Abstract
Introduction
Redness of the nail plate—erythronychia—is a common condition involving one or multiple digits. It may affect the entire nail or present as longitudinal red bands that extend from the proximal nail fold to the distal tip of the nail plate. Rarely, red bands may traverse the nail bed horizontally. Although erythronychia is often idiopathic, it has also been associated with amyloidosis, Darier’s disease, lichen planus, and various other cutaneous conditions. We describe the clinical features of a 64-year-old Caucasian man who presented with transverse and longitudinal erythronychia affecting his fingernails. In addition, we review the classification of erythronychia and summarize the acute and chronic conditions that have been associated with this clinical finding.
Methods
The features of a man with polydactylous transverse and longitudinal erythronychia are presented. In addition, PubMed was used to search the following terms: erythronychia, longitudinal erythronychia, red lunulae, and subungual. All papers were reviewed, and relevant articles, along with their references, were evaluated. Informed consent was obtained from the patient for being included in the study.
Results
A 64-year-old Caucasian man with a past medical history significant for testicular cancer and pulmonary embolism presented with multiple horizontal pink-red bands affecting his fingernails. The discoloration was most prominent in the region distal to the lunula. In addition, the nails of the fifth digit of his left hand and third digit of his right hand featured longitudinal red bands extending from the distal curvature of the lunula to the free edge of the nail plate. A diagnosis of polydactylous longitudinal and transverse erythronychia, based on the clinical presentation, was established. Our patient’s red bands were asymptomatic and he was not concerned about the cosmetic appearance of his nails; therefore, no additional investigation or treatment was required.
Conclusion
Polydactylous transverse erythronychia is a rare condition characterized by the development of horizontal red bands affecting the fingernails or toe nails. It has only been previously described in a man with multiple system atrophy. In our patient, both transverse and longitudinal red bands were present simultaneously. Therefore, it is possible that horizontal erythronychia is an early clinical manifestation of longitudinal erythronychia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Erythronychia—red discoloration of the nail plate—is a benign, typically asymptomatic clinical entity that may affect one or multiple digits. The nail finding is frequently idiopathic, but has also been associated with various benign and malignant conditions, including glomus tumors [1], Darier’s disease [1], malignant melanoma [2], and hemiplegia [3]. The discoloration most commonly presents as longitudinal red or pink-red bands that extend from the proximal nail fold to the distal tip of the nail plate. However, albeit rarely, red bands may also extend across the nail bed horizontally.
The clinical features of a 64-year-old man who developed not only polydactylous transverse erythronychia but also polydactylous longitudinal erythronychia are described. In addition, the classification of erythronychia is reviewed, and the acute and chronic conditions that have been associated with this clinical finding are summarized. Informed consent was obtained from the patient for being included in the study.
Case Report
A 64-year-old Caucasian man presented for evaluation of several lesions on his scalp. His past medical history was significant for testicular cancer with lung metastasis; he had been in remission for over 20 years following treatment with chemotherapy (cisplatin) and resection of his left testicle and the right lower lobe of his lung. In addition, he had developed multiple pulmonary emboli 4 years earlier and was receiving 7.5 mg of warfarin (Coumadin) orally each day.
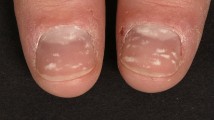
Examination of his scalp revealed multiple actinic keratoses; these lesions were treated with liquid nitrogen cryotherapy. A complete head-to-toe cutaneous examination was performed and demonstrated horizontal red-colored bands affecting six of his distal fingernails (Figs. 1, 2, 3). Prominent longitudinal red bands were also observed on the fifth digit of his left hand (Figs. 1, 2) and the third digit of his right hand (Figs. 1, 3) extending from the distal curvature of the lunula to the free edge of the nail plate.
