Abstract
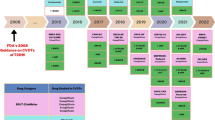
For many years, clinical studies could not show that lowering glucose in patients with type 2 diabetes leads to better macrovascular outcomes. In the past few years, new data have shown that treatment with two classes of dugs developed as “glucose-lowering agents,” SGLT2 inhibitors and GLP-1 receptor agonists, can reduce macrovascular and renal complications. These studies have prompted debate about the main aim of type 2 diabetes management. In this review, three eras of diabetes management are described according to the treatment recommendations, such as the ADA/EASD consensus, moving from a pure glucocentric view into the present cardio-renal outcome-oriented approach, this has been endorsed by major diabetes and cardiology societies. While in the first era normalizing HbA1c was the only focus (e.g., UK Prospective Diabetes Study), failing to show a reduction in cardiovascular morbidity and mortality, further studies analyzing the pros and cons of intensified control such as ACCORD, VADT, ADVANCE recognized that treatment intensification was associated with weight gain and hypoglycemia, thereby potentially reducing the benefits of glycemic control. Therefore, the focus in the second area was on controlling HbA1c without these unwanted effects. The consistent beneficial results of several cardiovascular outcome trials with SGLT2 inhibitors and GLP-1 receptor agonists showing significantly improved cardio-renal outcomes, induced a paradigm shift: a change from (only) control of HbA1c to an organ-protective approach with the main focus now on cardio-renal risk; this is now considered as the third era. Recent data indicating beneficial effects of glucose-lowering agents in particular SGLT2 inhibitors even in subjects without diabetes, improving hospitalization for heart failure and renal outcomes might reveal another new era, which could then be considered a fourth era. While current international guidelines call for this paradigm shift, registry data show that we are still far from translating this objective into real-world practice.

Similar content being viewed by others
References
Dal Canto E, Ceriello A, Ryden L, et al. Diabetes as a cardiovascular risk factor: an overview of global trends of macro and micro vascular complications. Eur J Prev Cardiol. 2019;26(2S):25–32.
Chilton RJ, Dungan KM, Shubrook JH, Umpierrez GE. Cardiovascular risk and the implications for clinical practice of cardiovascular outcome trials in type 2 diabetes. Prim Care Diabetes. 2019;14(3):193–212.
Bethel MA, McMurray JJV. class effect for sodium glucose-cotransporter-2 inhibitors in cardiovascular outcomes: implications for the cardiovascular disease specialist. Circulation. 2018;137(12):1218–20.
Bethel MA, Patel RA, Merrill P, et al. Cardiovascular outcomes with glucagon-like peptide-1 receptor agonists in patients with type 2 diabetes: a meta-analysis. Lancet Diabetes Endocrinol. 2018;6(2):105–13.
Zelniker TA, Wiviott SD, Raz I, et al. Comparison of the effects of glucagon-like peptide receptor agonists and sodium-glucose cotransporter 2 inhibitors for prevention of major adverse cardiovascular and renal outcomes in type 2 diabetes mellitus. Circulation. 2019;139(17):2022–31.
Gerstein HC, Colhoun HM, Dagenais GR, et al. Dulaglutide and cardiovascular outcomes in type 2 diabetes (REWIND): a double-blind, randomised placebo-controlled trial. Lancet. 2019;394(10193):121–30.
Giugliano D, Maiorino MI, Bellastella G, et al. GLP-1 receptor agonists for prevention of cardiorenal outcomes in type 2 diabetes: an updated meta-analysis including the REWIND and PIONEER 6 trials. Diabetes Obes Metab. 2019;21(11):2576–80.
Perkovic V, Jardine MJ, Neal B, et al. Canagliflozin and renal outcomes in type 2 diabetes and nephropathy. N Engl J Med. 2019;380(24):2295–306.
