Abstract
In this review we discuss the role of intraocular surgery preoperative prophylaxis. The correct choice of antimicrobial drug is variable in each surgical setting, according to the available strengths of evidence, the anatomical district involved, and the type of procedure. In the ophthalmic surgical field, there has been a progressive shift from antibiotic formulations, which are known to cause antibiotic resistance, to a new class of antiseptic compounds, which proved to be effective not only against bacteria, but also against fungi, protozoa, and viruses. Among these, povidone–iodine (PVI) is a water-soluble polymer that can form a complex with iodine, and the perioperative application of PVI 5–10% eye drop for 3 min is the gold standard for infection prophylaxis. A new formulation of 0.6% PVI eye drop is a new option for infection prophylaxis in the days before surgery. Chlorhexidine is a biguanide compound, which is a valid alternative with a good safety and efficacy profile and is the antiseptic of choice in patients with iodine allergy. New compounds that are currently being studied include polyhexamethylene biguanide (PHMB), picloxydine, ozone, hypochlorous acid (HOCl), and Biosecur. PHMB is a biguanide polymer that was found to be more effective than PVI in in vitro studies for reducing microorganisms and extending the duration of antisepsis, but to date, there are no formulations available on the market for preoperative ocular surgery in which it is present as main ingredient. Ozone is a molecule with oxidizing effect, which showed interesting preliminary results but is not effective against virus, Staphylococcus aureus and Candida albicans. HOCl has a natural bactericidal propriety but its applicability to prophylaxis of ocular infection in the setting of ocular surgery is not established. Biosecur is a non-toxic organic alcohol-free compound that exhibited bactericidal and fungicidal effect versus all common microorganisms and is currently available as an ocular spray.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Why carry out this study? |
Preoperative prophylaxis is essential to minimizing surgery-related infections and can be achieved with a new class of antiseptic compounds that showed effects against bacteria, fungi, protozoa, and viruses. |
Newly introduced formulations with lower concentration of povidone–iodine or chlorhexidine are used in the preoperative days to reduce the conjunctival bacterial load. |
In vitro/vivo studies are assessing the efficacy of new compounds, including PHMB, picloxydine, ozone, hypochlorous acid, and Biosecur. |
A correct risk management protocol for infection prophylaxis may reduce healthcare-acquired infections and the related medical–legal disputes. |
What was learned from the study? |
Prophylaxis of infection represents a crucial step of intraocular surgery. Povidone–iodine is a compound well studied in the literature, and it is broadly used even if at different concentrations. Chlorhexidine is becoming more used as published studies demonstrate good safety and efficacy profiles with reduced patient discomfort. Moreover, there are new compounds such as picloxydine, ozone, hypochlorous acid, and Biosecur that showed very interesting preliminary results. |
Introduction
Preoperative prophylaxis is the standard of care before ophthalmic surgery to reduce the risk of postoperative infections [1, 2]. Different strategies for ocular antisepsis are adopted preoperatively to decrease the number of pathological microorganisms residing in the ocular surface at the time of surgery. The survey of the European Observatory of Cataract Surgery suggested a considerable level of heterogeneity among European countries in the use of antiseptics both before and in the operating room [3]. Grzybowski et al. compared various endophthalmitis prophylaxis patterns around the world and concluded that there is no global consensus regarding endophthalmitis prophylaxis with cataract surgery [4].
In particular, povidone–iodine (PVI) solution is considered the most effective antiseptic to reduce postoperative endophthalmitis rates [1, 5, 6]. In 1984, Apt et al. first demonstrated the effect of PVI on the conjunctiva with a reduction of nearly 90% of the ocular surface flora [7]. There is evidence from several studies that the bacteria residing in the lids, tear film, and adnexa are the main agents responsible for infection. In fact, most common microorganisms implicated in postoperative endophthalmitis are coagulase-negative staphylococci (CNS), especially Staphylococcus epidermidis and Staphylococcus aureus [8, 9]. These organisms are the most common in patient’s own flora from the eyelid and conjunctiva [10]. Using molecular epidemiological techniques in the case of endophthalmitis, microbes isolated from the vitreous were found to be genetically indistinguishable from conjunctival organisms isolated from the patient’s eyelid in more than 80% of cases [8]. In this scenario, preoperative prophylaxis plays a key role in the prevention of postoperative endophthalmitis. In 2013, the European Society of Cataract and Refractive Surgeons (ESCRS) published the “Guidelines for Prevention and Treatment of Endophthalmitis Following Cataract Surgery,” highlighting unequivocally the clinical benefit of the use of the intracameral injection of cefuroxime at the end of cataract surgery thanks to the fivefold reduction in postoperative endophthalmitis rates [11]. At the same time, the use of PVI applied as ophthalmic solution to the cornea, conjunctival sac, and periocular skin immediately prior to surgery is considered mandatory. Surgical disciplines, including ophthalmic surgery, play a key role in healthcare-acquired infections and related medical malpractice cases. Intraocular procedures expose an unavoidable risk of endophthalmitis, and therefore ophthalmic surgery is highly involved in medico–legal controversies, showing a litigation/conviction ratio higher than in other specialties.
Currently, there is no universal consensus regarding the use of ophthalmic preparations in the form of eye drop, spray, or medicated wipes in the days before the surgery [11]. This review aims at highlighting the recent evidence and controversies in the field of preoperative prophylaxis of infection during ophthalmic surgery. Furthermore, since surgical disciplines, including ophthalmic surgery, suffer from the risk of healthcare-acquired infections and are highly involved in medico–legal controversies, a particular focus will be placed on this issue.