The digits on the left hand show distinct 2- to 5-mm red bands horizontally traversing the distal nail beds of the 2nd, 3rd, and 4th digits. The arrows on the 3rd fingernail demarcate the proximal margin of the transverse red band. A linear 2-mm red band extends from the proximal nail fold to the free edge of the distal nail plate of the 5th digit
The digits on the right hand shows distinct 2- to 5-mm red bands horizontally traversing the distal nail beds of the 2nd, 4th and 5th digits. The arrows on the 4th digit demonstrate transverse erythronychia affecting the distal fingernail. A broad longitudinal 5-mm red band extends from the proximal nail fold to the free edge of the distal nail plate of the 3rd digit
The clinical presentation established the diagnoses of polydactylous transverse and longitudinal erythronychia. The red bands were asymptomatic and he was not concerned about the cosmetic appearance of his nails. Therefore, no additional investigation or treatment was required.
Discussion
Erythronychia is a benign, yet common, clinical entity characterized by red discoloration of the nails of one or multiple digits. The condition is typically asymptomatic; it may reflect discoloration of the nail plate itself or appear as a manifestation of a subungual lesion or neoplasm. Various presentations of erythronychia have been described, each of which can be classified based on location and pattern of discoloration (Table 1) [1, 4–10].
Erythronychia has been described in both men and women. There is no distinct gender predilection. It occurs most frequently among middle-aged individuals [11], but has also been reported in patients ranging in age from 18 to 87 years [11–13].
Erythronychia most commonly presents as linear red bands that extend from the proximal nail fold to the distal tip of the nail plate. This variant of erythronychia—known as “longitudinal erythronychia”—was first described by Baran and Perrin in 2000; the investigators had identified 16 individuals with “a red longitudinal streak found in the nail plate” [12].
Longitudinal erythronychia is classified based on the number of affected nails and the number of red bands present on each affected nail [14]. Four basic variants have been described: Type IA, Type IB, Type IIA, and Type IIB. Type IA describes a single red band affecting a single nail. Type IB refers to bifid red bands affecting a single nail. Type IIA describes a single red band affecting multiple nails, and Type IIB denotes multiple red bands affecting multiple nails.
Typically, the single red bands are less than 3 mm in diameter [15]. However, single bands ranging from 4 to 6 mm wide have also been described [14]. When multiple bands are present on a single nail, the width of each band is usually less than 1 mm in diameter [14].
Interestingly, longitudinal erythronychia is frequently identified in the fingernails but is rarely observed in the toenails. It has been hypothesized that discoloration affecting the subungual tissues of the toes is less likely to be visualized due to the thickness of the toenails. Alternatively, it is possible that individuals are seldom aware of changes in toenail color and thus erythronychia of the toenails is simply underdiagnosed [11, 15].
Longitudinal erythronychia is typically asymptomatic. However, albeit rarely, affected individuals may seek medical attention due to pain in the affected digit, nail fragility, or concern about the cosmetic appearance of the lesions [16].
Although longitudinal erythronychia is often idiopathic, it has also been associated with benign subungual tumors, malignant subungual tumors, and various cutaneous conditions and systemic diseases (Table 2) [1–4, 6–8, 11–13, 16–43].
Monodactylous longitudinal erythronychia, when characterized by a single linear red band on a single nail, is most often reported in individuals with benign subungual tumors such as glomus tumor [1, 2, 11, 12, 18, 19], onychopapilloma [2, 11, 12, 19, 20], and warty dyskeratoma [1, 12, 19, 21, 22]. Rarely, it has been associated with malignant subungual tumors, including squamous cell carcinoma and malignant melanoma [2, 6, 8, 11–13, 17–25]. Monodactylous longitudinal erythronychia has also been observed in patients with hemiplegia [3, 17] and those with postsurgical scars from distal digit surgery [11, 18].
