Abstract
Premature birth is a leading cause of infant mortality which is often attributed to irregular breathing and apnea of prematurity. A common treatment for apnea is caffeine to stimulate the brain’s respiratory center. However, caffeine’s long term effect on infant development is not fully comprehended. We hypothesized that noninvasive localized body stimulation regularizes breathing pattern. We investigated the impact of electrical or mechanical stimulation on breathing in mice. After the mice were ventilated for 28 s to induce apnea, mice were taken off the ventilator while receiving mechanical, electrical, or no stimulation in a randomized order. Both stimuli targeted the diaphragm area through a custom-built belt with vibrating motors or adhesive electrodes. After each apnea cycle, the time to take the first breath (T) was recorded. The electrical stimulation given at 4.5, 8.3, 16.7 V (pulse rate = 3 Hz, pulse width = 120 μs) showed no reduction in T. Electrical stimulation at pulse rates of 10 or 20 Hz (16.7 V, pulse width 260 μs) showed a detrimental effect increasing T by ~ 7% compared to control values (p = 0.005, p = 0.038 respectively). High and medium intensity mechanical stimulations significantly reduced T by 11.74 (p < 10−13) and by 17.08% (p < 10−8), respectively. Further reducing the amplitude of vibrations did not affect T. When the probe was attached to the ankles, only the high intensity vibrations resulted in a decrease in T (p < 10−13). Mechanical vibrations, applied at various intensities and locations, could be used to treat irregular breathing and apnea in infants.



Similar content being viewed by others
References
Zhao J, Gonzalez F, Mu D. Apnea of prematurity: from cause to treatment. Eur J Pediatr. 2011;170:1097–105. https://doi.org/10.1007/s00431-011-1409-6.
Frey U, Silverman M, Barabási AL, Suki B. Irregularities and power law distributions in the breathing pattern in preterm and term infants. J Appl Physiol (Bethesda, MD). 1985;1998(85):789–97. https://doi.org/10.1152/jappl.1998.85.3.789.
Eichenwald EC. Newborn C on FA. Apnea of prematurity. Pediatrics. 2015. https://doi.org/10.1542/peds.2015-3757.
Martin RJ, Abu-Shaweesh JM, Baird TM. Apnoea of prematurity. Paediatr Respir Rev. 2004;5(Suppl A):S377–82.
Schmidt B, Roberts RS, Davis P, Doyle LW, Barrington KJ, Ohlsson A, et al. Caffeine therapy for apnea of prematurity. N Engl J Med. 2006;354:2112–21. https://doi.org/10.1056/NEJMoa054065.
Steer P, Flenady V, Shearman A, Charles B, Gray PH, Henderson-Smart D, et al. High dose caffeine citrate for extubation of preterm infants: a randomised controlled trial. Arch Dis Child Fetal Neonatal Ed. 2004;89:F499–503. https://doi.org/10.1136/adc.2002.023432.
Hoecker C, Nelle M, Poeschl J, Beedgen B, Linderkamp O. Caffeine impairs cerebral and intestinal blood flow velocity in preterm infants. Pediatrics. 2002;109:784–7.
Ergenekon E, Dalgiç N, Aksoy E, Koç E, Atalay Y. Caffeine intoxication in a premature neonate. Paediatr Anaesth. 2001;11:737–9.
Anderson BJ, Gunn TR, Holford NH, Johnson R. Caffeine overdose in a premature infant: clinical course and pharmacokinetics. Anaesth Intensive Care. 1999;27:307–11.
Carnielli VP, Verlato G, Benini F, Rossi K, Cavedagni M, Filippone M, et al. Metabolic and respiratory effects of theophylline in the preterm infant. Arch Dis Child Fetal Neonatal Ed. 2000;83:F39–43.
Marcus CL, Meltzer LJ, Roberts RS, Traylor J, Dix J, D’ilario J, et al. Long-term effects of caffeine therapy for apnea of prematurity on sleep at school age. Am J Respir Crit Care Med. 2014;190:791–9. https://doi.org/10.1164/rccm.201406-1092OC.
Schmidt B, Roberts RS, Davis P, Doyle LW, Barrington KJ, Ohlsson A, et al. Long-term effects of caffeine therapy for apnea of prematurity. N Engl J Med. 2007;357:1893–902. https://doi.org/10.1056/NEJMoa073679.
Schmidt B, Anderson PJ, Doyle LW, Dewey D, Grunau RE, Asztalos EV, et al. Survival without disability to age 5 years after neonatal caffeine therapy for apnea of prematurity. JAMA. 2012;307:275–82. https://doi.org/10.1001/jama.2011.2024.
