Abstract
Background
Dipeptidyl peptidase-4 (DPP-4) inhibitors are a new class of antidiabetic drugs used for treating type 2 diabetes mellitus. While many studies have reported on the cost-effectiveness of DPP-4 inhibitors for treating type 2 diabetes, a systematic review of economic evaluations of DPP-4 inhibitors is currently lacking.
Objectives
The aim of this systematic review was to assess the cost effectiveness of DPP-4 inhibitors for patients with type 2 diabetes.
Data Sources
MEDLINE, EMBASE, National Health Service Economic Evaluation Database (NHS EED), Web of Science, EconLit databases, and the Cochrane Library were searched in November 2013.
Study Eligibility Criteria, Participants and Interventions
Studies assessing the cost effectiveness of DPP-4 inhibitors for type 2 diabetes were eligible for analysis. DPP-4 inhibitor monotherapy or combinations with other antidiabetic agents were included in the review. The DPP-4 inhibitors were all marketed drugs. Two reviewers independently reviewed titles, abstracts, and articles sequentially to select studies for data abstraction based on the inclusion and exclusion criteria. Disagreements were resolved by consensus.
Study Appraisal and Synthesis Methods
The quality of included studies was assessed according to the 24-item checklist of the Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. The costs reported by the included studies were converted to US dollars via purchasing power parities (PPP) in the year 2013 using the CCEMG–EPPI-Center Cost Converter.
Results
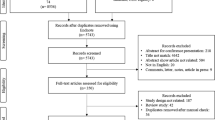
A total of 11 published studies were selected for inclusion; all were cost-utility analyses. Nine studies were conducted from a payer perspective and one used a societal perspective; however, the perspective of the other study was unclear. Four studies were of good quality, six were of moderate quality, and one was of low quality. Of the seven studies comparing DPP-4 inhibitors plus metformin with sulfonylureas plus metformin, six concluded that DPP-4 inhibitors were cost effective in patients with type 2 diabetes who were no longer adequately controlled by metformin monotherapy. Five studies compared DPP-4 inhibitors with thiazolidinediones, and whether DPP-4 inhibitors were cost effective was uncertain. Only two economic evaluations provided data to compare DPP-4 inhibitors versus insulin, and the results favored the use of DPP-4 inhibitors as second-line therapy.
Limitations
Synthesis of the data was impossible because of heterogeneity in the methodology and data sources of the economic evaluations, and the inclusion criteria excluded conference abstracts. It was difficult to find reliable weightings for each of the items of the CHEERS checklist, and the ratings were dichotomous.
Conclusions and Implications of Key Findings
This study provides the first systematic evaluation of DPP-4 inhibitors for patients with type 2 diabetes. It found that, in patients with type 2 diabetes who do not achieve glycemic targets with antidiabetic monotherapy, DPP-4 inhibitors as add-on treatment may represent a cost-effective option compared with sulfonylureas and insulin. However, high-quality cost-effectiveness analyses that utilize long-term follow-up data and have no conflicts of interest are still needed.

Similar content being viewed by others
References
World Health Organization. Diabetes programme, 2013. Available at: http://www.who.int/diabetes/en/. Accessed 20 Nov 2013.
Danaei G, Finucane MM, Lu Y, Singh GM, Cowan MJ, Paciorek CJ, et al. National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2.7 million participants. Lancet. 2011;378(9785):31–40.
World Health Organization. Global status report on noncommunicable diseases, 2010. Available at: http://www.who.int/nmh/publications/ncd_report2010/en/. Accessed 20 Nov 2013.
Zhang P, Zhang X, Brown J, Vistisen D, Sicree R, Shaw J, et al. Global healthcare expenditure on diabetes for 2010 and 2030. Diabetes Res Clin Pract. 2010;87(3):293–301.
van Dieren S, Beulens JW, van der Schouw YT, Grobbee DE, Neal B. The global burden of diabetes and its complications: an emerging pandemic. Eur J Cardiovasc Prev Rehabil. 2010;17(Suppl 1):S3–8.
