Abstract
Background
Acromegaly is a rare chronic disabling disorder, in which growth hormone (GH) excess is associated with a range of clinical features and systemic complications. The present study aims to evaluate the association between pretreatment basal GH levels as well as GH levels after oral glucose tolerance test (OGTT) and cardio-metabolic comorbidities, including diabetes mellitus (DM), left ventricular hypertrophy (LVH) and hypertension (HTN) in patients with active acromegaly.
Methods
A retrospective study of the medical records regarding 113 patients with acromegaly registered at two main centers of Iran Pituitary Tumor Registry during 2011–2018.
Results
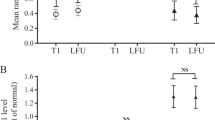
The mean age of the patients was 42.76 ± 11.6 (range: 21–72) years. Mean GH level at baseline was 21 ng/ml while nadir GH levels at 60 and 120 min after glucose were 6.95 and 9.05 ng/ml, respectively. There was a negative correlation between age and basal serum GH level (r= -0.196, p = 0.038). Hypertension and diabetes mellitus were detected in 26.8% and 19.7% of the patients. A positive correlation was detected between serum GH values and systolic blood pressure. There was not any significant difference in basal GH and GH post OGTT regarding DM, Diastolic blood pressure and LVH.
Conclusions
Our findings suggest that pretreatment basal GH levels are higher in younger patients with acromegaly. Furthermore, higher GH values (0, 60 and 120 min) during OGTT are associated with higher systolic blood pressure. A comprehensive evaluation of this population regarding comorbidities should be performed.

Similar content being viewed by others
References
Kauppinen-Mäkelin R, Sane T, Reunanen A, Välimäki MJ, Niskanen L, Markkanen H et al (2005) A nationwide survey of mortality in acromegaly. J Clin Endocrinol Metab 90(7):4081–6
Melmed S (2006) Acromegaly. New England. J Med 355(24):2558–73
Colao A, Amato G, Pedroncelli A, Baldelli R, Grottoli S, Gasco V et al (2002) Gender-and age-related differences in the endocrine parameters of acromegaly. J Endocrinol Investig 25(6):532–8
Katznelson L, Laws ER Jr, Melmed S, Molitch ME, Murad MH, Utz A et al (2014) Acromegaly: an endocrine society clinical practice guideline. J Clin Endocrinol Metab 99(11):3933–51. https://doi.org/10.1210/jc.2014-2700
Holdaway IM (2007) Excess mortality in acromegaly. Horm Res 68(Suppl 5):166–72
Ramos-Levi AM, Marazuela M (2017) Cardiovascular comorbidities in acromegaly: an update on their diagnosis and management. Endocrine 55(2):346–59. https://doi.org/10.1007/s12020-016-1191-3
Melmed S, Colao A, Barkan A, Molitch M, Grossman AB, Kleinberg D et al (2009) Guidelines for acromegaly management: an update. J Clin Endocrinol Metab 94(5):1509–17. https://doi.org/10.1210/jc.2008-2421
Vitale G, Pivonello R, Auriemma RS, Guerra E, Milone F, Savastano S et al (2005) Hypertension in acromegaly and in the normal population: prevalence and determinants. Clin Endocrinol 63(4):470–6. https://doi.org/10.1111/j.1365-2265.2005.02370.x
Rieger A, Rainov NG, Ebel H, Sanchin L, Shibib K, Helfrich C et al (1997) Factors predicting pituitary adenoma invasiveness in acromegalic patients. Neurosurg Rev 20(3):182–7
Powlson AS, Gurnell M (2016) Cardiovascular Disease and Sleep-Disordered Breathing in Acromegaly. Neuroendocrinology 103(1):75–85. https://doi.org/10.1159/000438903
Bondanelli M, Ambrosio MR, degli Uberti EC (2001) Pathogenesis and prevalence of hypertension in acromegaly. Pituitary 4(4):239–49
Frara S, Maffezzoni F, Mazziotti G, Giustina A (2016) Current and emerging aspects of diabetes mellitus in acromegaly. Trends Endocrinol Metab 27(7):470–83. https://doi.org/10.1016/j.tem.2016.04.014
James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, Handler J et al (2014) 2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8). JAMA 311(5):507–20. https://doi.org/10.1001/jama.2013.284427
American Diabetes A (2015) (2) Classification and diagnosis of diabetes. Diabetes Care 38 Suppl(Supplement 1):S8–S16. https://doi.org/10.2337/dc15-S005
Haliloglu O, Kuruoglu E, Ozkaya HM, Keskin FE, Gunaldi O, Oz B et al (2016) Multidisciplinary approach for acromegaly: A single tertiary center’s experience. World Neurosurg 88:270–6. https://doi.org/10.1016/j.wneu.2015.12.092
Petersenn S, Buchfelder M, Gerbert B, Franz H, Quabbe HJ, Schulte HM et al (2009) Age and sex as predictors of biochemical activity in acromegaly: analysis of 1485 patients from the German Acromegaly Register. Clin Endocrinol 71(3):400–5. https://doi.org/10.1111/j.1365-2265.2009.03547.x
