Abstract
Metastatic non-small cell lung cancer (NSCLC) is refractory with a very poor prognosis. Docetaxel (DTX) injection (Taxotere®) has been approved for the treatment of locally advanced or metastatic NSCLC. However, its clinical application is restricted by severe adverse effects and non-selective tissue distribution. In this study, we successfully developed DTX-loaded human serum albumin (HSA) nanoparticles (DNPs) with modified Nab technology, by introducing medium-chain triglyceride (MCT) as a stabilizer. The optimized formulation had a particle size of approximately 130 nm and a favorable stabilization time of more than 24 h. DNPs dissociated in circulation in a concentration-dependent manner and slowly released DTX. Compared with DTX injection, DNPs were more effectively taken up by NSCLC cells, thus exerting stronger inhibitory effects on their proliferation, adhesion, migration, and invasion. In addition, DNPs showed prolonged blood retention and increased tumor accumulation relative to DTX injection. Ultimately, DNPs produced more potent inhibitory effects on primary or metastatic tumor foci than DTX injections but caused markedly lower organ toxicity and hematotoxicity. Overall, these results support that DNPs hold great potential for the treatment of metastatic NSCLC in clinical.
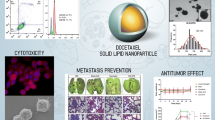
Graphical Abstract









Similar content being viewed by others
Availability of data and materials
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Herbst RS, MorgenszternC D. Boshoff The biology and management of non-small cell lung cancer. Nature. 2018;553:446–54.
Akanda ZZ, Neeson PJ, John T, Barnett S, Hanna GG, et al. A narrative review of combined stereotactic ablative radiotherapy and immunotherapy in metastatic non-small cell lung cancer. Transl Lung Cancer Res. 2021;10:2766–78.
Davies AM, Lara PN Jr., Mack PC, Gandara DR. Docetaxel in non-small cell lung cancer: a review. Expert Opin Pharmacother. 2003;4:553–65.
de Weger VA, Beijnen JH, Schellens JH. Cellular and clinical pharmacology of the taxanes docetaxel and paclitaxel-a review. Anticancer Drugs. 2014;25:488–94.
Lemjabbar-Alaoui H, Hassan OU, YangP YW. Buchanan Lung cancer: biology and treatment options. Biochim Biophys Acta. 2015;1856:189–210.
ten Tije AJ, Verweij J, LoosA WJ. Sparreboom Pharmacological effects of formulation vehicles : implications for cancer chemotherapy. Clin Pharmacokinet. 2003;42:665–85.
Bissery MC. Preclinical pharmacology of docetaxel. Eur J Cancer. 1995;31A(Suppl 4):S1-6.
Kratz F. A clinical update of using albumin as a drug vehicle - a commentary. J Control Release. 2014;190:331–6.
Desai N, Trieu V, Yao Z, Louie L, Ci S, et al. Increased antitumor activity, intratumor paclitaxel concentrations, and endothelial cell transport of cremophor-free, albumin-bound paclitaxel, ABI-007, compared with cremophor-based paclitaxel. Clin Cancer Res. 2006;12:1317–24.
Kamphorst JJ, Nofal M, Commisso C, Hackett SR, Lu W, et al. Human pancreatic cancer tumors are nutrient poor and tumor cells actively scavenge extracellular protein. Cancer Res. 2015;75:544–53.
Yardley DA. nab-Paclitaxel mechanisms of action and delivery. J Control Release. 2013;170:365–72.
Kushwah V, Katiyar SS, Dora CP, Kumar Agrawal A, Lamprou AA, et al. Co-delivery of docetaxel and gemcitabine by anacardic acid modified self-assembled albumin nanoparticles for effective breast cancer management. Acta Biomater. 2018;73:424–36.
Kordezangeneh M, Irani S, Mirfakhraie R, Esfandyari-Manesh M, Atyabi F, et al. Regulation of BAX/BCL2 gene expression in breast cancer cells by docetaxel-loaded human serum albumin nanoparticles. Med Oncol. 2015;32:208.
