Abstract
Ureterorenoscopy and double‑J stents are frequently associated with complicated urinary tract infections (cUTI’s). To date, it remains unclear whether longer indwelling stent duration increases the risk of cUTI’s and recommendations on this subject are therefore lacking. This study investigates whether double‑J stent placement and longer indwelling stent duration prior to URS increase the risk of post-URS cUTI’s. Adult patients undergoing ureterorenoscopy in 2019 were eligible for study participation. Records were retrospectively collected. Potential risk factors were evaluated using multivariate logistic regression models. 16.9% of the prestented patients was diagnosed with a UTI, compared to 7.1% in the non-prestented group (p = 0.034). Female gender, preoperative positive urine cultures and stone recurrence were significant risk factors. This study demonstrated a correlation between preoperative placement of double‑J stents and post-URS complicated UTI’s. However, neither preoperative double‑J stent placement nor longer indwelling stent time was a significant risk factor for postoperative complicated UTI’s.
Samenvatting
Ureterorenoscopie en dubbel-J-verblijfskatheters worden veelvuldig geassocieerd met gecompliceerde urineweginfecties. Tot op heden blijft het onduidelijk of een langere verblijfsduur van dubbel-J-katheters de kans op gecompliceerde urineweginfecties verhoogt, waardoor aanbevelingen voor dit onderwerp ontbreken. Deze studie onderzoekt of de aanwezigheid en de verblijfsduur van dubbel-J-katheters vóór URS onafhankelijke risicofactoren zijn voor post-ureterorenoscopie gecompliceerde urineweginfecties. Data van alle volwassen patiënten die een ureterorenoscopie ondergingen in 2019 werden retrospectief verzameld. Potentiële risicofactoren werden geëvalueerd middels multivariate logistische regressiemodellen. 16,9% van de patiënten met een preoperatieve dubbel-J-verblijfskatheter kreeg een gecompliceerde urineweginfectie, in vergelijking met 7,1% in de groep zonder preoperatieve stent (p = 0,034). Vrouwelijk geslacht, preoperatieve positieve urinekweken en recidiverende urolithiasis bleken significante risicofactoren. Deze studie demonstreerde een correlatie tussen preoperatief geplaatste dubbel-J-verblijfskatheters en post-URS gecompliceerde urineweginfecties. Echter, bij multivariate logistische regressieanalyse bleken preoperatief geplaatste dubbel-J-verblijfskatheters of langdurig katheterverblijf geen significante risicofactoren voor post-URS gecompliceerde urineweginfecties.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Over the past years, there has been growing interest in ureterorenoscopy (URS) as a urologic treatment. URS has been shown to be a safe intervention with relatively low complication rates of 3.5% [1] to 7.4% [2]. Also, it has been highlighted to be an effective treatment for urolithiasis, with stone-free rates up to 85.6% [1, 2] and a limited number of patients needing retreatment. Despite these advantages, URS has been associated with the development of urinary tract infections (UTI’s) and sepsis [3,4,5]. Risk factors for infectious complications following URS involve size of stone, preoperative acute pyelonephritis, polyuria, preoperative infection history, comorbidity score and residual fragments [3,4,5].
URS can be preceded by the placement of a stent, resulting in low complication rates and with stone-free rates up to 97.3% [6,7,8]. However, indwelling stents on their own have adverse effects. Symptoms such as haematuria, dysuria, urge incontinence and storage problems have been reported [9], with 68% of patients experiencing these urinary tract symptoms within an indwelling time of one month [9, 10]. These symptoms seem to cause great impact on quality of life and contribute to disturbance in daily activities of patients [9]. Additionally, UTI’s have been described in patients with double‑J stents. Although the relationship between UTI’s, colonised indwelling double‑J stents and bacteriuria has been investigated by many researchers, results have not been conclusive [11,12,13,14,15,16,17,18,19]. Longer indwelling stent time has been associated with bacterial colonisation in 29.4% [11] to 100% [15, 20], whereas bacteriuria has only been described in 13% to 26.2% [11,12,13,14,15, 17, 18, 20, 21] of the prestented patients. This highlights the fact that bacterial colonisation of double‑J stents does not by definition cause bacteriuria; neither does bacteriuria impose the presence of a UTI [13, 22]. The inconsistency in previous studies clearly shows the discrepancy in the association of indwelling stent time and the rate of colonisation, bacteriuria and the understanding of its consequence in the development of UTI’s [14]. Consequently, to date, no recommendations have been suggested for maximum preoperative indwelling stent duration.