Scandinavian Simvastatin Survival Study group. Scandinavian Simvastatin Survival Study (4S). Lancet. 1994;344:1383–9
Heart Outcomes Prevention Evaluation Study Investigators. Effects of an angiotensin-converting-enzyme inhibitor, ramipril, on cardiovascular events in high-risk patients. N Engl J Med. 2000;342:145–53.
Seltzer HS. A summary of criticisms of the findings and conclusions of the University Group Diabetes Program (UGDP). Diabetes. 1972;21(9):976–9.
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352(9131):837–53.
UK Prospective Diabetes Study (UKPDS) Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet. 1998.352(9131):854–65.
Pirart J. Diabetes mellitus and its degenerative complications: a prospective study of 4,400 patients observed between 1947 and 1973 (3rd and last part) (author’s transl). Diabetes Metab. 1977;3(4):245–56.
Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321(7258):405–12.
Marx N, McGuire DK, Perkovic V, et al. Composite primary end points in cardiovascular outcomes trials involving type 2 diabetes patients: should unstable angina be included in the primary end point? Diabetes Care. 2017;40(9):1144–51.
Griffin SJ, Leaver JK, Irving GJ. Impact of metformin on cardiovascular disease: a meta-analysis of randomised trials among people with type 2 diabetes. Diabetologia. 2017;60(9):1620–29.
Holman RR, Paul SK, Bethel MA, Matthews DR, Neil HA. 10-year follow-up of intensive glucose control in type 2 diabetes. N Engl J Med. 2008;359(15):1577–89.
Matthews DR, Cull CA, Stratton IM, Holman RR, Turner RC, UK Prospective Diabetes Study (UKPDS) Group. UKPDS 26: sulphonylurea failure in non-insulin-dependent diabetic patients over six years. Diabet Med. 1998;15(4):297–303.
Efficacy of atenolol and captopril in reducing risk of macrovascular and microvascular complications in type 2 diabetes: UKPDS 39. UK Prospective Diabetes Study Group. Bmj, 1998. 317(7160): p. 713-20.
Stratton IM, Cull CA, Adler AI, et al. Additive effects of glycaemia and blood pressure exposure on risk of complications in type 2 diabetes: a prospective observational study (UKPDS 75). Diabetologia. 2006;49(8):1761–9.
Haffner SM. The Scandinavian Simvastatin Survival Study (4S) subgroup analysis of diabetic subjects: implications for the prevention of coronary heart disease. Diabetes Care. 1997;20(4):469–71.
Colhoun HM, Betteridge DJ, Durrington PN, et al. Primary prevention of cardiovascular disease with atorvastatin in type 2 diabetes in the Collaborative Atorvastatin Diabetes Study (CARDS): multicentre randomised placebo-controlled trial. Lancet. 2004;364(9435):685–96.
Gaede P, Vedel P, Larsen N, et al. Multifactorial intervention and cardiovascular disease in patients with type 2 diabetes. N Engl J Med. 2003;348(5):383–93.
Gaede P, Lund-Andersen H, Parving HH, Pedersen O. Effect of a multifactorial intervention on mortality in type 2 diabetes. N Engl J Med. 2008;358(6):580–91.
Rodriguez-Gutierrez R, Montori VM. Glycemic control for patients with type 2 diabetes mellitus: our evolving faith in the face of evidence. Circ Cardiovasc Qual Outcomes. 2016;9(5):504–12.
Nathan DM, Buse JB, Davidson MB, et al. Medical management of hyperglycaemia in type 2 diabetes mellitus: a consensus algorithm for the initiation and adjustment of therapy: a consensus statement from the American Diabetes Association and the European Association for the Study of Diabetes. Diabetologia. 2009;52(1):17–30.
Gerstein HC, Miller ME, Byington RP, et al. Effects of intensive glucose lowering in type 2 diabetes. N Engl J Med. 2008;358(24):2545–59.
Patel A, MacMahon S, Chalmers J, et al. Intensive blood glucose control and vascular outcomes in patients with type 2 diabetes. N Engl J Med. 2008;358(24):2560–72.
Duckworth W, Abraira C, Moritz T, et al. Glucose control and vascular complications in veterans with type 2 diabetes. N Engl J Med. 2009;360(2):129–39.
