Abstract
Inhalation route of drug delivery is the most favorable for pulmonary infections wherein direct drug delivery is desired to the lungs. Tuberculosis is one such infection suffering from poor therapeutic efficacy because of low patient compliance due to high drug dosing and lengthy treatment protocols. The current research work was undertaken to develop a dry powder inhaler (DPI) for administration of three first-line antitubercular antibiotics directly to the lungs to improve the treatment rates. Nanoformulations of isoniazid, pyrazinamide, and rifampicin were prepared, spray-dried to obtain a dry powder system, and blended with inhalation grade lactose to develop the DPI. The DPI was evaluated for its flow properties, pulmonary deposition, dissolution profile, and stability. The DPI possessed excellent flow properties with a fine particle fraction of 45% and a mass median aerodynamic diameter of approximately 5 µm indicating satisfactory lung deposition. In vitro drug release exhibited a sustained release of the formulations. In vivo studies showed a prolonged deposition in the lung at elevated concentrations compared to oral therapy. Stability studies proved that the formulation remained stable at accelerated and long-term stability conditions. The DPI could complement the existing oral therapy in enhancing the therapeutic efficacy in patients.
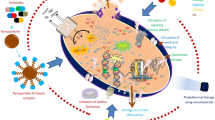
Graphical abstract






Similar content being viewed by others
References
Traini D, Young PM. Delivery of antibiotics to the respiratory tract: an update. Expert Opin Drug Deliv. 2009;6:897–905.
Zhou QT, Leung SSY, Tang P, et al. Inhaled formulations and pulmonary drug delivery systems for respiratory infections. Adv Drug Deliv Rev. 2015;85:83–99.
LaVan DA, McGuire T, Langer R. Small-scale systems for in vivo drug delivery. Nat Biotechnol. 2003;21:1184–91.
Hirota K, Hasegawa T, Nakajima T, et al. Delivery of rifampicin-PLGA microspheres into alveolar macrophages is promising for treatment of tuberculosis. J Control Release. 2010;142:339–46.
Chan JGY, Chan HK, Prestidge CA, et al. A novel dry powder inhalable formulation incorporating three first-line anti-tubercular antibiotics. Eur J Pharm Biopharm. 2013;83:285–92.
Blasi P, Schoubben A, Giovagnoli S, et al. Fighting tuberculosis: old drugs, new formulations. Expert Opin Drug Deliv. 2009;6:977–93.
Bihari Yadav A, Sharma R, Muttil P, et al. Inhalable microparticles containing isoniazid and rifabutin target macrophages and “stimulate the phagocyte” to achieve high efficacy †. Indian J Exp Biol. 2009;47:469–74.
Misra A, Hickey AJ, Rossi C, et al. Inhaled drug therapy for treatment of tuberculosis. Tuberculosis. 2011;91:71–81.
Sharma R, Muttil P, Yadav AB, et al. Uptake of inhalable microparticles affects defence responses of macrophages infected with Mycobacterium tuberculosis H37Ra. J Antimicrob Chemother. 2007;59:499–506.
Momin MAM, Tucker IG, Das SC. High dose dry powder inhalers to overcome the challenges of tuberculosis treatment. Int J Pharm. 2018;550:398–417.
Rifater Tablets - Summary of Product Characteristics (SmPC) - emc. 2019. https://www.medicines.org.uk/emc/product/1596/smpc. Accessed 27 May 2020.
Pourshahab PS, Gilani K, Moazeni E, et al. Preparation and characterization of spray dried inhalable powders containing chitosan nanoparticles for pulmonary delivery of isoniazid. J Microencapsul. 2011;28(7):605–13.
Nakarani M, Misra A, Patel J, Vaghani S. Itraconazole nanosuspension for oral delivery: formulation, characterization and in vitro comparison with marketed formulation. DARU J Pharm Sci. 2010;18(2):8490.
Thorat S, Meshram S. Formulation and product development of pressurised metered dose inhaler: an overview. PharmaTutor. 2015;3:53–64.
Muttil P, Kaur J, Kumar K, et al. Inhalable microparticles containing large payload of anti-tuberculosis drugs. Eur J Pharm Sci. 2007;32:351.
Muttil P, Wang C, Hickey AJ. Inhaled drug delivery for tuberculosis therapy. Pharm Res. 2009;26:2401–16.
Pai RV, Jain RR, Bannalikar AS, Menon MD. Development and evaluation of chitosan microparticles based dry powder inhalation formulations of rifampicin and rifabutin. J Aerosol Med Pulm Drug Deliv. 2016;29(2):179–95. https://doi.org/10.1089/jamp.2014.1187.
Bernkop-Schnürch A, Dünnhaupt S. Chitosan-based drug delivery systems. Eur J Pharm Biopharm. 2012;81(3):463–9. https://doi.org/10.1016/j.ejpb.2012.04.007.
Müller R, Junghanns. Nanocrystal technology, drug delivery and clinical applications. Int J Nanomedicine. 2008;3:295.
Chogale MM, Gaikwad SS, Kulkarni SP, Patravale VB. Quality-by-design enabled chitosan nanoparticles for antitubercular therapy: formulation, statistical optimization, and in vitro characterization. Current Drug Therapy. 2021;16(1):64–82.
Chogale MM, Gite SM, Patravale VB. Comparison of media milling and microfluidization methods for engineering of nanocrystals: a case study. Drug Dev Ind Pharm. 2020;46(11):1763–75.
Cook RO, Pannu RK, Kellaway IW. Novel sustained release microspheres for pulmonary drug delivery. J Control Release. 2005;104:79–90.
