International Agency for the Prevention of Blindness [Internet]. https://www.iapb.org/learn/vision-atlas/solutions/cost-effectiveness/. Accessed 15 Dec 2021.
Moher D, Shamseer L, Clarke M, Ghersi D, Liberati A, Petticrew M, et al. Preferred reporting items for systematic review and meta-analysis protocols (PRISMA-P) 2015 statement. Revista Espanola de Nutricion Humana y Dietetica [Internet]. 2016;20:148–60. https://doi.org/10.1186/2046-4053-4-1.
Liberati A, Altman DG, Tetzlaff J, Mulrow C, Gøtzsche PC, Ioannidis JPA, et al. The PRISMA statement for reporting systematic reviews and meta-analyses of studies that evaluate healthcare interventions: explanation and elaboration. BMJ. 2009;339:2700.
Boluyt N, Tjosvold L, Lefebvre C, Klassen TP, Offringa M. Usefulness of systematic review search strategies in finding child health systematic reviews in MEDLINE. Arch Pediatr Adolesc Med. 2008;162:111–6.
Veritas Health Innovation M. Covidence systematic review software [Internet]. www.covidence.org. Accessed 29 May 2020.
World Health Organization. ICD-10 : international statistical classification of diseases and related health problems : tenth revision, 2nd ed. World Health Organization. [Internet]. 2004. https://apps.who.int/iris/handle/10665/42980. Accessed 29 May 2020.
Molinier L, Bauvin E, Combescure C, Castelli C, Rebillard X, Soulié M, et al. Methodological considerations in cost of prostate cancer studies: a systematic review. Value Health. 2008;11:878–85.
Figure 15.5.a: Drummond checklist [Internet]. https://handbook-5-1.cochrane.org/chapter_15/figure_15_5_a_drummond_checklist_drummond_1996.htm. Accessed 29 May 2020.
Campbell M, McKenzie JE, Sowden A, Katikireddi SV, Brennan SE, Ellis S, et al. Synthesis without meta-analysis (SWiM) in systematic reviews: reporting guideline. BMJ [Internet]. 2020. https://doi.org/10.1136/bmj.l6890.
Prices-Inflation (CPI)—OECD Data [Internet]. https://data.oecd.org/price/inflation-cpi.htm. Accessed 25 Aug 2020.
Conversion rates—Purchasing power parities (PPP)—OECD Data [Internet]. https://data.oecd.org/conversion/purchasing-power-parities-ppp.htm. Accessed 25 Aug 2020.
Honeycutt AA, Grosse SD, Dunlap LJ, Schendel DE, Chen H, Brann E, et al. Economic costs of mental retardation, cerebral palsy, hearing loss, and vision impairment. Research in Social Science and Disability. Bingley: Emerald Group Publishing Limited; 2003. p. 207–28.
Socioeconomic impact of low vision and blindness from paediatric eye disease in Australia Save Sight Institute The University of Sydney. 2016. Report prepared by Deloitte Access Economics [Internet]. https://www.deloitte.com/au/en/services/economics/analysis/socioeconomic-impact-low-vision-blindness-paediatric-eye-disease-australia.html
Guide Dogs for the Blind Association. The costs of blindness: an analysis of the costs of visual impairment and blindness in the United Kingdom [Internet]. https://publications.parliament.uk/pa/cm200203/cmhansrd/vo031119/text/31119w67.htm. Accessed 11 November 2020.
Wittenborn J, Rein D. Cost of vision problems: the Economic Burden of Vision Loss and Eye Disorders in the United States. NORC. University of Chicago; 2013.
Zin AA, Magluta C, Pinto MF, Entringer AP, Mendes-Gomes MA, Moreira ME, et al. Retinopathy of prematurity screening and treatment cost in Brazil. Rev Panam Salud Publica [Internet]. 2014;36:37–43.
Stillwaggon E, Carrier CS, Sautter M, McLeod R. Maternal serologic screening to prevent congenital toxoplasmosis: a decision-analytic economic model. PLoS Negl Trop Dis. 2011;5: e1333.
Noble J, Hollands H, Forooghian F, Yazdani A, Sharma S, et al. Evaluating the cost-effectiveness of anterior uveitis investigation by Canadian ophthalmologists. Can J Ophthalmol [Internet]. 2008;43:652–7.