The aim of this study is to investigate whether preoperative double‑J stent placement and its indwelling stent time increases the risk of post-URS complicated UTI’s.
Materials
We retrospectively reviewed records of all patients who underwent a URS from 1 January 2019 to 31 December 2019 at a large non-academic teaching hospital in Utrecht, the Netherlands. Ethical approval was obtained by the institutional review board (20.090). Data was electronically collected and included age, sex, Body Mass Index (BMI), American Society of Anaesthesiologists (ASA) score and comorbidities such as diabetes mellitus, diabetic nephropathy, chronic renal failure, and cardiovascular disease. Additionally, pre-, peri- and postoperative data was collected, including stone characteristics and the presence of nephrostomy catheters or preoperative hydronephrosis. Adult patients treated with a URS were eligible for inclusion. Study exclusion criteria were absent.
Patients needing URS for diagnostic matters or for the treatment of urolithiasis, nephrolithiasis or ureteral stenosis were admitted to the waiting list of our hospital. About half of the patients had received a preoperative indwelling double‑J stent due to unbearable pain, fever or kidney failure induced by urolithiasis, or due to stenosis of the urinary tract. Surgery was performed as soon as possible under general anaesthesia. According to our hospitals protocol, perioperative antibiotic administration was completed with cefazolin in all cases. Perioperative double‑J stent placement was done in patients with a suspected development of postoperative oedema, remaining stenosis, or perforation. Pre- and postoperative urine cultures were performed if patients presented to the urology outpatient department or to the emergency department with symptoms of the urinary tract or fever.
Our study outcome was determined as the presence of a post-URS complicated UTI, which was defined as having a positive urine culture and fever (temperature of > 38 °Celsius) or urosepsis within 90 days after surgery.
Statistical analysis was conducted using SPSS IBM Statistics (version 26.0). Descriptive statistics were mentioned as frequencies and percentages for categorical variables, continuous variables were mentioned by median and interquartile range. We evaluated potential confounders and multicollinearity among covariables. The Mann-Whitney test was assessed to compare medians of different variables. The Pearson’s r correlation test was used to assess correlations between continuous variables, whereas the Chi-square test evaluated the association between categorical variables. Subsequently, potential confounders and statically significant risk factors, described in a recent systematic review and meta-analysis by Sun et al. [23], were added to the univariate logistic regression model. Multivariate logistic regression was conducted for all those variables with a p-value < 0.2 in the univariate model and for variables of interest for the research question. Variables were considered to be significant risk factors when p < 0.05 was reached in the multivariate model. Risk factors were expressed by their adjusted odds ratio (OR), 95% coincidence interval (CI) and p-value. All results were analysed using a two-tailed test.
Results
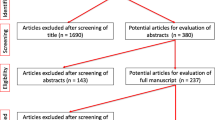
During a one-year study period, 195 individual patients underwent a URS and were included in the study. No patients were excluded. Patients’ demographics are reported in Tab. 1. There were 81 (41.5%) females. Patients had a median (interquartile range (IQR)) age of 56 years old (38–67) and a median (IQR) BMI of 25.46 kg/m2 (23.40–28.72). Median (IQR) ASA score was two (one-two). Twenty-five patients had diabetes mellitus, of which 20.0% had diabetic nephropathy. Also, 4.6% had chronic renal failure and 68 (34.9%) patients had cardiovascular disease, of which 32.4% had isolated hypertension. One hundred twenty-five (64.1%) patients had none of these previous comorbidities. 43.6% had preoperative hydronephrosis and 4.1% had a nephrostomy catheter.
Eighty-three (42.6%) patients had received an indwelling double‑J stent prior to URS, due to one of the following indications: unbearable pain, fever or kidney failure caused by urolithiasis (63.9%), stenosis of the urinary tract (3.6%) or perioperative placement during previous URS’s (32.5%). Median (IQR) indwelling stent time was 49 days (38–100), of which 16 (19.3%) had an indwelling time of < 30 days, 32 (38.6%) of 31–60 days, nine (10.8%) of 61–90 days and 26 (31.3%) of > 90 days.
Median (IQR) URS operation time was 67 minutes (61–95). Most patients underwent URS as a consequence of urolithiasis, of which 62.9% were treated for single sided stones and most patients experienced a first stone episode (51.8%). A perioperative ureteral stent was placed at the end of the procedure in 85.6% of the cases.