Rabbani NR, Seville PC. The influence of formulation components on the aerosolisation properties of spraydried powders. J Control Release. 2005;110:130–40.
Saint-Lorant G, Leterme P, Gayot A, Flament MP. Influence of carrier on the performance of dry powder inhalers. Int J Pharm. 2007;334:85–91.
Yu H, Teo J, Chew JW. Hadinoto K (2016) Dry powder inhaler formulation of high-payload antibiotic nanoparticle complex intended for bronchiectasis therapy: spray drying versus spray freeze drying preparation. Int J Pharm. 2016;499(1–2):38–46. https://doi.org/10.1016/j.ijpharm.2015.12.072.
Zeng XM, Martin GP, Marriott C. Particulate Interactions in Dry Powder Formulation for Inhalation. CRC Press. 2000.
De Boer AH, Hagedoorn P, Gjaltema D, et al. Air classifier technology (ACT) in dry powder inhalation Part 2. The effect of lactose carrier surface properties on the drug-to-carrier interaction in adhesive mixtures for inhalation. Int J Pharm. 2003;260:201–216.
Iida K, Hayakawa Y, Okamoto H, et al. Effect of surface layering time of lactose carrier particles on dry powder inhalation properties of salbutamol sulfate. Chem Pharm Bull. 2004;52:350–3.
Hamishehkar H, Emami J, Najafabadi AR, et al. Pharmacokinetics and pharmacodynamics of controlled release insulin loaded PLGA microcapsules using dry powder inhaler in diabetic rats. Biopharm Drug Dispos. 2010;31:189–201.
Islam N, Stewart P, Larson I, Hartley P. Lactose surface modification by decantation: are drug-fine lactose ratios the key to better dispersion of salmeterol xinafoate from lactose-interactive mixtures? Pharm Res. 2004;21:492–9.
Adi H, Larson I, Stewart PJ. Adhesion and redistribution of salmeterol xinafoate particles in sugar-based mixtures for inhalation. Int J Pharm. 2007;337:229–38.
Zeng XM, Martin GP, Tee SK, Marriott C. The role of fine particle lactose on the dispersion and deaggregation of salbutamol sulphate in an air stream in vitro. Int J Pharm. 1998;176:99–110.
Joshi M, Misra A. Dry powder inhalation of liposomal Ketotifen fumarate: formulation and characterization. Int J Pharm. 2001;223:15–27.
Zeng XM, Martin GP, Marriott C, Pritchard J. Lactose as a carrier in dry powder formulations: the influence of surface characteristics on drug delivery. J Pharm Sci. 2001;90:1424–1434.
Ali M. Pulmonary drug delivery. In: Handbook of non-invasive drug delivery systems. Elsevier, 2010:209–246.
Dunbar C. Analysis of cascade impactor mass distributions. 2014. https://doi.org/10.1089/jam.2005.18.439. Accessed 05 July 2020.
Sheth P, Stein SW, Myrdal PB. Factors influencing aerodynamic particle size distribution of suspension pressurized metered dose inhalers. AAPS PharmSciTech. 2014;16:192–201.
Bhutani H, Mariappan T, Singh S. The physical and chemical stability of anti-tuberculosis fixed-dose combination products under accelerated climatic conditions. Int J Tuberc Lung Dis. 2004;8:1073–80.
Baniasadi S, Shahsavari N, Namdar R, Kobarfard F. Stability assessment of isoniazid and rifampin liquid dosage forms in a national referral center for tuberculosis. Int J Pharm Sci Res. 2015;6:706–9.
Santoveña-Estévez A, Suárez-González J, Cáceres-Pérez AR, et al. Stability study of isoniazid and rifampicin oral solutions using hydroxypropyl-Β-cyclodextrin to treat tuberculosis in paediatrics. Pharmaceutics. 2020;12(2):195. https://doi.org/10.3390/pharmaceutics12020195.
Acknowledgements
The authors would like to thank Lupin Ltd. (Aurangabad, India) for the gift samples of Isoniazid, Pyrazinamide, and Rifampicin; Capsugel (Mumbai, India) for the gift sample of inhalation grade size 3 capsules; and DFE Pharma (Goch, Germany) for the gift sample of inhalation grade lactose.
Funding
This study was funded by University Grants Commission-Basic Science Research (UGC BSR).
Author information
Authors and Affiliations
Contributions
Conceptualization: Manasi Chogale, Sagar Dhoble, Vandana Patravale; methodology: Manasi Chogale, Sagar Dhoble, Vandana Patravale; formal analysis and investigation: Manasi Chogale, Sagar Dhoble, Vandana Patravale; writing: Manasi Chogale; original draft preparation: Manasi Chogale; writing: review and editing: Manasi Chogale, Vandana Patravale; supervision: Vandana Patravale.
Corresponding author
Ethics declarations
Ethics approval
The in vivo lung deposition study was performed as per the procedures and guidelines of the Committee for the Purpose of Control and Supervision of Experimental Animals (CPCSEA), India, at the Institute of Chemical Technology, Mumbai, India. The experiments were performed on receiving approval of the animal study protocol submitted to the Institutional Animal Ethics Committee (IAEC) of the Institute of Chemical Technology (Protocol no. IAEC/ICT/2017/P56: To study the biodistribution of developed novel nanoformulation for tuberculosis via pulmonary route).
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chogale, M.M., Dhoble, S.B. & Patravale, V.B. A triple combination 'nano' dry powder inhaler for tuberculosis: in vitro and in vivo pulmonary characterization. Drug Deliv. and Transl. Res. 11, 1520–1531 (2021). https://doi.org/10.1007/s13346-021-01005-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13346-021-01005-5