Aas AM, Ohrvik J, Malmberg K, Ryden L, Birkeland KI, DIGAMI 2 Investigators. Insulin-induced weight gain and cardiovascular events in patients with type 2 diabetes. A report from the DIGAMI 2 study. Diabetes Obes Metab. 2009;11(4):323–9.
Ganz ML, Wintfeld NS, Li Q, Lee YC, Gatt E, Huang JC. Severe hypoglycemia rates and associated costs among type 2 diabetics starting basal insulin therapy in the United States. Curr Med Res Opin. 2014;30(10):1991–2000.
Hirst JA, Farmer AJ, Dyar A, Lung TW, Stevens RJ. Estimating the effect of sulfonylurea on HbA1c in diabetes: a systematic review and meta-analysis. Diabetologia. 2013;56(5):973–84.
Wallia A, Molitch ME. Insulin therapy for type 2 diabetes mellitus. JAMA. 2014;311(22):2315–25.
Roumie CL, Hung AM, Greevy RA, Grijalva CG, Liu X, Murff HJ, et al. Comparative effectiveness of sulfonylurea and metformin monotherapy on cardiovascular events in type 2 diabetes mellitus: a cohort study. Ann Intern Med. 2012;157(9):601–10.
Zoungas S, Patel A, Chalmers J, de Galan BE, Li Q, Billot L, et al. Severe hypoglycemia and risks of vascular events and death. New Engl J Med. 2010;363(15):1410–8.
Davidson MH. Potential impact of dipeptidyl peptidase-4 inhibitors on cardiovascular pathophysiology in type 2 diabetes mellitus. Postgrad Med. 2014;126(3):56–65.
Esposito K, Chiodini P, Maiorino MI, Bellastella G, Capuano A, Giugliano D. Glycaemic durability with dipeptidyl peptidase-4 inhibitors in type 2 diabetes: a systematic review and meta-analysis of long-term randomised controlled trials. BMJ Open. 2014;4(6):e005442.
Wong HK, Ong KL, Cheung CL, Cheung BM. Utilization of glucose, blood pressure, and lipid lowering medications among people with type II diabetes in the United States, 1999–2010. Ann Epidemiol. 2014;24(7):516–21.e1.
Moher D, Liberati A, Tetzlaff J, Altman DG; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151(4):264–9, W64.
Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D, et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS)—explanation and elaboration: a report of the ISPOR Health Economic Evaluation Publication Guidelines Good Reporting Practices Task Force. Value Health. 2013;16(2):231–50.
Husereau D, Drummond M, Petrou S, Carswell C, Moher D, Greenberg D, et al. Consolidated Health Economic Evaluation Reporting Standards (CHEERS) statement. Pharmacoeconomics. 2013;31(5):361–7.
Hamberg-van Reenen HH, Proper KI, van den Berg M. Worksite mental health interventions: a systematic review of economic evaluations. Occup Environ Med. 2012;69(11):837–45.
Mihalopoulos C, Chatterton ML. Economic evaluations of interventions designed to prevent mental disorders: a systematic review. Early Interv Psychiatry. Epub 24 Jun 2014.
CCEMG–EPPI-Centre Cost Converter, v. 1.4 (last update: 27 January 2014). Available at: http://eppi.ioe.ac.uk/costconversion/. Accessed 7 June 2014.
Bergenheim K, Williams SA, Bergeson JG, Stern L, Sriprasert M. US cost-effectiveness of saxagliptin in type 2 diabetes mellitus. Am J Pharm Benefits. 2012;4(1):20–8.
Cristiani M, Citarella A, Belisari A, Didoni G, Mantovani LG, Montella S. Valutazione economica dell’impiego di saxagliptin nel trattamento del diabete di tipo 2 in Italia. Farmeconomia e Percorsi Terapeutici. 2010;11(2):103–15.
