Abstract
Human cathelicidin refers to the cationic antimicrobial peptide hCAP18/LL-37. LL-37 is formed by cleavage of the propeptide hCAP18 coded by the CAMP gene. The active form of vitamin D, 1,25-dihydroxyvitamin D (1,25(OH)D), has been shown to induce the CAMP gene expression through promoter activation. We previously failed to demonstrate in a clinical trial that supplementation of 25-hydroxyvitamin D (25(OH)D) improves LL-37 serum levels. The aim of this work was to evaluate the impact of 25(OH)D supplementation on intracellular expression of CAMP and secretion of LL-37 in an ex vivo model using the peripheral blood mononuclear cells (PBMC). PBMC collected from healthy donors and incubated with different concentrations of 25(OH)D (0 ng/ml: control (D0); 25 ng/ml: deficient (D25); 75 ng/ml: physiological (D75); 125 ng/ml: supraphysiological (D125)) were stimulated or not with lipopolysaccharide (LPS, 100 ng/ml) or synthetic double-stranded RNA Poly (I: C) (PIC, 10 µg/ml). The intracellular expressions of the CAMP gene and the hCAP18 peptide were measured respectively after 24-h and 48-h incubation periods. The concentration of LL-37 was determined in the culture medium after 48-h incubation. 25(OH)D significantly induced CAMP gene expression at 24 h with a maximum effect at a dose of D125 in either unstimulated (tenfold expression) or stimulated (LPS: 100-fold expression; PIC: 15-fold expression) conditions. Intracellular hCAP18 peptide was overexpressed at 48 h under unstimulated (1.5-fold, D125) and stimulated conditions, LPS (twofold, D125) and PIC (2.5-fold, D125). The secretion of LL-37 in the culture medium was significantly induced by 25(OH)D only in both stimulated (LPS and PIC) conditions in a dose-dependent manner. Our results demonstrate that 25(OH)D incubation increases intracellular expression of CAMP and hCAP18, but extracellular secretion of LL-37 antimicrobial peptide is increased by 25(OH)D only when PBMC from healthy donors were stimulated with bacterial or viral immune mimetic.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
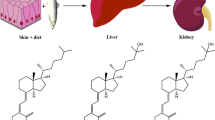
Cathelicidin is a generic name that can refer not only to the CAMP gene (cationic antimicrobial peptide), hCAP18 peptide (human cationic antimicrobial peptide 18 kDa), but also to LL-37 peptide (37 amino acid residues with diLeucine at the N-terminus, 4.5 kDa). hCAP18 peptide is coded by the CAMP gene whose expression is regulated by vitamin D. More precisely, the active form of vitamin D 1,25-dihydroxyvitamin D (1,25(OH)D) binds to the vitamin D nuclear receptor (VDR) [1], enabling dimerization with retinol X receptor (RXR). This complex enters the nucleus to bind to a consensus vitamin D response element (VDRE) in the CAMP gene promoter, thus enhancing hCAP18 expression [2]. hCAP18 is widely expressed especially in the monocyte/macrophage lineage in which it is stored in lysosomes or vacuoles [3]. Cleavage of the C-terminal end of hCAP18 by serine proteinase 3 in immune cells generates the active form of the cathelicidin, LL-37, and an inactive peptide, cathelin [4]. The two peptides, active form LL-37 and hCAP18, could be released, but LL-37 is considered as the major form present in the bloodstream. LL-37 plays a prominent role in innate host defense against bacteria and certain viruses, fungi, and parasites. The LL-37 microbicidal effect is principally due to its cationic properties allowing permeabilization of microorganism’s membrane [2]. Toll-like receptors (TLRs) 1, 2, and 4, induced by pathogen immune stimulators, were also reported to upregulate the expression of VDR and vitamin D hydroxylase genes, leading to the induction of cathelicidin production and eradication of intracellular Mycobacterium (M.) tuberculosis [1].
