Abstract
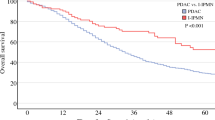
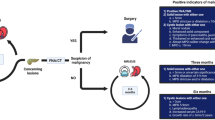
Insulinoma is a rare pancreatic neuroendocrine tumor with an incidence of 1–4 cases per million. Here we present our 10 years of experience in 13 cases of insulinoma. We retrospectively reviewed all insulinoma patients diagnosed and treated between 2012 and 2022. Clinical and pathological features, diagnostic methods, and follow-up results of insulinoma patients were discussed. A total of 13 patients were included in this study (7 men, and 6 women). The mean age at the time of diagnosis was 58 (36.5–70.5) years. There is only one patient diagnosed with MEN-1 syndrome. The mean time from the onset of symptoms to the diagnosis was 15 (7–27.5) months. In the prolonged fasting test, symptomatic hypoglycemia occurred in all patients within 48 h. The median size of lesions was 15 (12–24) mm, and 46.2% of these lesions were isolated in the pancreatic tail. Ga-68 DOTATATE PET/CT detected lesions with 100% accuracy. Three patients met the criteria for malignant insulinoma. Octreotide LAR was given to 1 patient with metastatic disease and 1 patient who did not accept surgery. The metastatic patient received 8 cycles of Lu treatment and died after 51 months of follow-up. The diagnosis of insulinoma can be challenging. The 48-h fasting test period provided sufficient information for the diagnosis of insulinoma. Ga-68 DOTATATE PET/CT may be an alternative in cases where cross-sectional imaging cannot localize the pancreatic lesion.


Similar content being viewed by others
Data Availability
The datasets used are available from the corresponding author upon reasonable request.
References
Service FJ, Mcmahon MM, Obrien PC, Ballard DJ (1991) Functioning Insulinoma—incidence, recurrence, and long-term survival of patients: a 60-year study. Mayo Clin Proc 66:711–719. https://doi.org/10.1016/S0025-6196(12)62083-7
Sotoudehmanesh R, Hedayat A, Shirazian N et al (2007) Endoscopic ultrasonography (EUS) in the localization of insulinoma. Endocrine 31:238–241. https://doi.org/10.1007/S12020-007-0045-4/FIGURES/3
Baudin E, Caron P, Lombard-Bohas C et al (2013) Malignant insulinoma: Recommendations for characterisation and treatment Insulinome malin : caractérisation et traitement ♦. Ann Endocrinol (Paris) 74:523–533. https://doi.org/10.1016/j.ando.2013.05.009
Iglesias P, Díez JJ (2014) MANAGEMENT OF ENDOCRINE DISEASE: A clinical update on tumor-induced hypoglycemia. Eur J Endocrinol 170:R147–R157. https://doi.org/10.1530/EJE-13-1012
Okabayashi T, Shima Y, Sumiyoshi T et al (2013) Diagnosis and management of insulinoma. World J Gastroenterol 19:829–837. https://doi.org/10.3748/wjg.v19.i6.829
Aydemir E, Ateş C, Saridaş FM et al (2022) Evaluation of insulinoma cases presented with hyperinsulinemic hypoglycemia: a single-centre experience. Turkish J Intern Med 4:23–28. https://doi.org/10.46310/TJIM.1073351
Peltola E, Hannula P, Huhtala H et al (2018) Characteristics and outcomes of 79 patients with an Insulinoma: A nationwide retrospective study in Finland. Int J Endocrinol 2018:. https://doi.org/10.1155/2018/2059481
Yu J, Ping F, Zhang H et al (n.d.) Clinical management of malignant insulinoma: a single Institution’s experience over three decades. https://doi.org/10.1186/s12902-018-0321-8
Hasanov R, Samadov E, Bayramov N et al (2020) Surgical management of insulinomas at the Azerbaijan Medical University: a retrospective study of 21 cases over a 10-year period. Turkish J Med Sci 50:1262–1269. https://doi.org/10.3906/sag-2001-150
Shirzad N, Ahmadi P, Shahsiah R, Hemmatabadi M (2021) Insulinoma: spectrum of clinicopathological features in a tertiary center. Istanbul Med J 22:61–67. https://doi.org/10.4274/IMJ.GALENOS.2021.45202
