Abstract
Introduction
Multiple sclerosis (MS) has significant financial consequences for healthcare systems, individual patients and households, and the wider society. This study examines the distribution of MS costs and resource utilisation across cost categories and from various perspectives, as MS disability increases.
Methods
Two hundred and fourteen patients with MS were recruited from a specialist MS outpatient clinic in Ireland and included in an interview-based study on MS-related healthcare resource consumption and costs. Patients were grouped into three categories based on disability: mild [Expanded Disability Status Scale (EDSS) score 0–3.5, n = 114], moderate (EDSS 4.0–6.5, n = 72) and severe (EDSS 7.0–9.5, n = 27). The mean annual direct and indirect costs (in year 2012 values) were estimated using non-parametric bootstrapping.
Results
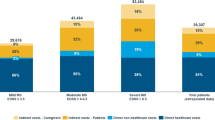
Participants were 66.4 % female, with a mean age of 47.6 years and a mean EDSS score of 3.6. The majority had relapsing-remitting MS (RRMS) (53 %). The mean annual direct (indirect) costs per person were €10,249 (€9,447), €13,045 (€31,806) and €56,528 (€39,440) in mild, moderate and severe MS, respectively. Direct costs are driven by the cost of disease-modifying therapies and professional home help in mild and severe MS, respectively. Between 74 % (severe MS) and 96 % (mild MS) of all direct costs are borne by the healthcare payer, the remainder being incurred by patients, their families or other non-healthcare organisations.
Conclusions
MS is associated with high levels of healthcare resource consumption and costs, and these costs increase with increasing disability. There is potential to significantly reduce the economic burden of MS through interventions that prevent progression from mild or moderate MS to severe MS, help support independent living at home and keep people with MS in the work force.


Similar content being viewed by others
References
Tremlett H, Zhao Y, Rieckmann P, Hutchinson M. New perspectives in the natural history of multiple sclerosis. Neurology. 2010;74(24):2004–15.
Lublin FD, Reingold SC. Defining the clinical course of multiple sclerosis: results of an international survey. Neurology. 1996;46(4):907–11.
WHO and MSIF, Atlas: multiple sclerosis resources in the world. London: Multiple Sclerosis International Federation, 2008. Available at: http://www.msif.org/en/about_msif/what_we_do/atlas_of_ms/index.html. Accessed 31 July 2013.
Lonergan R, Kinsella K, Fitzpatrick P, Brady J, Murray B, Dunne C, et al. Multiple sclerosis prevalence in Ireland: relationship to vitamin D status and HLA genotype. J Neurol Neurosurg Psychiatry. 2011;82(3):317–22. doi:10.1136/jnnp.2010.220988.
Fogarty E, Walsh C, Adams R, McGuigan C, Barry M, Tubridy N. Relating health-related quality of life to disability progression in multiple sclerosis, using the 5-level EQ-5D. Mult Scler. 2013. doi:10.1177/1352458512474860.
Beer S, Khan F, Kesselring J. Rehabilitation interventions in multiple sclerosis: an overview. J Neurol. 2012;259(9):1994–2008.
Weinshenker BG, Bass B, Rice GPA, Noseworthy J, Carriere W, Baskerville J, et al. The natural history of multiple sclerosis: a geographically based study. I. Clinical course and disability. Brain. 1989;112(1):133–46.
Karampampa K, Gustavsson A, Miltenburger C, Eckert B. Treatment experience, burden and unmet needs (TRIBUNE) in MS study: results from five European countries. Mult Scler. 2012;18(2 Suppl):7–15.
Kobelt G, Berg J, Atherly D, Hadjimichael O. Costs and quality of life in multiple sclerosis: a cross-sectional study in the United States. Neurology. 2006;66(11):1696–702.
McCrone P, Heslin M, Knapp M, Bull P, Thompson A. Multiple sclerosis in the UK: service use, costs, quality of life and disability. Pharmacoeconomics. 2008;26(10):847–60.
Kobelt G, Berg J, Lindgren P, Fredrikson S, Jonsson B. Costs and quality of life of patients with multiple sclerosis in Europe. J Neurol Neurosurg Psychiatry. 2006;77(8):918–26.
Casado V, Martinez-Yelamos S, Martinez-Yelamos A, Carmona O, Alonso L, Romero L et al. Direct and indirect costs of multiple sclerosis in Baix Llobregat (Catalonia, Spain), according to disability. BMC Health Services Research. 2006;6.
Blahova Dusankova J, Kalincik T, Dolezal T, Kobelt G, Havrdova E. Cost of multiple sclerosis in the Czech Republic: the COMS study. Mult Scler. 2012;18(5):662–8.
Kappos L, Polman CH, Freedman MS, Edan G, Hartung HP, Miller DH, et al. Treatment with interferon beta-1b delays conversion to clinically definite and McDonald MS in patients with clinically isolated syndromes. Neurology. 2006;67(7):1242–9.
Jacobs LD, Beck RW, Simon JH, Kinkel RP, Brownscheidle CM, Murray TJ, et al. Intramuscular interferon beta-1a therapy initiated during a first demyelinating event in multiple sclerosis. N Eng J Med. 2000;343(13):898–904.