While a positive correlation between 25(OH)D supplementation and CAMP expression has been established [5], the link between circulating 25(OH)D and the hCAP18 and/or LL-37 blood peptides remains unclear both in healthy and diseased subjects. In volunteers presenting health issues, Kanda et al. (2012) have reported a positive correlation in atopic dermatitis patients as well as Lungu et al. (2021) in tuberculosis patients [6, 7] contrary to Meca et al. (2021) [8]. In healthy volunteers, Bhan et al. (2011) [9] and Dixon et al. (2012) [10] also reported a significant positive correlation but only when serum concentration of 25(OH)D was under the threshold value of 32 ng/ml. In contrast, Stukes et al. (2016) and Lungu et al. (2021) were unable to confirm the correlation between 25(OH)D and LL-37 circulating levels in a cohort of healthy volunteers [7, 11]. The meta-analysis performed by Acen et al. (2021) does not have sufficient eligible studies to perform a correlation meta-analysis of vitamin D and LL-37 levels [12]. Recent studies in vitamin D–supplemented volunteers failed to enhance cathelicidin plasmatic level [13, 14]; our team observed the same absence of effect in a placebo-controlled clinical trial with vitamin D supplementation in elderly volunteers [15]. Despite a strong improvement in serum 25(OH)D concentrations, we found no variation in LL-37 serum concentrations.
In view of these conflicting results, our objective was to clarify the ex vivo conversion process of hCAP18 to LL-37 in blood immune cells and to evaluate if 25(OH)D supplementation could enhance the LL-37 release to the extracellular compartment. Therefore, we established an ex vivo culture of freshly isolated peripheral blood mononuclear cells (PBMC) from healthy donors. The cells were incubated with several doses of 25(OH)D to assess intracellular CAMP gene expression, hCAP18 peptide expression, and LL-37-secreted concentrations in the culture medium. In addition to 25(OH)D, certain PBMCs were stimulated with bacterial or viral mimetics, respectively. Lipopolysaccharide (LPS) is known to induce CAMP overexpression via Toll-like receptor 4 (TLR4) induction [16], as well as polyinosinic cytidylic acid (PIC), a well-known activator of TLR3 [17]. Concomitantly, we explored the vitamin D’s metabolic actors: expression of CYP27B1 and CYP24A1 enzyme genes as well as VDR gene.
Materials and methods
Cell culture
The human blood samples were obtained from healthy volunteers of the local French blood agency (Etablissement Français du Sang, EFS, Auvergne-Rhône-Alpes). After full pertinent information, written informed consent was obtained from all blood donors involved in the study as statutory required (article R.1221–5 of the Public Health Code, 12/01/2009 and 11/06/2006 decrees). Ethical review and approval were not required for this study in accordance with the local legislation and institutional requirements.
PBMC were isolated from the buffy-coats by Ficoll-Histopaque (Sigma) density gradient centrifugation. After isolation, PBMC (106 cells/ml) were cultured for 24 h or 48 h in RPMI-1640 complete medium (37 °C, 5% CO2) with several doses of 25(OH)D (Sigma Aldrich, ref 739,650) (0 ng/ml: control (D0); 25 ng/ml: deficient (D25); 75 ng/ml: physiological (D75); 125 ng/ml: supraphysiological (D125)), stimulated or not by a bacterial agent (extract of Escherichia coli lipopolysaccharides 055B5 (LPS): 100 ng/ml) ref. L6529 (Sigma-Aldrich), or a viral mimetic agent (synthetic double-stranded RNA Poly (I: C) (PIC): 10 µg/ml) ref. P1038 (Sigma-Aldrich).
RT-qPCR
RT-qPCR was performed as described in [18] after 24 h of cell incubation. Quality of the RNA has been checked by the ratio 260:280 nm (comprised between 1.8 and 2) obtained from Nanodrop assay, and by agarose gel electrophoresis of RNA.
The cycle threshold (Ct) values in qPCR gave an overview of the gene expression variation in the samples. According to the variations of Ct values, 18S showed the smallest gene expression variation in our samples. Using NormFinder, 18S was the most stable tested housekeeping gene. The expression of CAMP (F-GCTAACCTCTACCGCCTCCT, R-GGTCACTGTCCCCATACACC), CYP27B1 (F-CGAGAAGGACCTGGAGTCTG, R-TCTGGGACACGAGAATTTCC), CYP24A1 (F-ATGAGCACGTTTGGGAGGAT, R-TGCCAGACCTTGGTGTTGAG), and VDR (F-CTGACCCTGGAGACTTTGA, R-TTCCTCTGCACTTCCTCATC) target genes was assessed using 18S mRNA (F-AGCTTATGACCCGCACTTAC, R-GTCTGTGATGCCCTTAGATG) as the housekeeping gene for normalization. The comparative Ct method (2−ΔΔCT) was used to calculate the relative gene expression of a given sample, normalized within the sample to the housekeeping gene, and relative to the expression of the same gene in another sample: 2−ΔΔCT method with ΔΔCT = [ΔCT (sample1) − ΔCT (sample2)] and ΔCT = [CT(target gene) − geometric mean CT (housekeeping gene)] as described in [19].