This review is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Traditional Use of Antibiotics
Preoperative prophylaxis with topical antibiotics has been widely used in the past. The main class of antibiotics studied is fluoroquinolones, and all studies demonstrated a reduction in conjunctival bacterial load. Specifically, multiple studies showed a synergic effect between the use of topical levofloxacin 0.3% on the preoperative day and PVI irrigation to reduce the conjunctival bacteria load [12, 13]. Moxifloxacin and gatifloxacin showed similar results and the application four times a day, both one day and three days before surgery, was equally effective in the reduction of colony-forming units (CFU) [14, 15]. Although the efficacy is well established, comparative studies of both moxifloxacin and gatifloxacin against PVI 5% have shown no significant effects on further reduction in the bacterial colonization rate [16, 17].
Regarding the relationship between topical therapy with preoperative antibiotics and endophthalmitis, an observational and cross-sectional study focused on the incidence of this complication after cataract extraction on 464,996 operations reported that short-term topical antibiotics given as add-on prophylaxis did not confer a clear-cut benefit in addition to intracameral antibiotics to reduce the rate of endophthalmitis [18].
Hence, preoperative topical antibiotics do not add any clear supplementary efficacy over PVI alone to reduce the incidence of endophthalmitis. Additionally, the routine use of preoperative fluoroquinolones may select a fluoroquinolone-resistant conjunctival flora [19, 20]. For these reasons, the preoperative use of topical antibiotics is not advisable.
Antiseptics and Disinfectants
In the last few years, trends in endophthalmitis prophylaxis have changed significantly. Different drugs have been adopted for ocular antisepsis to decrease the overgrowth of pathological microorganisms before the surgery. Antiseptics are biocides or products that destroy or inhibit the growth of microorganisms in or on living tissue. Antiseptics have shown numerous advantages over antibiotics. First, they have a wide range of mechanisms that makes them active not only against bacteria, but also against fungi, protozoa, and viruses [21, 22]. In addition, they do not have a selective mechanism of action, and this makes antiseptics less susceptible to the development of resistance by microorganisms. Finally, their effectiveness is not affected by the presence of a biofilm [23].
Thanks to these characteristics, antiseptics have established themselves as leaders in preoperative prophylaxis in ophthalmic surgery as well. The following sections will describe the antiseptics used in preoperative prophylaxis, in vitro and in vivo evidence of their efficacy, and the main comparison studies (Table 1).
Povidone–Iodine (0.6% and 5–10%)
Povidone-iodine (PVI), also known as polyvinylpyrrolidone, is a water-soluble polymer with a high molecular weight that can form a complex with iodine [24]. Free iodine released from the complex provides antimicrobial action with a significant decrease in the microbial flora, bacteria, viruses, fungi, and protozoans [7, 25, 26]. A typical chemical property of this iodophor is that the concentration of free iodine increases with the dilution of PVI due to a weakening of the chemical bonding between iodine and povidone [27]. In clinical practice, different studies revealed the safety and tolerability profile of PVI on the ocular surface; however, due to corneal endothelial cell toxicity it cannot be used inside the eye [28, 29]. Despite different concentrations of PVI having been used, the ESCRS recommends applying PVI 5–10% to reach bactericidal efficacy to the cornea, conjunctival sac, and periocular skin for a minimum of 3 min before surgery [11, 30]. Ta et al. demonstrated that PVI at 5% used for 1 min is quicker, less toxic, and equally effective than PVI at 10% in preparation for ocular surgery. In addition, the rate of aqueous humor contamination at the end of surgery did not differ significantly between groups [27]. Results from another study showed that repeated irrigation of the operative field with 0.25% PVI during cataract surgery achieved a very low bacterial contamination rate in the anterior chamber [31]. To date, the use of PVI formulations has become the single most effective method of preoperative antisepsis. However, PVI at 5% cannot be used as preparation for ocular surgery during the preoperative days due to its irritant effects related to the duration of exposure; on the contrary, if used at lower concentrations (0.5–1%) it is less toxic and relatively safe [32]. This low concentration needs only a few seconds to kill bacteria, but unfortunately, has a short duration of cytotoxic effect, requiring frequent applications [33, 34].
Several formulations were used as preoperative prophylaxis prior to cataract surgery. In 2021 Musumeci et al. demonstrated that 0.6% PVI eye drop (IODIM, Medivis, Catania, Italy) used for 3 days in patients who underwent cataract surgery were effective in reducing the conjunctival bacterial load [35]. Accordingly, Pinna et al. showed that 0.6% PVI eye drop had rapid in vitro antimicrobial activity against common etiologic agents of ocular infection, such as S. epidermidis, S. aureus, and P. aeruginosa [36]. In vivo non-prospective studies reported the effectiveness of 0.6% PVI eye drop treatment in reducing the conjunctival bacterial load [37, 38]. According to published results, PVI eye drop at low concentrations (0.6%) is efficacious in preoperative prophylaxis, allowing for the eradication of conjunctival bacteria and ensuring satisfactory ocular tolerability.
Chlorhexidine (CHX)
Chlorhexidine is a biguanide compound whose activity is dependent on the pH of the environment; the optimal range is between 5.5 and 7.0 [21]. CHX is a cationic molecule able to bind to negatively charged bacterial membrane phospholipids [39]. Antimicrobial CHX effect is dose dependent; in particular, it presents bacteriostatic activity at low concentrations (0.02–0.06%) and bactericidal activity at higher concentrations (> 0.12%) [40]. Overall, it has a wide spectrum activity against Gram-positive and Gram-negative bacteria, some yeasts, and some viruses [41]. The ESCRS supports the use of CHX 0.05% for ocular surface preparation as measures for ocular antisepsis in patients with iodine allergy [11]. Merani et al. reported that CHX 0.05% or 0.1% was well tolerated and associated with a low rate of post-intravitreal injection endophthalmitis [42]. Additionally, Oakley et al. reported an endophthalmitis rate of 0.023% in 4322 intravitreal injections using aqueous chlorhexidine gluconate (0.1% Pfizer, New York) [43]. This is comparable with the published rates of PVI [44].