Preoperative urine cultures were performed in 48 (24.6%) patients. Thirteen (27.1%) of these patients were diagnosed with a preoperative UTI and were treated with culture-based targeted antibiotics before surgery. Furthermore, 46.2% of the patients with a preoperative UTI were also diagnosed with a postoperative complicated UTI. 14.3% of the patients with a negative preoperative urine culture and 7.5% of the patients without a preoperatively performed urine culture developed a post-URS complicated UTI.
Postoperative urine cultures were performed in 22.6% of all patients. Of these, 9.1% and 25% were diagnosed with an uncomplicated and complicated UTI, respectively. Tab. 2 presents all bacteria found in the urine cultures.
Univariate logistic regression indicated the following variables as potential risk factors for complicated UTI’s post-URS: female gender (OR 4.062; 95% CI 1.467–11.253; p = 0.007), preoperative positive urine culture (OR 6.861; 95% CI 1.615–29.147; p = 0.009), stone recurrence (OR 4.598; 95% CI 1.490–14.190; p = 0.008) and preoperative placement of double-J stents (OR 2.126; 95% CI 0.785–5.760; p = 0.138). Adjustment by multivariate logistic regression revealed the following risk factors: female gender (OR 5.765; 95% CI 1.808–18.384; p = 0.003), preoperative positive urine culture (OR 9.070; 95% CI 2.376–34.631; p = 0.001) and stone recurrence (OR 4.598; 95% CI 1.490–14.190; p = 0.008). Results are shown in Tab. 3.
In a subgroup analysis of all 83 patients with preoperative placement of double‑J stents, 14 (16.9%) patients were diagnosed with a UTI post-URS, compared to eight (7.1%) in the group without indwelling stents, p = 0.034. 9.6% of the patients with a post-URS UTI had urosepsis and 7.2% presented with urinary tract symptoms and fever. Most UTI’s were seen in the group of patients with an indwelling stent time of 31 to 60 days. The following risk factors were associated with UTI’s among prestented patients, using univariate logistic regression: female gender (OR 7.333; 95% CI 1.861–28.894; p = 0.004), BMI (OR 0.873; 95% CI 0.726–1.051; p = 0.151), stone recurrence (OR 4.990; 95% CI 1.228–20.285; p = 0.025) and preoperative positive urine cultures (OR 5.822; 95% CI 0.841–40.299; p = 0.074). Subsequently, multivariate logistic regression was conducted for factors with p-value < 0.2 and for variables of interest in our study. Female gender (OR 9.927; 95% CI 2.021–48.768; p = 0.005), preoperative positive urine cultures (OR 6.505; 95% CI 1.282–32.998; p = 0.024) and stone recurrence (OR 6.992; 95% CI 1.414–34.581; p = 0.017) were considered to be significant risk factors amongst prestented patients. See Tab. 4.
Discussion
In this study we sought to determine whether preoperative placement of double‑J stents and their indwelling time were associated with an increased risk of post-URS complicated UTI’s. Limited research has evaluated the influence of indwelling stent time on infectious complications; therefore, guidelines on recommended stent duration are unavailable.
Although we showed a correlation between preoperative placement of double‑J stents and post-URS complicated UTI’s, no significant association was demonstrated after adjustment for cofounders and multicollinearity in multivariate logistic regression analysis. Additionally, amongst patients with a double‑J stent, longer indwelling stent time was not a significant independent risk factor for post-URS infectious complications. However, female gender, preoperative positive urine cultures and stone recurrence were significant risk factors for post-URS infections.
Our results showed higher postoperative infection rates among prestented patients compared to non-prestented patients (16.9% vs 7.1%). Our findings were conform to those of Moses et al. [24]. They conducted a retrospective study with 550 patients undergoing URS, in which they observed higher infection rates among prestented patients compared to non-prestented patients (84.2% and 58.6%, respectively). Corroborating Grabe et al. [25], they therefore claim prior stent insertion being an independent risk factor for post-URS infections [24]. Conversely, other prior studies [26, 27] declare to have found no statistically significant difference in infection rates between these groups. A recent study by Southern et al. [28] evaluated systemic inflammatory response syndrome (SIRS) among 2746 patients undergoing URS. SIRS was mostly described amongst patients with prior stent insertion. Although a significant correlation was demonstrated between SIRS and prior stent insertion (p = 0.003), it did not appear to be an independent risk factor for SIRS using logistic regression analysis [28]. These findings correspond to those of the present study. Prior stent insertion was associated with postoperative infectious complications (p = 0.034). Yet, prior stent insertion appeared to be a non-significant risk factor when adjusted by covariables in the logistic regression model (p = 0.091). However, a proportion of the patients in the Netherlands report postoperative infectious symptoms to the general practitioner, without informing their urologist. This may lead to an underestimation of these results.