Western blotting
Western blots were performed as previously described [20] after 48 h of cell incubation. The membranes were exposed to primary antibodies (CAMP, Sigma Aldrich, ref. SAB5300171, dilution 1/1000; and GAPDH, Cell Signaling Technology #5174, dilution 1/2000). The relative expression was obtained by normalization with GAPDH expression levels.
ELISA
LL-37 was quantified in the PBMC culture media after 48 h of cell incubation using a double-sandwich ELISA, following the manufacturer’s guidelines (Hycult Biotechnology, ref: HK321). The HK321 LL-37 ELISA does not discriminate between LL-37 peptide and the full-length precleaved hCAP18 protein. The concentrations of LL-37 were normalized with protein content of culture media.
Statistical analysis
Data are presented as mean ± sem and were analyzed using GraphPad Prism5. Two-way ANOVA (dose: 25(OH)D and treatment: immune stimuli) with Bonferroni post hoc test was used to evaluate the 25(OH)D dose response in unstimulated and LPS- and PIC-stimulated conditions. Test result was considered significant when p < 0.05.
When working with relative expression data, the value of control condition (i.e., unstimulated D0 condition) was set to “1,” and other values were normalized accordingly to facilitate interpretation.
Results
PBMC express CYP27B1, CYP24A1, and VDR.
To accomplish 25(OH)D metabolism in situ, circulating immune cells must express CYP27B1 (coding for 1α-hydroxylase) for activation of 1,25(OH)D and CYP24A1 (coding for 24 hydroxylase) which inactivate all forms of vitamin D by hydroxylation at carbon position 24. Both enzymes are expressed constitutively in PBMC in unstimulated conditions (Fig. 1a, b, and c: “Unstimulated D0”).
Vitamin D enzyme machinery and VDR mRNA expressions are present in healthy donors’ PBMCs. Cells were incubated for 24 h with 25(OH)D (D0: 0 ng/ml, D25: 25 ng/ml, D75: 75 ng/ml, D125: 125 ng/ml) in either unstimulated or stimulated (LPS lipopolysaccharide, 100 ng/ml; PIC polyinosinic-polycytidylic acid, 10 µg/ml) condition. Results are expressed as means ± sem of fold change relative to control, i.e., D0 unstimulated condition. Data were analyzed by two-way ANOVA followed by Bonferroni post-test. (a) VDR expression (n = 4). Two-way ANOVA: ns (not significant). (b) CYP27B1 expression (n = 4). Two-way ANOVA: ns. (c) CYP24A1 expression (n = 5). Two-way ANOVA: ns
Furthermore, we explored the effect of 25(OH)D with or without LPS or PIC stimuli on the enzyme gene expressions in PBMC. After 24 h, we observed no statistically significant dose effect on CYP24A1, CYP27B1, and VDR expression with 25(OH)D in unstimulated or LPS- or PIC-stimulated conditions (Fig. 1a, b, c).
Interestingly, 25(OH)D seemed to induce an overexpression of CYP27B1 in the presence of LPS (Fig. 1b), but insignificant, probably due to the large variation in data. Moreover, the highest dose of 25(OH)D seemed to enhance the expression of CYP24A1 in both unstimulated and LPS- or PIC-stimulated conditions (Fig. 1c).
25(OH)D induces intracellular overexpression of CAMP mRNA and hCAP18 peptide
We evaluated the expression of the CAMP gene after 24-h incubation and its protein product, hCAP18 peptide, after 48-h incubation with 25(OH)D. We observed a significant dose-dependent effect of 25(OH)D on the overexpression of the CAMP gene, with the highest effect for the dose of 125 ng/ml, regardless of the presence of stimulants (Fig. 2a).
