Abstract
Background
New onset seizures in pregnancy and postpartum are considered eclampsia as the default diagnosis. Other causes, such as intracranial haemorrhage, subarachnoid haemorrhage, cerebral venous sinus thrombosis or acute ischaemic stroke, have a similar mode of presentation, but need prompt diagnosis and institution of specific measures to decrease the risk of mortality and morbidity. Neuroimaging plays an important role in providing a specific diagnosis and hence aids in proper management. We hypothesised to find any correlation of laboratory parameters with neuroimaging abnormalities along with providing an insight to specific diagnoses in patients of new onset seizures in pregnancy with a presumptive diagnosis of eclampsia.
Methods
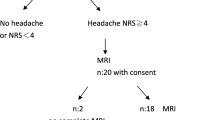
This was a hospital-based descriptive observational study conducted in SCB Medical College, Odisha, in the year 2018–2020 with a total of 70 clinically confirmed cases of eclampsia. They were subjected to cranial MR imaging along with routine investigations with no change in the emergency treatment protocol followed in the department. Data was compiled using Microsoft Excel 2016 and IBM SPSS statistics for Windows, version 27, and comparisons among MRI normal and abnormal group were stated.
Results
58 (82.86%) were MR imaging positive or abnormal, while 12 (17.14%) were MR imaging negative or normal. Cortical venous thrombosis without infarction was diagnosed in 25 (43.1%) patients, 6 (10.34%) had infarction, posterior reversible encephalopathy syndrome was seen in 19 (32.76%) cases, and 8 (13.79%) had hypertensive leukoencephalopathy. The mean gestational age at the time of presentation was significantly lower in the MRI abnormal group (p = 0.012). The AST and LDH values were found to be significantly higher in the MRI abnormal group, with p = 0.02 and 0.01, respectively.
Conclusion
Patients with imaging abnormalities have a severe form of disease in eclampsia. Neuroimaging in provisionally diagnosed cases of eclampsia will modify the management and hence prognosis in these patients.



Similar content being viewed by others
References
Sajith M, Nimbargi V, Modi A, Sumariya R, Pawar A. Incidence of pregnancy induced hypertension and prescription pattern of antihypertensive drugs in pregnancy. Int J Pharma Sci Res. 2014;23:4.
Khan KS, Wojdyla D, Say L, Gülmezoglu AM, Van Look PF. WHO analysis of causes of maternal death: a systematic review. Lancet. 2006;367(9516):1066–74.
Gestational Hypertension and Preeclampsia. ACOG practice bulletin, number 222. Obstet Gynecol. 2020;135(6):e237–60. https://doi.org/10.1097/AOG.0000000000003891. (PMID: 32443079).
Edlow JA, Caplan LR, O’Brien K, Tibbles CD. Diagnosis of acute neurological emergencies in pregnant and post-partum women. Lancet Neurol. 2013;12(2):175–85.
Patil MM. Study of neuroimaging in patients with refractory eclampsia. J South Asian Federation Obstet Gynaecol. 2013;5(1):4–7.
Shah AK, Rajamani K, Whitty JE. Eclampsia: a neurological perspective. J Neurol Sci. 2008;271(1–2):158–67.
Aya AG, Ondze B, Ripart J, Cuvillon P. Seizures in the peripartum period: epidemiology, diagnosis and management. Anaesth Crit Care Pain Med. 2016;1(35):S13-21.
Schwartz RB, Feske SK, Polak JF, DeGirolami U, Iaia A, Beckner KM, Bravo SM, Klufas RA, Chai RY, Repke JT. Preeclampsia-eclampsia: clinical and neuroradiographic correlates and insights into the pathogenesis of hypertensive encephalopathy. Radiology. 2000;217(2):371–6.
Demirtas Ö, Gelal F, Vidinli BD, Demirtas LO, Uluç E, Baloglu A. Cranial MR imaging with clinical correlation in preeclampsia and eclampsia. Diagn Interv Radiol. 2005;11(4):189.
