Abstract
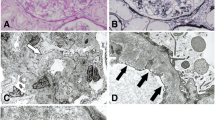
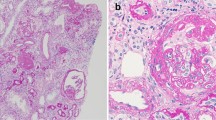
A 79-year-old Japanese man was admitted to our hospital because of proteinuria and kidney dysfunction. He was diagnosed with chronic myeloid leukemia 13 years before and was treated with imatinib. Deep molecular response was achieved but he developed 1+ proteinuria in the first year, which gradually worsened thereafter. Imatinib was discontinued 12 years later but proteinuria and kidney dysfunction were progressive. Percutaneous kidney biopsy revealed mild mesangial hyper-cellularity and matrix increase, swelling of endothelial cells, and partial double contours of glomerular tufts. Subendothelial edema in the interlobular artery was also noted. Immunofluorescence was not remarkable. Electron microscopy revealed endothelial injury with severe sub-endothelial edema. Since imatinib had already been discontinued, conservative therapy with maximal dose of azilsartan was administered. A second biopsy was performed 1 year later because of further deterioration of kidney function, which revealed markedly increased global glomerulosclerosis and severe interstitial fibrosis and tubular atrophy. Segmental glomerulosclerosis with podocyte hyperplasia was also observed. Electron microscopy revealed glomerulosclerotic changes and partially attenuated endothelial injury. Two and a half years later, proteinuria reduced, progression of kidney dysfunction slowed, and he was independent on dialysis therapy. Molecular response of chronic myeloid leukemia was also maintained. The clinical course suggested that endothelial and podocyte injuries were induced by imatinib, and that the nephrotoxic effects lasted for a few years after discontinuation.



Similar content being viewed by others
References
Baccarani M, Cortes J, Pane F, Niederwieser D, Saglio G, Apperley J, et al. Chronic myeloid leukemia: an update of concepts and management recommendations of European LeukemiaNet. J Clin Oncol. 2009;27:6041–51.
Blackstein ME, Blay JY, Corless C, Driman DK, Riddell R, Soulières D, et al. Gastrointestinal stromal tumors: consensus statement on diagnosis and treatment. Can J Gastroenterol. 2006;20:157–63.
Kalmanti L, Saussele S, Lauseker M, Müller MC, Dietz CT, Heinrich L, et al. Safety and efficacy of imatinib in CML over a period of 10 years: data from the randomized CML-study IV. Leukemia. 2015;29:1123–32.
Al-Kali A, Farooq S, Tfayli A. Tumor lysis syndrome after starting treatment with Gleevec in a patient with chronic myelogenous leukemia. J Clin Pharm Ther. 2009;34:607–10.
François H, Coppo P, Hayman JP, Fouqueray B, Mougenot B, Ronco P. Partial Fanconi syndrome induced by imatinib therapy: a novel cause of urinary phosphate. Am J Kidney Dis. 2008;51:298–301.
Foringer JR, Verani RR, Tija VM, Finkel KW, Samuels JA, Guntupalli JS. Acute renal failure secondary to imatinib mesylate treatment in prostate cancer. Ann Pharmacother. 2005;39:2136–8.
de Oliveira RA, Marques IDB, Seguro AC, Andrade V. Electrolyte disturbances and acute kidney injury induced by imatinib therapy. NDT Plus. 2009;2:27–9.
Marcolino MS, Boersma E, Clementino NCD, Macedo AV, Marx-Neto AD, Silva MHCR, et al. Imatinib treatment duration is related to decreased estimated glomerular filtration rate in chronic myeloid leukemia patients. Ann Oncol. 2011;22:2073–9.
Al Aly Z, Ashley JMP, Gellens ME, Gonzalez EA. Thrombotic thrombocytopenic purpura in a patient treated with imatinib mesylate: true association or mere coincidence? Am J Kidney Dis. 2005;45:762–8.
Martino S, Daguindau E, Ferrand C, Bamoulid J, Hayette S, Nicolini FE, et al. A successful renal transplantation for renal failure after dasatinib-induced thrombotic thrombocytopenic purpura in a patient with imatinib-resistant chronic myelogenous leukaemia on nilotinib. Leuk Res Rep. 2013;2:29–31.
Ojeda-Uribe M, Merieau S, Guillon M, Aujoulat O, Hinschberger O, Eisenmann JC, et al. Secondary thrombotic microangiopathy in two patients with Philadelphia-positive hematological malignancies treated with imatinib mesylate. J Oncol Pharm Pract. 2016;22:361–70.
Rogulj IM, Matišić V, Arsov B, Boban L, Juginović A, Molnar V, et al. Dasatinib-induced nephrotic syndrome: a case of phenoconversion? Croat Med J. 2019;60:250–4.
Ochiai S, Sato Y, Minakawa A, Fukuda A, Fujimoto S. Dasatinib-induced nephrotic syndrome in a patient with chronic myelogenous leukemia: a case report. BMC Nephrol. 2019;20:87.
Wallace E, Lyndon W, Chumley P, Jaimes EA, Fatima H. Dasatinib-induced nephrotic-range proteinuria. Am J Kidney Dis. 2013;61:1026–31.
Seki Y, Nagano O, Koda R, Morita S, Hasegawa G. Pathological findings suggesting vascular endothelial damage in multiple organs in chronic myelogenous leukemia patients on long-term tyrosine kinase inhibitor therapy. Int J Hematol. 2020;1112:584–91.
Thomas SM, Brugge JS. Cellular functions regulated by Src family kinases. Annu Rev Cell Dev Biol. 1997;13:513–609.
Aman J, van Bezu J, Damanafshan A, Huveneers S, Eringa EC, Vogel SM, et al. Effective treatment of edema and endothelial barrier dysfunction with imatinib. Circulation. 2012;126:2728–38.
Ciuclan L, Hussey MJ, Burton V, Good R, Duggan N, Beach S, et al. Imatinib attenuates hypoxia-induced pulmonary arterial hypertension pathology via reduction in 5-hydroxytryptamine through inhibition of tryptophan hydroxylase 1 expression. Am J Respir Crit Care Med. 2013;187:78–89.
Tuuminen R, Dashkevich A, Keränen MA, Raissadati A, Krebs R, Jokinen JJ, et al. Platelet-derived growth factor-B protects rat cardiac allografts from ischemia–reperfusion injury. Transplantation. 2016;100:303–13.
Sakurai M, Kikuchi T, Karigane D, Kasahara H, Matsuki E, Hashida R, et al. Renal dysfunction and anemia associated with long-term imatinib treatment in patients with chronic myelogenous leukemia. Int J Hematol. 2019;109:292–8.
Okamoto S, Ureshino H, Kawaguchi A, Miyazono M, Ikeda Y, Kimura S. Assessment of estimated glomerular filtration rate in patients with chronic myeloid leukemia following discontinuation of tyrosine kinase inhibitors. Int J Hematol. 2020;112:41–5.
Acknowledgements
We thank Cathel Kerr, B.Sc., Ph.D., from Edanz (https://jp.edanz.com/ac) for editing a draft of this manuscript. This case was discussed at the 23rd Kyushu Okinawa Kidney Biopsy Forum.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from the patient described in this case report.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
About this article
Cite this article
Morita, N., Ozaki, T., Yokota, S. et al. Focal segmental glomerulosclerosis and concurrent glomerular microangiopathy after long-term imatinib administration. CEN Case Rep 11, 134–140 (2022). https://doi.org/10.1007/s13730-021-00622-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13730-021-00622-w