Abstract
Dissolving microneedle (MN) patches are usually formulated with a blend of drug and excipients added for mechanical strength and drug stabilization. In this study, we developed MNs made of pure drug to maximize drug loading capacity. MN patches were fabricated for transdermal delivery of montelukast sodium (MS) which is used to treat asthma and allergic rhinitis. We developed three different fabrication methods — solvent casting, melt casting, and solvent washing — and determined that filling molds with MS powder followed by a solvent washing method enabled MS to be loaded selectively to the MNs. Drug localization was confirmed with Raman imaging. MNs were able to penetrate in vitro and ex vivo skin models, and maintained strong mechanical properties during 6 months’ storage at 22 °C. MS was also stable and compatible with the formulation used for the patch backing layer after 3 months’ storage at 40 °C. MS delivery efficiency into skin was 55%, which enabled delivery of 3.2 mg MS into porcine skin ex vivo, which is in the range of MS doses in human clinical use. We conclude that the solvent washing method can be used to prepare MNs containing pure drug, such as MS at milligram doses in a ~ 1 cm2 MN patch.
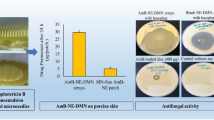
Graphical abstract









Similar content being viewed by others
Availability of data and material
Data are available by contacting the authors.
Code availability
Not applicable.
References
Caminati M, Morais-Almeida M, Bleecker E, Ansotegui I, Canonica GW, Bovo C, et al. Biologics and global burden of asthma: a worldwide portrait and a call for action. World Allergy Organ J. 2021. https://doi.org/10.1016/j.waojou.2020.100502.
May JR, Dolen WK. Management of allergic rhinitis: a review for the community pharmacist. Clin Ther. 2017. https://doi.org/10.1016/j.clinthera.2017.10.006.
Peters-Golden M, Gleason MM, Togias A. Cysteinyl leukotrienes: multi-functional mediators in allergic rhinitis. Clin Exp Allergy. 2006. https://doi.org/10.1111/j.1365-2222.2006.02498.x.
Panchal R, Patel H, Patel V, Joshi P, Parikh A. Formulation and evalution of montelukast sodium - chitosan based spray dried microspheres for pulmonary drug delivery. J Pharm Bioallied Sci. 2012. https://doi.org/10.4103/0975-7406.94160.
Barbosa JS, Almeida Paz FA, Braga SS. Montelukast medicines of today and tomorrow: from molecular pharmaceutics to technological formulations. Drug Deliv. 2016. https://doi.org/10.3109/10717544.2016.1170247.
Azizoglu E, Ozer O. Fabrication of montelukast sodium loaded filaments and 3D printing transdermal patches onto packaging material. Int J Pharm. 2020. https://doi.org/10.1016/j.ijpharm.2020.119588.
Im SH, Jung HT, Ho MJ, Lee JE, Kim HT, Kim DY, et al. Montelukast nanocrystals for transdermal delivery with improved chemical stability. Pharmaceutics. 2019. https://doi.org/10.3390/pharmaceutics12010018.
Patil-Gadhe A, Pokharkar V. Montelukast-loaded nanostructured lipid carriers: Part I Oral bioavailability improvement. Eur J Pharm Biopharm. 2014. https://doi.org/10.1016/j.ejpb.2014.05.019.
Almajidi YQ, Mahdi ZH, Maraie NK. Preparation and in vitro evaluation of montelukast sodium oral nanoemulsion. Int J Appl Pharm. 2018. https://doi.org/10.22159/ijap.2018v10i5.28367.
Ingrole RSJ, Azizoglu E, Dul M, Birchall JC, Gill HS, Prausnitz MR. Trends of microneedle technology in the scientific literature, patents, clinical trials and internet activity. Biomaterials. 2021. https://doi.org/10.1016/j.biomaterials.2020.120491.
Prausnitz MR. Engineering microneedle patches for vaccination and drug delivery to skin. Annu Rev Chem Biomol Eng. 2017. https://doi.org/10.1146/annurev-chembioeng-060816-101514.
Ahmed Saeed Al-Japairai K, Mahmood S, Hamed Almurisi S, Reddy Venugopal J, Rebhi Hilles A, Azmana M, et al. Current trends in polymer microneedle for transdermal drug delivery. Int J Pharm. 2020. https://doi.org/10.1016/j.ijpharm.2020.119673.
