Abstract
Topical preparations of hydrocortisone can be used for the anti-inflammatory treatment of the female genital area. Although the drug is a low-strength corticosteroid, systemic absorption and distribution of the drug are the most common safety risks associated with this therapy. In the current investigation, we elucidate the physicochemical properties of lipid-based drug carrier systems that govern the local bioavailability of hydrocortisone for intravaginal administration. For this purpose, we compared various proliposome formulations with a commercial cream. Depending on the availability of physiological acceptors, encapsulation and drug release from the lipid phase were found to be the most important drivers of drug bioavailability. The high permeability of hydrocortisone leads to rapid transport of the drug across the mucosal cell layer as indicated by experiments using HEC-1-A and CaSki cell monolayer models. Under sink conditions, differences in the release from the liposomes as determined in the Dispersion Releaser were almost negligible. However, under non-sink conditions, the drug release plateaued at levels corresponding to the encapsulation efficiency. After redispersion, all liposomal formulations performed better than the commercial drug product indicating that the encapsulation into the lipid phase is the main driver sustaining the release.
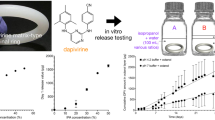
Graphical Abstract






Similar content being viewed by others
Availability of data and materials
Materials are commercially available; data will be made available on request.
Abbreviations
- ANOVA:
-
Analysis of variance
- β-CD:
-
Methyl-β-cyclodextrin
- C:
-
Cholesterol
- Caco-2:
-
Carcinoma colon
- CaSki:
-
Human cervical carcinoma
- CC50 :
-
Half-maximal cytotoxic concentration
- CE:
-
Cellulose ester
- DLS:
-
Dynamic light scattering
- DSC:
-
Differential scanning calorimetry
- EE%:
-
Encapsulation efficiency
- EPC:
-
Egg phosphatidylcholine
- f1:
-
Difference factor
- f2:
-
Similarity factor
- HBSS:
-
Hank’s Balanced Salt solution
- HEC-1-A:
-
Human endometrial adenocarcinoma
- HPLC-UV:
-
High-performance liquid chromatography with ultraviolet detection
- LOD:
-
Limit of detection
- LOQ:
-
Limit of quantitation
- MWCO:
-
Molecular weight cutoff
- Papp :
-
Apparent permeability coefficients
- PDI:
-
Polydispersity index
- PER:
-
Permeability enhancement ratio
- PTDR:
-
Pharma Test Dispersion Releaser
- PTFE:
-
Polytetrafluoroethylene
- SPC:
-
Soy phosphatidylcholine
- sVSF:
-
Simplified vaginal simulant fluid
- SE:
-
Standard error
- SD:
-
Standard deviation
- TEER:
-
Transepithelial electrical resistance
- TEM:
-
Transmission electron microscopy
- US-FDA:
-
United States Food and Drug Administration
References
das Neves J, Notario-Pérez F, Sarmento B. Women-specific routes of administration for drugs: a critical overview. Adv Drug Deliv Rev. 2021;176:113865.
Pavelić Ž, Škalko-Basnet N, Schubert R. Liposomal gels for vaginal drug delivery. Int J Pharm. 2001;219:139–49.
das Neves J, Amiji M, Sarmento B. Mucoadhesive nanosystems for vaginal microbicide development: friend or foe? WIREs Nanomed Nanobiotechnol. 2011;3:389–99.
Vanić Ž, Škalko-Basnet N. Nanopharmaceuticals for improved topical vaginal therapy: can they deliver? Eur J Pharm Sci. 2013;50:29–41.
Richardson JL, Whetstone J, Fisher AN, Watts P, Farraj NF, Hinchcliffe M, et al. Gamma-scintigraphy as a novel method to study the distribution and retention of a bioadhesive vaginal delivery system in sheep. J Control Release. 1996;42:133–42.
Vermani K, Garg S. The scope and potential of vaginal drug delivery. Pharm Sci Technol Today. 2000;3:359–64.
Patravale VB, Mandawgade SD. Novel cosmetic delivery systems: an application update. Int J Cosmet Sci. 2008;30:19–33.
Zhang H. Thin-film Hydration Followed by Extrusion Method for Liposome Preparation. In: D’Souza GGM, editor. Liposomes: Methods and Protocols. New York, NY: Springer New York 2017;17–22.