A recent study by Chen et al. [29] evaluated the development of acute pyelonephritis in 6459 patients with ureteral stents. They described a significant association between stent duration and acute pyelonephritis. Additionally, Altunal et al. [30] acknowledged equal findings. However, they applied the Student t-test and Chi-square test to evaluate this question, without any adjustments for covariables or potential confounders. Therefore, their findings may have been falsely assessed. To the best of our knowledge, Nevo et al. [31], a prospective study including 601 patients with preoperative stent placement, has been the first and only study to pinpoint the association between preoperative indwelling stent time and post-URS infection rates. They highlighted the fivefold lower risk of post-URS UTI development for patients with an indwelling stent duration of < 30 days, compared to those exceeding this number of days. They therefore recommend obtaining an indwelling stent time of less than one month. These findings are in contrast with our study results. Although 71.4% of the infections occurred after an indwelling time of 30 days, longer indwelling stent time pre-URS was not considered to be a significant risk factor for post-URS infectious complications (p = 0.721). The discrepancy between previous and present results may be explained by the fact that patients in our study cohort were relatively young and healthy. Forty-two percent was younger than 50 years old and 77.1% had an ASA score of ≤ two. Younger and healthier patients are less likely to develop infectious complications. Also, our study group was considerably smaller compared to previous studies. Lastly, the mean indwelling stent duration of our study cohort was shorter compared to Nevo et al. [31], which may be explained by apparent shorter waiting lists in our hospital.
Overall, 72.7% of the patients with infectious complications were female. Furthermore, adjusted OR declared that woman pose a 5.77-fold higher risk of developing postoperative UTI’s. Previous studies presented analogous results, pointing out 57.9% to 69.6% of the patient with infectious complications being female and emphasising its significant consequence in causing severe infections [27,28,29, 32]. In consideration of a possible explanation for our results, we evaluated the following potential confounders: age, comorbidity, ASA score and preoperative stenting. However, woman in our study group were younger, healthier (less comorbidities, lower ASA scores) and had lower prestenting rates than men. An explanation for our results may be the anatomic difference of the urogenital system in woman: due to shorter female urethra length bacteria can reach the bladder more rapidly than in men.
Thirteen patients were diagnosed with a preoperative UTI. All these patients were treated with antibiotics after assessment of an antibiotic sensitivity test, in order to examine bacteria resistance. Subsequently, 46.2% of the patients with a preoperative UTI developed a post-URS complicated UTI. These patients, compared to patients with a preoperative UTI without a post-URS UTI, had higher ASA scores and higher rates of cardiovascular disease and diabetes mellitus. Preoperative UTI’s were significantly correlated with postoperative UTI’s in multivariate logistic regression analysis, amongst the overall cohort and amongst prestented patients, respectively p = 0.001 and p = 0.024. These results were congruous to prior studies [33,34,35]. All these studies stated a 3.49 to 4.88-fold higher risk for post-URS infection development when patients were diagnosed with a preoperative UTI, comparable to our study results.
Our results pointed out a fivefold increased risk for post-URS infections when recurrence of stones was present, being a statically significant risk factor for postoperative UTI’s. Although recurrence rates are high in urolithiasis, few publications have studied this issue. Hanna et al. [36] published a retrospective study investigating 172 patients undergoing ureteroscopy for stone treatment. The analysis of potential risk factors described significance for female gender; however, stone recurrence was non-significant. Mitsuzuka et al. [4] reported non-significancy for stone reappearance, using the Chi-square test. Yet, no adjustments for covariables or cofounders were executed. Recognition of stone recurrence is important in the approach of postoperative UTI’s, considering 80% of these patients have recurrent UTI’s in the first year following URS [37].
Few studies have pinpointed the exact relation between indwelling stent time and postoperative infectious complications. Due to the great use of preoperative double‑J stents and due to the absence of recommendations for maximum indwelling stent duration, our findings could be of useful value.