However, it is important to use an aqueous solution of CHX gluconate rather than preparations containing alcohol or detergents, which have been shown to cause epithelial, stromal, and endothelial toxicity, and in the most severely affected cases, permanent stromal scarring or bullous keratopathy [45, 46]. The current understanding of CHX bacterial activity profiles shows resistance among methicillin-resistant Staphylococcus aureus and other staphylococci. Furthermore, it is inactive against Enterobacteriaceae, Pseudomonas aeruginosa, all Actinobacteria spp., and all spores [23]. In 1999, CHX was used in Sweden in combination with intracameral cefuroxime in cataract surgery with a postoperative endophthalmitis rate that was stable at around 0.02% [47, 48]. At the same time, in Australia the use of CHX instead of PVI before intravitreal injections did not record changes in the endophthalmitis rates [42].
Dropsept (Iromed Group s.r.l, Rome, Italy), a new preparation based on CHX 0.02%, Vitamin E and D-a-Tocopherol polyethylene glycol 1000 succinate, was recently introduced. An in vitro study by Tognetto et al. showed a good antiseptic activity against E. coli, a weaker activity against the staphylococci strains and P. aeruginosa, while Candida albicans was not affected [49]. Similar in vitro results were shown by Caruso et al., with effective bactericidal activity on S. aureus, S. epidermidis, and Escherichia coli, but with no inhibitory effect on the growth of P. aeruginosa. In addition, Dropsept showed antiviral activity against HAdV-2 and HCoV-OC43 and amoebicidal activity [50]. These in vitro results are very interesting and promising, but in vivo studies using Dropsept or CHX at a concentration of 0.02% have yet to be performed to confirm its effectiveness in the prophylaxis of post-surgical endophthalmitis as well as its ocular tolerability.
Polyhexamethylene Biguanide (PHMB)
Polyhexamethylene biguanide (PHMB) is a biguanide polymer used as a compound in preservative, disinfectant, and broad-spectrum antiseptic [51, 52]. Biguanides are potent chemical bases, and as a result, PHMB compounds have a high positive charge at physiological pH [53]. In the past, it was believed that the mechanism of action was mostly based on the disruption of microbial membranes [52, 54,55,56], but more recently, the ability to specifically bind and compress bacterial DNA, halting bacterial cell division, has been reported. This mechanical antibacterial method of action might contribute to the explanation of the minimal incidence of antibiotic resistance associated with the use of PHMB, despite considerable testing since its synthesis [52]. PHMB has been shown as effective against a broad range of infections, including Acanthamoeba castellanii [57], S. epidermidis [54, 57], and E. coli strains [52, 54]. The segregation of the polymer into endosomes, which appears to protect the nucleus from its negative effects, leaves mammalian cells mostly unaffected by it [52]. In addition, in comparison to other antimicrobials, PHMB resulted in quicker wound healing [58]. A prospective, randomized, double-masked controlled trial in 90 healthy volunteers was conducted to assess the safety and tolerability of preservative-free PHMB at three dosage levels (0.04%, 0.06%, and 0.08%). Except for corneal punctate keratopathy caused by PHMB 0.08%, which healed completely in 7–14 days, there was no tendency for an increased incidence of any mild adverse events (AEs) as PHMB concentrations rose [59]. Randomized clinical research found that PHMB was more effective than PVI at reducing microorganisms and extending the duration of antisepsis [60]. Ristau et al. showed a low incidence of endophthalmitis following intravitreal injections (IVIs) using polyhexanide as an antiseptic, which was equivalent to the incidence in earlier trials using PVI [61]. To the best of our knowledge, despite PHMB being present as a preservative in several eye drops, there are no formulations available on the market for preoperative ocular surgery that have it as main ingredient.
Picloxydine Dihydrochloride
Picloxydine dihydrochloride is another biguanide with significant antiseptic power. There are few studies in the literature showing its efficacy in the setting of ophthalmology. Budzinskaya et al. showed the efficacy of eye antiseptic picloxydine 0.05% against conjunctival bacteria in patients undergoing intravitreal injections [62]. Three different formulations containing Picloxydine are commercially available: Vitabact (Thea Pharma GmbH; Ciba Vision; Novartis Crop, Novartis; Excelvision, O.C.A.), Medibact (Medipak), and Bactavit (Rompharm). More studies on this molecule are needed to provide robust results.
Ozone
Ozone is a molecule with oxidizing effect that has been extensively studied for its antiseptic and antiinflammatory properties [63,64,65,66]. The mechanism of action is based on penetration of ozonides into the wall of the target pathogen and hydrolyzation, forming reactive oxygen species that alter the pathogen proteins, lipids, and DNA/RNA [67].
A specific ophthalmic formulation has been recently developed composed of ozonized oil 0.5% in liposomes plus hypromellose (Ozodrop, FB VISION S.p.A., San Benedetto del Tronto, Italy). Caruso et al. showed an inhibition of the growth of S. epidermidis and E. coli in vitro after 24 h, and S. aureus and P. aureginosa after only 7 days. Ozodrop did not exert any antiviral activity and antiamoebic effect [50]. Again in vitro, Tognetto et al. showed antimicrobial efficacy of Ozodrop against S. epidermidis, E. coli, and P. aeruginosa. Moreover, no activity was detected against S. aureus strains and C. albicans [49]. Focusing on the anti-Candida effect, Celenza et al. showed an antifungal effect on several Candida species [65]. Regarding clinical studies, Spadea et al. published the results of an interventional, non-randomized, clinical study on patients undergoing cataract surgery [67]. This study showed a reduction of > 90% in microbial load in > 90% of the samples presented in the group treated with Ozodrop, with optimal ocular tolerability. Liposomal ozonated oil has shown similar effects to other traditional antiseptics, with a wide antimicrobial power and a low rate of adverse events [49, 50]. Therefore, it may be an interesting option before ophthalmic surgery as an alternative to traditional compounds.