Batavia R, Taylor KMG, Craig DQM, Thomas M. The measurement of beclomethasone dipropionate entrapment in liposomes: a comparison of a microscope and an HPLC method. Int J Pharm. 2001;212:109–19.
Darwis Y, Kellaway IW. Nebulisation of rehydrated freeze-dried beclomethasone dipropionate liposomes. Int J Pharm. 2001;215:113–21.
Elhissi AMA, O’Neill MAA, Roberts SA, Taylor KMG. A calorimetric study of dimyristoylphosphatidylcholine phase transitions and steroid–liposome interactions for liposomes prepared by thin film and proliposome methods. Int J Pharm. 2006;320:124–30.
Shah H, Madni A, Rahim MA, Jan N, Khan A, Khan S, et al. Fabrication, in vitro and ex vivo evaluation of proliposomes and liposomal derived gel for enhanced solubility and permeability of diacerein. PLoS ONE. 2021;16: e0258141.
Gala RP, Khan I, Elhissi AMA, Alhnan MA. A comprehensive production method of self-cryoprotected nano-liposome powders. Int J Pharm. 2015;486:153–8.
das Neves J, Nunes R, Machado A, Sarmento B. Polymer-based nanocarriers for vaginal drug delivery. Adv Drug Deliv Rev. 2015;92:53–70.
Pavelić Ž, Škalko-Basnet N, Filipović-Grčić J, Martinac A, Jalšenjak I. Development and in vitro evaluation of a liposomal vaginal delivery system for acyclovir. J Control Release. 2005;106:34–43.
Berginc K, Suljaković S, Škalko-Basnet N, Kristl A. Mucoadhesive liposomes as new formulation for vaginal delivery of curcumin. Eur J Pharm Biopharm. 2014;87:40–6.
Hunt CA, Tsang S. α-Tocopherol retards autoxidation and prolongs the shelf-life of liposomes. Int J Pharm. 1981;8:101–10.
Grit M, Crommelin DJA. Chemical stability of liposomes: implications for their physical stability. Chem Phys Lipid. 1993;64:3–18.
Wong M, Thompson TE. Aggregation of dipalmitoylphosphatidylcholine vesicles. Biochemistry. 1982;21:4133–9.
Payne NI, Ambrose CV, Timmins P, Ward MD, Ridgway F. Proliposomes: a novel solution to an old problem. J Pharm Sci. 1986;75:325–9.
Payne NI, Browning I, Hynes CA. Characterization of proliposomes. J Pharm Sci. 1986;75:330–3.
Perrett S, Golding M, Williams WP. A simple method for the preparation of liposomes for pharmaceutical applications: characterization of the liposomes. J Pharm Pharmacol. 1991;43:154–61.
Alves GP, Santana MHA. Phospholipid dry powders produced by spray drying processing: structural, thermodynamic and physical properties. Powder Technol. 2004;145:139–48.
Parhizkar E, Sadeghinia D, Hamishehkar H, Yaqoubi S, Nokhodchi A, Alipour S. Carrier effect in development of rifampin loaded proliposome for pulmonary delivery: a quality by design study. Adv Pharm Bull. 2022;12:336–45.
Chen C-M, Alli D. Use of fluidized bed in proliposome manufacturing. J Pharm Sci. 1987;76:419.
Kumar R, Gupta RB, Betegeri G. Formulation, characterization, and in vitro release of glyburide from proliposomal beads. Drug Delivery. 2001;8:25–7.
Singh N, Kushwaha P, Ahmad U, Abdullah M. Proliposomas: Una aproximación para el desarrollo de liposoma estables. Ars Pharmaceutica (Internet). 2019;60:231–40.
Xia F, Hu D, Jin H, Zhao Y, Liang J. Preparation of lutein proliposomes by supercritical anti-solvent technique. Food Hydrocoll. 2012;26:456–63.
Xia F, Jin H, Zhao Y, Guo X. Supercritical antisolvent-based technology for preparation of vitamin D3 proliposome and its characteristics. Chin J Chem Eng. 2011;19:1039–46.
Chu C, Tong S-s, Xu Y, Wang L, Fu M, Ge Y-r, et al. Proliposomes for oral delivery of dehydrosilymarin: preparation and evaluation in vitro and in vivo. Acta Pharmacol Sinica. 2011;32:973–80.
Kurakula M, Srinivas C, Kasturi N, Diwan PD. Formulation and evaluation of prednisolone proliposomal gel for effective topical pharmacotherapy. Int J Pharm Sci Drug Res. 2012;4:35–43.
