Abstract
Purpose
Lifestyle changes in diabetes mellitus leads to metabolic syndrome, thus resulting in a hike in micro and macrovascular complications in diabetes mellitus patients. The main objective of the study was to identify the occurrence of metabolic syndrome and to evaluate the gender-associated difference in each component of metabolic syndrome by using International Diabetic Federation (IDF) and National Cholesterol Education Program Adult Treatment Panel III (NCEP ATP III)criteria.
Methods
This is a cross-sectional study conducted in 350 type II diabetes mellitus patients. All the study participants within 30–80 years were enrolled. Subjects with type I DM and pregnant women were excluded from the study.
Results
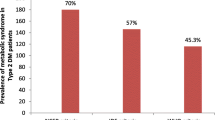
The occurrence of metabolic syndrome among the diabetic population was found to be 42.28% and 28.85% using the IDF and the NCEP ATP III criteria respectively. It was observed that the prevalence was found to be higher in females than males as per IDF and NCEP ATP III criteria and was found to be statistically significant (p < 0.001). Central obesity elevated blood pressure, and reduced high-density lipoprotein was significantly higher in female patients. The most frequently occurring risk factor in this study population was central obesity followed by hypertension. A comparative analysis of IDF and NCEP ATP III criteria implies that when compared to diabetes patients without metabolic syndrome, all the metabolic risk elements were significantly higher in diabetes patients with metabolic syndrome.
Conclusions
This study concluded that the occurrence of metabolic syndrome was dreadfully high among the diabetic population, especially among female subjects.


Similar content being viewed by others
References
Khanal P, Mandar BK, Patil BM, Hullatti KK. In silico Antidiabetic Screening of Borapetoside C, Cordifolioside A and Magnoflorine. Indian J Pharm Sci. 2019; 81: 550 – 55.
Khanal P, Patil BM, Mandar BK, et al. Network pharmacology-based assessment to elucidate the molecular mechanism of anti-diabetic action of Tinospora cordifolia. Clin Phytosci. 2019;5:35.
James M, Varghese TP, Vijayan A, Anagha PP, Muhas C, Hyder M. Link between Metabolic Syndrome and Diabetes Mellitus: A Pathophysiological Implication. Int J Sci Technol Res. 2019;11:1935–40.
Rezaianzadeh A, Namayandeh SM, Sadr SM. National Cholesterol Education Program Adult Treatment Panel III Versus International Diabetic Federation Definition of Metabolic Syndrome, Which One is Associated with Diabetes Mellitus and Coronary Artery Disease? Int J Prev Med. 2012;3:552–58.
Faizal R, George L, Lakshmanan P, Varghese TP. Assesment of diabetes related quality of life and the impact of pharmaceutical care in its improvement. J Coastal Life Med. 2016: 4; 649 – 51.
Nsiah K, Shang O, Boateng KA, Mensah FO. Prevalence of metabolic syndrome in type 2 diabetes mellitus patients. Int J Appl Basic Med Res. 2015;5:133–38.
Ford ES, Giles WH, Dietz WH. Prevalence of the metabolic syndrome among US adults: Findings from the third National Health and Nutrition Examination Survey. JAMA. 2002;287:3569.
Huang P. A comprehensive definition for metabolic syndrome. Dis Model Mech. 2009;2:231–37.
Felix Val K, Titty WK, Owiredu WK, Agyei Frimpong MT. Prevalence of metabolic syndrome and its components among diabetes patients in Ghana. J Biol Sci. 2008;8:105761.
Linu Mohan P, Jishnu NA, Remya PJ. Prevalence of metabolic syndrome in psychiatric OP patients in tertiary care hospital, Kerala. Indian J Pharm Pract. 2012;5:58–61.
Mawlieh BS, Shastry CS, Chand S. Evaluation of anti-diabetic activity of two marketed herbal formulations. Research J Pharm Tech. 2020;13:664 – 68.
Mayer-Davis EJ, et al. Intensity and amount of physicial activity in relation to insulin sensitivity: the insulin resistance atherosclerosis study. J Am Med Assoc. 1998;279:669–74.
Nsiah K, Shang VO, Boateng KA, Mensah FO. Prevalence of metabolic syndrome in type 2 diabetes mellitus patients. Int J Appl Basic Med Res. 2015;5:133–38.
White UA, Tchoukalova YD. Sex dimorphism and depot differences in adipose tissue function. Biochim Biophys Acta. 2014 Mar;1842:377–92.
Xiao J, Li Wu C, Gao YX, Wang SL, Wang L, Yun Lu Q, Wang XJ, et al. Prevalence of metabolic syndrome and its risk factors among rural adults in Nantong, China. Sci Rep. 2016;6:38089.
Bhat RA, Laway BA, Zargar AH. Prevalence of metabolic syndrome in Kashmir valley of Indian subcontinent. Indian J Med Sci. 2010;64:259–64.
Yadav D, Mahajan S, Subramanian SK, Bisen PS, Chung CH, Prasad GB. Prevalence of metabolic syndrome in type 2 diabetes mellitus using NCEP-ATPIII, IDF and WHO definition and its agreement in Gwalior Chambal region of Central India. Glob J Health Sci. 2013;17:5:142–55.
Sawant A, Mankeshwar R, Shah S, Raghavan R, Dhongde G, Raje H, et al. Prevalence of metabolic syndrome in urban India. Cholesterol. 2011;2011:920983.
Peterson PN, Spertus JA, Magid DJ, Masoudi FA, Reid K, Hamman RF, et al. The impact of diabetes on one year health status outcomes following acute coronary syndrome. BMC Cardiovasc Disord. 2006;6;41.
Zafar U, Khaliq S, Ahmad HU, Manzoor S, Lone KP. Metabolic syndrome: an update on diagnostic criteria, pathogenesis, and genetic links. Hormones (Athens). 2018;17:299–13.
Sharma KK, Mathur Mukul, Lodha S, Sharma SK, Sharma N, Gupta R. Study of differences in presentation, risk factors and management in diabetic and nondiabetic patients with acute coronary syndrome. Indian J Endocrinol Metab. 2016;20:354–58.
Supriya Simon A, Dinesh Roy D, Jayapal V, Vijayakumar T. Biochemical and genetic studies on cardiometabolic syndrome. Indian J Clin Biochem. 2010;25:164–68.
Chiolero A, Faeh D, Paccaud F, Cornuz J. Consequences of smoking for body weight, body fat distribution, and insulin resistance. Am J Clin Nutr. 2008;87:801–09.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
On behalf of all authors, the corresponding author states that there is no conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
James, M., Varghese, T.P., Sharma, R. et al. Association Between Metabolic Syndrome and Diabetes Mellitus According to International Diabetic Federation and National Cholesterol Education Program Adult Treatment Panel III Criteria: a Cross-sectional Study. J Diabetes Metab Disord 19, 437–443 (2020). https://doi.org/10.1007/s40200-020-00523-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-020-00523-2