25(OH)D induces dose-dependent intracellular CAMP gene and hCAP18 peptide expression. Cells were incubated with 25(OH)D (D0: 0 ng/ml, D25: 25 ng/ml, D75: 75 ng/ml, D125: 125 ng/ml) in unstimulated and stimulated (LPS lipopolysaccharide, 100 ng/ml; PIC polyinosinic-polycytidylic acid, 10 µg/ml) conditions. Results are expressed as means ± sem of fold change relative to control, i.e., D0 unstimulated condition. Data were analyzed by two-way ANOVA followed by Bonferroni post-test. (a) CAMP mRNA expression by RT Q-PCR after 24-h incubation (n = 5). Two-way ANOVA 25(OH)D effect: p < 0.001. (b) hCAP18 expression by western blot after 48-h incubation (n = 4). Two-way ANOVA 25(OH)D effect: p < 0.001. Two-way ANOVA stimuli effect, p = 0.0032. Letters indicate significant differences (p < 0.05) after two-way ANOVA Bonferroni post-test of 25(OH)D effect. Asterisks (*) indicate p-value of one-way ANOVA
On the contrary, hCAP18 peptide expression was both significantly 25(OH)D dose-dependent (p < 0.001) and stimulus-dependent (p = 0.0032), indicating the importance of the presence of microbial patterns (Fig. 2b).
25(OH)D induces LL-37 secretion only in LPS- or PIC-stimulated PBMC
The concentration of LL-37 in the culture medium of PBMC was quantified after 48-h incubation with 25(OH)D. Two-way ANOVA returned significant interaction effect of 25(OH)D and different stimuli of p = 0.022. Presence of both PIC and LPS stimuli induced higher LL-37 secretion in response to 25(OH)D presence, while no effect was observed on the unstimulated condition (Fig. 3). In LPS condition, overproduction of LL-37 is observed with all doses of 25(OH)D, while in PIC condition the stimulation of LL-37 production is only obtained with 125 ng/ml of 25(OH)D.
Extracellular LL-37 peptide concentration conditioned by 25(OH)D only when combined with microbial mimetics. Cells were incubated with 25(OH)D (D0: 0 ng/ml, D25: 25 ng/ml, D75: 75 ng/ml, D125: 125 ng/ml) in unstimulated and stimulated (LPS lipopolysaccharide, 100 ng/ml; PIC polyinosinic-polycytidylic acid, 10 µg/ml) conditions. Supernatant LL37 concentrations normalized by total protein concentrations are expressed as means ± sem (n = 3). Letters indicate significant differences (p < 0.05) of two-way ANOVA followed by Bonferroni post-test. Two-way ANOVA: 25(OH)D effect, p = 0.0475; interaction term 25(OH)D × stimuli, p = 0.022
Discussion
We have previously conducted a clinical trial where we failed to evidence the increase in circulating concentrations of LL-37 following the vitamin D supplementation in healthy volunteers [15]. Following discrepancies on the efficiency of oral vitamin D supplementation as an inductor of LL-37 secretion, we decided to determine the ex vivo effect of vitamin D on LL-37 production from human PBMC. Therefore, we exposed PBMC to four different doses of 25(OH)D to mimic depletion, deficiency, optimal, and supra-physiological blood concentrations. In addition, PBMC were incubated in unstimulated condition or with either bacterial LPS, known to stimulate CAMP expression via Toll-like receptor 4 (TLR4) induction [16], or PIC, a well-known activator of TLR3 simulating viral infection [17].
We confirm that PBMC express the VDR gene and that therefore they may be reactive to the genomic effects of vitamin D. Moreover, we confirm that PBMC can metabolize 25(OH)D since they express CYP27B1 (coding for 1α-hydroxylase) which hydroxylates 25(OH)D at carbon 1α to form 1,25(OH)D, the active metabolite of vitamin D, and CYP24A1 (coding for 24-hydroxylase) which inactivates all forms of vitamin D by hydroxylation at carbon 24 position.