Nagarkar R, Singh M, Nguyen HX, Jonnalagadda S. A review of recent advances in microneedle technology for transdermal drug delivery. J Drug Deliv Sci Technol. 2020. https://doi.org/10.1016/j.jddst.2020.101923.
Sawatdee S, Nakpheng T, Wan Yi BT, Yu Shen BT, Nallamolu S, Srichana T. Formulation development and in-vitro evaluation of montelukast sodium pressurized metered dose inhaler. J Drug Deliv Sci Technol. 2020. https://doi.org/10.1016/j.jddst.2020.101534.
Lee JW, Park J-H, Prausnitz MR. Dissolving microneedles for transdermal drug delivery. Biomaterials. 2008. https://doi.org/10.1016/j.biomaterials.2007.12.048.
Arya J, Prausnitz MR. Microneedle patches for vaccination in developing countries. J Control Release. 2016. https://doi.org/10.1016/j.jconrel.2015.11.019.
Yang J, Liu X, Fu Y, Song Y. Recent advances of microneedles for biomedical applications: drug delivery and beyond. Acta Pharm Sin B. 2019. https://doi.org/10.1016/j.apsb.2019.03.007.
Rouphael NG, Paine M, Mosley R, Henry S, McAllister D V, Kalluri H, et al. The safety, immunogenicity, and acceptability of inactivated influenza vaccine delivered by microneedle patch (TIV-MNP 2015): a randomised, partly blinded, placebo-controlled, phase 1 trial. Lancet. 2017.https://doi.org/10.1016/S0140-6736(17)30575-5.
Fernando GJP, Hickling J, Jayashi Flores CM, Griffin P, Anderson CD, Skinner SR, et al. Safety, tolerability, acceptability and immunogenicity of an influenza vaccine delivered to human skin by a novel high-density microprojection array patch (NanopatchTM). Vaccine. 2018. https://doi.org/10.1016/j.vaccine.2018.05.053.
Duarah S, Sharma M, Wen J. Recent advances in microneedle-based drug delivery: special emphasis on its use in paediatric population. Eur J Pharm Biopharm. 2019. https://doi.org/10.1016/j.ejpb.2019.01.005.
Mooney K, McElnay JC, Donnelly RF. Paediatricians’ opinions of microneedle-mediated monitoring: a key stage in the translation of microneedle technology from laboratory into clinical practice. Drug Deliv Transl Res. 2015. https://doi.org/10.1007/s13346-015-0223-5.
McCrudden MTC, Alkilani AZ, McCrudden CM, McAlister E, McCarthy HO, Woolfson a D, et al. Design and physicochemical characterisation of novel dissolving polymeric microneedle arrays for transdermal delivery of high dose, low molecular weight drugs. J Control Release. 2014. https://doi.org/10.1016/j.jconrel.2014.02.007.
Ripolin A, Quinn J, Larrañeta E, Vicente-Perez EM, Barry J, Donnelly RF. Successful application of large microneedle patches by human volunteers. Int J Pharm. 2017. https://doi.org/10.1016/j.ijpharm.2017.02.011.
Kathuria H, Li H, Pan J, Lim SH, Kochhar JS, Wu C, et al. Large size microneedle patch to deliver lidocaine through skin. Pharm Res. 2016. https://doi.org/10.1007/s11095-016-1991-4.
Zhan H, Ma F, Huang Y, Zhang J, Jiang X, Qian Y. Application of composite dissolving microneedles with high drug loading ratio for rapid local anesthesia. Eur J Pharm Sci. 2018. https://doi.org/10.1016/j.ejps.2018.06.014.
Kim S, Yang H, Eum J, Ma Y, Fakhraei Lahiji S, Jung H. Implantable powder-carrying microneedles for transdermal delivery of high-dose insulin with enhanced activity. Biomaterials. 2020. https://doi.org/10.1016/j.biomaterials.2019.119733.
Kim YC, Lee JW, Esser ES, Kalluri H, Joyce JC, Compans RW, et al. Fabrication of microneedle patches with lyophilized influenza vaccine suspended in organic solvent. Drug Deliv Transl Res. 2021. https://doi.org/10.1007/s13346-021-00927-4.
Chu LY, Choi S-O, Prausnitz MR. Fabrication of dissolving polymer microneedles for controlled drug encapsulation and delivery: bubble and pedestal microneedle designs. J Pharm Sci. 2010. https://doi.org/10.1002/jps.22140.