Hypochlorous Acid
Hypochlorous acid (HOCl) has a natural bactericidal propriety since it is generated as a portion of the cytotoxic myeloperoxidase in neutrophils [68]. In vitro studies demonstrated that HOCl triggers oxidation of nucleotides, deactivation of cell enzymes, interruption of cell membranes and prompt cell lysis [69]. Therefore, HOCl is potentially a highly active compound versus all infectious human pathogens. Furthermore, HOCl was not toxic when used on the ocular surface, making it an established adjuvant to manage eye infections [70]. However, its applicability to prophylaxis of infection in the setting of ocular surgery is not established. A study by Kanclerz et al. reported results of conjunctival swabs performed in patients undergoing cataract surgery that were randomized to either 10% PVI or HOCl solution; according to their results there was a significant difference, with the HOCl group reporting a higher number of positive swabs [71]. An advantage of the HOCl group was the significantly lower level of discomfort. Overall, more evidence is needed, and currently, there is an ongoing open-label, single-group clinical trial (NCT04568213) testing the effect of HOCl disinfection on ocular flora prior to cataract surgery [72].
Biosecur
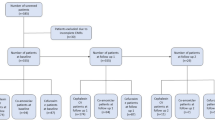
Biosecur is a non-toxic organic alcohol-free compound containing citrus bioflavonoids suspended in glycerin. Mencucci et al. tested in vitro a liposomal commercial formulation, Oftasecur Ocular Spray (OFFHEALTH S.p.a., Florence, Italy) containing 0.2% biosecur, reporting bactericidal and fungicidal effects versus all common microorganisms at dilutions varying from 1:2 to 1:16 [73]. Moreover, Vagge et al. tested the compound in vivo in a prospective study on patients undergoing IVIs, reporting a significant decrease in conjunctival bacterial load after a 4-day prophylactic treatment [74] (Fig. 1).
Toxic Anterior Segment Syndrome Related to Antisepsis
Toxic anterior segment syndrome (TASS) is a condition characterized by an acute, sterile postoperative inflammation due to a noninfectious agent that penetrates the anterior segment perioperatively [75]. The likelihood of an antiseptic agent causing a TASS is very low according to published literature. However, there are a few reports in which residual antiseptic solution on surgical instruments has been described as the causative agent of TASS [76, 77].
Risk Management Strategies
Infection prevention and control represent a fundamental goal in all medically invasive procedures. Modern medicine is facing a progressive spread of multiresistant bacterial clones that are difficult to eradicate due to the uncontrolled use of antibiotics in the last decades. In some surgical contexts, the preventive administration of systemic antibiotics (usually 30–60 min before the skin incision) is a well-accepted practice and considered necessary to reduce the risk of perioperative infections. In the field of ophthalmic surgery, on the contrary, there are many different practices of disinfection used in different countries [47].
Although the use of antibiotics is surely effective in the reduction of conjunctival bacterial flora [13], the prophylactic effect against infection being not so valuable must be considered. On the other hand, this practice has the risk of inducing resistant bacteria [31]. In this context, the introduction of chemical disinfectants is very helpful because they can work in an effective way while preventing the emergence of new antibiotic resistance [78]. PVI is widely used, and its safety has been strongly established. One of the advantages of PVI is that it does not induce antibiotic resistance and has a wide antimicrobial spectrum [78], so its use can be considered effective in reducing the risk of infections related to intraocular procedures. In addition to the advantages of safety and effectiveness in preventing infections and avoiding the selection of multiresistant bacteria, another important aspect of PVI is the lower cost compared with antibiotics. This aspect is very important and must be considered because health expenditure is continually growing worldwide. It is necessary for healthcare providers to choose the most efficient products that ensure safety and are economically cost effective. From this perspective, the evaluation of risk–benefit ratio led us to consider that the use of antibiotics in place of PVI can be considered not justified. Since the safety and effectiveness of PVI has been well acknowledged by several scientific studies [1, 35], ocular surgeons can use PVI without the risk of incurring medical claims for not having administered antibiotics.
From a medico–legal point of view, the occurrence of healthcare-acquired infections (HAIs) can be a potential source of liability for the surgeon and the healthcare facility. Furthermore, the increasing complexity of medical and surgical activity along with the evolution of the law in the matter of professional liability require medical treatments to be increasingly safer for the patient’s health [79, 80]. HAIs are generally defined as infections of bacterial, fungal, or viral origin that are contracted in any healthcare setting (hospitals, outpatient clinics, dialysis centers, long-term care, home care, territorial residential facilities) and that at the time of admission to the facility or prior to the provision of care were neither clinically manifest nor incubating [81]. The Ministry of Health estimates that every year in Italy 450,000–700,000 infections occur in hospitalized persons (overall, a care-related infection occurs in 4–7% of hospitalizations) [82]. Concerning the surgical setting, it has been estimated that surgical wound infection is the most common cause of nosocomial infection with a doubled risk of death compared with patients undergoing the same procedures without developing infections [83]. It should be emphasized that the surgical disciplines are also those most involved in HAIs related medical malpractice cases. In intraocular procedures, infectious endophthalmitis due to bacterial or fungal infection is a potentially devastating complication [30, 84]. Furthermore, a study showed that ophthalmic surgery had a significant litigation/conviction ratio (83.3%), much higher compared with other branches. These data also underline the importance of implementing increasingly effective preventive measures to reduce medical–legal disputes that are, in some cases, particularly burdensome in health and economic terms [24]. The centrality of the prevention issue in the context of HAIs, including the proper application of asepsis measures, is further emphasized by the fact that in Italy the omission of such measures is one of the main elements in defining and circumscribing the healthcare liability that may result.