Dluhy RG, McMahon GT. Intensive glycemic control in the ACCORD and ADVANCE trials. N Engl J Med. 2008;358(24):2630–3.
Group AS, Gerstein HC, Miller ME, et al. Long-term effects of intensive glucose lowering on cardiovascular outcomes. N Engl J Med. 2011;364(9):818–28.
Yki-Jarvinen H. Thiazolidinediones. N Engl J Med. 2004;351(11):1106–18.
Kaul S, Bolger AF, Herrington D, Giugliano RP, Eckel RH. Thiazolidinedione drugs and cardiovascular risks: a science advisory from the American Heart Association and American College of Cardiology Foundation. Circulation. 2010;121(16):1868–77.
Holman RR, Cull CA, Turner RC. A randomized double-blind trial of acarbose in type 2 diabetes shows improved glycemic control over 3 years (U.K. Prospective Diabetes Study 44). Diabetes Care. 1999;22(6):960–4.
Chow E, Bernjak A, Williams S, et al. Risk of cardiac arrhythmias during hypoglycemia in patients with type 2 diabetes and cardiovascular risk. Diabetes. 2014;63(5):1738–47.
Riddle MC. Counterpoint: Intensive glucose control and mortality in ACCORD—still looking for clues. Diabetes Care. 2010;33(12):2722–4.
Genuth S, Ismail-Beigi F. Clinical implications of the ACCORD trial. J Clin Endocrinol Metab. 2012;97(1):41–8.
Group AS. Nine-year effects of 3.7 years of intensive glycemic control on cardiovascular outcomes. Diabetes Care. 2016;39(5):701–8.
Zoungas S, Chalmers J, Neal B, et al. Follow-up of blood-pressure lowering and glucose control in type 2 diabetes. N Engl J Med. 2014;371(15):1392–406.
Reaven PD, Hayward RA, Zhou J. Intensive glucose control and type 2 diabetes—15 years on. Reply. N Engl J Med. 2019;381(13):1293.
Currie CJ, Peters JR, Tynan A, et al. Survival as a function of HbA(1c) in people with type 2 diabetes: a retrospective cohort study. Lancet. 2010;375(9713):481–9.
Inzucchi SE, Bergenstal RM, Buse JB, et al. Management of hyperglycemia in type 2 diabetes, 2015: a patient-centered approach: update to a position statement of the American Diabetes Association and the European Association for the Study of Diabetes. Diabetes Care. 2015;38(1):140–9.
Zinman B, Wanner C, Lachin JM, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373:2117–28.
Guidance for Industry. Diabetes mellitus—evaluating cardiovascular risk in new antidiabetic therapies to treat type 2 diabetes. http://www.fda.gov/downloads/Drugs/GuidanceComplianceRegulatoryInformation/Guidances/UCM071627.pdfeutm_term=guidance. Accessed 6 June 2021.
Azim S, Baker WL, White WB. Evaluating cardiovascular safety of novel therapeutic agents for the treatment of type 2 diabetes mellitus. Curr Cardiol Rep. 2014;16(11):541.
Krentz AJ, Hompesch M. Cardiovascular safety of new drugs for diabetes: getting the balance right? Pharm Med. 2014;28:109–17.
Scheen AJ. Safety of dipeptidyl peptidase-4 inhibitors for treating type 2 diabetes. Expert Opin Drug Saf. 2015;14(4):505–24.
Scirica BM, Bhatt DL, Braunwald E, et al. Saxagliptin and cardiovascular outcomes in patients with type 2 diabetes mellitus. N Engl J Med. 2013;369(14):1317–26.
White WB, Cannon CP, Heller SR, et al. Alogliptin after acute coronary syndrome in patients with type 2 diabetes. N Engl J Med. 2013;369(14):1327–35.
Packer M. Worsening heart failure during the use of DPP-4 inhibitors: pathophysiological mechanisms, clinical risks, and potential influence of concomitant antidiabetic medications. JACC Heart Fail. 2018;6(6):445–51.