We do not report any significant variation of CYP24A1, CYP27B1, and VDR expression following 25(OH)D incubation even if CYP24A1 seemed to be overexpressed in unstimulated and LPS-stimulated conditions and CYP27B1 only in LPS-stimulated condition. In the kidneys, it has been shown that high levels of circulating 1,25(OH)D stimulate CYP24A1 activity and impair CYP27B1 activity as a negative feedback loop [21]. In macrophages, a slight CYP27B1 inhibition was observed in the presence of 25(OH)D (but not with 1,25(OH)D) after 24 h of incubation [22]. In accordance with our results, the ability of 1,25(OH)D to enhance CYP24A1 activity has been previously reported in monocytes after 24-h incubation [23]. The same authors reported that 1,25(OH)D supplementation induced overexpression of VDR [23]. In contrast, Shirvani-Farsani et al. (2017) reported a VDR underexpression after vitamin D treatment in PBMC of multiple sclerosis patients suggesting that inflammatory state of cells is a key determinant for VDR expression [24]. Nevertheless, the lack of significance of our results could be due to variability in response and composition of PBMC (lymphocyte/monocyte distribution) from different volunteers.
Similar to previously described, 25(OH)D exposition results in an overexpression of the CAMP gene and the hCAP18 peptide in PBMC cultures under 24 h. This effect is stronger on gene expression than peptide expression suggesting a post-transcriptional regulation. This kind of regulation was previously described in mouse promyelocytic cell line in which the overexpression of the miRNA “miR-130a” downregulated hCAP18 peptide expression [25].
Confirming our clinical trial results, PBMC incubated in unstimulated condition, i.e., without microbial mimetics, showed secreted LL-37 concentration unchanged regardless of the 25(OH)D dose. Interestingly, we found a significant increase of LL-37 production in the presence of 25(OH)D when PBMC were stimulated with bacterial mimetic LPS (TLR4 agonist) or viral mimetic PIC (TLR3 agonist). TLR activators are known to interfere with VDR signaling and to modulate the release of LL-37 [1, 26]. Liu et al. reported that the TLR (1–2-4) activation of monocytes/macrophages by pathogen stimulators upregulated the expression of VDR and vitamin D hydroxylase genes, leading to the induction of cathelicidin production and the killing of intracellular M. tuberculosis [1].
In the THP-1 human blood monocytic cell line, LPS and 1,25(OH)D both increased VDR mRNA levels 20 h after treatment [27]. Others have shown that exposure of keratinocytes to PIC increased the rate of 1,25(OH)D production and the expression of CYP27B1 [28]. These results suggest that TLR agonists activate vitamin D metabolism and signaling in situ. In keratinocytes, the in situ production of vitamin D which is known to have anti-inflammatory properties would permit to control the inflammatory process due to TLR inducers such as PIC, TNF, or LPS and to stimulate cathelicidin production [29].
How LPS and PIC trigger VDR signaling is still a matter of debate. Zhao et al. (2018) reported evidence that LPS downregulates VDR expression in oral mucosal epithelia dependent on TNFα-miR346 signaling, and further suggested that vitamin D/VDR can suppress LPS-induced keratinocyte apoptosis by regulating NF-κB pathway [30]. Conversely, 1,25(OH)D is known to upregulate TLR10 and to downregulate TLR 2, 4, and 5 in human monocyte THP-1 suggesting possible crosstalk between VDR and TLR signaling [31]. This crosstalk between VDR and TLR signaling pathways could explain why release of LL-37 is dependent on vitamin D concentration only when PBMC are stimulated by LPS or PIC. Actually, the TLR4-inducer LPS is known to be a key regulator of the expression and the activity of serine proteinase 3 that cleaves hCAP18 into LL-37 and cathelin [32]. Induction of TLR pathways would potentialize VDR signaling so that we observed a higher concentration of LL-37 with high doses of 25(OH)D only in stimulated conditions which allowed to strongly activate serine proteinase 3.
Whether the processing of LL-37 occurs inside the cell granules or it involves extracellular compartment is still debated. Pioneer studies reported that hCAP18 is excreted and then processed to LL-37 extracellularly in a reaction catalyzed by serine proteinase 3 [4]. More recent works advanced that neutrophils and monocytes express serine proteinase 3 so that the processing could occur in vacuoles before exocytosis [33]. Nevertheless, this control of processing and externalization could occur in vivo both inside the cells (to release adequate amounts of the antimicrobial peptide in case of infection by bacteria, virus, and fungi) and/or outside the cells (if LL-37 concentration is too high in the bloodstream). This regulation is crucial because the LL-37 killing mechanisms are not specific so that in excess it can become a cytotoxic agent towards commensal bacteria and/or host cells [34].