Conclusions
Ophthalmic surgery procedures are nowadays very commonly performed worldwide. Preoperative prophylaxis is therefore a crucial step to reduce infections; at the same time, there is the need to reduce antibiotic use due to continuously growing antibiotic resistance. In this scenario, antiseptic compounds are a valuable tool. PVI is well established in the literature and broadly used, although at different concentrations. CHX is becoming more used as published literature demonstrates a good safety and efficacy profile with reduced patient discomfort. Lastly, there are new compounds such as picloxydine, ozone, HOCl, and Biosecur that show very interesting preliminary results, but further studies are needed to confirm these outcomes.
Change history
20 February 2023
A Correction to this paper has been published: https://doi.org/10.1007/s40123-023-00682-4
References
Ciulla TA, Starr MB, Masket S. Bacterial endophthalmitis prophylaxis for cataract surgery: an evidence-based update. Ophthalmology. 2002;109:13–24.
Haripriya A, Baam ZR, Chang DF. Endophthalmitis prophylaxis for cataract surgery. Asia Pac J Ophthalmol (Phila). 2017;6(4):324–9.
Behndig A, Cochener-Lamard B, Güell J, Kodjikian L, Mencucci R, Nuijts R, et al. Surgical, antiseptic, and antibiotic practice in cataract surgery: results from the European Observatory in 2013. J Cataract Refract Surg. 2015;41:2635–43.
Behnding A, Ravindran R, Flynn H, Relhan N, Hernandez-Camarena J, Valdez-Garcia J, et al. Endophthalmitis prophylaxis in cataract surgery: overview of current practice patterns around the world. Curr Pharm Des. 2017;23:565–73.
Carrim ZI, Mackie G, Gallacher G, Wykes WN. The efficacy of 5% povidone-iodine for 3 minutes prior to cataract surgery. Eur J Ophthalmol. 2009;19(4):560–4.
Wu PC, Li M, Chang SJ, et al. Risk of endophthalmitis after cataract surgery using different protocols for povidone- iodine preoperative disinfection. J Ocul Pharmacol Ther. 2006;22(1):54–61.
Apt L, Isenberg S, Yoshimori R, Paez JH. Chemical preparation of the eye in ophthalmic surgery: iii. Effect of povidone-iodine on the conjunctiva. Arch Ophthalmol. 1984;102:728–9.
Speaker MG, Milch FA, Shah MK, Eisner W, Kreiswirth BN. Role of external bacterial flora in the pathogenesis of acute postoperative endophthalmitis. Ophthalmology. 1991;98:639–50.
Barry P, Gettinby G, Lees F, Peterson M, Revie C, Seal D, et al. Prophylaxis of postoperative endophthalmitis following cataract surgery: Results of the ESCRS multicenter study and identification of risk factors. J Cataract Refract Surg. 2007;33:978–88.
Groden LR, Murphy B, Rodnite J, Genvert GI. Lid flora in blepharitis. Cornea. 1991;10:50–3.
Barry P, Cordovés L, Gardner S. ESCRS guidelines for prevention and treatment of endophthalmitis following cataract surgery: prevention & treatment endophthalmitis. [cited 2022 Dec 14]; www.escrs.org. Accessed 15 Nov 2022.
Li B, Nentwich MM, Hoffmann LE, Haritoglou C, Kook D, Kampik A, et al. Comparison of the efficacy of povidone-iodine 1.0%, 5.0%, and 10.0% irrigation combined with topical levofloxacin 0.3% as preoperative prophylaxis in cataract surgery. J Cataract Refract Surg. 2013;39:994–1001.
Miño de Kaspar H, Kreutzer TC, Aguirre-Romo I, Ta CN, Dudichum J, Bayrhof M, et al. A prospective randomized study to determine the efficacy of preoperative topical levofloxacin in reducing conjunctival bacterial flora. Am J Ophthalmol. 2008;145:136-142.e2.
He L, Ta CN, Hu N, SinnarMiñ de Kaspar SH. Prospective randomized comparison of 1-day and 3-day application of topical 0.5% moxifloxacin in eliminating preoperative conjunctival bacteria. J Ocul Pharmacol Ther. 2009;25(4):373–8.
Moss JM, Nguyen D, Liu YI, Singh K, Montague A, Egbert PR, et al. Comparison of one-day versus one-hour application of topical gatifloxacin in eliminating conjunctival bacterial flora. Ophthalmology. 2008;115:2013–6.
Moss JM, Sanislo SR, Ta CN. A prospective randomized evaluation of topical gatifloxacin on conjunctival flora in patients undergoing intravitreal injections. Ophthalmology. 2009;116:1498–501.
Halachimi-Eyal O, Lang Y, Keness Y, Miron D. Preoperative topical moxifloxacin 0.5% and povidone-iodine 5.0% versus povidone-iodine 5.0% alone to reduce bacterial colonization in the conjunctival sac. J Cataract Refract Surg. 2009;35:2109–14.
Friling E, Lundström M, Stenevi U, Montan P. Six-year incidence of endophthalmitis after cataract surgery: Swedish national study. J Cataract Refract Surg. 2013;39:15–21.
Miller D. Update on the epidemiology and antibiotic resistance of ocular infections. Middle East Afr J Ophthalmol. 2017;24:30–42.