Elgart JF, Caporale JE, Gonzalez L, Aiello E, Waschbusch M, Gagliardino JJ. Treatment of type 2 diabetes with saxagliptin: a pharmacoeconomic evaluation in Argentina. Health Econ Rev. 2013;3(1):11.
Erhardt W, Bergenheim K, Duprat-Lomon I, McEwan P. Cost effectiveness of saxagliptin and metformin versus sulfonylurea and metformin in the treatment of type 2 diabetes mellitus in Germany: a Cardiff diabetes model analysis. Clin Drug Investig. 2012;32(3):189–202.
Granström O, Bergenheim K, McEwan P, Sennfalt K, Henriksson M. Cost-effectiveness of saxagliptin (Onglyza®) in type 2 diabetes in Sweden. Prim Care Diabetes. 2012;6(2):127–36.
Grzeszczak W, Czupryniak L, Kolasa K, Sciborski C, Lomon ID, McEwan P. The cost-effectiveness of saxagliptin versus NPH insulin when used in combination with other oral antidiabetes agents in the treatment of type 2 diabetes mellitus in Poland. Diabetes Technol Ther. 2012;14(1):65–73.
Klarenbach S, Cameron C, Singh S, Ur E. Cost-effectiveness of second-line antihyperglycemic therapy in patients with type 2 diabetes mellitus inadequately controlled on metformin. CMAJ. 2011;183(16):E1213–20.
McEwan P, Evans M, Bergenheim K. A population model evaluating the costs and benefits associated with different oral treatment strategies in people with type 2 diabetes. Diabetes Obes Metab. 2010;12(7):623–30.
Nita ME, Eliaschewitz FG, Ribeiro E, Asano E, Barbosa E, Takemoto M, et al. Cost-effectiveness and budget impact of saxagliptine as additional therapy to metformin for the treatment of diabetes mellitus type 2 in the Brazilian private health system. Rev Assoc Med Bras. 2012;58(3):294–301.
Schwarz B, Gouveia M, Chen J, Nocea G, Jameson K, Cook J, et al. Cost-effectiveness of sitagliptin-based treatment regimens in European patients with type 2 diabetes and haemoglobin A1c above target on metformin monotherapy. Diabetes Obes Metab. 2008;10(Suppl 1):43–55.
Waugh N, Cummins E, Royle P, Clar C, Marien M, Richter B, et al. Newer agents for blood glucose control in type 2 diabetes: systematic review and economic evaluation. Health Technol Assess. 2010;14(36):1–248.
Resch B, Sommer C, Nuijten MJ, Seidinger S, Walter E, Schoellbauer V, et al. Cost-effectiveness of palivizumab for respiratory syncytial virus infection in high-risk children, based on long-term epidemiologic data from Austria. Pediatr Infect Dis J. 2012;31(1):e1–8.
Strom Williams JL, Lynch CP, Winchester R, Thomas L, Keith B, Egede LE. Gender differences in composite control of cardiovascular risk factors among patients with type 2 diabetes. Diabetes Technol Ther. 2014;16(7):421–7.
McGill JB, Vlajnic A, Knutsen PG, Recklein C, Rimler M, Fisher SJ. Effect of gender on treatment outcomes in type 2 diabetes mellitus. Diabetes Res Clin Pract. 2013;102(3):167–74.
Tobias DK, Pan A, Jackson CL, O’Reilly EJ, Ding EL, Willett WC, et al. Body-mass index and mortality among adults with incident type 2 diabetes. New Engl J Med. 2014;370(3):233–44.
Sculpher MJ, Pang FS, Manca A, Drummond MF, Golder S, Urdahl H, et al. Generalisability in economic evaluation studies in healthcare: a review and case studies. Health Technol Assess. 2004;8(49):iii–iv, 1–192.