Polydactylous longitudinal erythronychia, in which there are single or multiple linear red bands affecting multiple nails, may occur among individuals with cutaneous conditions such as acantholytic dyskeratotic epidermal nevus [1, 26, 27], acantholytic epidermolysis bullosa [1, 28], acrokeratosis verruciformis of Hopf [1, 6, 29–32], Darier’s disease [1, 2, 4, 7, 11, 12], and lichen planus [1, 2, 4, 11, 12, 33]. In addition, polydactylous longitudinal erythronychia has been associated with various systemic diseases including amyloidosis [1, 2, 12, 34–39], graft-versus-host disease [2, 34, 40–42], and pseudobulbar syndrome [43].
The evaluation of monodactylous longitudinal erythronychia (Type IA or Type IB) typically involves assessment for local neoplastic processes [2]. A biopsy of the affected nail or subungual tissue or both may be required to establish a diagnosis [16]. Magnetic resonance imaging can also be utilized to define a local tumor [44]. Longitudinal erythronychia associated with a dermal tumor located solely within the matrix, such as a glomus tumor, can be treated via simple excision [2, 16]. However, excision of the entire nail apparatus or amputation of the affected digit may be indicated if a malignant neoplasm is discovered [16].
Individuals who present with polydactylous longitudinal erythronychia (Type IIA or Type IIB) should be evaluated for associated cutaneous conditions and systemic diseases [2]. If an underlying condition is not detected, then a biopsy may be required in order to establish a diagnosis [2]. However, the occurrence of multiple longitudinal red bands on multiple digits is usually idiopathic and requires no additional investigation [14].
It is important to distinguish longitudinal erythronychia from longitudinal pseudoerythronychia. Longitudinal erythronychia is characterized by a non-blanchable red discoloration of the fingernails or toenails. In contrast, individuals who present with longitudinal pseudoerythronychia exhibit red bands that vary in intensity depending on the position of the digit relative to the heart. It has therefore been hypothesized that longitudinal pseudoerythronychia represents a manifestation of a local microcirculatory phenomena [14].
Histopathologic features of longitudinal erythronychia include acanthosis of the nail bed epithelium and hyperplasia of the vascular tissue of the dermal papilla in the distal matrix. In addition, there is often a distal longitudinal papillomatosis characterized by stratified layers of fusiform eosinophilic cells arranged in a V-shape. Fibrosis and inflammatory infiltrate within the distal nail bed is common. Lastly, there is frequently a distal subungual keratosis that shows parakeratosis with acanthosis and papillomatosis, multinucleated giant cells, and no dysplasia [1, 2, 11, 12].
Although erythronychia most commonly presents as longitudinal bands, our patient presented with linear pink-red bands which extended horizontally across his distal fingernails. To the best of our knowledge, this presentation of erythronychia—which may be referred to as “transverse erythronychia”—has been described in only one other individual: a 41-year-old man with a 4-year history of multiple system atrophy who presented with horizontal red bands that traversed the lateral nail folds on all of his fingernails [8]. Investigators postulated that disturbances to microcirculatory homeostatic mechanisms secondary to multiple system atrophy may have contributed to the development of the transverse erythronychia in this individual.
Longitudinal erythronychia is thought to arise due to matrix function loss and longitudinal thinning of the ventral plate [2, 11]. The thinning of the nail plate creates a longitudinal groove into which the neighboring nail bed swells, resulting in a vascular congestion that manifests as erythema. As the nail grows distally, it also becomes more susceptible to trauma from activities of daily living. The thinned nail plate may disintegrate distally, exposing the nail bed and promoting the formation of multinucleate giant cells and a protruding keratosis [2, 11].
The mechanism of pathogenesis for transverse erythronychia remains to be established. However, it is widely recognized that internal and/or external thinning of the nail plate can result in erythronychia. The most common endogenous cause of focal nail plate thinning is interruption of cell division in the nail matrix; this frequently manifests as Beau’s lines—horizontal grooves in the nail plate that grow with the nail. The most common external cause of erythronychia is filing or buffing of the dorsal surface of the nail plate. Elderly patients typically have thinner nails; therefore, focal erythronychia in the elderly may represent a non-pathologic process. Indeed, although we are aware of only one other report that specifically describes transverse erythronychia, transverse erythronychia may represent an incidental finding that is not commonly reported in the literature.