Pfeffer MA, Claggett B, Diaz R, et al. Lixisenatide in patients with type 2 diabetes and acute coronary syndrome. N Engl J Med. 2015;373(23):2247–57.
Holman RR, Bethel MA, Mentz RJ, et al. Effects of once-weekly exenatide on cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2017;377(13):1228–39.
Wiviott SD, Raz I, Bonaca MP, et al. Dapagliflozin and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2019;380(4):347–57.
Sattar N, McLaren J, Kristensen SL, Preiss D, McMurray JJ. SGLT2 Inhibition and cardiovascular events: why did EMPA-REG Outcomes surprise and what were the likely mechanisms? Diabetologia. 2016;59(7):1333–9.
Roder ME. Major adverse cardiovascular event reduction with GLP-1 and SGLT2 agents: evidence and clinical potential. Ther Adv Chronic Dis. 2018;9(1):33–50.
Vallon V, Thomson SC. Targeting renal glucose reabsorption to treat hyperglycaemia: the pleiotropic effects of SGLT2 inhibition. Diabetologia. 2017;60(2):215–25.
Schnell O, Cos X, Cosentino F, Forst T, Giorgino F, Heersprink HJL, Kosiborod M, Wanner C, Standl E. Report from the CVOT summit 2020: new cardiovascular and renal outcomes. Cardiovasc Diabetol. 2021;20(1):75. https://doi.org/10.1186/s12933-021-01254-1.
Cefalu WT, Kaul S, Gerstein HC, et al. Cardiovascular outcomes trials in type 2 diabetes: where do we go from here? reflections from a diabetes care editors’ expert forum. Diabetes Care. 2018;41(1):14–31.
Thomson SC, Vallon V. Renal effects of sodium-glucose co-transporter inhibitors. Am J Cardiol. 2019;124(Suppl 1):S28–35.
Cherney DZ, Odutayo A, Aronson R, Ezekowitz J, Parker JD. Sodium glucose cotransporter-2 inhibition and cardiorenal protection: JACC review topic of the week. J Am Coll Cardiol. 2019;74(20):2511–24.
Sloan LA. Review of glucagon-like peptide-1 receptor agonists for the treatment of type 2 diabetes mellitus in patients with chronic kidney disease and their renal effects. J Diabetes. 2019;11(12):938–48.
Vaduganathan M, Januzzi JL Jr. Preventing and treating heart failure with sodium-glucose co-transporter 2 inhibitors. Am J Cardiol. 2019;124(Suppl 1):S20–7.
Ferrannini E, Mark M, Mayoux E. CV Protection in the EMPA-REG OUTCOME trial: a “thrifty substrate” hypothesis. Diabetes Care. 2016;39(7):1108–14.
Drucker DJ. The ascending GLP-1 road from clinical safety to reduction of cardiovascular complications. Diabetes. 2018;67(9):1710–9.
Inzucchi SE, Zinman B, Fitchett D, et al. How does empagliflozin reduce cardiovascular mortality? Insights from a mediation analysis of the EMPA-REG OUTCOME Trial. Diabetes Care. 2018;41(2):356–63.
Home P. Controversies for glucose control targets in type 2 diabetes: exposing the common ground. Diabetes Care. 2019;42(9):1615–23.
Davies MJ, D'Alessio DA, Fradkin J, et al. Management of hyperglycemia in type 2 diabetes, 2018. A consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2018;41(12):2669–701.
Arnett DK, Blumenthal RS, Albert MA, et al. 2019 ACC/AHA guideline on the primary prevention of cardiovascular disease: executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. J Am Coll Cardiol. 2019;74(10):1376–414.
Cosentino F, Grant PJ, Aboyans V, et al. 2019 ESC guidelines on diabetes, pre-diabetes, and cardiovascular diseases developed in collaboration with the EASD. Eur Heart J. 2019;41(2):255–323.
