Abstract
Purpose
For patients with uncontrolled epilepsy, the severity and postictal sequelae of seizures might be more impactful than their frequency. Seizure severity is often assessed using patient-reported outcome (PRO) instruments; however, evidence of content validity for existing instruments is lacking. Our aim was to understand the real-life experiences of patients with uncontrolled epilepsy.
Methods
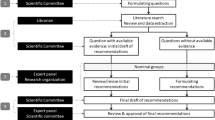
A preliminary conceptual model was developed. The model was refined through (1) a targeted literature review of qualitative research on seizure severity; (2) interviews with four clinical epilepsy experts to evaluate identified concepts; and (3) qualitative interviews with patients with uncontrolled epilepsy, gathering descriptions of symptoms and impacts of epilepsy, focusing on how patients experience and describe “seizure severity.” Findings were summarized in a final conceptual model of seizure severity in epilepsy.
Results
Twenty-five patients (12 who experienced primary generalized tonic–clonic seizures and 13 who experienced partial-onset seizures) expressed 42 different symptoms and 26 different impacts related to seizures. The final conceptual model contained a wide range of concepts related to seizure frequency, symptoms, and duration.
Conclusion
Our model identified several new concepts that characterize the patient experience of seizure severity. A seizure severity PRO instrument should cover a wide range of seizure symptoms alongside frequency and duration of seizures. This qualitative work reinforces the notion that measuring seizure frequency is insufficient and that seizure severity is important in defining the patient’s experience of epilepsy. This model could be used to assess the content validity of existing PRO instruments, or could support the development of a new one.

Similar content being viewed by others
References
Kwan P, Brodie MJ. Early identification of refractory epilepsy. N Engl J Med. 2000;342:314–9.
Schmidt D. Effect of antiepileptic drugs on the postictal state: a critical overview. Epilepsy Behav. 2010;19:176–81.
Kwan P, Brodie MJ. Neuropsychological effects of epilepsy and antiepileptic drugs. Lancet. 2001;357:216–22.
Bautista RE, Glen ET. Seizure severity is associated with quality of life independent of seizure frequency. Epilepsy Behav. 2009;16:325–9.
Tilz C, Stefan H, Hopfengaertner R, Kerling F, Genow A, Wang-Tilz Y. Influence of levetiracetame on ictal and postictal EEG in patients with partial seizures. Eur J Neurol. 2006;13:1352–8.
Smith DF, Baker GA, Dewey M, Jacoby A, Chadwick DW. Seizure frequency, patient-perceived seizure severity and the psychosocial consequences of intractable epilepsy. Epilepsy Res. 1991;9:231–41.
French JA. Proof of efficacy trials: endpoints. Epilepsy Res. 2001;45:53–6 (discussion 57–9).
Jacoby A, Baker G, Smith D, Dewey M, Chadwick D. Measuring the impact of epilepsy: the development of a novel scale. Epilepsy Res. 1993;16:83–8.
Cramer JA, French J. Quantitative assessment of seizure severity for clinical trials: a review of approaches to seizure components. Epilepsia. 2001;42:119–29.
US Department of Health and Human Services, Food and Drug Administration, Center for Drug Evaluation and Research, Center for Biologics Evaluation and Research, Center for Devices and Radiological Health. Guidance for industry: patient-reported outcome measures: use in medical product development to support labeling claims. Silver Spring: Food and Drug Administration; 2009. http://www.fda.gov/downloads/Drugs/…/Guidances/UCM193282.pdf. Accessed 5 Aug 2015.
Cramer JA, Smith DB, Mattson RH, Delgado Escueta AV, Collins JF. A method of quantification for the evaluation of antiepileptic drug therapy. Neurology. 1983;33(3 Suppl 1):26–37.
Duncan JS, Sander JW. The Chalfont Seizure Severity Scale. J Neurol Psychiatry. 1991;54:873–6.
O’Donoghue MF, Duncan JS, Sander JW. The National Hospital Seizure Severity Scale: a further development of the Chalfont Seizure Severity Scale. Epilepsia. 1996;37:563–71.
Baker GA, Smith DF, Dewey M, Morrow J, Crawford PM, Chadwick DW. The development of a seizure severity scale as an outcome measure in epilepsy. Epilepsy Res. 1991;8:245–51.
Carpay JA, Vermuelen J, Stroink H, Brouwer OF, Peters AC, Aldenkamp AP, et al. Seizure severity in children with epilepsy: a parent-completed scale compared with clinical data. Epilepsia. 1997;38:346–52.
Cramer JA, Baker GA, Jacoby A. Development of a new seizure severity questionnaire: initial reliability and validity testing. Epilepsy Res. 2002;48:187–97.
Gallop K, Wild D, Verdian L, Kerr M, Jacoby A, Baker G, et al. Lennox-Gastaut syndrome (LGS): development of conceptual models of health-related quality of life (HRQL) for caregivers and children. Seizure. 2010;19:23–30.