To consolidate our data, it could be necessary to increase the number of donors’ PBMC samples and to determine the cathelicidin expression after longer incubation time in order to distinguish between genomic and non-genomic regulation process. Moreover, we cannot affirm undoubtedly that LL-37 is the only peptide present in the culture media since the LL-37 ELISA kit used does not discriminate between the LL-37 and hCAP18 forms. It would be of great interest to develop a well-calibrated reference method to discriminate LL-37 and hCAP18 quantification in biological samples. For the moment, this is only possible by using SELDI-TOF mass spectrometry, as previously used to detect LL-37 in pellets of 1,25(OH)D-stimulated primary human monocytes [1].
Conclusion
In circulating PBMC, intracellular expression of human cathelicidin is induced by 25(OH)D in both unstimulated and stimulated cells. However, extracellular production of LL-37 appears dependent on 25(OH)D only when PBMC are stimulated by bacterial or viral pathogen mimetics which is the major finding of our work. These data suggest that release of LL-37 in extracellular compartment is finely regulated to avoid non-specific killing of host microbiota since bactericidal properties of this cationic peptide are not strictly specific. Further studies should be encouraged to clarify the process of cleavage and externalization/degranulation of LL-37 given that this antibacterial and antiviral peptide could be a key factor in the reduced risk of influenza and COVID-19 infections associated to vitamin D supplementation as recently suggested [35, 36].
Change history
24 January 2022
A Correction to this paper has been published: https://doi.org/10.1007/s13105-022-00873-w
References
Liu PT, Stenger S, Li H et al (2006) Toll-like receptor triggering of a vitamin D-mediated human antimicrobial response. Science 311:1770–1773. https://doi.org/10.1126/science.1123933
Vandamme D, Landuyt B, Luyten W, Schoofs L (2012) A comprehensive summary of LL-37, the factotum human cathelicidin peptide. Cell Immunol 280:22–35. https://doi.org/10.1016/j.cellimm.2012.11.009
Chen X, Zou X, Qi G et al (2018) Roles and mechanisms of human cathelicidin LL-37 in cancer. Cell Physiol Biochem 47:1060–1073. https://doi.org/10.1159/000490183
Sorensen OE (2001) Human cathelicidin, hCAP-18, is processed to the antimicrobial peptide LL-37 by extracellular cleavage with proteinase 3. Blood 97:3951–3959. https://doi.org/10.1182/blood.V97.12.3951
Chun RF, Liu NQ, Lee T et al (2015) Vitamin D supplementation and antibacterial immune responses in adolescents and young adults with HIV/AIDS. J Steroid Biochem Mol Biol 148:290–297. https://doi.org/10.1016/j.jsbmb.2014.07.013
Kanda N, Hau CS, Tada Y et al (2012) Decreased serum LL-37 and vitamin D3 levels in atopic dermatitis: relationship between IL-31 and oncostatin M. Allergy 67:804–812. https://doi.org/10.1111/j.1398-9995.2012.02824.x
Lungu PS, Kilembe W, Lakhi S et al (2021) A comparison of vitamin D and cathelicidin (LL-37) levels between patients with active TB and their healthy contacts in a high HIV prevalence setting: a prospective descriptive study. Trans R Soc Trop Med Hyg 16:trab126. https://doi.org/10.1093/trstmh/trab126
Meca A-D, Ștefănescu S, Bogdan M et al (2021) Crosstalk between vitamin D axis, inflammation and host immunity mechanisms: a prospective study. Exp Ther Med 21:608. https://doi.org/10.3892/etm.2021.10040
Bhan I, Camargo CA, Wenger J et al (2011) Circulating levels of 25-hydroxyvitamin D and human cathelicidin in healthy adults. J Allergy Clin Immunol 127:1302-1304.e1. https://doi.org/10.1016/j.jaci.2010.12.1097
Dixon BM, Barker T, McKinnon T et al (2012) Positive correlation between circulating cathelicidin antimicrobial peptide (hCAP18/LL-37) and 25-hydroxyvitamin D levels in healthy adults. BMC Res Notes 5:575. https://doi.org/10.1186/1756-0500-5-575