Cernat A, Jamieson M, Kavelaars R, Khalili S, Bhambhwani V, Mireskandari K, et al. Immediate versus delayed sequential bilateral cataract surgery in children: a cost-effectiveness analysis. Br J Ophthalmol [Internet]. 2022;106:211–7.
Prusa A, Kasper DC, Sawers L, Walter E, Hayde M, Stillwaggon E. Congenital toxoplasmosis in Austria: prenatal screening for prevention is cost-saving. PLoS Negl Trop Dis [Internet]. 2017;11: e0005648.
Dave H. Simultaneous vs sequential bilateral cataract surgery for infants with congenital cataracts. Arch Ophthalmol [Internet]. 2010;128:1050. https://doi.org/10.1001/archophthalmol.2010.136.
Minden K, Niewerth M, Listing J, Möbius D, Thon A, Ganser G, et al. The economic burden of juvenile idiopathic arthritis—results from the German paediatric rheumatologic database. Clin Exp Rheumatol. 2009;27:863–9.
Dave H, Gordillo L, Yang Z, Zhang MS, Hubbard GB, Olsen TW. The societal burden of blindness secondary to retinopathy of prematurity in Lima, Peru. Am J Ophthalmol [Internet]. 2012;154:750–5.
Korvenranta E, Lehtonen L, Rautava L, Häkkinen U, Andersson S, Gissler M, et al. Impact of very preterm birth on health care costs at five years of age. Pediatrics. 2010;125:e1109–14.
Wang J, Jin L, Lu Q, Botah RR, Ali R, Li J, et al. Barriers, costs, and attitudes toward pediatric cataract surgery at two large facilities in China and India. Ophthalmic Epidemiol [Internet]. 2019;26:47–54. https://doi.org/10.1080/09286586.2018.1513043?needAccess=true.
Anderzén-Carlsson A. CHARGE Syndrome-a five case study of the syndrome characteristics and health care consumption during the first year in life. J Pediatr Nurs [Internet]. 2015;30:6–16.
O’Connor PM, Chou S-L, Lamoureux EL, Keeffe JE. Costs of vision impairment in childhood and youth: diary case studies. Optom Vis Sci [Internet]. 2008;85:1106–9.
Wright SE, Keeffe JE, Thies LS. Direct costs of blindness in Australia. Clin Exp Ophthalmol [Internet]. 2000;28:140–2. https://doi.org/10.1046/j.1442-9071.2000.00296.x?download=true.
Rahi JS, Cable N. Severe visual impairment and blindness in children in the UK. Lancet [Internet]. 2003;362:1359–65.
Rothschild MI, Russ R, Brennan KA, Williams CJ, Berrones D, Patel B, et al. The economic model of retinopathy of prematurity (EcROP) screening and treatment: Mexico and the United States. Am J Ophthalmol [Internet]. 2016;168:110–21.
Dunbar JA, Hsu V, Christensen M, Black B, Williams P, Beauchamp G. Cost-utility analysis of screening and laser treatment of retinopathy of prematurity. J Am Assoc Pediatr Ophthalmol Strabismus. 2009;13:186–90.
Roberts T, Frenkel JK. Estimating income losses and other preventable costs caused by congenital toxoplasmosis in people in the United States. J Am Vet Med Assoc. 1990;196:249–56.
Liu D, Huang L, Mukkamala L, Khouri AS. The economic burden of childhood glaucoma. J Glaucoma [Internet]. 2016;25:790–7.
Wittenborn JS, Zhang X, Feagan CW, Crouse WL, Shrestha S, Kemper AR, et al. The economic burden of vision loss and eye disorders among the united states population younger than 40 years. Ophthalmology. 2013;120:1728–35.
Naguib MM, Soares RR, Anzures R, Kamel J, Chandrasekar EK, Rothschild M, et al. Regionally specific economic impact of screening and treating retinopathy of prematurity in middle-income societies in the Philippines. J Pediatr Ophthalmol Strabismus [Internet]. 2019;56:388–96.
Rothschild MI, Russ R, Brennan KA, Williams CJ, Berrones D, Patel B, et al. The economic model of retinopathy of prematurity (EcROP) screening and treatment: Mexico and the United States. Am J Ophthalmol. 2016;168:110–21.
Shamanna B, Dandona L, Rao GN. Economic burden of blindness in India. Indian J Ophthalmol [Internet]. 1998;46:169–72.
Javitt J, Cas RD, Chiang YP. Cost-effectiveness of screening and cryotherapy for threshold retinopathy of prematurity. Pediatrics [Internet]. 1993;91:859–66.
