Abstract
Introduction
Despite their relative frequency, paraovarian cyst received only scant attention. Clinician should be aware of the complications of paraovarian cyst.
Objective
To analyse the clinical profile, complications and management of paraovarian cyst.
Materials and Methods
Retrospective analysis of 51 patients with operative diagnosis of paraovarian cyst was carried out at our institution over a 5-year period.
Results
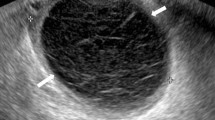
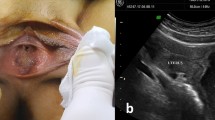
Majority (60.78%) of paraovarian cysts were found in the third and fourth decades, and the mean age of the patients was 31.8 years. 62.74% patients with paraovarian cyst presented with abdominal pain, and the rest were an incidental finding. Ultrasound made a correct diagnosis in 47.05% of patients. Mean size of paraovarian cyst was 7.51 cm. Complications of paraovarian cyst noted in our study are cyst enlargement (79.62%), adnexal torsion (18.51%), haemorrhage (7.4%), rupture (1.85%) and benign tumour (12.96%). 84.31% paraovarian cysts were managed by laparoscopy. Fertility-sparing surgery was done in 57.39% of paraovarian cysts.
Conclusion
Paraovarian cyst should be considered in the differential diagnosis of adnexal mass. The importance of differentiating it from ovarian cyst cannot be overemphasized. Laparoscopic approach and preferably a fertility-sparing surgery should be considered in the management of complications of paraovarian cyst.
Similar content being viewed by others
References
Kiseli M, Caglar GS, Cengiz SD, et al. Clinical diagnosis and complications of paratubal cysts: review of the literature and report of uncommon presentations. Arch Gynecol Obstet. 2012;285(6):1563–9.
Gupta A, Gupta P, Manaktala U, et al. Clinical, radiological and histopathological analysis of paraovarian cysts. J Midlife Health. 2016;7(2):78–82.
Bosnalı O, Moralıoğlu S, Cerrah-Celayir A. Occurrence of paratubal cysts in childhood: an analysis of 26 cases. Turk J Pediatr. 2016;58(3):266–70.
Muolokwu E, Sanchez J, Bercaw JL, et al. Paratubal cysts, obesity, and hyperandrogenism. J Pediatr Surg. 2011;46(11):2164–7.
Dietrich JE, Adeyemi O, Hakim J, et al. Paratubal cyst size correlates with obesity and dysregulation of the Wnt signaling pathway. J Pediatr Adolesc Gynecol. 2017;30(5):571–7.
Sokalska A, Timmerman D, Testa AC, et al. Diagnostic accuracy of transvaginal ultrasound examination for assigning a specific diagnosis to adnexal masses. Ultrasound Obstet Gynecol. 2009;34(4):462–70.
Valsky DV, Esh-Broder E, Cohen SM, et al. Added value of the gray-scale whirlpool sign in the diagnosis of adnexal torsion. Ultrasound Obstet Gynecol. 2010;36(5):630–4.
Sasaki KJ, Miller CE. Adnexal torsion: review of the literature. J Minim Invasive Gynecol. 2014;21(2):196–202.
De Sanctis V, Soliman AT, Elsedfy H, et al. An adolescent with an asymptomatic adnexal cyst: to worry or not to worry? Medical versus surgical management options. Acta Biomed. 2017;88(2):232–6.
Muolokwu E, Sanchez J, Bercaw JL, et al. The incidence and surgical management of paratubal cysts in a pediatric and adolescent population. J Pediatr Surg. 2011;46(11):2161–3.
Agarwal P, Agarwal P, Bagdi R, et al. Ovarian preservation in children for adenexal pathology, current trends in laparoscopic management and our experience. J Indian Assoc Pediatr Surg. 2014;19(2):65–9.
Smorgick N, Herman A, Schneider D, et al. Paraovarian cysts of neoplastic origin are underreported. JSLS. 2009;13(1):22–6.
Ryu KJ, Kim IS, Bae HS, et al. Paratubal cancer found at the time of laparoscopic surgery for adnexal torsion: a case report and literature review. Eur J Gynaecol Oncol. 2014;35(6):741–4.
Lee S, Ahn KH, Park HT, et al. Paratubal borderline malignancy: a case of a 17-year-old adolescent female treated with laparo-endoscopic single-site surgery and a review of the literature. J Pediatr Adolesc Gynecol. 2016;29(1):74–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Statement
This study was approved by the institutional ethical committee. Since this study is a retrospective analysis, no ethical issues are involved.
Additional information
Dr. Anitha Durairaj is an Assistant professor in the Department of Obstetrics and Gynaecology at Velammal Medical College Hospital and Research Institute, Madurai. She completed her MD in OBG in 2011 from the Institute of Obstetrics and Gynaecology, Madras Medical College, Chennai. She has special interest in teaching, endoscopic surgeries and high-risk obstetrics.
Rights and permissions
About this article
Cite this article
Durairaj, A., Gandhiraman, K. Complications and Management of Paraovarian Cyst: A Retrospective Analysis. J Obstet Gynecol India 69, 180–184 (2019). https://doi.org/10.1007/s13224-018-1152-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13224-018-1152-2