Li CL, Li YH, Gao YQ, Wei N, Zhao X, et al. Direct comparison of two albumin-based paclitaxel-loaded nanoparticle formulations: is the crosslinked version more advantageous? Int J Pharmaceut. 2014;468:15–25.
Sato T, Okazaki M, Sano J, Kato C, Shimizu K, et al. Binding affinities of paclitaxel and docetaxel for generic and nanoparticle albumin-bound paclitaxel-derived albumin from human serum. Biomed Rep. 2021;14:35.
Fanali G, di Masi A, Trezza V, Marino M, Fasano M, et al. Human serum albumin: from bench to bedside. Mol Aspects Med. 2012;33:209–90.
Sohail MF, Rehman M, Sarwar HS, Naveed S, Salman O, et al. Advancements in the oral delivery of Docetaxel: challenges, current state-of-the-art and future trends. Int J Nanomed. 2018;13:3145–61.
Cheng HX, Liu H, Zhang YY, Zou GL. Interaction of the docetaxel with human serum albumin using optical spectroscopy methods. J Lumin. 2009;129:1196–203.
Elsadek BF. Kratz Impact of albumin on drug delivery - new applications on the horizon. J Control Release. 2012;157:4–28.
Kratz F. Albumin as a drug carrier: design of prodrugs, drug conjugates and nanoparticles. J Control Release. 2008;132:171–83.
Clarke SJLP. Rivory Clinical pharmacokinetics of docetaxel. Clin Pharmacokinet. 1999;36:99–114.
Torzilli PA, Bourne JW, Cigler T, Vincent CT. A new paradigm for mechanobiological mechanisms in tumor metastasis. Semin Cancer Biol. 2012;22:385–95.
Park K. Albumin: a versatile carrier for drug delivery. J Control Release. 2012;157:3–3.
Kellar A, EganD C. Morris Preclinical murine models for lung cancer: clinical trial applications. Biomed Res Int. 2015;2015: 621324.
Wood SL, Pernemalm M, Crosbie PA, Whetton AD. The role of the tumor-microenvironment in lung cancer-metastasis and its relationship to potential therapeutic targets. Cancer Treat Rev. 2014;40:558–66.
Mazzaccara C, Labruna G, Cito G, Scarfo M, De Felice M, et al. Age-related reference intervals of the main biochemical and hematological parameters in C57BL/6J, 129SV/EV and C3H/HeJ mouse strains. PLoS ONE. 2008;3: e3772.
Hu K, Miao L, Goodwin TJ, Li J, Liu Q, et al. Quercetin remodels the tumor microenvironment to improve the permeation, retention, and antitumor effects of nanoparticles. ACS Nano. 2017;11:4916–25.
Funding
This work was supported by the Shanghai Municipal Natural Science Foundation (19ZR1406200) and the National Natural Science Foundation of China (Grant No. 81872428 and 81703010).
Author information
Authors and Affiliations
Contributions
Yunlong Cheng: methodology, software, validation, formal analysis, investigation, and writing — original draft. Xiaoying Pang: methodology, software, validation, resources, formal analysis, and investigation. Jing Wu: methodology, software, validation, resources, and formal analysis. Lingling Zhou: methodology, software, and validation. Jingxu Cao, Liuchang Wang, Kang Qian, Peng Yang, Minjun Xu, Dongyu Sheng, Ran Meng, Pengzhen Wang, Qian Guo, and Shuting Xu: methodology and validation. Yan Wei: conceptualization, resources, and writing — review and editing, and funding acquisition. Qizhi Zhang: conceptualization; resources; writing, review and editing; supervision; project administration; and funding acquisition. All authors reviewed the results and approved the final version of the manuscript.
Corresponding authors
Ethics declarations
Ethics approval and consent to participate
Ethical approval to conduct the study was obtained from the Institutional Animal Care and Use Committee (IACUC) of the School of Pharmacy, Fudan University (approval number: SYXK(Hu) 2015–0023).
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cheng, Y., Pang, X., Wu, J. et al. Medium-chain triglyceride-stabilized docetaxel-loaded HSA nanoparticles effectively inhibited metastatic non-small cell lung cancer. Drug Deliv. and Transl. Res. 13, 2869–2884 (2023). https://doi.org/10.1007/s13346-023-01355-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-023-01355-2