Petrossians P, Daly AF, Natchev E, Maione L, Blijdorp K, Sahnoun-Fathallah M et al (2017) Acromegaly at diagnosis in 3173 patients from the Liège Acromegaly Survey (LAS) Database. Endocr Relat Cancer 24(10):505–18. https://doi.org/10.1530/ERC-17-0253
Colao A, Ferone D, Marzullo P, Lombardi G (2004) Systemic complications of acromegaly: epidemiology, pathogenesis, and management. Endocr Rev 25(1):102–52. https://doi.org/10.1210/er.2002-0022
Schilbach K, Nicolay SS, Haenelt M, Lechner A, Gar C, Schopohl J et al (2017) Diagnosis of acromegaly: Sex and BMI are the major determinants of growth hormone suppression during oral glucose tolerance test (OGTT)
Dal J, Feldt-Rasmussen U, Andersen M, Kristensen L, Laurberg P, Pedersen L et al (2016) Acromegaly incidence, prevalence, complications and long-term prognosis: a nationwide cohort study. Eur J Endocrinol 175(3):181–90
Park JY, Kim JH, Kim SW, Chung JH, Min Y-K, Lee M-S et al (2014) Using Growth Hormone Levels to Detect Macroadenoma in Patients with Acromegaly. Endocrinol Metab 29(4):450–6
Iuchi S, Saeki N, Uchino Y, Higuchi Y, Tatsuno I, Nakamura S et al (2000) Cavernous sinus invasion and tumor proliferative potential of growth hormone-producing pituitary tumors. Endocr J 47(Suppl):77–9
Alexopoulou O, Bex M, Kamenicky P, Mvoula AB, Chanson P, Maiter D (2014) Prevalence and risk factors of impaired glucose tolerance and diabetes mellitus at diagnosis of acromegaly: a study in 148 patients. Pituitary 17(1):81–9. https://doi.org/10.1007/s11102-013-0471-7
Arosio M, Reimondo G, Malchiodi E, Berchialla P, Borraccino A, De Marinis L et al (2012) Predictors of morbidity and mortality in acromegaly: an Italian survey. Eur J Endocrinol 167(2):189–98. https://doi.org/10.1530/eje-12-0084
Fieffe S, Morange I, Petrossians P, Chanson P, Rohmer V, Cortet C et al (2011) Diabetes in acromegaly, prevalence, risk factors, and evolution: data from the French Acromegaly Registry. Eur J Endocrinol 164(6):877–84
Portocarrero-Ortiz LA, Vergara-Lopez A, Vidrio-Velazquez M, Uribe-Diaz AM, Garcia-Dominguez A, Reza-Albarran AA et al (2016) The Mexican Acromegaly Registry: Clinical and Biochemical Characteristics at Diagnosis and Therapeutic Outcomes. J Clin Endocrinol Metab 101(11):3997–4004. https://doi.org/10.1210/jc.2016-1937
Espinosa-de-los-Monteros AL, Gonzalez B, Vargas G, Sosa E, Mercado M (2011) Clinical and biochemical characteristics of acromegalic patients with different abnormalities in glucose metabolism. Pituitary 14(3):231–5. https://doi.org/10.1007/s11102-010-0284-x
Fedrizzi D, Rodrigues TC, Costenaro F, Scalco R, Czepielewski MA (2011) Hypertension-related factors in patients with active and inactive acromegaly. Arq Bras Endocrinol Metabol 55(7):468–74
Amado A, Araújo F, Carvalh D (2018) Cardiovascular risk factors in acromegaly: What’s the impact of disease control? Exp Clin Endocrinol Diabetes 26(8):505–512
Sacca L, Napoli R, Cittadini A (2003) Growth hormone, acromegaly, and heart failure: an intricate triangulation. Clin Endocrinol 59(6):660–71. https://doi.org/10.1046/j.1365-2265.2003.01780.x
Sardella C, Cappellani D, Urbani C, Manetti L, Marconcini G, Tomisti L et al (2016) Disease activity and lifestyle influence comorbidities and cardiovascular events in patients with acromegaly. Eur J Endocrinol 175(5):443–53. https://doi.org/10.1530/eje-16-0562
Ohtsuka H, Komiya I, Aizawa T, Yamada T (1995) Hypertension in acromegaly: hereditary hypertensive factor produces hypertension by enhancing IGF-I production. Endocr J 42(6):781–7
Vitale G, Galderisi M, Pivonello R, Spinelli L, Ciccarelli A, De Divitiis O et al (2004) Prevalence and determinants of left ventricular hypertrophy in acromegaly: impact of different methods of indexing left ventricular mass. Clin Endocrinol 60(3):343–9. https://doi.org/10.1111/j.1365-2265.2004.01985.x
Colao A, Marzullo P, Di Somma C, Lombardi G (2001) Growth hormone and the heart. Clin Endocrinol 54(2):137–54. https://doi.org/10.1046/j.1365-2265.2001.01218.x
Funding
This study was funded by Tehran University of Medical Sciences (TUMS) and Endocrinology and Metabolism Research Institute affiliated to TUMS (Grant number 1396-01-98-2146).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
*This paper is derived from the dissertation of Dr. Leila Hedayati for obtaining internal medicine specialty.
Rights and permissions
About this article
Cite this article
Hedayati Zafarghandi, L., Khamseh, M.E., Fooladgar, M. et al. Pretreatment serum GH levels and cardio-metabolic comorbidities in acromegaly; analysis of data from Iran Pituitary Tumor Registry. J Diabetes Metab Disord 19, 319–325 (2020). https://doi.org/10.1007/s40200-020-00512-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40200-020-00512-5