Rojanarat W, Nakpheng T, Thawithong E, Yanyium N, Srichana T. Levofloxacin-proliposomes: opportunities for use in lung tuberculosis. Pharmaceutics. 2012;4:385–412.
Ning M-Y, Guo Y-Z, Pan H-Z, Yu H-M, Gu Z-W. Preparation and evaluation of proliposomes containing clotrimazole. Chem Pharm Bull. 2005;53:620–4.
Anderson M, Kutzner S, Kaufman RH. Treatment of vulvovaginal lichen planus with vaginal hydrocortisone suppositories. Obstet Gynecol. 2002;100:359–62.
Manfre M, Adams D, Callahan G, Gould P, Lang S, McCubbins H, et al. Hydrocortisone cream to reduce perineal pain after vaginal birth: a randomized controlled trial. MCN Am J Matern Child Nurs. 2015;40.
Lennernäs H, Skrtic S, Johannsson G. Replacement therapy of oral hydrocortisone in adrenal insufficiency: the influence of gastrointestinal factors. Expert Opin Drug Metab Toxicol. 2008;4:749–58.
Corbo DC, Liu J-C, Chien YW. Drug absorption through mucosal membranes: effect of mucosal route and penetrant hydrophilicity. Pharm Res. 1989;6:848–52.
das Neves J, Araújo F, Andrade F, Michiels J, Ariën KK, Vanham G, et al. In vitro and ex vivo evaluation of polymeric nanoparticles for vaginal and rectal delivery of the anti-HIV drug dapivirine. Mol Pharm. 2013;10:2793–807.
das Neves J, Sarmento B. Precise engineering of dapivirine-loaded nanoparticles for the development of anti-HIV vaginal microbicides. Acta Biomater. 2015;18:77–87.
Facchinatto WM, Galante J, Mesquita L, Silva DS, Martins dos Santos D, Moraes TB, et al. Clotrimazole-loaded N-(2-hydroxy)-propyl-3-trimethylammonium, O-palmitoyl chitosan nanoparticles for topical treatment of vulvovaginal candidiasis. Acta Biomater. 2021;125:312–21.
Grammen C, Augustijns P, Brouwers J. In vitro profiling of the vaginal permeation potential of anti-HIV microbicides and the influence of formulation excipients. Antiviral Res. 2012;96:226–33.
Notario-Pérez F, Galante J, Martín-Illana A, Cazorla-Luna R, Sarmento B, Ruiz-Caro R, et al. Development of pH-sensitive vaginal films based on methacrylate copolymers for topical HIV-1 pre-exposure prophylaxis. Acta Biomater. 2021;121:316–27.
Janas C, Mast MP, Kirsamer L, Angioni C, Gao F, Mantele W, et al. The dispersion releaser technology is an effective method for testing drug release from nanosized drug carriers. Eur J Pharm Sci. 2017;115:73–83.
Mast M-P, Modh H, Knoll J, Fecioru E, Wacker MG. An update to dialysis-based drug release testing - data analysis and validation using the Pharma Test Dispersion Releaser. Pharmaceutics. 2021;13:12.
Turpeinen U, Markkanen H, Välimäki M, Stenman UH. Determination of urinary free cortisol by HPLC. Clin Chem. 1997;43:1386–91.
Präbst K, Engelhardt H, Ringgeler S, Hübner H. Basic colorimetric proliferation assays: MTT, WST, and resazurin. In: Gilbert DF, Friedrich O, editors. Cell viability assays: methods and protocols. New York, NY: Springer New York. 2017;1–17.
Commission CP. Chinese Pharmacoepia (Ch.P.) 10th Edition. 2015.
Rastogi R, Su J, Mahalingam A, Clark J, Sung S, Hope T, et al. Engineering and characterization of simplified vaginal and seminal fluid simulants. Contraception. 2016;93:337–46.
Danaei M, Dehghankhold M, Ataei S, Hasanzadeh Davarani F, Javanmard R, Dokhani A, et al. Impact of particle size and polydispersity index on the clinical applications of lipidic nanocarrier systems. Pharmaceutics. 2018;10:2.
Nezzal A, Aerts L, Verspaille M, Henderickx G, Redl A. Polymorphism of sorbitol. J Cryst Growth. 2009;311:3863–70.
Khan I, Yousaf S, Subramanian S, Korale O, Alhnan MA, Ahmed W, et al. Proliposome powders prepared using a slurry method for the generation of beclometasone dipropionate liposomes. Int J Pharm. 2015;496:342–50.