Jyotsna VP, Pal S, Kandasamy D et al (2016) Evolving management of insulinoma: experience at a tertiary care centre. Indian J Med Res 144:771. https://doi.org/10.4103/IJMR.IJMR_1477_14
Anakal MG, Kalra P, Dharmalingam M et al (2014) Insulinoma case series: experience of a tertiary care center. Indian J Endocrinol Metab 18:858. https://doi.org/10.4103/2230-8210.141385
Niederle B, Selberherr A, Bartsch DK et al (2021) Multiple endocrine neoplasia type 1 and the pancreas: diagnosis and treatment of functioning and non-functioning pancreatic and duodenal neuroendocrine neoplasia within the MEN1 syndrome – an international consensus statement. Neuroendocrinology 111:609–630. https://doi.org/10.1159/000511791
Sada A, Yamashita TS, Glasgow AE et al (2021) Comparison of benign and malignant insulinoma. Am J Surg 221:437–447. https://doi.org/10.1016/J.AMJSURG.2020.08.003
Gopal RA, Acharya SV, Menon SK et al (2010) Clinical profile of insulinoma: Analysis from a tertiary care referral center in India. Indian J Gastroenterol 29:205–208. https://doi.org/10.1007/S12664-010-0051-Y/FIGURES/2
Sharma A, Varshney P, Kasliwal R et al (2022) Insulinoma—accurate preoperative localization is the key to management: an initial experience. Indian J Surg Oncol 13:403–411. https://doi.org/10.1007/S13193-022-01534-6/FIGURES/2
Paul TV, Jacob JJ, Vasan SK et al (2008) Management of insulinomas: Analysis from a tertiary care referral center in India. World J Surg 32:576–582. https://doi.org/10.1007/S00268-007-9390-Y/TABLES/3
Placzkowski KA, Vella A, Thompson GB et al (2009) Secular trends in the presentation and management of functioning Insulinoma at the Mayo Clinic, 1987–2007. J Clin Endocrinol Metab 94:1069–1073. https://doi.org/10.1210/JC.2008-2031
Grant CS (2005) Insulinoma. Best Pract Res Clin Gastroenterol 19:783–798. https://doi.org/10.1016/J.BPG.2005.05.008
Prasad V, Sainz-Esteban A, Arsenic R et al (2016) Role of (68)Ga somatostatin receptor PET/CT in the detection of endogenous hyperinsulinaemic focus: an explorative study. Eur J Nucl Med Mol Imaging 43:1593–1600. https://doi.org/10.1007/S00259-016-3331-7
Nockel P, Babic B, Millo C et al (2017) Localization of Insulinoma using 68Ga-DOTATATE PET/CT Scan. J Clin Endocrinol Metab 102:195. https://doi.org/10.1210/JC.2016-3445
Shah R, Sehemby M, Garg R et al (2022) 68Ga-DOTATATE PET/CT imaging in endogenous hyperinsulinemic hypoglycemia: A tertiary endocrine centre experience. Clin Endocrinol (Oxf) 96:190–199. https://doi.org/10.1111/CEN.14586
Partelli S, Bartsch DK, Capdevila J et al (2017) ENETS consensus guidelines for the standards of care in neuroendocrine tumours: surgery for small intestinal and pancreatic neuroendocrine tumours. Neuroendocrinology 105:255–265. https://doi.org/10.1159/000464292
Nikfarjam M, Warshaw AL, Axelrod L et al (2008) Improved contemporary surgical management of insulinomas: a 25-year experience at the Massachusetts General Hospital. Ann Surg 247:165–172. https://doi.org/10.1097/SLA.0B013E31815792ED
Zhao YP, Zhan HX, Zhang TP et al (2011) Surgical management of patients with insulinomas: result of 292 cases in a single institution. J Surg Oncol 103:169–174. https://doi.org/10.1002/JSO.21773
Mishra A, Neyaz Z, Yadav S et al (2022) Outcome of pre-operative vs intraoperative localization techniques in insulinoma: experience in a tertiary referral center. Indian J Surg: 1–6. https://doi.org/10.1007/S12262-022-03569-Z/FIGURES/2
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Consent for Publication
Not applicable.
Competing Interests
All co-authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Sözen, M., Cantürk, Z., Selek, A. et al. Clinicopathological Features of Insulinoma: A Single Tertiary Center Experience. Indian J Surg Oncol 14, 564–570 (2023). https://doi.org/10.1007/s13193-023-01774-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13193-023-01774-0