Milder E, Vander J, Shah C, Garg S. Changes in antibiotic resistance patterns of conjunctival flora due to repeated use of topical antibiotics after intravitreal injection. Ophthalmology. 2012;119:1420–4.
Mcdonnell G, Russell AD. Antiseptics and disinfectants: activity, action, and resistance. Clin Microbiol Rev. 1999;12:147–79.
Eggers M, Koburger-Janssen T, Ward LS, Newby C, Müller S. Bactericidal and virucidal activity of povidone-iodine and chlorhexidine gluconate cleansers in an in vivo hand hygiene clinical simulation study. Infect Dis Ther. 2018;7:235–47.
Grzybowski A, Brona P, Kim SJ. Microbial flora and resistance in ophthalmology: a review. Graefe’s Arch Clin Exp Ophthalmol. 2017;255:851–62.
Saggers BA, Stewart GT. Polyvinyl-pyrrolidone-iodine: an assessment of antibacterial activity. Epidemiol Infect. 1964;62:509–18.
Chou SF, Lin CH, Chang SW. Povidone–iodine application induces corneal cell death through fixation. Br J Ophthalmol. 2011;95:277–83.
Ricciardelli G, Giannaccare G, di Zazzo A, Coassin M, Scorcia V, Romano MR, et al. Efficacy and tolerability of polyvinylpyrrolidone-iodine 0.6% treatment in adenoviral keratoconjunctivitis: a prospective randomized controlled study. Eye. 2021;36:160–6.
Ta CN, Singh K, Egbert PR, de Kaspar HM. Prospective comparative evaluation of povidone-iodine (10% for 5 minutes versus 5% for 1 minute) as prophylaxis for ophthalmic surgery. J Cataract Refract Surg. 2008;34:171–2.
Speaker MG, Menikoff JA. Prophylaxis of endophthalmitis with topical povidone-iodine. Ophthalmology. 1991;98:1769–75.
Alp BN, Elibol O, Sargon MF, Aslan OS, Yanyali A, Karabas L, et al. The effect of povidone iodine on the corneal endothelium. Cornea. 2000;19:546–50.
Binder CA, Miaeo De Kaspar H, Klauû V, Kampik A, Binder CA, Bender CA, et al. Preoperative infection prophylaxis with 1 % polyvidon-iodine solution based on the example of conjunctival staphylococci. Ophthalmologe. 1999;96:663–7.
Shimada H, Arai S, Nakashizuka H, Hattori T, Yuzawa M. Reduction of anterior chamber contamination rate after cataract surgery by intraoperative surface irrigation with 0.25% povidone–iodine. Am J Ophthalmol. 2011;151:11-17.e1.
Jiang J, Wu M, Shen T. The toxic effect of different concentrations of povidone iodine on the rabbit’s cornea. Cutan Ocul Toxicol. 2009;28(3):119–24.
Ahmed Y, Scott IU, Pathengay A, Bawdekar A, Flynn HW. Povidone-iodine for endophthalmitis prophylaxis. Am J Ophthalmol. 2014;157:503–4.
Peden MC, Hammer ME, Suñer IJ. Dilute povidone-iodine prophylaxis maintains safety while improving patient comfort after intravitreal injections. Retina. 2019;39:2219–24.
Musumeci R, Troiano P, Martinelli M, Piovella M, Carbonara C, Rossi S, et al. Effectiveness of 0.66% povidone-iodine eye drops on ocular surface flora before cataract surgery: a nationwide microbiological study. Jo Clin Med. 2021;10:2198.
Pinna A, Donadu MG, Usai D, Dore S, D’Amico-Ricci G, Boscia F, et al. In vitro antimicrobial activity of a new ophthalmic solution containing povidone-iodine 0.6% (IODIM®). Acta Ophthalmol. 2020;98:e178–80.
Reibaldi M, Avitabile T, Bandello F, Longo A, Bonfiglio V, Russo A, et al. The effectiveness of 0.6% povidone iodine eye drops in reducing the conjunctival bacterial load and needle contamination in patients undergoing anti-VEGF intravitreal injection: a prospective, randomized study. J Clin Med. 2019;8:1031.
Tognetto D, Pastore MR, Belfanti L, Merli R, Vinciguerra AL, Busetti M, et al. In vivo antimicrobial activity of 0.6% povidone-iodine eye drops in patients undergoing intravitreal injections: a prospective study. Sci Rep. 2021;11:1–6.
Hidalgo E, Dominguez C. Mechanisms underlying chlorhexidine-induced cytotoxicity. Toxicol In Vitro. 2001;15:271–6.
Jenkins S, Addy M, Wade W. The mechanism of action of chlorhexidine. J Clin Periodontol. 1988;15:415–24.
Karpiński TM, Szkaradkiewicz AK. Chlorhexidine–pharmaco-biological activity and application. Eur Rev Med Pharmacol Sci. 2015;19(7):1321–6.
Merani R, McPherson ZE, Luckie AP, Gilhotra JS, Runciman J, Durkin S, et al. Aqueous chlorhexidine for intravitreal injection antisepsis: a case series and review of the literature. Ophthalmology. 2016;123:2588–94.
Oakley CL, Vote BJ. Aqueous chlorhexidine (0.1%) is an effective alternative to povidone–iodine for intravitreal injection prophylaxis. Acta Ophthalmol. 2016;94:e808–9.
Dossarps D, Bron AM, Koehrer P, Aho-Glélé LS, Creuzot-Garcher C, Berthon L, et al. Endophthalmitis after intravitreal injections: incidence, presentation, management, and visual outcome. Am J Ophthalmol. 2015;160:17-25.e1.