Comi G, Martinelli V, Rodegher M, Moiola L, Bajenaru O, Carra A, et al. Effect of glatiramer acetate on conversion to clinically definite multiple sclerosis in patients with clinically isolated syndrome (PreCISe study): a randomised, double-blind, placebo-controlled trial. Lancet Neurology. 2009;374(9700):1503–11.
Comi G, Filippi M, Barkhof F, Durelli L, Edan G, Fernandez O, et al. Effect of early interferon treatment on conversion to definite multiple sclerosis: a randomised study. Lancet. 2001;357(9268):1576–82.
Beecham J, Knapp M. Costing psychiatric interventions. In: Thornicroft G, editor. Measuring mental health needs. 2nd ed. London: Gaskell; 2001.
Clarke PM, Fiebig DG, Gerdtham UG. Optimal recall length in survey design. J Health Econ. 2008;27(5):1275–84.
Department of Finance (An Roinn Airgeadais) Ireland. Test discount rate. 2010. Available at: http://www.finance.gov.ie/viewdoc.asp?DocID=5387. Accessed 31 July 2013.
Central Statistics Office. Earnings and labour costs. Ireland: Central Statistics Office; 2013.
Kurtzke JF. Rating neurologic impairment in multiple sclerosis: an Expanded Disability Status Scale (EDSS). Neurology. 1983;33(11):1444–52.
The Multiple Sclerosis Society of Ireland. http://www.ms-society.ie/pages/living-with-ms. Accessed 31 July 2014.
Health Service Executive Primary Care Reimbursement Service (HSE-PCRS). Statistical analysis of claims and payments 2011. Dublin 2012.
Association of British Neurologists. Revised (2009) Association of British neurologists’ guidelines for prescribing in multiple sclerosis. London; 2009.
Goodin DS, Frohman EM, Garmany GP Jr, Halper J, Likosky WH, Lublin FD, et al. Disease modifying therapies in multiple sclerosis: report of the therapeutics and technology assessment subcommittee of the American Academy of Neurology and the MS council for clinical practice guidelines. Neurology. 2002;58(2):169–78.
Larg A, Moss JR. Cost-of-illness studies: a guide to critical evaluation. Pharmacoeconomics. 2011;29(8):653–71.
Rotstein DL, Mamdani M, O’Connor PW. Increasing use of disease modifying drugs for MS in Canada. Can J Neurol Sci. 2010;37(3):383–8.
Goodin DS, Jones J, Li D, Traboulsee A, Reder AT, Beckmann K, et al. Establishing long-term efficacy in chronic disease: use of recursive partitioning and propensity score adjustment to estimate outcome in MS. PLoS One. 2011;6(11):e22444.
Shirani A, Zhao Y, Karim ME, Evans C, Kingwell E, Van Der Kop ML, et al. Association between use of interferon beta and progression of disability in patients with relapsing-remitting multiple sclerosis. JAMA J Am Med Assoc. 2012;308(3):247–56.
Karampampa K, Gustavsson A, van Munster ET, Hupperts RM, Sanders EA, Mostert J et al. Treatment experience, burden, and unmet needs (TRIBUNE) in multiple sclerosis study: the costs and utilities of MS patients in The Netherlands. J Med Econ. 2013. doi:10.3111/13696998.2013.807267.
OECD Average Annual Wages. 2011. Available at: http://stats.oecd.org/Index.aspx?DataSetCode=AV_AN_WAGE. Accessed 13 June 2013.
Health Service Executive (HSE) Casemix Unit: ready reckoner of acute hospital inpatient activity and costs (summarised by DRG) relating to 2010 costs and activity. 2012.
Nursing home support scheme cost of care in public nursing homes. 2011. Available at: http://www.hse.ie/eng/services/list/4/olderpeople/nhss/costhse.pdf. Accessed 13 June 2013.
Nursing homes support scheme maximum agreed prices with private and voluntary nursing homes. 2012. Available at: http://www.irishnursinghomes.ie/CostofCarePrivateandVoluntaryNursingHomes.pdf. Accessed 13 June 2013.
Madden D, Nolan A, Nolan B. GP reimbursement and visiting behaviour in Ireland. Health Econ. 2005;14(10):1047–60. doi:10.1002/hec.995.
Consolidated salary scales in accordance with financial emergency measures in the public interest (No. 2) Act 2009 (No. 41 of 2009). Available at: http://www.hse.ie/eng/staff/Benefits_Services/pay/Payscalesjan2010.pdf. Accessed 13 June 2013.
Primary care reimbursement service. Reimbursable items. http://www.sspcrs.ie/druglist/search.jsp. Accessed 13 June 2013.
Acknowledgments
We have no conflicts of interest. No funding was received for this study.
Author contributions
The study was conceptualised and initiated by EF. All authors contributed to the study design. Data acquisition was conducted by EF, NT and CMcG. EF and CW performed the study analyses. EF drafted the manuscript. All authors contributed to revisions of the manuscript and critically revised the manuscript for intellectual content. EF is the guarantor for the overall content.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Fogarty, E., Walsh, C., McGuigan, C. et al. Direct and Indirect Economic Consequences of Multiple Sclerosis in Ireland. Appl Health Econ Health Policy 12, 635–645 (2014). https://doi.org/10.1007/s40258-014-0128-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40258-014-0128-3