Gilliam F, Kuzniecky R, Faught E, Black L, Carpenter G, Schrodt R. Patient-validated content of epilepsy-specific quality-of-life measurement. Epilepsia. 1997;38:233–6.
Bryant-Comstock L, Scott-Lennox J, Lennox R. Assessment of seizure severity with adjunctive lamotrigine therapy: results from a US observational study. Epilepsy Behav. 2001;2:152–7.
Smith D, Baker GA, Jacoby A, Chadwick DW. The contribution of the measurement of seizure severity to quality of life research. Qual Life Res. 1995;4:143–58.
Guekht AB, Mitrokhina TV, Lebedeva AV, Dzugaeva FK, Milchakova LE, Lokshina OB, et al. Factors influencing on quality of life in people with epilepsy. Seizure. 2007;16:128–33.
Leidy NK, Elixhauser A, Rentz AM, Beach R, Pellock J, Schachter S, et al. Telephone validation of the Quality of Life in Epilepsy Inventory-89 (QOLIE-89). Epilepsia. 1999;40:97–106.
Cavanna AE. Seizures and consciousness. In: Schachter SC, Holmes GL, Kasteleijn-Nost Trenité D, editors. Behavioral aspects of epilepsy: principles and practices. New York: Demos Medical Publishing; 2008. p. 99–104.
Sierra M, Berrios GE. The Cambridge Depersonalization Scale: a new instrument for the measurement of depersonalization. Psychiatry Res. 2000;93:153–64.
Nijenhuis ER, Spinhoven P, Van Dyck R, Van der Hart O, Vanderlinden J. The development and psychometric characteristics of the Somatoform Dissociation Questionnaire (SDQ-20). J Nerv Ment Dis. 1996;184:688–94.
Devinsky O, Vickrey BG, Cramer J, Perrine K, Hermann B, Meador K, et al. Development of the quality of life in epilepsy inventory. Epilepsia. 1995;36:1089–104.
Bernstein EM, Putnam FW. Development, reliability, and validity of a dissociation scale. J Nerv Ment Dis. 1986;174:727–35.
Carlson EB, Putnam FW, Ross CA, Torem M, Coons P, Dill DL, et al. Validity of the Dissociative Experiences Scale in screening for multiple personality disorder: a multicenter study. Am J Psychiatry. 1993;150:1030–6.
Derogatis LR, Kourlesis SM. An approach to evaluation of sexual problems in the cancer patient. CA Cancer J Clin. 1981;31:46–50.
Hovinga CA, Asato MR, Manjunath R, Wheless JW, Phelps SJ, Sheth RD, et al. Association of non-adherence to antiepileptic drugs and seizures, quality of life, and productivity: survey of patients with epilepsy and physicians. Epilepsy Behav. 2008;13:316–22.
Harden CL, Maroof DA, Nikolov B, Fowler K, Sperling M, Liporace J, et al. The effect of seizure severity on quality of life in epilepsy. Epilepsy Behav. 2007;11:208–11.
Jacoby A, Baker GA. Quality-of-life trajectories in epilepsy: a review of the literature. Epilepsy Behav. 2008;12:557–71.
Chiesa V, Gardella E, Tassi L, Canger R, Lo Russo G, Piazzini A, et al. Age-related gender differences in reporting ictal fear: analysis of case histories and review of the literature. Epilepsia. 2007;48:2361–4.
Bazil CW. Epilepsy and sleep disturbance. Epilepsy Behav. 2003;4(Suppl 2):S39–45.
de Weerd A, de Haas S, Otte A, Trenité DK, van Erp G, Cohen A, et al. Subjective sleep disturbance in patients with partial epilepsy: a questionnaire-based study on prevalence and impact on quality of life. Epilepsia. 2004;45:1397–404.
Elwes RD, Marshall J, Beattie A, Newman PK. Epilepsy and employment: a community based survey in an area of high unemployment. J Neurol Neurosurg Psychiatry. 1991;54:200–3.
Shikiar R, Halpern MT, Rentz AM, Khan ZM. Development of the Health and Work Questionnaire (HWQ): an instrument for assessing workplace productivity in relation to worker health. Work. 2004;22:219–29.
Scambler G, Hopkins A. Being epileptic: coming to terms with stigma. Sociol Health Illn. 1986;8:26–43.
Jacoby A. Stigma, epilepsy, and quality of life. Epilepsy Behav. 2002;3:10–20.
Jacoby A. Felt versus enacted stigma: a concept revisited. Evidence from a study of people with epilepsy in remission. Soc Sci Med. 1994;38:269–74.
Boylan LS, Flint LA, Labovitz DL, Jackson SC, Starner K, Devinsky O. Depression but not seizure frequency predicts quality of life in treatment-resistant epilepsy. Neurology. 2004;62:258–61.
Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961;4:561–71.
Lovibond PF, Lovibond SH. The structure of negative emotional states: comparison of the Depression Anxiety Stress Scales (DASS) with the Beck Depression and Anxiety Inventories. Behav Res Ther. 1995;33:335–43.
Hamilton M. The assessment of anxiety states by rating. Br J Med Psychol. 1959;32:50–5.
Ware JE Jr, Sherbourne CD. The MOS 36-Item Short-Form Health Survey (SF-36): I. Conceptual framework and item selection. Med Care. 1992;30:473–83.
Baker G, Jacoby A, Buck D, Stalgis C, Monnet D. Quality of life of people with epilepsy: a European study. Epilepsia. 1997;38:353–62.
Jacoby A, Johnson A, Chadwick D. Psychosocial outcomes of antiepileptic drug discontinuation. The Medical Research Council Antiepileptic Drug Withdrawal Study Group. Epilepsia. 1992;33:1123–31.
Leppik IE, Biton V, Sander JW, Wieser HG. Levetiracetam and partial seizure subtypes: pooled data from three randomized, placebo-controlled trials. Epilepsia. 2003;44:1585–7.
Chan CJ, Zou G, Wiebe S, Speechley KN. Global Assessment of the Severity of Epilepsy (GASE) Scale in children: validity, reliability, responsiveness. Epilepsia. 2015;. doi:10.1111/epi.13216.
Vickrey BG, Berg AT, Sperling MR, Shinnar S, Langfitt JT, Bazil CW, et al. Relationships between seizure severity and health-related quality of life in refractory localization-related epilepsy. Epilepsia. 2000;41:760–4.
Borghs S, de la Loge C, Brabant Y, Cramer J. Sensitivity testing of the Seizure Severity Questionnaire (SSQ). Epilepsy Behav. 2014;31:281–5.
Center for Drug Evaluation and Research. Guidelines for the clinical evaluation of antiepileptic drugs (adults and children). Rockville: US Department of Health and Human Services, Food and Drug Administration; 1981. http://www.fda.gov/downloads/drugs/guidancecomplianceregulatoryinformation/guidances/ucm071582.pdf. Accessed 5 Aug 2015.
Committee for Medicinal Products for Human Use. Guideline on clinical investigation of medicinal products in the treatment of epileptic disorders. London: European Medicines Agency; 2010. http://www.ema.europa.eu/docs/en_GB/document_library/Scientific_guideline/2010/01/WC500070043.pdf. Accessed 13 Nov 2015.
Kerr C, Nixon A, Angalakuditi M. The impact of epilepsy on children and adult patients’ lives: development of a conceptual model from qualitative literature. Seizure. 2011;20:764–74.
Rapport F, Clement C, Doel MA, Hutchings HA. Qualitative research and its methods in epilepsy: contributing to an understanding of patients’ lived experiences of the disease. Epilepsy Behav. 2015;45:94–100.
Fisher RS, Nune G, Roberts SE, Cramer JA. The Personal Impact of Epilepsy Scale (PIES). Epilepsy Behav. 2015;42:140–6.
Proposal for revised clinical and electroencephalographic classification of epileptic seizures. From the Commission on Classification and Terminology of the International League Against Epilepsy. Epilepsia 1981;22:489–501. Available at: http://www.ilae.org/Visitors/Documents/CommissionSeizuresEpilepsia1981.pdf.
Acknowledgments
The authors wish to acknowledge and thank the epilepsy experts and patients who completed the interviews, and Barbara Pelgrims, Ph.D. (UCB Pharma, Brussels, Belgium), for publication coordination. Editorial assistance was provided by Jennifer Bodkin, Ph.D. (Evidence Scientific Solutions, Horsham, UK), and funded by UCB Pharma. This included formatting of the text and tables, collection of author contribution and conflict of interest statements, and assistance with the online submission process by uploading files.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Author contributions
All authors contributed to the design of the study. Erin Tomaszewski and Katarina Halling collected the data. Simon Borghs, Erin Tomaszewski, and Katarina Halling analyzed and interpreted the data. All authors contributed to the development and final decision to submit the manuscript, and act as guarantors.
Funding
This study was funded by UCB Pharma.
Conflict of interest
Simon Borghs is an employee of UCB Pharma. Erin Tomaszewski and Katarina Halling were employees of PRO Consulting at the time when this research was conducted. Christine de la Loge was an employee of UCB Pharma at the time when this research was conducted and is currently an independent consultant.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Borghs, S., Tomaszewski, E.L., Halling, K. et al. Understanding the Patient Perspective of Seizure Severity in Epilepsy: Development of a Conceptual Model. Patient 9, 419–431 (2016). https://doi.org/10.1007/s40271-016-0165-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40271-016-0165-0