Tabor E, Bostwick DC, Evans CC. Corneal damage due to eye contact with chlorhexidine gluconate. JAMA. 1989;261:557–8.
Varley GA, Meisler DM, Benes SC, McMahon JT, Zakov ZN, Fryczkowski A. Hibiclens keratopathy. A clinicopathologic case report. Cornea. 1990;9:341–6.
Behndig A, Montan P, Stenevi U, Kugelberg M, Lundström M. One million cataract surgeries: Swedish National Cataract Register 1992–2009. J Cataract Refract Surg. 2011;37:1539–45.
Behndig A, Cochener B, Güell JL, Kodjikian L, Mencucci R, Nuijts RMMA, et al. Endophthalmitis prophylaxis in cataract surgery: overview of current practice patterns in 9 European countries. J Cataract Refract Surg. 2013;39:1421–31.
Tognetto D, Pastore MR, Guerin GM, Decorti G, Franzin M, Lagatolla C, et al. Bactericidal activity of three different antiseptic ophthalmic preparations as surgical prophylaxis. Graefe’s Arch Clin Exp Ophthalmol. 2022;260:289–93.
Caruso C, Eletto D, Tosco A, Pannetta M, Scarinci F, Troisi M, et al. Comparative evaluation of antimicrobial, antiamoebic, and antiviral efficacy of ophthalmic formulations. Microorganisms. 2022;10:1156.
Mulder GD, Cavorsi JP, Lee DK. Polyhexamethylene biguanide (PHMB): an addendum to current topical antimicrobials. Wounds. 2007;19:173–82.
Chindera K, Mahato M, Kumar Sharma A, Horsley H, Kloc-Muniak K, Kamaruzzaman NF, et al. The antimicrobial polymer PHMB enters cells and selectively condenses bacterial chromosomes. Sci Rep. 2016;6:1–13.
Wessels S, Ingmer H. Modes of action of three disinfectant active substances: a review. Regul Toxicol Pharmacol. 2013;67:456–67.
Gilbert P, Pemberton D, Wilkinson DE. Synergism within polyhexamethylene biguanide biocide formulations. J Appl Bacteriol. 1990;69:593–8.
Mafra CSP, Carrijo-Carvalho LC, Chudzinski-Tavassi AM, de Taguchi FMC, Foronda AS, de Carvalho FRS, et al. Antimicrobial action of biguanides on the viability of acanthamoeba cysts and assessment of cell toxicity. Invest Ophthalmol Vis Sci. 2013;54:6363–72.
Forstner C, Leitgeb J, Schuster R, Dosch V, Kramer A, Cutting KF, et al. Bacterial growth kinetics under a novel flexible methacrylate dressing serving as a drug delivery vehicle for antiseptics. Int J Mol Sci. 2013;14:10582–90.
Gilbert P, Das JR, Jones Mv, Allison DG. Assessment of resistance towards biocides following the attachment of micro-organisms to, and growth on, surfaces. J Appl Microbiol. 2001;91:248–54.
Kramer A, Roth B, Müller G, Rudolph P, Klöcker N. Influence of the antiseptic agents polyhexanide and octenidine on FL cells and on healing of experimental superficial aseptic wounds in piglets. Skin Pharmacol Physiol. 2004;17:141–6.
Papa V, van der Meulen I, Rottey S, Sallet G, Overweel J, Asero N, et al. Safety and tolerability of topical polyhexamethylene biguanide: a randomised clinical trial in healthy adult volunteers. Br J Ophthalmol. 2022;106:190–6.
Hansmann F, Kramer A, Ohgke H, Strobel H, Müller M, Geerling G. Lavasept® as an alternative to PVP-iodine for preoperative desinfection in ophthalmic surgery: randomized, controlled, prospective double-blind trial. Ophthalmologe. 2005;102:1043–50.
Ristau T, Kirchhof B, Fauser S. Antisepsis with polyhexanide is effective against endophthalmitis after intravitreal injections. Acta Ophthalmol. 2014;92:e494–6.
Budzinskaya Mv, Khalatyan AS, Strakhovskaya MG, Zhukhovitsky VG. Ocular flora in patients undergoing intravitreal injections: antibiotic resistance patterns and susceptibility to antiseptic picloxydine. Int J Ophthalmol. 2020;13:85–92.
Spadea L, Tonti E, Spaterna A, Marchegiani A. Use of ozone-based eye drops: a series of cases in veterinary and human spontaneous ocular pathologies. Case Rep Ophthalmol. 2018;9:287–98.
Marchegiani A, Magagnini M, Cerquetella M, Troiano P, Franchini I, Franchini A, et al. Preoperative topical liposomal ozone dispersion to reduce bacterial colonization in conjunctival sac and periocular skin: preliminary study in dogs. Exp Eye Res. 2019;189: 107848.
Celenza G, Iorio R, Cracchiolo S, Petricca S, Costagliola C, Cinque B, et al. Antimycotic activity of ozonized oil in liposome eye drops against Candida spp. Transl Vis Sci Technol. 2020;9:4–4.
Pérez-Santonja JJ, Güell JL, Gris O, Dorrego XMV, Pellicer E, Benítez-Del-castillo JM. Liposomal ozonated oil in ocular infections: a review of preclinical and clinical studies, focusing on its antiseptic and regenerative properties. Clin Ophthalmol. 2022;16:1953–62.
Spadea L, Zanotto E, Cavallo R, Campagna G, Giannico MI, Costagliola C. Effectiveness of liposomal ozonized oil in reducing ocular microbial flora in patients undergoing cataract surgery. J Cataract Refract Surg. 2021;47:1548–55.