Stukes TM, Shary JR, Wei W et al (2016) Circulating cathelicidin concentrations in a cohort of healthy children: influence of age, body composition, gender and vitamin D status. PLoS ONE 11:e0152711. https://doi.org/10.1371/journal.pone.0152711
Acen EL, Biraro IA, Worodria W et al (2021) Impact of vitamin D status and cathelicidin antimicrobial peptide on adults with active pulmonary TB globally: a systematic review and meta-analysis. PLoS ONE 16:e0252762. https://doi.org/10.1371/journal.pone.0252762
Harrison SE, Oliver SJ, Kashi DS et al (2021) Influence of vitamin D supplementation by simulated sunlight or oral D3 on respiratory infection during military training. Med Sci Sports Exerc 53:1505–1516. https://doi.org/10.1249/MSS.0000000000002604
Sanders EC, Burkes RM, Mock JR et al (2021) Bronchoalveolar lavage and plasma cathelicidin response to 25-hydroxy vitamin D supplementation: a pilot study. Chronic Obstr Pulm Dis 8:371–381. https://doi.org/10.15326/jcopdf.2021.0220
Goncalves-Mendes N, Talvas J, Dualé C et al (2019) Impact of vitamin D supplementation on influenza vaccine response and immune functions in deficient elderly persons: a randomized placebo-controlled trial. Front Immunol 10:65. https://doi.org/10.3389/fimmu.2019.00065
Li G, Domenico J, Jia Y et al (2009) NF-kappaB-dependent induction of cathelicidin-related antimicrobial peptide in murine mast cells by lipopolysaccharide. Int Arch Allergy Immunol 150:122–132. https://doi.org/10.1159/000218115
Sokolova TM, Shuvalov AN, Poloskov VV et al (2014) Grippol, Vaxigrip and influvac vaccines–inductors of innate and adaptive immunity factor genes in human blood cells. Zh Mikrobiol Epidemiol Immunobiol 5:37–43
Mahbouli S, Talvas J, der Vartanian A et al (2018) Activation of antioxidant defences of human mammary epithelial cells under leptin depend on neoplastic state. BMC Cancer 18:1264. https://doi.org/10.1186/s12885-018-5141-8
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) method. Methods 25:402–408. https://doi.org/10.1006/meth.2001.1262
Talvas J, Caris-Veyrat C, Guy L et al (2010) Differential effects of lycopene consumed in tomato paste and lycopene in the form of a purified extract on target genes of cancer prostatic cells. Am J Clin Nutr 91:1716–1724. https://doi.org/10.3945/ajcn.2009.28666
Bikle DD (2014) Vitamin D metabolism, mechanism of action, and clinical applications. Chem Biol 21:319–329. https://doi.org/10.1016/j.chembiol.2013.12.016
Rafique A, Rejnmark L, Heickendorff L, Møller HJ (2019) 25(OH)D3 and 1.25(OH)2D3 inhibits TNF-α expression in human monocyte derived macrophages. PLoS One 14(4):e0215383. https://doi.org/10.1371/journal.pone.0215383
Kreutz M, Andreesen R, Krause SW et al (1993) 1,25-dihydroxyvitamin D3 production and vitamin D3 receptor expression are developmentally regulated during differentiation of human monocytes into macrophages. Blood 82:1300–1307
Shirvani-Farsani Z, Kakhki MP, Gargari BN et al (2017) The expression of VDR mRNA but not NF-κB surprisingly decreased after vitamin D treatment in multiple sclerosis patients. Neurosci Lett 653:258–263. https://doi.org/10.1016/j.neulet.2017.05.050
Larsen MT, Häger M, Glenthøj A et al (2014) miRNA-130a regulates C/EBP-ε expression during granulopoiesis. Blood 123:1079–1089. https://doi.org/10.1182/blood-2013-08-523233
Siswanto S, Zuhriyah L, Handono K et al (2015) Mycobacterium tuberculosis DNA increases vitamin D receptor mRNA expression and the production of nitric oxide and cathelicidin in human monocytes. Malays J Med Sci 22:18–24
Pramanik R, Asplin JR, Lindeman C et al (2004) Lipopolysaccharide negatively modulates vitamin D action by down-regulating expression of vitamin D-induced VDR in human monocytic THP-1 cells. Cell Immunol 232:137–143. https://doi.org/10.1016/j.cellimm.2005.03.004