Conclusion
Erythronychia describes a benign red discoloration affecting the nails of one or multiple digits. It is most commonly observed in the fingernails, but may occasionally affect the toenails as well. Although it is most prevalent among middle-aged men and women, erythronychia has also been reported in younger individuals and the elderly.
The specific region of the nail affected in erythronychia may vary: red discoloration may appear within the nail plate, nail bed, and/or lunula. However, the most common variant of erythronychia is longitudinal erythronychia, which is characterized by a longitudinal band that travels from the proximal nail fold to the distal tip of the nail plate. Longitudinal erythronychia is classified into four categories based on the number of digits affected and the number of red bands that appear on each digit.
Transverse erythronychia is characterized by linear pink-red bands that traverse the distal fingernails horizontally. This rare variant of erythronychia has been described in only two individuals, including our patient. We hypothesize that in our patient transverse erythronychia may represent an early manifestation of erythronychia that subsequently evolves into the more common longitudinal presentation.
Erythronychia is frequently idiopathic, especially when it presents as one or more longitudinal red bands affecting multiple digits. However, longitudinal erythronychia can be associated with numerous local and systemic cutaneous conditions. Therefore, in addition to a complete clinical history, an evaluation of the nails or the patient or both may be warranted in individuals who present with red discoloration of their nails.
References
Baran R. The red nail—always benign? Actas Dermosifiliogr. 2009;100:106–13 (PMID: 20096204).
Jellinek NJ. Longitudinal erythronychia: suggestions for evaluation and management. J Am Acad Dermatol. 2011;64:167e1–11 (PMID: 20709428).
Siragusa M, Schepis C, Palazzo R, Fabrizi G, Guarneri B, Del Gracco S, Spada RS, Ferri R. Skin pathology findings in a cohort of 1500 adult and elderly subjects. Int J Dermatol. 1999;38:361–6 (PMID: 10369546).
Baran R. Red nails [abstract]. European Nail Society Meeting. 2004 Nov 17; Florence. Dermatol Online J. 2005;11(1):9.
Cohen PR. Red lunula: case report and literature review. J Am Acad Dermatol. 1992;26:292–4 (PMID: 2645322).
Baran R, Dawber RPR, Richert B. Physical signs. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management, chap 2. 3rd ed. Osney Mead: Blackwell; 2001. p. 48–103.
Cohen PR. The lunula. J Am Acad Dermatol. 1996;34:943–53 (PMID: 8647987).
Siragusa M, Del Gracco S, Elia M, Ferri R, Schepis C. Peculiar dyschromic changes of finger nails in a patient with multiple system atrophy [letter]. Int J Dermatol. 1998;37:156–60 (PMID: 9542679).
Cohen PR. Incidental (malignancy) and coincidental (idiopathic polydactylous longitudinal erythronychia) conditions in patients with segmental neurofibromatosis. Cutis. 2013;91(4):179–80 (PMID: 23763076).
Cohen PR. Longitudinal erythronychia associated with graft-versus-host disease. Skinmed. 2011;9(5):327–9 (PMID: 22165051).
de Berker DA, Perrin C, Baran R. Localized longitudinal erythronychia: diagnostic significance and physical explanation. Arch Dermatol. 2004;140:1253–7 (PMID: 15492189).
Baran R, Perrin C. Longitudinal erythronychia with distal subungual keratosis: onychopapilloma of the nail bed and Bowen’s disease. Br J Dermatol. 2000;143:132–5 (PMID: 10886147).
Harwood M, Telang GH, Robinson-Bostom L, Jellinek N. Melanoma and squamous cell carcinoma on different nails of the same hand. J Am Acad Dermatol. 2008;58:323–6 (PMID: 18222331).
de Berker D. Erythronychia. Dermatol Ther. 2012;25:603–11 (PMID: 23210759).