Korvenranta E, Lehtonen L, Rautava L, Häkkinen U, Andersson S, Gissler M, et al. Impact of very preterm birth on health care costs at five years of age. Pediatrics [Internet]. 2010;125:e1109–14.
Jackson KM, Scott KE, Zivin JG, Bateman DA, Flynn JT, Keenan JD, et al. Cost-utility analysis of telemedicine and ophthalmoscopy for retinopathy of prematurity management. Arch Ophthalmol [Internet]. 2008;126:493–9.
Liu D, Huang L, Mukkamala L, Khouri AS. The economic burden of childhood glaucoma. J Glaucoma. 2016;25:790–7.
Brown GC, Brown MM, Sharma S, Tasman W, Brown HC. Cost-effectiveness of treatment for threshold retinopathy of prematurity. Pediatrics [Internet]. 1999;104:e47.
Jackson KM, Scott KE, Graff Zivin J, Bateman DA, Flynn JT, Keenan JDCMF. Cost-utility analysis of telemedicine and ophthalmoscopy for retinopathy of prematurity management. Arch Ophthalmol [Internet]. 2008;126:4–493.
Kamholz KL, Cole CH, Gray JE, Zupancic JAF. Cost-effectiveness of early treatment for retinopathy of prematurity. Pediatrics [Internet]. 2009;123:262–9.
Hughes DA, Culeddu G, Plumpton CO, Wood E, Dick AD, Jones AP, et al. Cost-effectiveness analysis of adalimumab for the treatment of uveitis associated with juvenile idiopathic arthritis. Ophthalmology [Internet]. 2019;126:415–24.
Lyons CJ, Lambert SR, Taylor D, Hoyt CS. Taylor and Hoyt’s Pediatric Ophthalmology and Strabismus. 6th edition. 2022. ISBN: 9780702082986.
Adams J, Hillier-Brown FC, Moore HJ, Lake AA, Araujo-Soares V, White M, et al. Searching and synthesising ‘grey literature’ and ‘grey information’ in public health: critical reflections on three case studies. Syst Rev. 2016;5:164.
Higgins JPT, Thomas J, Chandler J, Cumpston M, Li T, Page MJ WV (editors). Cochrane Handbook for Systematic Reviews of Interventions [Internet]. 6.2. 2021. https://handbook-5-1.cochrane.org/chapter_15/15_6_3_meta_analysis_of_resource_use_and_cost_data.htm. Accessed 31 Jan 2022.
Meads C, Hyde C. What is the cost of blindness? [Internet]. Br J Ophthalmol. 2003;87:1201–4.
Rowen D, Rivero-Arias O, Devlin N, Ratcliffe J. Review of Valuation Methods of Preference-Based Measures of Health for Economic Evaluation in Child and Adolescent Populations: Where are We Now and Where are We Going? Pharmacoeconomics [Internet]. 2020;38:325–40. https://doi.org/10.1007/s40273-019-00873-7.
Ramanan AV, Dick AD, Jones AP, McKay A, Williamson PR, Compeyrot-Lacassagne S, et al. Adalimumab plus methotrexate for uveitis in juvenile idiopathic arthritis. N Engl J Med. 2017;376:1637–46.
Russell S, Bennett J, Wellman JA, Chung DC, Yu ZF, Tillman A, et al. Efficacy and safety of voretigene neparvovec (AAV2-hRPE65v2) in patients with RPE65-mediated inherited retinal dystrophy: a randomised, controlled, open-label, phase 3 trial. Lancet [Internet]. 2017;390:849–60.
Zimmermann MR, Lubinga SJ, Rind D, Chapman RH, Carlson JJ. A cost-effectiveness analysis of voretigene neparvovec for vision loss due to biallelic Rpe65-mediated inherited retinal disease. Value Health. 2018;21:S205–6.
Viriato D, Bennett N, Sidhu R, Hancock E, Lomax H, Trueman D, et al. An economic evaluation of voretigene neparvovec for the treatment of biallelic RPE65-mediated inherited retinal dystrophies in the UK. Adv Ther. 2020;37:1233–47.
Dale NJ, Sakkalou E, O’Reilly MA, Springall C, Sakki H, Glew S, et al. Home-based early intervention in infants and young children with visual impairment using the Developmental Journal: longitudinal cohort study. Dev Med Child Neurol [Internet]. 2019;61:697–709.