Miodovnik M, Koren R, Ziv E, Ravid A (2012) The inflammatory response of keratinocytes and its modulation by vitamin D: the role of MAPK signaling pathways. J Cell Physiol 227:2175–2183. https://doi.org/10.1002/jcp.22951
Schauber J, Dorschner RA, Coda AB et al (2007) Injury enhances TLR2 function and antimicrobial peptide expression through a vitamin D–dependent mechanism. J Clin Invest 117:803–811. https://doi.org/10.1172/JCI30142
Zhao B, Li R, Yang F et al (2018) LPS-induced vitamin D receptor decrease in oral keratinocytes is associated with oral lichen planus. Sci Rep 8:763. https://doi.org/10.1038/s41598-018-19234-z
Verma R, Jung JH, Kim JY (2014) 1,25-dihydroxyvitamin D3 up-regulates TLR10 while down-regulating TLR2, 4, and 5 in human monocyte THP-1. J Steroid Biochem Mol Biol 141:1–6. https://doi.org/10.1016/j.jsbmb.2013.12.012
Chen Y, Liu Z, Pan T et al (2018) JMJD3 is involved in neutrophil membrane proteinase 3 overexpression during the hyperinflammatory response in early sepsis. Int Immunopharmacol 59:40–46. https://doi.org/10.1016/j.intimp.2018.03.027
Zhou Z, Richard C, Ménard HA (2000) De novo synthesis of proteinase 3 by cytokine primed circulating human polymorphonuclear neutrophils and mononuclear cells. J Rheumatol 27:2406–2411
Sancho-Vaello E, Gil-Carton D, François P et al (2020) The structure of the antimicrobial human cathelicidin LL-37 shows oligomerization and channel formation in the presence of membrane mimics. Sci Rep 10:2045–2322. https://doi.org/10.1038/s41598-020-74401-5
Grant WB, Lahore H, McDonnell SL et al (2020) Evidence that Vitamin D supplementation could reduce risk of influenza and COVID-19 infections and deaths. Nutrients 12(4):988. https://doi.org/10.3390/nu12040988
Crane-Godreau MA, Clem KJ, Payne P, Fiering S (2020) Vitamin D deficiency and air pollution exacerbate COVID-19 through suppression of antiviral peptide LL37. Front Public Health 8:232. https://doi.org/10.3389/fpubh.2020.00232
Funding
This work was supported by the 2014 Bernard Beaufrère research prize from the French Society of Clinical Nutrition and Metabolism (SFNEP). Société Française de Nutrition Entérale et Parentérale, prix Bernard Beaufrère 2014,Talvas Jérémie.
Author information
Authors and Affiliations
Contributions
The authors declare that all data were generated in-house and that no paper mill was used. The authors’ responsibilities were as follows: NGM, MCF, AR, MPV, and JT designed the protocol; SAD, GM, KL, SR, NGM, RB, MPV, and JT performed the experiments, analyzed the data, and wrote the manuscript; and all the authors read and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval
Ethical review and approval were not required for this study in accordance with the local legislation and institutional requirements.
Consent to participate
The human blood samples were obtained from healthy volunteers of the local French blood agency (Etablissement Français du Sang, EFS, Auvergne-Rhône-Alpes). After full pertinent information, written informed consents were obtained from all blood donors involved in the study as statutory required (article R.1221–5 of the Public Health Code, 12/01/2009 and 11/06/2006 decrees).
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Key Points
•PBMC are able to activate vitamin D in situ
•Vitamin D stimulates cathelicidin antimicrobial peptide production by PBMC
•Anti-infectious effect of vitamin D is observable when immune cells are stimulated
Rights and permissions
About this article
Cite this article
Aldekwer, S., Goncalves-Mendes, N., Bingula, R. et al. 25-Hydroxyvitamin D potentializes extracellular cathelicidin release from human PBMC stimulated ex vivo with either bacterial (LPS) or viral (P: IC) mimetics. J Physiol Biochem 78, 335–342 (2022). https://doi.org/10.1007/s13105-021-00868-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13105-021-00868-z