Gao B, Liu FL, Zhao B. Association of degree and type of edema in posterior reversible encephalopathy syndrome with serum lactate dehydrogenase level: initial experience. Eur J Radiol. 2012;81(10):2844–7.
American College of Obstetricians and Gynecologists. ACOG practice bulletin no. 202: gestational hypertension and preeclampsia. Obstet Gynecol. 2019;133(1):e1-25.
Strandgaard S, Sengupta D, Mackenzie ET, Rowan JO, Olesen J, Skinhøj E, Lassen NA, Harper AM. The lower and upper limits for autoregulation of cerebral blood flow. Cerebral circulation and metabolism. 1975 (3–6)
Benedetti TJ, Quilligan EJ. Cerebral edema in severe pregnancy-induced hypertension. Am J Obstet Gynecol. 1980;137(7):860–2.
Will AD, Lewis KL, Hinshaw D, Jordan K, Cousins L, Hasso A, Thompson J. Cerebral vasoconstriction in toxemia. Neurology. 1987;37(9):1555–7.
Qureshi AI, Frankel MR, Ottenlips JR, Stern BJ. Cerebral hemodynamics in preeclampsia and eclampsia. Arch Neurol. 1996;53(12):1226–31.
Gant NF, Daley GL, Chand S, Whalley PJ, MacDonald PC. A study of angiotensin II pressor response throughout primigravid pregnancy. J Clin Investig. 1973;52(11):2682–9.
Chakravarty A, Chakrabarti SD. The neurology of eclampsia: some observations. Neurol India. 2002;50(2):128.
Chandra I, Sun L. Preterm and term preeclampsia: differences in biochemical parameter and pregnancy outcomes. Postgrad Med. 2018;130(8):703–7.
Bojja V, Keepanasseril A, Nair PP, Sunitha VC. Clinical and imaging profile of patients with new-onset seizures & a presumptive diagnosis of eclampsia–a prospective observational study. Pregnancy Hypertens. 2018;1(12):35–9.
Sharma G, Joshi G, Purohit RC. Cranial MR imaging in eclampsia and severe preeclampsia: a prospective study. J Evol Med Dent Sci. 2014;3(13):3250–60.
Dogra R, Thakur R, Thakur V, Pal A, Chamotra S, Chaudhary A. Neuro-imaging in severe hypertensive disorders of pregnancy: a study from North Indian tertiary health care institution. Int J Reprod Contracept Obstet Gynecol. 2020;9(6):2347.
Kokila MS, Dwivedi AD. Correlation of clinical and neuroimaging findings affecting management in postpartum eclampsia: a prospective study. J South Asian Federation Obstet Gynaecol. 2013;3(3):125–30.
Harandou M, Madani N, Labibe S, Messouak O, Boujraf S, Benkirane S, Houssni B, Maaroufi M, Lemhadri M, Tizniti S, Belahsen F. Neuroimaging findings in eclamptic patients still symptomatic after 24 hours: a descriptive study about 19 cases. Ann Francaises D’anesthesie et de Reanim. 2006;25(6):577–83.
Acknowledgements
The authors are immensely grateful to Dr. Pallabi Thakur, Junior Resident, Dept. of Obstetrics and Gynaecology for her help in the collection of data.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in the study were in accordance with ethical standards of the institutional and/or national research committee. (Application No.-227/26.08.20).
Informed Consent of Publication
Informed consent was obtained from all participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The study is conducted in the department of O&G and department of Radiology, S.C.B.Medical College, Cuttack.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mohapatra, K., Sultana, N.N., Behuria, S. et al. Neuroimaging Features in Eclamptic Encephalopathy and their Correlation with Clinical and Laboratory Parameters: a Prospective Observational Study. J Obstet Gynecol India (2024). https://doi.org/10.1007/s13224-023-01899-w
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s13224-023-01899-w