Suitchmezian V, Jeß I, Näther C. Structural, thermodynamic, and kinetic aspects of the trimorphism of hydrocortisone. J Pharm Sci. 2008;97:4516–27.
Byeon JC, Lee S-E, Kim T-H, Ahn JB, Kim D-H, Choi J-S, et al. Design of novel proliposome formulation for antioxidant peptide, glutathione with enhanced oral bioavailability and stability. Drug Delivery. 2019;26:216–25.
Hazemoto N, Harada M, Suzuki S, Kaiho F, Haga M, Kato Y. Effect of phosphatidylcholine and cholesterol on pH-sensitive liposomes. Chem Pharm Bull (Tokyo). 1993;41:1003–6.
Naylor LJ, Bakatselou V, Dressman JB. Comparison of the mechanism of dissolution of hydrocortisone in simple and mixed micelle systems. Pharm Res. 1993;10:865–70.
Standardization IOf. ISO 10993–5:2009 Biological Evaluation of Medical Devices - Part 5: tests for in vitro cytotoxicity. Geneva, Switzerland. 2009.
Gorodeski GI. Estrogen increases the permeability of the cultured human cervical epithelium by modulating cell deformability. Am J Physiol Cell Physiol. 1998;275:C888–99.
Machado RM, Palmeira-de-Oliveira A, Gaspar C, Martinez-de-Oliveira J, Palmeira-de-Oliveira R. Studies and methodologies on vaginal drug permeation. Adv Drug Deliv Rev. 2015;92:14–26.
Heimbach T, Oh D-M, Li LY, Forsberg M, Savolainen J, Leppänen J, et al. Absorption rate limit considerations for oral phosphate prodrugs. Pharm Res. 2003;20:848–56.
Cao Z, Zhang X, Wang C, Liu L, Zhao L, Wang J, et al. Different effects of cholesterol on membrane permeation of arginine and tryptophan revealed by bias-exchange metadynamics simulations. J Chem Phys. 2019;150: 084106.
Zhang L, Bennett WFD, Zheng T, Ouyang P-K, Ouyang X, Qiu X, et al. Effect of cholesterol on cellular uptake of cancer drugs pirarubicin and ellipticine. J Phys Chem B. 2016;120:3148–56.
Ramanathan R, Jiang Y, Read B, Golan-Paz S, Woodrow KA. Biophysical characterization of small molecule antiviral-loaded nanolipogels for HIV-1 chemoprophylaxis and topical mucosal application. Acta Biomater. 2016;36:122–31.
Jøraholmen MW, Basnet P, Acharya G, Škalko-Basnet N. PEGylated liposomes for topical vaginal therapy improve delivery of interferon alpha. Eur J Pharm Biopharm. 2017;113:132–9.
Acknowledgements
Marc-Phillip Mast acknowledges the State of Hessen for financial contributions to the LOEWE research center for Translational Medicine and Pharmacology (Frankfurt, Germany). Matthias G. Wacker acknowledges the Singaporean Ministry of Education (A-0004627-00-00) and the Resilience & Growth Fund of the National Research Foundation (A-0000065-09-00) for financial support. José das Neves acknowledges financing by Portuguese funds through FCT – Fundação para a Ciência e a Tecnologia/Ministério da Ciência, Tecnologia e Ensino Superior in the framework of the project “Institute for Research and Innovation in Health Sciences” (UID/BIM/04293/2019). This work was supported by the Ministry of Science and Higher Education of the Russian Federation (grant No. 075-15-2020-792, Unique identifier RF-190220X0031).
Funding
All funding sources have been declared under Acknowledgements.
Author information
Authors and Affiliations
Contributions
Conceptualization: MPM, MGW; investigation: MPM, LM; writing—original draft preparation: MPM; writing—review and editing: MPM, KG, JdN, MGW, S.G.; funding acquisition: JdN, MGW; supervision: JdN, MGW, SG. All authors have read and agreed to the published version of the manuscript.
Corresponding authors
Ethics declarations
Ethics approval
Not applicable.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mast, MP., Mesquita, L., Gan, K. et al. Encapsulation and release of hydrocortisone from proliposomes govern vaginal delivery. Drug Deliv. and Transl. Res. 13, 1022–1034 (2023). https://doi.org/10.1007/s13346-022-01263-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-022-01263-x