Cohen PR. Idiopathic polydactylous longitudinal erythronychia. J Clin Aesthet Dermatol. 2011;4(4):22–8 (PMID: 21532874).
Cohen PR. Longitudinal erythronychia: individual or multiple linear red bands of the nail plate: a review of clinical features and associated conditions. Am J Clin Dermatol. 2011;12:217–31 (PMID: 21668031).
Siragusa M, Schepis C, Cosentino FI, Spada RS, Toscano G, Ferri R. Nail pathology in patients with hemiplegia. Br J Dermatol. 2001;144:557–60 (PMID: 11260014).
Abimelec P, Dumontier C. Basic and advanced nail surgery: part 2. Indications and complications. Chapter 24. In: Scher RK, Daniel III CR, editors. Nails: diagnosis, therapy, surgery. 3rd ed. 2005; Philadelphia: Elsevier Saunders. p. 291–308.
Baran R, Haneke E, Drape J-L, Zook EG, Kreusch JF. Tumours of the nail apparatus and adjacent tissues. Chapter 11. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. 2001; Osney Mead: Blackwell. p. 515–630.
Baran R, Perrin C. Localized multinucleate distal subungual keratosis. Br J Dermatol. 1995;133:77–82 (PMID: 7669645).
Higashi N. Focal acantholytic dyskeratosis. Hifu. 1990;32:507–10.
Baran R, Perrin C. Focal subungual warty dyskeratoma. Dermatology. 1997;195:278–80 (PMID: 9407181).
Cogrel O, Beylot-Barry M, Doutre MS. Subungual squamous cell carcinoma revealed by longitudinal erythronychia. Ann Dermatol Venereol. 2008;135:883–5 (PMID: 19084707).
Reuter G, Keller F, Samama B, Boehm N. Maladie de Bowen ungueale a type d’erythronychie longitudinale: aspect dermoscopique et etude virologique. Ann Dermatol Venereol. 2005;132:569.
Dalle S, Depape L, Phan A, Balme B, Ronger-Savle S, Thomas L. Squamous cell carcinoma of the nail apparatus: clinicopathological study of 35 cases. Br J Dermatol. 2007;156:871–4 (PMID: 17263801).
Munro CS, Cox NH. An acantholytic dyskeratotic epidermal naevus with other features of Darier’s disease on the same side of the body. Br J Dermatol. 1992;127:168–71 (PMID: 1390147).
Cambiaghi S, Brusasco A, Grimalt R, Caputo R. Acantholytic dyskeratotic epidermal nevus as a mosaic form of Darier’s disease. J Am Acad Dermatol. 1995;32:284–6 (PMID: 7829719).
Hoffman MD, Fleming MG, Pearson RW. Acantholytic epidermolysis bullosa. Arch Dermatol. 1995;131:586–9 (PMID: 7741547).
Dhitavat J, Macfarlane S, Dode L, Leslie N, Sakuntabhai A, MacSween R, Saihan E, Hovnanian A. Acrokeratosis verruciformis of Hopf is caused by mutation in ATP2A2: evidence that it is allelic to Darier’s disease. J Invest Dermatol. 2003;120:229–32 (PMID: 12542527).
Juhlin L, Baran R. Hereditary and congenital nail disorders. Chapter 9. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. 2001; Osney Mead: Blackwell. p. 370–424.
Berk DR, Taube JM, Bruckner AL, Lane AT. A sporadic patient with acrokeratosis verruciformis of Hopf and a novel ATP2A2 mutation [letter]. Br J Dermatol. 2010;163:653–4 (PMID: 20518781).
Rallis E, Economidi A, Papadakis P, Verros C. Acrokeratosis verruciformis of Hopf (Hopf disease): case report and review of the literature. Dermatol Online J. 2005;11(2):10 (PMID: 16150218).
de Berker DAR, Baran R, Dawber RPR. The nail in dermatological diseases, Chap 5. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. 2001; Osney Mead: Blackwell. p. 172–222.
