Abstract
Justification
Management practices of functional constipation are far from satisfactory in developing countries like India; available guidelines do not comprehensively address the problems pertinent to our country.
Process
A questionnaire-based survey was conducted among selected practising pediatricians and pediatric gastroenterologists in India, and the respondents agreed on the need for an Indian guideline on the topic. A group of experts were invited to present the published literature under 12 different headings, and a consensus was developed to formulate the practice guidelines, keeping in view the needs in Indian children.
Objective
To formulate practice guidelines for the management of childhood functional constipation that are relevant to Indian children.
Recommendations
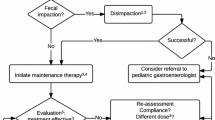
Functional constipation should be diagnosed only in the absence of red flags on history and examination. Those with impaction and/or retentive incontinence should be disimpacted with polyethylene glycol (hospital or home-based). Osmotic laxatives (polyethylene glycol more than 1 year of age and lactulose/lactitol less than 1 year of age) are the first line of maintenance therapy. Stimulant laxatives should be reserved only for rescue therapy. Combination therapies of two osmotics, two stimulants or two classes of laxatives are not recommended. Laxatives as maintenance therapy should be given for a prolonged period and should be tapered off gradually, only after a successful outcome. Essential components of therapy for a successful outcome include counselling, dietary changes, toilet-training and regular follow-up.
Similar content being viewed by others
References
Yadav M, Singh PK, Mittal SK. Variation in bowel habits of healthy Indian children aged up to two years. Indian J Pediatr. 2014;81:446–9.
Sujatha B, Velayutham DR, Deivamani N, Bavanandam S. Normal bowel pattern in children and dietary and other precipitating factors in functional constipation. J Clin Diag Res. 2015;9:SC12–5.
Hyman PE, Milla PJ, Benninga MA, Davidson GP, Fleisher DF, Taminiau J. Childhood functional gastrointestinal disorders: neonate/toddler. Gastroenterology. 2006;130:1519–26.
Rasquin A, Di Lorenzo C, Forbes D, Guiraldes E, Hyams JS, Staiano A, et al. Childhood functional gastrointestinal disorders: child/adolescent. Gastroenterology. 2006;130:1527–37.
Tabbers MM, DiLorenzo C, Berger MY, Faure C, Langen-dam MW, Nurko S, et al. Evaluation and Treatment of Functional Constipation in Infants and Children: Evidence-Based Recommendations From ESPGHAN and NASPGHAN. J Pediatr Gastroenterol Nutr. 2014;58:258–74.
Loening-Baucke V. Urinary incontinence and urinary tract infection and their resolution with treatment of chronic constipation of childhood. Pediatrics. 1997;100:228–32.
Burgers R, de Jong TP, Visser M, Di Lorenzo C, Dijkgraaf MG, Benninga MA. Functional defecation disorders in children with lower urinary tract symptoms. J Urol. 2013;189:1886–91.
Borowitz SM, Cox DJ, Tam A, Ritterband LM, Sutphen JL, Penberthy JK. Precipitants of constipation during early childhood. J Am Board Fam Pract. 2003;16:213–8.
Bardisa-Ezcurra L, Ullman R, Gordon J. Guideline Development Group. Diagnosis and Management of Idiopathic Childhood Constipation: Summary of NICE Guidance. BMJ. 2010;340:c2585.
Gold DM, Levine J, Weinstein TA, Kessler BH, Pettei MJ. Frequency of digital rectal examination in children with chronic constipation. Arch Pediatr Adolesc Med. 1999;153:377–9.
Rockney RM, McQuade WH, Days AL. The plain abdominal roentgenogram in the management of encopresis. Arch Pediatr Adolesc Med. 1995;149:623–7.
Pashankar D. Childhood constipation: evaluation and management. Clin Colon Rectal Surg. 2005;18:120–7.
Chogle A, Saps M. Yield and cost of performing screening tests for constipation in children. Can J Gastroenterol. 2013;27:e35–8.
Khanna V, Poddar U, Yachha SK. Etiology and clinical spectrum of constipation in Indian children. Indian Pediatr. 2010;47:1025–30.
Bekkali NLH, van den Berg MM, Dijkgraaf MG, van Wijk MP, Bongers ME, Liem O, et al. Rectal fecal impaction treatment in childhood constipation: enemas versus high doses oral PEG. Pediatrics. 2009;124:e1108–15.
Chen SL, Cai SR, Deng L, Zhang XH, Luo TD, Peng JJ, et al. Efficacy and complications of polyethylene glycols for treatment of constipation in children: A meta-analysis. Medicine (Baltimore). 2014;93:e65.
Guest JF, Candy DC, Clegg JP, Edwards D, Helter MT, Dale AK, et al. Clinical and economic impact of using macrogol 3350 plus electrolytes in an outpatient setting compared to enemas and suppositories and manual evacuation to treat paediatric faecal impaction based on actual clinical practice in England and Wales. Curr Med Res Opin. 2007;23:2213–25.
Gordon M, Naidoo K, Akobeng AK, Thomas AG. Osmotic and stimulant laxatives for the management of childhood constipation. Cochrane Database Syst Rev. 2012:11;7:CD009118.
Loening-Baucke V. Prevalence, symptoms and outcome of constipation in infants and toddlers. J Pediatr. 2005;146:359–63.
Pijpers MA, Bongers ME, Benninga MA, Berger MY. Functional constipation in children: A systematic review on prognosis and predictive factors. J Pediatr Gastroenterol Nutr. 2010;50:256–68.
Bongers ME, van Wijk MP, Reitsma JB, Benninga MA. Long-term prognosis for childhood constipation: clinical outcomes in adulthood. Pediatrics. 2010;126: e156–62.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Yachha, S.K., Srivastava, A., Mohan, N. et al. Management of Childhood Functional Constipation: Consensus Practice Guidelines of Indian Society of Pediatric Gastroenterology, Hepatology and Nutrition and Pediatric Gastroenterology Chapter of Indian Academy of Pediatrics. Indian Pediatr 55, 885–892 (2018). https://doi.org/10.1007/s13312-018-1402-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13312-018-1402-5