Nonetheless, some limitations should be considered while interpreting our study results. First, due to its retrospective design, data collection was restricted to electronical records and patient follow-up was limited. This may have led to an underestimation of the reported post-URS UTI’s. Additionally, despite of the prevailing guidelines [38], pre-URS urine cultures were not performed in every patient. If urine cultures would have been completed in all patients, asymptomatic UTI’s and resistance patterns of bacteria could have been traced. Consequently, knowledge of the resistance patterns could have had an influence on the type of the perioperative antibiotic, which could possibly have prevented some of the post-URS UTI’s. Second, our study cohort was rather small. Future studies consisting larger cohorts may lead to further conclusions. Lastly, since certain stone types have been associated with the development of UTI’s [39], stone analysis should be included in future studies.
In conclusion, this study demonstrated a correlation between preoperative placement of double‑J stents and post-URS complicated UTI’s. However, neither preoperative double‑J stent placement nor longer indwelling stent time was a significant risk factor for postoperative complicated UTI’s in multivariate logistic regression analysis.
References
de la Rosette J, Denstedt J, Geavlete P, et al. The clinical research office of the endourological society ureteroscopy global study: indications, complications, and outcomes in 11,885 patients. J Endourol. 2014;28:131–9.
Somani BK, Giusti G, Sun Y, et al. Complications associated with ureterorenoscopy (URS) related to treatment of urolithiasis: the Clinical Research Office of Endourological Society URS Global study. World J Urol. 2017;35:675–81.
Baseskioglu B. The prevalence of urinary tract infection following flexible ureterenoscopy and the associated risk factors. Urol J. 2019;16:439–42.
Mitsuzuka K, Nakano O, Takahashi N, Satoh M. Identification of factors associated with postoperative febrile urinary tract infection after ureteroscopy for urinary stones. Urolithiasis. 2016;44:257–62.
Zhong W, Leto G, Wang L, Zeng G. Systemic inflammatory response syndrome after flexible ureteroscopic lithotripsy: a study of risk factors. J Endourol. 2015;29:25–8.
Lumma PP, Schneider P, Strauss A, et al. Impact of ureteral stenting prior to ureterorenoscopy on stone-free rates and complications. World J Urol. 2013;31:855–9.
Rubenstein RA, Zhao LC, Loeb S, Shore DM, Nadler RB. Prestenting improves ureteroscopic stone-free rates. J Endourol. 2007;21:1277–80.
Shields JM, Bird VG, Graves R, Gómez-Marín O. Impact of preoperative ureteral stenting on outcome of ureteroscopic treatment for urinary lithiasis. J Urol. 2009;182:2768–74.
Joshi HB, Okeke A, Newns N, Keeley FX, Timoney AG. Characterization of urinary symptoms in patients with ureteral stents. Urology. 2002;59:511–6.
Joshi HB, Stainthorpe A, MacDonagh RP, et al. Indwelling ureteral stents: evaluation of symptoms, quality of life and utility. J Urol. 2003;169:1065–9.
Aydin HR, Irkilata L, Aydin M, et al. Incidence of bacterial colonisation after indwelling of double‑J ureteral stent. Arch Ital Urol Androl. 2016;87:291–4.
Farsi HM, Mosli HA, Al-Zemaity MF, et al. Bacteriuria and colonization of double-pigtail ureteral stents: long-term experience with 237 patients. J Endourol. 1995;9:469–72.
Kehinde EO, Rotimi VO, Al-Hunayan A, et al. Bacteriology of urinary tract infection associated with indwelling J ureteral stents. J Endourol. 2004;18:891–6.
Klis R, Korczak-Kozakiewicz E, Denys A, Sosnowski M, Rozanski W. Relationship between urinary tract infection and self-retaining Double‑J catheter colonization. J Endourol. 2009;23:1015–9.
Kliś R, Szymkowiak S, Madej A, et al. Rate of positive urine culture and double‑J catheters colonization on the basis of microorganism DNA analysis. Cent European J Urol. 2014;67:81–5.
Ozgur BC, Ekıcı M, Yuceturk CN, et al. Bacterial colonization of double J stents and bacteriuria frequency. Kaohsiung J Med Sci. 2013;29:658–61.
Paick SH, Park HK, Oh SJ, et al. Characteristics of bacterial colonization and urinary tract infection after indwelling of double‑J ureteral stent. Urology. 2003;62:214–7.
Shabeena KS, Bhargava R, Manzoor MAP, et al. Characteristics of bacterial colonization after indwelling double‑J ureteral stents for different time duration. Urol Ann. 2018;10:71–5.