Silveira S, Martin FJ, Flaherty M, Russell HC. Reporting on Australian childhood visual impairment: the first 10 years. Eye. 2022;36:1412–8.
Chong CF, McGhee CNJ, Dai SH. Causes of childhood low vision and blindness in New Zealand. Clin Exp Ophthalmol [Internet]. 2019;47:165–70.
Delay A, Rice M, Bush E, Harpster K. Interventions for children with cerebral visual impairment: a scoping review. Dev Med Child Neurol. 2022;65:469–78.
Jacobs SE, Berg M, Hunt R, Tarnow-Mordi WO, Inder TE, Davis PG. Cooling for newborns with hypoxic ischaemic encephalopathy. Cochrane Database of Syst Rev. 2013. https://doi.org/10.1002/14651858.CD003311.pub3.
Juul SE, Comstock BA, Wadhawan R, Mayock DE, Courtney SE, Robinson T, et al. A randomized trial of erythropoietin for neuroprotection in preterm infants. N Engl J Med. 2020;382:233–43.
Akisu M, Huseyinov A, Yalaz M, Cetin H, Kultursay N. Selective head cooling with hypothermia suppresses the generation of platelet-activating factor in cerebrospinal fluid of newborn infants with perinatal asphyxia. Prostaglandins Leukot Essent Fatty Acids. 2003;69:45–50.
Shankaran S, Laptook A, Wright LL, Ehrenkranz RA, Donovan EF, Fanaroff AA, et al. Whole-body hypothermia for neonatal encephalopathy: animal observations as a basis for a randomized, controlled pilot study in term infants. Pediatrics. 2002;110:377–85.
Zhou WH, Cheng GQ, Shao XM, Liu XZ, Shan RB, Zhuang DY, et al. Selective head cooling with mild systemic hypothermia after neonatal hypoxic-ischemic encephalopathy: a multicenter randomized controlled trial in China. J Pediatr [Internet]. 2010;157:367–72 (372.e1-3).
Marques AP, Ramke J, Cairns J, Butt T, Zhang JH, Jones I, et al. The economics of vision impairment and its leading causes: a systematic review. EClinicalMedicine. 2022;46: 101354.
Smith AF, Sadeq A, Kinzel E, Bhambhwani V. A Systematic Review of Economic Evaluations Conducted for Interventions to Screen, Treat, and Manage Retinopathy of Prematurity (ROP) in the United States, United Kingdom, and Canada. Ophthalmic Epidemiol [Internet]. 2022. https://doi.org/10.1080/09286586.2022.2084757.
Ungar WJ, Gerber A. The uniqueness of child health and challenges to measuring costs and consequences. Economic evaluation in child health. Oxford: Oxford University Press; 2010.
World Health Organization (WHO). ICD-11: Vision impairment including blindness [Internet]. http://id.who.int/icd/entity/1103667651. Accessed 5 Oct 2020.
Acknowledgment
For the purpose of open access, the author has applied a Creative Commons Attribution (CC BY) licence to any Author Accepted Manuscript version arising.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
LJT is funded by the Medical Research Council University College London Doctoral Training Programme, the grant that supported this work: MR/N013867/1. ALS is supported by a National Institute for Health Research (NIHR) Clinician Scientist grant (grant number CS-2018-18-ST2-005). ALS and JSR are supported by the NIHR Biomedical Research Centres at Moorfields Eye Hospital/University College London Institute of Ophthalmology. JSR is an NIHR Senior Investigator. DEP is funded by an NIHR Advanced Fellowship (NIHR300054). All research at Great Ormond Street Hospital NHS Foundation Trust and University College London Great Ormond Street Institute of Child Health is made possible by the NIHR Great Ormond Street Hospital Biomedical Research Centre.
Conflict of interest
All authors declare no conflicts of interest.
Author contributions
LJT conceptualised the article, performed the literature search, screened all articles, extracted data and drafted the original manuscript. DEP and SK screened articles, extracted data and critically revised the manuscript. MCB supervised data visualisation and critically appraised the manuscript. ALS and JSR provided supervision on all aspects and critically appraised the manuscript. All authors approved the final manuscript.
Ethics approval
This study did not require research ethics approval.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Teoh, L.J., Kellett, S., Patel, D.E. et al. Evaluating the Quantity and Quality of Health Economic Literature in Blinding Childhood Disorders: A Systematic Literature Review. PharmacoEconomics 42, 275–299 (2024). https://doi.org/10.1007/s40273-023-01311-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-023-01311-5