Zhang Y, Hong J, Chi J, Gu W, Ning G, Wang W. Head-to-head comparison of dipeptidyl peptidase-IV inhibitors and sulfonylureas: a meta-analysis from randomized clinical trials. Diabetes Metab Res Rev. 2014;30(3):241–56.
Wu D, Li L, Liu C. Efficacy and safety of dipeptidyl peptidase-4 inhibitors and metformin as initial combination therapy and as monotherapy in patients with type 2 diabetes mellitus: a meta-analysis. Diabetes Obes Metab. 2014;16(1):30–7.
Schwartz SL. Treatment of elderly patients with type 2 diabetes mellitus: a systematic review of the benefits and risks of dipeptidyl peptidase-4 inhibitors. Am J Geriatr Pharmacother. 2010;8(5):405–18.
Zintzaras E, Miligkos M, Ziakas P, Balk EM, Mademtzoglou D, Doxani C, et al. Assessment of the relative effectiveness and tolerability of treatments of type 2 diabetes mellitus: a network meta-analysis. Clin Ther. 2014;36(10):1443–53.e9.
Colin X, Detournay B, Briand Y, Delaitre O. PDB22 potential budget impact of linagliptin in France estimated from current pattern of dipeptidyl peptidase 4 inhibitors prescriptions. Value Health. 2012;15(7):A497.
Nauck MA, Meininger G, Sheng D, Terranella L, Stein PP, Sitagliptin Study 024 Group. Efficacy and safety of the dipeptidyl peptidase-4 inhibitor, sitagliptin, compared with the sulfonylurea, glipizide, in patients with type 2 diabetes inadequately controlled on metformin alone: a randomized, double-blind, non-inferiority trial. Diabetes Obes Metab. 2007;9(2):194–205.
Scott R, Loeys T, Davies MJ, Engel SS, Sitagliptin Study 801 Group. Efficacy and safety of sitagliptin when added to ongoing metformin therapy in patients with type 2 diabetes. Diabetes Obes Metab. 2008;10(10):959–69.
Goke B, Gallwitz B, Eriksson J, Hellqvist A, Gause-Nilsson I, D1680C00001 Investigators. Saxagliptin is non-inferior to glipizide in patients with type 2 diabetes mellitus inadequately controlled on metformin alone: a 52-week randomised controlled trial. Int J Clin Pract. 2010;64(12):1619–31.
Hermansen K, Kipnes M, Luo E, Fanurik D, Khatami H, Stein P, et al. Efficacy and safety of the dipeptidyl peptidase-4 inhibitor, sitagliptin, in patients with type 2 diabetes mellitus inadequately controlled on glimepiride alone or on glimepiride and metformin. Diabetes Obes Metab. 2007;9(5):733–45.
Bolli G, Dotta F, Rochotte E, Cohen SE. Efficacy and tolerability of vildagliptin vs. pioglitazone when added to metformin: a 24-week, randomized, double-blind study. Diabetes Obes Metab. 2008;10(1):82–90.
McIntosh B, Cameron C, Singh SR, Yu C, Ahuja T, Welton NJ, et al. Second-line therapy in patients with type 2 diabetes inadequately controlled with metformin monotherapy: a systematic review and mixed-treatment comparison meta-analysis. Open Med. 2011;5(1):e35–48.
DeFronzo RA, Hissa MN, Garber AJ, Luiz Gross J, Yuyan Duan R, Ravichandran S, et al. The efficacy and safety of saxagliptin when added to metformin therapy in patients with inadequately controlled type 2 diabetes with metformin alone. Diabetes Care. 2009;32(9):1649–55.
Chacra AR, Tan GH, Apanovitch A, Ravichandran S, List J, Chen R, et al. Saxagliptin added to a submaximal dose of sulphonylurea improves glycaemic control compared with uptitration of sulphonylurea in patients with type 2 diabetes: a randomised controlled trial. Int J Clin Pract. 2009;63(9):1395–406.