Heijmans R, Singh SS, Lieverse AG, Sijbrands EJG, van Hoek M. The effect of guideline revisions on vascular complications of type 2 diabetes. Ther Adv Endocrinol Metab. 2019;10:2042018819875408.
Wittbrodt E, Chamberlain D, Arnold SV, Tang F, Kosiborod M. Eligibility of patients with type 2 diabetes for sodium-glucose co-transporter-2 inhibitor cardiovascular outcomes trials: an assessment using the Diabetes Collaborative Registry. Diabetes Obes Metab. 2019;21(8):1985–9.
Arnold SV, de Lemos JA, Rosenson RS, et al. Use of guideline-recommended risk reduction strategies among patients with diabetes and atherosclerotic cardiovascular disease. Circulation. 2019;140(7):618–20.
Zannad F, Ferreira JP, Pocock SJ, Anker SD, Butler J, Filippatos G, Brueckmann M, Ofstad AP, Pfarr E, Jamal W, Packer M. SGLT2 inhibitors in patients with heart failure with reduced ejection fraction: a meta-analysis of the EMPEROR-Reduced and DAPA-HF trials. Lancet. 2020;396(10254):819–29.
Heerspink HJL, Stefánsson BV, Correa-Rotter R, Chertow GM, Greene T, Hou FF, Mann JFE, McMurray JJV, Lindberg M, Rossing P, Sjöström CD, Toto RD, Langkilde AM, Wheeler DC, DAPA-CKD Trial Committees and Investigators. Dapagliflozin in patients with chronic kidney disease. N Engl J Med. 2020;383(15):1436–46.
Ryan DH, Lingvay I, Colhoun HM, Deanfield J, Emerson SS, Kahn SE, Kushner RF, Marso S, Plutzky J, Brown-Frandsen K, Gronning MOL, Hovingh GK, Holst AG, Ravn H, Lincoff AM. Semaglutide effects on cardiovascular outcomes in people with overweight or obesity (SELECT) rationale and design. Am Heart J. 2020;229:61–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This article received no funding.
Conflict of interest
Stephan Jacob: Honoraria, research support and consulting fees from Amgen, AstraZeneca, Bayer, Berlin-Chemie, Boehringer Ingelheim, Daiichi Sankyo, Esanum, Eli Lilly, Medcon, Merck, MSD, Novartis, Novo Nordisk, Roche, Sanofi-Aventis, Servier. Andrew Krentz: Lecture fees from Bayer, Boehringer Ingelheim, Eli Lilly, GlaxoSmithKline, Novo Nordisk, Merck, Pfizer, Servier, Takeda. Research grants from Fujisawa, Pfizer, Servier, Novo Nordisk. John Deanfield: Received CME honoraria and/or consulting fees from Amgen, Boehringer Ingelheim, Merck, Pfizer, Aegerion, Novartis, Sanofi, Takeda, Novo Nordisk, Bayer. Member of Study Steering Committees for Novo Nordisk. Research grants from British Heart Foundation, MRC(UK), NIHR, PHE, MSD, Pfizer, Aegerion, Colgate, Roche. Lars Ryden: Advisory Board/Speaker: AstraZeneca, Bayer AG, Boehringer Ingelheim, MSD, Novo Nordisk, Sanofi-Aventis. Research support: Swedish Heart-Lung Foundation, Swedish Diabetes Foundation, Family Erling Perssons Foundation, Karolinska Institutet, Private Foundations,Stockholm County Council, Swedish Medical Assembly, Amgen, Bayer, Boehringer Ingelheim, MSD, Novo Nordisk.
Ethics approval, Consent to participate, Consent for publication, Availability of data and materials and Code availability
Not applicable.
Rights and permissions
About this article
Cite this article
Jacob, S., Krentz, A.J., Deanfield, J. et al. Evolution of Type 2 Diabetes Management from a Glucocentric Approach to Cardio-Renal Risk Reduction: The New Paradigm of Care. Drugs 81, 1373–1379 (2021). https://doi.org/10.1007/s40265-021-01554-6
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40265-021-01554-6