Nobile S, Carnielli VP. Caffeine for preterm infants: current indications and uncertainties. Acta Bio-Medica Atenei Parm. 2015;86(Suppl 1):32–5.
Poets CF, Khan SR. Former preterm infants, caffeine was good for you, but now beware of snoring! Am J Respir Crit Care Med. 2014;190:720–1. https://doi.org/10.1164/rccm.201409-1588ED.
Bloch-Salisbury E, Indic P, Bednarek F, Paydarfar D. Stabilizing immature breathing patterns of preterm infants using stochastic mechanosensory stimulation. J Appl Physiol (Bethesda, MD). 1985;2009(107):1017–27. https://doi.org/10.1152/japplphysiol.00058.2009.
Pichardo R, Adam JS, Rosow E, Bronzino J, Eisenfeld L. Vibrotactile stimulation system to treat apnea of prematurity. Biomed Instrum Technol. 2003;37:34–40.
Smith VC, Kelty-Stephen D, Qureshi Ahmad M, Mao W, Cakert K, Osborne J, et al. Stochastic resonance effects on apnea, bradycardia, and oxygenation: a randomized controlled trial. Pediatrics. 2015;136:e1561–8. https://doi.org/10.1542/peds.2015-1334.
Camargo VC, Honorato da Silva S, Freitas de Amorim M, Nohama P. Instrumentation for the detection and interruption of apnea episodes for premature newborn. Conf Proc Annu Int Conf IEEE Eng Med Biol Soc IEEE Eng Med Biol Soc Annu Conf. 2014;2014:2127–30. https://doi.org/10.1109/EMBC.2014.6944037.
Lovell JR, Eisenfeld L, Rosow E, Adam J, Bronzino JD. The design, development and application of a virtual instrument system to assess vibrotactile stimulation to interrupt neonatal apnea. Proc. 19th Annu. Int. Conf. IEEE Eng. Med. Biol. Soc. 1997;3:1150–3. https://doi.org/10.1109/iembs.1997.756557.
Svenningsen NW, Wittström C, Hellström-Westas L. OSCILLO-oscillating air mattress in neonatal care of very preterm babies. Technol Health Care Off J Eur Soc Eng Med. 1995;3:43–6.
Korner AF, Guilleminault C, den Hoed JV, Baldwin RB. Reduction of sleep apnea and bradycardia in preterm infants on oscillating water beds: a controlled polygraphic study. Pediatrics. 1978;61:528–33.
Williamson JR, Bliss DW, Browne DW, Indic P, Bloch-Salisbury E, Paydarfar D. Using physiological signals to predict apnea in preterm infants. 2011 Conf. Rec. Forty Fifth Asilomar Conf. Signals Syst. Comput. ASILOMAR, 2011, p. 1098–102. https://doi.org/10.1109/acssc.2011.6190183.
Hoppenbrouwers T, Hodgman JE, Harper RM, Hofmann E, Sterman MB, McGinty DJ. Polygraphic studies of normal infants during the first six months of life: III. Incidence of apnea and periodic breathing. Pediatrics. 1977;60:418–25.
Morton SU, Smith VC. Treatment options for apnoea of prematurity. Arch Dis Child Fetal Neonatal Ed. 2016;101:F352–6. https://doi.org/10.1136/archdischild-2015-310228.
Gaugler C, Marlier L, Messer J. Sensory stimulations for the treatment of idiopathic apneas of prematurity. Arch Pediatr Organe Off Soc Francaise Pediatr. 2007;14:485–9. https://doi.org/10.1016/j.arcped.2007.01.013.
Lin Y-W, Cheng C-M, LeDuc PR, Chen C-C. Understanding sensory nerve mechanotransduction through localized elastomeric matrix control. PLoS ONE. 2009;4:e4293. https://doi.org/10.1371/journal.pone.0004293.
Priplata AA, Niemi JB, Harry JD, Lipsitz LA, Collins JJ. Vibrating insoles and balance control in elderly people. Lancet Lond Engl. 2003;362:1123–4. https://doi.org/10.1016/S0140-6736(03)14470-4.
Acknowledgements
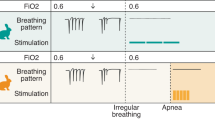
The authors thank Rana Akleh for the mouse cartoon in Fig. 1
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Research involving human participants and/or animals
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. This article does not contain any studies with human participants performed by any of the authors.
Rights and permissions
About this article
Cite this article
Bou Jawde, S., Scheuermann, A., Bartolák-Suki, E. et al. The effect of mechanical or electrical stimulation on apnea length in mice. Biomed. Eng. Lett. 8, 329–335 (2018). https://doi.org/10.1007/s13534-018-0076-1
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13534-018-0076-1