Pradhan AD, Everett BM, Cook NR, Rifai N, Ridker PM. Effects of initiating insulin and metformin on glycemic control and inflammatory biomarkers among patients with type 2 diabetes: the LANCET randomized trial. JAMA. 2009;302(11):1186–94.
Monami M, Marchionni N, Mannucci E. Long-acting insulin analogues versus NPH human insulin in type 2 diabetes: a meta-analysis. Diabetes Res Clin Pract. 2008;81(2):184–9.
Phung OJ, Scholle JM, Talwar M, Coleman CI. Effect of noninsulin antidiabetic drugs added to metformin therapy on glycemic control, weight gain, and hypoglycemia in type 2 diabetes. JAMA. 2010;303(14):1410–8.
Garcia-Ruiz AJ, Perez-Costillas L, Montesinos AC, Alcalde J, Oyaguez I, Casado MA. Cost-effectiveness analysis of antipsychotics in reducing schizophrenia relapses. Health Econ Rev. 2012;2(1):8.
McCabe C, Claxton K, Culyer AJ. The NICE cost-effectiveness threshold: what it is and what that means. Pharmacoeconomics. 2008;26(9):733–44.
Dakin H, Devlin N, Feng Y, Rice N, O’Neill P, Parkin D. The influence of cost-effectiveness and other factors on NICE decisions. HERC research paper 01/13; Oxford: Health Economics Research Centre. Available at: http://www.herc.ox.ac.uk/downloads/NICE. Accessed 6 Aug 2014.
Yazdanpanah Y, Perelman J, DiLorenzo MA, Alves J, Barros H, Mateus C, et al. Routine HIV screening in Portugal: clinical impact and cost-effectiveness. PloS One. 2013;8(12):e84173.
Hallinen T, Soini EJ. The impact of the pharmaceutical pricing system on cost-effectiveness results: Finnish analysis. Open Pharmacoecon Health Econ J. 2011;3:6–10.
Cleemput I, Neyt M, Thiry N, De Laet C, Leys M. Threshold values for cost-effectiveness in health care. KCE reports 100C. Brussels: Belgian Health Care Knowledge Centre, 2008. Available at: http://kce.fgov.be/sites/default/files/page_documents/d20081027396.pdf. Accessed 10 Aug 2014.
Neilson AR, Sieper J, Deeg M. Cost-effectiveness of etanercept in patients with severe ankylosing spondylitis in Germany. Rheumatology. 2010;49(11):2122–34.
Acknowledgments
The evidence synthesis upon which this article was based was funded by Bristol-Myers Squibb (Shanghai, China) for Jinsong Geng, Yiwei Mao, Peng Zhang, and Yingyao Chen. Jinsong Geng also accepted funding from the China Medical Board (Grant Number 11-067) and the Shanghai Public Health 3-Year Program (GWDTR 201205, GWHW 2012S10) to go to the RAND Corporation in the US to complete the manuscript. The funders played no role in the study design; collection, analysis, and interpretation of data; writing of the report; or the decision to submit the paper for publication. They accept no responsibility for its contents.
All authors contributed to the conception and design of this work, and approved the final manuscript. Jinsong Geng, Yiwei Mao, and Peng Zhang were independent reviewers of the literature and were also responsible for study abstraction and writing of the manuscript. Hao Yu supervised all study activities and was responsible for the final manuscript review. Yingyao Chen is the overall guarantor of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
Registration This systematic review was registered with PROSPERO (Registration Number: CRD42013003354).
Rights and permissions
About this article
Cite this article
Geng, J., Yu, H., Mao, Y. et al. Cost Effectiveness of Dipeptidyl Peptidase-4 Inhibitors for Type 2 Diabetes. PharmacoEconomics 33, 581–597 (2015). https://doi.org/10.1007/s40273-015-0266-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40273-015-0266-y