Bertone C, Mollicone A, Russo S, Sasso P, Fasciani R, Riccardi C, et al. The role of hypochlorous acid in the management of eye infections: a case series. Drugs Context. 2022;11:1–8.
Sakarya S, Gunay N, Karakulak M, Ozturk B, Ertugrul B. Hypochlorous acid: an ideal wound care agent with powerful microbicidal, antibiofilm, and wound healing potency. Wounds. 2014;26:342–50.
Klocek MS, Mammen A, Dhaliwal D, Kowalski RP. Time-kill comparison of povidone iodine to hypochlorous acid against endophthalmitis isolates of staphylococci. Invest Ophthalmol Vis Sci. 2016;57:5861–5861.
Kanclerz P, Grzybowski A, Olszewski B. Low efficacy of hypochlorous acid solution compared to povidone-iodine in cataract surgery antisepsis. Open Ophthalmol J. 2019;13:29–33.
Hypochlorous acid disinfection prior to cataract surgery - Full Text View - ClinicalTrials.gov. [cited 2022 Dec 14]. https://clinicaltrials.gov/ct2/show/NCT04568213. Accessed 15 Nov 2022.
Mencucci R, Ghelardi E, Celandroni F, Mazzantini C, Vecchione A, Pellegrini-Giampietro DE, et al. Antiseptics and the ocular surface: in vitro antimicrobial activity and effects on conjunctival and corneal epithelial cells of a new liposomal ocular spray containing Biosecur® citrus extract. Ophthalmol Ther. 2022;11:1067–77.
Vagge A, Ferro Desideri L, Carnevali A, del Noce C, Camposampiero D, Agrusta M, et al. Efficacy of a new commercial ocular spray containing oftasecur citrus extract for reducing microbial load in the conjunctiva of patients receiving intravitreal injections. Ophthalmol Ther. 2021;10:1025–32.
Hernandez-Bogantes E, Navas A, Naranjo A, Amescua G, Graue-Hernandez EO, Flynn HW, et al. Toxic anterior segment syndrome: a review. Surv Ophthalmol. 2019;64:463–76.
Jun EJ, Chung SK. Toxic anterior segment syndrome after cataract surgery. J Cataract Refract Surg. 2010;36:344–6.
Yang S, Yan X. Retrospective analysis of clinical characteristics of toxic anterior segment syndrome. Zhonghua Yan Ke Za Zhi. 2009;45:225–8.
Parikh SR, Parikh RS. Chemical disinfectants in ophthalmic practice. Indian J Ophthalmol. 2021;69:510.
Bollero D, Cortellini M, Stella M, et al. Pan-antibiotic resistance and nosocomial infection in burn patients: therapeutic choices and medico-legal problems in Italy. Ann Burns Fire Disasters. 2003; p. 182–7.
Treglia M, Pallocci M, Passalacqua P, Giammatteo J, de Luca L, Mauriello S, et al. Medical liability: review of a whole year of judgments of the civil court of Rome. Int J Environ Res Public Health. 2021;18:6019.
Treglia M, Pallocci M, Passalacqua P, Sabatelli G, de Luca L, Zanovello C, et al. Medico-legal aspects of hospital-acquired infections: 5-years of judgements of the civil court of Rome. Healthcare. 2022;10:1336.
Infezioni ospedaliere: cause e prevenzione - ISSalute [Internet]. [cited 2022 Dec 14]. https://www.issalute.it/index.php/la-salute-dalla-a-alla-z-menu/i/infezioni-ospedaliere%23link-di-approfondimento. Accessed 15 Nov 2022.
Gouvêa M, de Novaes CO, Pereira DMT, Iglesias AC. Adherence to guidelines for surgical antibiotic prophylaxis: a review. Braz J Infect Dis. 2015;19:517–24.
Zaharia A-C, Dumitrescu O-M, Rogoz R-E, Dimirache AE, Zemba M. Preoperative antisepsis in ophthalmic surgery (a review). Rom J Ophthalmol. 2021;65:120.
Acknowledgements
Funding
No funding or sponsorship was received for this study or publication of this article. The journal’s Rapid Service Fee was funded by the authors.
Author Contributions
Conceptualization, Alfredo Borgia and Giuseppe Giannaccare; methodology, Alfredo Borgia and Giuseppe Giannaccare; writing: original draft preparation, Alfredo Borgia, Daniela Mazzuca, Marcello Della Corte, Nicola Gratteri, Giovanni Fossati, Raffaele Raimondi, Luca Pagano, Vincenzo Scorcia, and Giuseppe Giannaccare; writing: review and editing, Alfredo Borgia, Vincenzo Scorcia, and Giuseppe Giannaccare; supervision, Alfredo Borgia, Vincenzo Scorcia, and Giuseppe Giannaccare. All authors have read and agreed to the published version of the manuscript.
Disclosures
Alfredo Borgia, Daniela Mazzuca, Marcello Della Corte, Nicola Gratteri, Giovanni Fossati, Raffaele Raimondi, Luca Pagano, Vincenzo Scorcia, and Giuseppe Giannaccare have nothing to declare.
Compliance with Ethics Guidelines
This article is based on previously conducted studies and does not contain any new studies with human participants or animals performed by any of the authors.
Data Availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Author information
Authors and Affiliations
Corresponding author
Additional information
The original online version of this article was revised to correct the author name Raffaele Raimondi.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License, which permits any non-commercial use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by-nc/4.0/.
About this article
Cite this article
Borgia, A., Mazzuca, D., Della Corte, M. et al. Prophylaxis of Ocular Infection in the Setting of Intraocular Surgery: Implications for Clinical Practice and Risk Management. Ophthalmol Ther 12, 721–734 (2023). https://doi.org/10.1007/s40123-023-00661-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40123-023-00661-9