Tosti A, Baran R, Dawber RPR. The nail in systemic diseases and druginduced changes, Chap 6. In: Baran R, Dawber RPR, de Berker DAR, et al., editors. Baran and Dawber’s diseases of the nails and their management. 3rd ed. 2001; Osney Mead: Blackwell. p. 223–329.
Mancuso G, Fanti PA, Berdondine RM. Nail changes as the only skin abnormality inmyeloma-associated systemic amyloidosis [letter]. Br J Dermatol. 1997;137:471–2 (PMID: 9349355).
Cholez C, Cuny J-F, Pouaha J, Thomas P, Tromp G, Truchetet F. Nail abnormalities and scleroderma-like lesions on the face associated with systemic amyloidosis. Ann Dermatol Venereol. 2005;132:252–4 (PMID: 15924049).
Derrick EK, Price ML. Primary systemic amyloid with nail dystrophy. J R Soc Med. 1995;88(5):290P–1P (PMID: 7636826).
Prat C, Moreno A, Vinas M, Jucgla A. Nail dystrophy in primary systemic amyloidosis [letter]. J Eur Acad Dermatol Venereol. 2008;22:107–9 (PMID: 18181984).
Desirello G, Nazzari G, Stradini D, Fusco F, Crovato F. Primary amyloidosis. G Ital Dermatol Venereol. 1988;123:99–101 (PMID: 3410506).
Sanli H, Arat M, Oskay T, Gurman G. Evaluation of nail involvement in patients with chronic cutaneous graft versus host disease: a single-center study from Turkey. Int J Dermatol. 2004;43:176–80 (PMID: 15009386).
Palencia SI, Rodriguez-Peralto JL, Castano E, Vanaclocha F, Iglesias L. Lichenoid nail changes as sole external manifestation of graft vs. host disease. Int J Dermatol. 2002;41:44–5 (PMID: 11895513).
Liddle BJ, Cowan MA. Lichen planus-like eruption and nail changes in a patient with graft-versus-host disease [letter]. Br J Dermatol. 1990;122:841–3 (PMID: 2369565).
Siragusa M, Del Gracco S, Ferri R, Schepis C. Longitudinal red streaks on the big toenails in a patient with pseudobulbar syndrome [letter]. J Eur Acad Dermatol Venereol. 2001;15(1):85–6 (PMID: 11451339).
Drape JL. Imaging of the tumors of the perionychium. Hand Clin. 2002;18:655–70 (PMID: 12516980).
Acknowledgements
No funding or sponsorship was received for this study or publication of this article. All named authors meet the International Committee of Medical Journal Editors (ICMJE) criteria for authorship for this manuscript, take responsibility for the integrity of the work as a whole, and have given final approval for the version to be published.
Disclosures
Carina Chang, Bryce D. Beutler and Philip R. Cohen have nothing to disclose.
Compliance with Ethics Guidelines
Informed consent was obtained from the patient for being included in the study.
Data Availability
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Open Access
This article is distributed under the terms of the Creative Commons Attribution-NonCommercial 4.0 International License (http://creativecommons.org/licenses/by-nc/4.0/), which permits any noncommercial use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
Author information
Authors and Affiliations
Corresponding author
Additional information
Enhanced content
To view enhanced content for this article go to http://www.medengine.com/Redeem/9297F0601567D31E.
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (https://creativecommons.org/licenses/by/4.0), which permits use, duplication, adaptation, distribution, and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Chang, C., Beutler, B.D. & Cohen, P.R. Polydactylous Transverse Erythronychia: Report of a Patient with Multiple Horizontal Red Bands Affecting the Fingernails. Dermatol Ther (Heidelb) 7, 255–262 (2017). https://doi.org/10.1007/s13555-017-0177-2
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13555-017-0177-2