Abstract
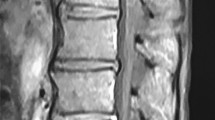
Nocardia is a Gram-positive, partially acid-fast, catalase-positive, and urease-positive bacterium that grows aerobically. We present an extremely rare case of cauda equina syndrome due to isolated intramedullary Nocardia farcinica infection. A 44-year-old male presented with low backache and gradually progressive weakness in bilateral lower limbs followed by paraplegia. He was found to have a well-defined, sharply demarcated ring-enhancing lesion located from T11-T12 to L3 vertebral body. He underwent laminectomy and decompression. The histopathological examination revealed a Gram-positive filamentous organism that looks like Nocardia. The culture report was suggestive of Nocardia farcinica. He was then treated with antibiotics and had a remarkable clinical and radiological improvement.



Similar content being viewed by others
Abbreviations
- CT scan:
-
Computed tomography scan
- MRI:
-
Magnetic resonance imaging
- ANCA:
-
Antineutrophil cytoplasmic antibody
- MPO:
-
Myeloperoxidase
- ANA:
-
Antinuclear antibody
- dsDNA:
-
Double-stranded deoxygenated nucleic acid
- ACE:
-
Angiotensin-converting enzyme
- ESR:
-
Erythrocyte sedimentation rate
- CRP:
-
C-reactive protein
- HBsAg:
-
Hepatitis B surface antigen
- DL spine:
-
Dorso-lumbar spine
- T1WI:
-
T1-weighted image
- T2WI:
-
T2-weighted image
- CSF:
-
Cerebrospinal fluid
References
Agterof MJ, van der Bruggen T, Tersmette M, ter Borg EJ, van den Bosch JM, Biesma DH (2007) Nocardiosis: a case series and a mini review of clinical and microbiological features. Neth J Med 65:199–202
Alshabani K, Buensalido JAL, Reyes MP, Soubani AO (2015) Intramedullary spinal cord abscess by Nocardia: a case report. Int J Case Rep Images 6(7):448–453
Beaman BL, Beama L (1994) Nocardia species: host–parasite relationships. Clin Microbiol Rev 7:213–264
Chatelus E, Javier RM, Sibilia J, Kuntz JL, Forestier E, Gaudias J (2007) Nocardia discitis in an immunocompetent patient. Joint Bone Spine 74:207–209
Deshmukh VR (2010) Midline trough corpectomies for the evacuation of an extensive ventral cervical and upper thoracic spinal epidural abscess. J Neurosurg Spine 13:229–233. https://doi.org/10.3171/2010.3.spine09589
Farina C, Boiron P, Goglio A, Provost F (1995) Human nocardiosis in northern Italy from 1982 to 1992. Scand J Infect Dis 27:23–27. https://doi.org/10.3109/00365549509018968
Hiller R, Singh H, Crone M (1999) Left leg paralysis in a renal transplant. Am J Kidney Dis 33(1):E4
Hong SB, Han K, Son BR, Shin KS, Rim BC (2012) First case of Nocardia nova spinal abscess in an immunocompetent patient. Braz J Infect Dis 16(2):196–199
Lee GY, Daniel RT, Brophy BP, Reilly PL (2002) Surgical treatment of nocardial brain abscesses. Neurosurgery. 51:668–672. https://doi.org/10.1227/00006123-200209000-00010
Lerner PL (1996) Nocardiosis. Clin Infect Dis 22:891–905
Schlaberg R, Fisher MA, Hanson KE (2014) Susceptibility profiles of Nocardia isolates based on current taxonomy. Antimicrob Agents Chemother 58(2):795–800
Siao P, McCabe P, Yagnik P (1989) Nocardial spinal epidural abscess. Neurology 39:996. https://doi.org/10.1212/wnl.39.7.996
Smith PW, Steinkraus GE, Henricks BW, Madson EC (1980) CNS nocardiosis: response to sulfamethoxazole-trimethoprim. ArchNeurol 37:729730. https://doi.org/10.1001/archneur.1980.00500600077017
Sorrell TC, Mitchell DH, Iredell JR, Chen SC-A. (2010) Nocardia species. In: Principles and practice of infectious diseases, 7, Mandell GL, Bennett JE, Dolin R (Eds), Churchill Livingstone Elsevier, Philadelphia; p. 3199
Welsh JD, Rhoades ER, Jaques W (1961) Disseminated nocardiosis involving spinal cord. Case report. Arch Intern Med Title 108:73–79. https://doi.org/10.1001/archinte.1961.03620070075009
Acknowledgments
The authors would like to acknowledge the patient who agreed to be a part of this case study. Also, we would like to acknowledge our hospital’s academic department and library which helped us immensely with the research work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chakraborty, T., Vyas, M., Goyal, A. et al. A rare case of isolated cauda equina Nocardia farcinica infection. J. Neurovirol. 26, 615–618 (2020). https://doi.org/10.1007/s13365-020-00863-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13365-020-00863-y