Yeniyol CO, Tuna A, Yener H, et al. Bacterial colonization of double J stents and bacteriuria frequency. Int Urol Nephrol. 2002;34:199–202.
Riedl CR, Plas E, Hübner WA, et al. Bacterial colonization of ureteral stents. Eur Urol. 1999;36:53–9.
Lifshitz DA, Winkler HZ, Gross M, et al. Predictive value of urinary cultures in assessment of microbial colonization of ureteral stents. J Endourol. 1999;13:735–8.
Cortes-Penfield NW, Trautner BW, Jump RLP. Urinary tract infection and asymptomatic bacteriuria in older adults. Infect Dis Clin North Am. 2017;31:673–88.
Sun J, Xu J, OuYang J. Risk factors of infectious complications following ureteroscopy: a systematic review and meta-analysis. Urol Int. 2020;104:113–24.
Moses RA, Ghali FM, Pais VM, et al. Unplanned hospital return for infection following ureteroscopy-can we identify modifiable risk factors? J Urol. 2016;195:931–6.
Grabe M, Botto H, Cek M, et al. Preoperative assessment of the patient and risk factors for infectious complications and tentative classification of surgical field contamination of urological procedures. World J Urol. 2012;30:39–50.
MacCraith E, O’Kelly J, Ryan J, et al. Predictors of emergency department attendance following ureterorenoscopy for urolithiasis. Ir J Med Sci. 2020;189:1445–9.
Yoshida S, Takazawa R, Uchida Y, et al. The significance of intraoperative renal pelvic urine and stone cultures for patients at a high risk of post-ureteroscopy systemic inflammatory response syndrome. Urolithiasis. 2019;47:533–40.
Southern JB, Higgins AM, Young AJ, et al. Risk factors for postoperative fever and systemic inflammatory response syndrome after ureteroscopy for stone disease. J Endourol. 2019;33:516–22.
Chen SJ, Huang CP, Chiu KY, et al. Association of acute pyelonephritis with double‑J ureteral stenting: a nationwide population-based case control study. Scand J Urol. 2021;55:61–6.
Altunal N, Willke A, Hamzaoğlu O. Ureteral stent infections: a prospective study. Braz J Infect Dis. 2017;21:361–4.
Nevo A, Mano R, Baniel J, et al. Ureteric stent dwelling time: a risk factor for post-ureteroscopy sepsis. BJU Int. 2017;120:117–22.
Özsoy M, Acar Ö, Sarica K, et al. Impact of gender on success and complication rates after ureteroscopy. World J Urol. 2015;33:1297–302.
Blackmur JP, Maitra NU, Marri RR, et al. Analysis of factors’ association with risk of postoperative urosepsis in patients undergoing ureteroscopy for treatment of stone disease. J Endourol. 2016;30:963–9.
Senocak C, Ozcan C, Sahin T, et al. Risk factors of infectious complications after flexible uretero-renoscopy with laser lithotripsy. Urol J. 2018;15:158–63.
Uchida Y, Takazawa R, Kitayama S, et al. Predictive risk factors for systemic inflammatory response syndrome following ureteroscopic laser lithotripsy. Urolithiasis. 2018;46:375–81.
Hanna B, Zhuo K, Chalasani V, et al. Association between ureteric stent dwell time and urinary tract infection. ANZ J Surg. 2021;91:187–91.
Oliver R, Ghosh A, Geraghty R, et al. Successful ureteroscopy for kidney stone disease leads to resolution of urinary tract infections: prospective outcomes with a 12-month follow-up. Cent European J Urol. 2017;70:418–23.
Türk C, Petřík A, Sarica K, et al. EAU guidelines on interventional treatment for urolithiasis. Eur Urol. 2016;69:475–82.
Nevo A, Shahait M, Shah A, et al. Defining a clinically significant struvite stone: a non-randomized retrospective study. Int Urol Nephrol. 2019;51:585–91.
Funding
This research received no external funding
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
L.J. Paulino Pereira, A.C.M. Kums, J.J.H. Beck and P.M.L. Hennus declare that they have no competing interests.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Paulino Pereira, L.J., Kums, A.C.M., Beck, J.J.H. et al. The influence of indwelling double-J stent duration prior to URS on postoperative complicated urinary tract infections. Tijdschr Urol 13, 76–82 (2023). https://doi.org/10.1007/s13629-023-00378-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13629-023-00378-1