Lee JN, Park C, Whitesides GM. Solvent compatibility of poly(dimethylsiloxane)-based microfluidic devices. Anal Chem. 2003. https://doi.org/10.1021/ac0346712.
Vekaria H, Limbasiya V, Patel P. Development and validation of RP-HPLC method for simultaneous estimation of montelukast sodium and fexofenadine hydrochloride in combined dosage form. J Pharm Res. 2013. https://doi.org/10.1016/j.jopr.2012.11.028.
Lee I-C, He J-S, Tsai M-T, Lin K-C. Fabrication of a novel partially dissolving polymer microneedle patch for transdermal drug delivery. J Mater Chem B. 2015. https://doi.org/10.1039/C4TB01555J.
Kim S, Eum J, Yang H, Jung H. Transdermal finasteride delivery via powder-carrying microneedles with a diffusion enhancer to treat androgenetic alopecia. J Control Release. 2019. https://doi.org/10.1016/j.jconrel.2019.11.002.
Park J-H, Choi S-O, Kamath R, Yoon Y-K, Allen MG, Prausnitz MR. Polymer particle-based micromolding to fabricate novel microstructures. Biomed Microdevices. 2007. https://doi.org/10.1007/s10544-006-9024-4.
De Santis F, Pantani R. Optical properties of polypropylene upon recycling. Sci World J. 2013. https://doi.org/10.1155/2013/354093.
Chu LY, Prausnitz MR. Separable arrowhead microneedles. J Control Release. 2011. https://doi.org/10.1016/j.jconrel.2010.10.033.
Li W, Tang J, Terry RN, Li S, Brunie A, Callahan RL, et al. Long-acting reversible contraception by effervescent microneedle patch. Sci Adv. 2019. https://doi.org/10.1126/sciadv.aaw8145.
Li W, Terry RN, Tang J, Feng MR, Schwendeman SP, Prausnitz MR. Rapidly separable microneedle patch for the sustained release of a contraceptive. Nat Biomed Eng. 2019. https://doi.org/10.1038/s41551-018-0337-4.
Moga KA, Bickford LR, Geil RD, Dunn SS, Pandya AA, Wang Y, et al. Rapidly-dissolvable microneedle patches via a highly scalable and reproducible soft lithography approach. Adv Mater. 2013. https://doi.org/10.1002/adma.201300526.
Taylor LS, Langkilde FW, Zografi G. Fourier transform Raman spectroscopic study of the interaction of water vapor with amorphous polymers. J Pharm Sci. 2001. https://doi.org/10.1002/jps.1041.
Larrañeta E, Moore J, Vicente-Pérez EM, González-Vázquez P, Lutton R, Woolfson AD, et al. A proposed model membrane and test method for microneedle insertion studies. Int J Pharm. 2014. https://doi.org/10.1016/j.ijpharm.2014.05.042.
Larrañeta E, Stewart S, Fallows SJ, Birkhäuer LL, McCrudden MTC, Woolfson AD, et al. A facile system to evaluate in vitro drug release from dissolving microneedle arrays. Int J Pharm. 2016. https://doi.org/10.1016/j.ijpharm.2015.11.038.
Acknowledgements
We thank Dr. Richard Terry for technical advice related to hydrogels and Donna Bondy for administrative support.
Funding
This work was supported by The Scientific and Technological Research Council of Turkey-TÜBİTAK (2214-A—International Research Fellowship Programme for PhD Students).
Author information
Authors and Affiliations
Contributions
Erkan Azizoglu: conceptualization, methodology, validation, investigation, formal analysis, data curation, writing—original draft, visualization, funding acquisition. Ozgen Ozer: conceptualization, supervision. Mark R. Prausnitz: conceptualization, methodology, resources, writing—review and editing, supervision, project administration.
Corresponding author
Ethics declarations
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Conflict of interest
Mark R Prausnitz is an inventor of microneedle patents, is a paid advisor, and is a founder/shareholder of companies developing microneedle-based products (Micron Biomedical). This potential conflict of interest has been disclosed and is managed by Georgia Tech.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Azizoglu, E., Ozer, O. & Prausnitz, M.R. Fabrication of pure-drug microneedles for delivery of montelukast sodium. Drug Deliv. and Transl. Res. 12, 444–458 (2022). https://doi.org/10.1007/s13346-021-01047-9
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-021-01047-9